RE the AI GLP1 company, Washington Post has an article today by someone who used one of those compounded products,…
Monday Morning Update 11/20/17
Top News
The VA is considering merging its Choice program – which allows veterans who can’t get timely VA appointments to see private doctors — with the military’s Tricare, which offers health insurance to active service members.
A VA statement says that work on the planned VA-DoD single EHR platform led VA Secretary David Shulkin to have conversations with the White House about merging the programs to “provide better care for veterans at a lower cost to taxpayers.”
Some large veteran groups immediately expressed concern with the plan, fearing that it could turn the VA’s direct care model into a DoD Tricare-like insurance program in which private providers deliver services and insured members pay premiums, deductibles, and co-pays.

Shulkin said in a May 2017 White House briefing:
In terms of our Choice Program, we still today only have three Department of Defense facilities that participate in the Choice network. We need to get the Department of Defense and VA to make all their facilities and our facilities open to veterans and to active service members. We certainly have to work with Congress and our veteran service organizations to redesign this Choice Program. It will expire essentially at the end of the year, and we need new legislation — this Congress — to make sure that veterans don’t go back to waiting longer than they need to wait to get care in the community. So we have to pass legislation this year.
Reader Comments

From Logic Pretzel: “Re: MHS Genesis. Deployment can’t continue beyond the four completed pilot sites until an independent assessment of cost and suitability is performed, which may not be finished until a year or more from now. That piles more risk on the VA’s piggyback decision and undercuts the credibility of their rationale that there’s no time to do a proper competitive search.” The DoD says the review will continue through late 2018, meaning that the VA is rushing into its no-bid contract with Cerner without even knowing whether DoD will continue its own Cerner rollout.
From Short Attn: “Re: HIStalk. It’s too long for me to read. I’m glad you at least run headlines to save me time.” I spend many hours each week extracting the health IT news and information that I think is most relevant and interesting, condensing it massively and dividing it into categories for easy skipping. You are free to consume as little or as much of what I write, but someone out there is poring over every word to gain an edge to allow them to steal your job or your customer. It’s good to have all the knowledge you can get when you’re a knowledge worker.

From Chalky Aftertaste: “Re: patient-preferred by whom? Check out this bizarre vanity press release.” A horribly written announcement published on a free press release service – I’d bet a stack of non-American currency that it wasn’t written by a native English speaker – lauds the medical accomplishments of an Indiana neurosurgeon, indisputably proven by a single fawning Facebook quote from an alleged patient and a short list of educational qualifications that includes “CMS Meaningful Use Stage 1 Certification from Epic Care Ambulatory EMR” (has he tapped into an unmet consumer demand for Epic-certified neurosurgeons?) The conferrer of the award is Patient Preferred Physicians and Practitioners, an “exclusive medical society” whose corporate address is a Boca Raton mail drop. Most of its honorees seem to be in late in their careers and I’m guessing their modest social media skills misled them into thinking that buying a vanity award would make them seem hipper.
From Pernicious: “Re: diagnostic apps and sites. Don’t you think these will revolutionize healthcare and that you should mention them more often?” No. Non-clinicians think patients are undiagnosed or misdiagnosed a lot more than happens in real life. We don’t have a diagnosis problem – we’re getting killed (literally) by conditions that have been perfectly diagnosed but are either untreated or expensively held in check at best. From a public health perspective, the last thing we need is wiring up millions of Americans, testing their genes, or poring over images of their innards to detect theoretical problems. That’s why experienced doctors roll their eyes at greenhorns who order tons of lab and imaging studies, with the near-certainty of finding something out of range requiring Whac-A-Mole action that’s not good for anyone except the companies making money off unnecessary tests and treatments. Western culture and medicine looks at illness and death much differently than most of the world, and our fascination with gadgetry and medical heroics that prop up the comforting illusion of immortality instead of taking on less-decisive public health issues has left us with a society that’s #1 by far in healthcare costs, but that barely beats Cuba in WHO’s health rankings.

From IA Taxpayer: “Re: University of Iowa Hospitals and Clinics. Shutting down its Epic Community Connect program. Team members were told on Friday, November 17. The business unit will be integrated into UIHC IT, UIHC is not seeking new Community Connect business, services to existing clients will be cut off, and layoff of 50 percent of the staff (more than 30 FTEs) will happen by July 1, 2018. The message is that the program has a financially flawed business model that provides only a fraction of the ongoing revenue needed to support existing staff. UIHC has negative margins, but within increased focus on patient-centered care, referral patterns from those hospitals that joined the program will be negatively impacted.” Unverified. I’ve emailed a contact there for a comment.
HIStalk Announcements and Requests
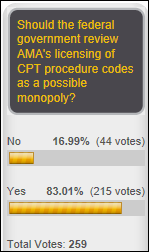
The vast majority of poll respondents think the federal government should review whether the AMA-owned CPT procedure code system constitutes a monopoly. An anonymous reader says rather insightfully that it’s not illegal to BE a monopoly, but rather to ACT like one, while John recalls an early copyright misuse claim in which the ruling was that while the federal government may have created a monopoly by mandating the use of CPT codes, AMA didn’t seek that monopoly. Another anonymous reader wonders whether AMA perpetuates the use of E&M codes, which he or she blames on note bloat and lack of usability of clinical documentation functions.
New poll to your right or here: will Cerner’s EHR allow the VA to exchange electronic information with non-VA providers?

I’m fascinated by the small number responses to my poll in which I asked HIStalkapalooza attendees what aspects drew them to the event. #1 by far was the hosts, stage show, and HISsies, which is surprising because the in-person feedback is usually that they couldn’t hear or didn’t care. Only 10 percent of respondents ranked “free food and drinks” as their motivator. Based on that, the ideal event would be open to everyone, feature a less-expensive dance band, let everyone buy their own food and drinks, and carry on the stage show as always. The only aspect I’ll miss (since I’m still not inclined to do it again) is the interesting roster of attendees, which as far as I know is unmatched since it included providers, vendors, professors, government officials, equities analysts, and even people from competing websites and publications.
It seems as though many members of the Greatest Musical generation of the 1960s and 1970s are dying lately as that cohort starts to hit the mortality wall. The latest: AC/DC co-founder, guitarist, and songwriter Malcolm Young, who died of dementia this weekend at 64 in leaving the band with one original member, his schoolboy-uniformed brother Angus Young. A third brother, AC/DC producer George Young, died last month at 70. Meanwhile, David Cassidy (aka Keith Partridge) is apparently also close to death from dementia and organ failure. Life is a (hopefully) long line to the cliff where it will eventually be your turn to be pushed off.
This Week in Health IT History
One year ago:
- The Gates Foundation issues a grant to create a blockchain-powered medical record.
- HIMSS and CHIME create an international group to manage programs outside of North America.
- HHS Secretary Sylvia Burwell warns that a “repeal and replace” approach to the ACA will cause the program to collapse due to insurers pulling out because of uncertainty, leaving 20 million more people uninsured.
Five years ago:
- HP writes down $9 billion after finding that its recent acquisition Autonomy misstated earnings.
- The CEO of Quest Diagnostics says the company is “redirecting” its EHR business (ChartMaxx, Care360) to work with enterprise EHR vendors like Cerner, Epic, and McKesson.
- The National Football League signs a contract with EClinicalWorks to provide an EHR that can support the research and treatment of player head injuries.
- New sales were announced by Acuo, Merge, 3M, and Humedica.
Ten years ago:
- A UK survey finds that GP support for the NPfIT project is down to 23 percent.
- Sunquest, fresh off its acquisition by Vista Equity Partners, announces that it will increase investment in its radiology information system and begin actively marketing it again.
- Wheaton Franciscan Healthcare VP of IT Tim Belec is shot by a 17-year-old robber in the organization’s parking lot as he leaves work.
- Dennis Quaid’s newborn twins are given a heparin overdose at Cedars Sinai due to improper stocking of a medication dispensing cabinet.
Last Week’s Most Interesting News
- VA Secretary David Shulkin asks a House appropriations subcommittee to approve using $782 million of the VA’s budget to kick off its Cerner project while sidestepping member questions about how Cerner will exchange information with community-based providers.
- A multi-day system downtime leaves CVS Pharmacy unable to fill prescriptions.
- Meditech announces a cloud-based, subscription-priced version of its EHR.
- A Black Book survey finds that only 19 percent of post-acute care providers have any degree of EHR capability and that 90 percent of long-term care providers don’t exchange information with referring doctors or hospitals.
- In England, a migrant rights group challenges an agreement by which NHS makes patient data available to the Home Office for immigration enforcement.
Webinars
November 30 (Thursday) 1:00 ET. “Making Clinical Communications Work in Your Complex Environment.” Sponsored by: PatientSafe Solutions. Presenters: Steve Shirley, VP/CIO, Parkview Medical Center; Richard Cruthirds, CIO, Peterson Health. Selecting, implementing, and managing a mobile clinical communications platform is a complex and sometimes painful undertaking. With multiple technologies, stakeholders, and disciplines involved, a comprehensive approach is required to ensure success. Hear two hospital CIOs share their first-hand experience, lessons learned, and demonstrated results from deploying an enterprise-wide mobile clinical communications solution.
December 5 (Tuesday) 2:00 ET. “Cornerstones of Order Set Optimization: Trusted Evidence.” Sponsored by: Wolters Kluwer. Updating order sets with new medical evidence is crucial to improving outcomes, but coordinating maintenance for hundreds of order sets with dozens of stakeholders is a huge logistical challenge. For most hospitals, managing order set content is labor intensive and the internal processes supporting it are far too inefficient. Evidence-based order sets are only as good as their content, which is why regular review and updates are essential. This webinar explores the relationship between clinical content and patient care with an eye toward building trust among the clinical staff. Plus, we will demonstrate a new evidence alignment tool that can easily incorporate the most current medical content into your order sets, regardless of format, including Cerner Power Plans and Epic SmartSets.
Previous webinars are on our YouTube channel. Contact Lorre for information.
Acquisitions, Funding, Business, and Stock
Drug company Roche will acquire laboratory-focused health analytics technology vendor Viewics. Roche Diagnostics offers laboratory analyzers, inventory software, and middleware and will deploy the Viewics solution to help labs improve profitability and care.

Madison, WI-based image sharing app vendor ImageMoverMD separates from its CEO, hires a former drug rep as president, and brings on a COO (who comes from Epic) and a sales director in hopes of boosting sales. The two physician co-founders are UW radiologists who are also board-certified in clinical informatics.
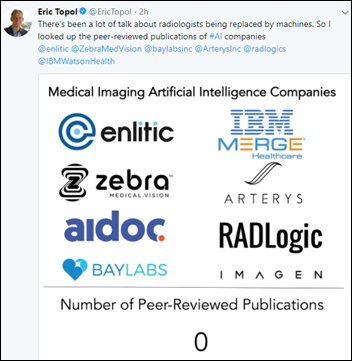
Eric Topol apparently isn’t convinced that radiologists will be replaced by artificial intelligence, based on the lack of peer-reviewed publications of the companies that offer imaging AI.

Advisory Board closes the sale of its healthcare business to Optum, with CEO Robert Musslewhite staying on.
People

Glenn Galloway (Children’s Health Network) joins Center for Diagnostic Imaging as CIO. He previously worked as CIO of Children’s Hospitals and Clinics of Minnesota and co-founded Healthia Consulting in 1998, spending several years as SVP of Ingenix Consulting after it acquired Healthia in 2007. Long-time readers will recall that Healthia (and thus Glenn) sponsored the first-ever HIStalkapalooza at HIMSS08 in Orlando, a two-hour cocktail party for around 200 attendees at what was then the Peabody Hotel.


ZappRx hires Rich Cramer (Upfront Healthcare Services) as VP of commercial operations and names James Cornicelli (UCB) as VP of corporate strategy.
Announcements and Implementations
Sunquest will integrate its Mitogen laboratory information management system for molecular diagnostics and precision medicine with oncology molecular decision support technology vendor N-of-One. Private pathology lab CellNetix will be the first customer.

South Georgia Medical Center (GA) goes live on Epic, saying that within the first two weeks it had exchanged information with 20 or more facilities.
Government and Politics
The controversial president of the Fresno, CA school board attacks a Center for Health Journalism writer for her newspaper series on sex education and high birth rates. He launches a Twitter tirade, compares her on talk radio to a “child sex predator,” and publishes her work phone number on Facebook in urging others to contact her.

A California state judge rules that Sutter Health intentionally destroyed 192 boxes of documents that were being sought by employers and labor unions who had charged Sutter with market power abuse and charging inflated prices.
Florida’s Agency for Healthcare Administration takes the next step after heavily redacting nursing home inspection records in claiming threats to the privacy of residents – removing the records from its website completely. Florida newspapers mentioned the censored inspection reports in their coverage of the deaths of 13 seniors in a rehabilitation center after September’s Hurricane Irma, after which the AHCA took all nursing home records offline without notice. Some South Florida counties have also refused to release the emergency management plans they approved for nursing homes – including the all-important sections of how they would keep residents comfortable during power outages –even though they had previously said they were public record.
Other

The local paper says patient appointments at Banner Health’s Tucson hospitals and clinics are being delayed due to its October 1 go-live of Cerner, with Banner’s chief clinical officer admitting that it has been a “painful period.” The health system expects the situation to be resolved by December 31. The Arizona Department of Health Services is investigating complaints about the impact of the new system but won’t provide details. Banner acquired the former money-losing University of Arizona Health Network in 2015, which had gone live (and well over budget) with its $115 million Epic project less than a year before. Banner’s corporate standard is Cerner.
A JAMA research letter questions whether hospitals are gaming the federal government’s Hospital Readmission Reduction Program in avoiding financial penalties by upcoding severity of illness instead of actually improving care.
County officials question the auditor and CEO of Blount Memorial Hospital (TN) about why they weren’t told that the hospital foundation’s since-fired executive director had embezzled $187,000 over nine years. The employee issued checks to herself using QuickBooks accounting software, then modified the QuickBooks entry to make it appear that the payee was a foundation business partner. The foundation did not require checks to bear a second signature and did not conduct yearly audits.

In England, a man who proposed to his girlfriend last New Year’s Eve — the day before he suffered from sepsis-induced brain damage that nearly killed him — proposes again from the rehab hospital, using eye-tracking technology to communicate. His girlfriend said “yes” a second and his therapists and caregivers prepared him to make his way down the aisle in a wheelchair and to place the ring on her finger. The eye-tracking technology is from Eye Gaze, which offers assistive technology and eye tracking human cognition research.
Sponsor Updates
- Medicity publishes a new report, “HIE Preparedness: Learning from Recent Health Care Disasters.”
- MedData and Experian Health will exhibit at the Illinois AAHAM Annual State Institute November 29-December 1 in East Peoria.
- Meditech will exhibit at the West Virginia HIMSS 2017 Fall Event November 30-December 1 in Morgantown.
- PatientPing announces that its ACO customers achieved $120 million in cost savings in 2016.
- Navicure will exhibit at HFMA Maine’s Revenue Cycle Workshop November 30-December 1 in Portland.
- A large health plan upgrades to ZeOmega’s Jiva 6.1 population health management solution.
- The Technology Association of Georgia recognizes Patientco’s Jason Kuo as 2017 TAG Product Manager of the Year.
- TransUnion partners with Mercy Home for Boys & Girls to launch the Friends First mentoring program.
- Verscend Technologies publishes a new white paper, “Thinking inside the box with a provider decision quadrant.”
- Visage Imaging previews its Visage 7 Enterprise Imaging Platform in a new video.
- Vocera Communications will present at the Piper Jaffray Healthcare Conference November 28 in November 28.
Blog Posts
- Supporting Veterans Through Improved Access to Quality Health Care (LifeImage)
- True Stories from Hurricane Harvey: Hospital Emergency Management for Severe Weather (LiveProcess)
- What You Need to Know About the MACRA Final Ruling (Meditech)
- Post-Acute Strategy: Using Technology to Attract and Retain Health System Relationships (Netsmart)
- Be Strong (NVoq)
- Sanford Health earns millions and increases patient satisfaction by improving patient collections (Experian Health)
- Secure Data Visibility at the Point of Care (PatientSafe Solutions)
- Healthcare Compliance: What it Costs and How it’s Done (The SSI Group)
- 5 Easy (and Absolutely Free) Ways to Show Gratitude to Patients and Staff (Solutionreach)
- Embracing Change (even when it hurts). (Voalte)
Contacts
Mr. H, Lorre, Jenn, Dr. Jayne, Lt. Dan.
Get HIStalk updates. Send news or rumors.
Contact us.





The reason I didn’t reply to your Histalkpalooza survey was simply because you did not offer networking with the great grp of ppl attending.
Same reason why I didn’t reply to the survey…
I’ve always loved AC/DC.
One tidbit others might enjoy. The movie “School of Rock” performed an awesome cover of “It’s a Long Way To the Top”, and it made me wonder. Why did this song seem to kind of disappear from the band’s repertoire? It’s a great song after all.
It turns out this was no accident. When AC/DC’s first lead singer passed away, the band decided they would no longer perform the song live. As a sign of respect.