I was born roughly 2 months after the US space program began (Explorer 1), and I've followed it all my…
News 5/24/17
Top News
The Bipartisan Policy Center calls for creating a public-private effort to set health IT safety priorities and to disseminate best practices.
The report recommends:
- General patient safety efforts should incorporate the safety of health IT throughout its life cycle.
- Health IT safety should be addressed via a non-punitive learning system similar to medical error reporting.
- Voluntary and mandatory reporting systems should collect de-identified data about health IT safety issues that can drive creation of evidence-based practices and tools.
The report does not specifically address ONC’s proposed EHR safety center.
Reader Comments
From Vaporware?: “Re: Cerner. How long do they get a free pass on selling interoperability without delivering? Beth Israel Deaconess Care Organization lists just six EHRS of the 40 its providers use – Cerner not among the six – that are willing and able to contribute information to its population health analytics system. Do the live MHS Genesis pilot sites have connectivity to outside EHRs?” I’ll invite readers with the firsthand experience with either project that I don’t have to comment anonymously.
From Chaste Kiss: “Re: this HIMSS-owned publication’s story. I’m embarrassed that I actually clicked the tweet to read more.” No wonder – you were cheated when a publication runs a story titled “Is a takeover of Athenahealth inevitable?” that doesn’t actually answer the question it poses (nor could it). It simply rewords a lazy Bloomberg opinion column in which those original authors speculated –without using any sources or providing evidence of analytical thought — that maybe Cerner, IBM, UnitedHealthGroup, Aetna, or Epic might be interested in buying Athenahealth (the fact that Epic was named means the authors are clueless). The embarrassingly lazy source article wasn’t improved one iota by having the HIT publication improperly legitimize it by rephrasing its undisciplined conclusions. In both cases, the writers seemed desperate to fill their allotted space with whatever fizzy “news” they could make up with a minimum of expended effort.
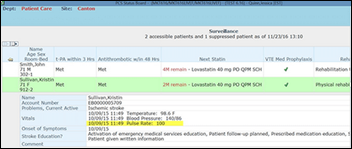
From Greg: “Re: sepsis monitoring. The new Meditech 6.1 Surveillance product has a rules-based approach that looks at real-time EMR clinical data in the EMR. There the clinician can be notified and take appropriate action in an efficient and sometimes life-saving manner. These actions can include orders, medications, labs, documentation, problems, interventions, etc. I have personally not seen another EMR that is as far advanced with regards to surveillance.”
From SgtPerkins: “Re: John Brownstein’s tweet about Epic’s App Orchard developer terms. It is no longer available. $50 says he got a C&D from Epic to remove it. Even their awful legalese is intellectual property to them.” Unverified. My screenshot of his tweet from the Boston Children’s chief innovation officer is here. My experience is that such takedown requests often come from an individual’s employer rather than the subject of their comments, especially when the employer is a partner of the company mentioned (as I well know, having been threatened in my early, less-anonymous HIStalk days with being fired by my hospital employer for writing about one of our vendors even though it wasn’t inside information). Also, Epic’s App Orchard legal wording wasn’t really a secret anyway since it’s publicly available and, as other readers have noted, is similar to that of the Apple Store.
HIStalk Announcements and Requests


Readers funded the DonorsChoose grant request of Mrs. D in Arkansas, who asked for writing journals and math activity kits and games for her elementary school class. She reports, “These materials have allowed students to learn using a hands on approach. We love all of our games and our writing journals! Students are so proud to have their own journal to write in each day. You have made all the difference! Thanks again.”
Webinars
None scheduled soon. Previous webinars are on our YouTube channel. Contact Lorre for information on webinar services.
Acquisitions, Funding, Business, and Stock
Post-acute care software vendor Optima Healthcare Solutions acquires Hospicesoft, which offers hospice software.
Sales
Five Ontario hospitals add PatientKeeper CPOE and medication reconciliation to their existing system and will expand their use of the company’s physician documentation solution, providing an overlay to Meditech Magic and other systems.
St. Joseph Health (CA) will expand its use of Clearsense analytics in implementing Inception for archiving, access, and visualization of its legacy Meditech data.
Harbin Clinic (GA) chooses analytics from PrecisionBI, a division of Meridian Medical Management.
People

A Philadelphia innovation organization recognizes Children’s Hospital of Philadelphia AVP/Chief Health Informatics Officer Bimal Desai, MD, MBI as its healthcare innovator of the year. He co-founded CHOP spinoff Haystack Informatics, which offers security technology that detects EHR snooping by learning normal staff behavior and calling out exceptions.

NantHealth hires Ron Louks (BlackBerry) as COO.
Announcements and Implementations

Rush Health (IL) launches Rush Health Connect, which aggregates information from its Epic and Allscripts EHRS using InterSystems HealthShare to give clinicians patient information and real-time alerts and notifications.
Change Healthcare joins the Hyperledger open source blockchain project.
The Fresno paper covers the use by Community Medical Centers of RightPatient iris recognition at patient registration, which the article explains isn’t an infrared scan, but rather just a photo of the patient’s eye. It also notes that palm vein ID systems are an alternative. RightPatient can also analyze a patient’s general headshot to identify them going forward.
DrFirst will integrate prescription pricing information from GoodRx into its e-prescribing platform.
Government and Politics
A VA OIG suicide prevention report finds that around 20 percent of inspected VA facilities don’t perform the mandated five outreach events per month, haven’t developed suicide prevention safety plans that are documented in the EHR, and don’t flag high-risk patients in the EHR. More alarmingly, OIG found that while 84 percent of non-clinical hospital hires completed their mandatory suicide prevention training within 90 days, nearly half of newly hired clinicians did not do so.

The director of Denmark’s version of the FDA expresses concern that US tech companies like Google and Apple are rolling out medically-related fitness tools and devices that “have no requirements to demonstrate efficacy and safety, but we are forced into the direction of taking them seriously.” The finance minister warns that while patients are notified by email any time their Denmark-based interoperable electronic medical records are viewed, private services and apps offer no such protection, explaining, “We need to make our citizens aware that there is no free lunch with these big companies. People should make some more demands when they give their data away. These companies want to know what you want before you know it yourselves. We need to look into regulation. These private companies will have this patient data for eternity. Can we be sure they’ll always do good things with it?”
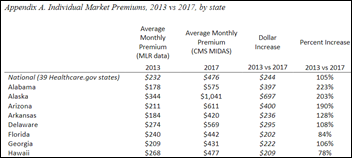
A report by HHS’s Office of the Assistant Secretary for Planning and Evaluation blames the Affordable Care Act for the 105 percent jump in premiums from 2013 to 2017 in the 39 states participating in Healthcare.gov, as the average monthly premium increased from $224 to $476. The report, however, didn’t look at the increase in non-exchange sold individual plans and admits in its “Limitations” section that much of the premium increase is probably due to older, sicker people signing up in 2017 vs. 2013. The analysis also fails to note that pre-ACA policies (Healthcare.gov went live in 2013) were often full of coverage loopholes, exclusions, lack of coverage for pre-existing conditions, and lack of insurer experience with an uncertain risk pool.
HIMSS complains about President Trump’s proposed federal budget that calls for major funding cuts for ONC, CDC, CMS, and NIH along with zero money for AHRQ, which would likely be rolled into NIH. The proposal also calls for cutting Medicaid by $800 billion over 10 years.
Other
A Spok survey of 100 hospital CIOs finds that 40 percent of hospitals don’t discipline staff members who violate mobile policies, 30 percent say a significant portion of hospital data is shared insecurely, and more than half of doctors and nurses are unhappy with the communications methods available outside their EHR. Forty-one percent of hospitals don’t offer secure texting and those that do are equally split between providing it via the personal devices of employees vs. hospital-issued technology. Nearly one-third of clinical staff can’t receive clinical alerts or mobile messages from colleagues. CIOs say their hospitals are still using pagers because they are appropriate for some groups, are reliable, and are cheap and easily supported. More than half of the respondents say their biggest challenge in protecting hospital data is a lack of money and people.
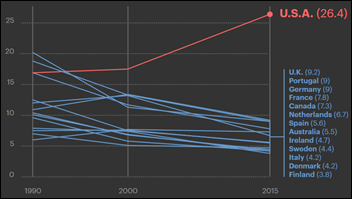
A ProPublica investigative piece observes that the still-increasing US maternal death rate is the highest in the developed world and 60 percent of those fatalities are preventable, profiling NICU nurse Lauren Bloomstein, who died of preeclampsia shortly after giving birth in which hospital medical errors apparently contributed. Factors include women giving birth later in life when their medical histories are complex, the nearly half of US pregnancies that are unplanned, the complications of C-sections, and the fragmented health/insurance system that makes it hard to get prenatal care (likely to get worse with any cutbacks to Medicaid, which pays for nearly half of US births). The article notes that perhaps the healthcare system is focused so much on saving the lives of babies – which it has done well – that it isn’t paying enough attention to the health of the mother. A standardized approach to quickly reacting to possible preeclampsia reduced UK maternal deaths to just two in three years, while up to 70 US mothers die of it annually even as US hospitals push back on implementing evidence-based processes.
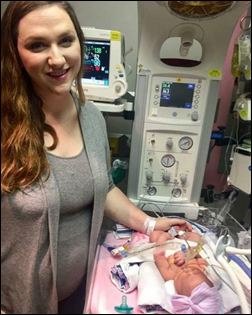
All you need to know about US health insurance is contained in this one story. An Army veteran whose wife requires pregnancy-related injections not covered by their medical insurance finds that they make $70 too much per month to quality for Medicaid, so they move from North Carolina to Alabama for a job that offers better insurance. He pays COBRA to cover the one-month lapse before their new insurance kicks in. The baby came in early, the NC insurance wouldn’t pay since Alabama is out of network, and the couple gets a bill for a two-week NICU stay for $178,000, of which neither insurance would pay a penny. They can’t get loans and he will lose his defense-related job if they file bankruptcy. They raised a few thousand dollars in a GoFundMe campaign and are hoping to work out a hospital payment plan for the balance that will probably last the rest of their lives.

Instead of the help desk tech term PEBCAK (problem exists between chair and keyboard), this was PEBCASW (steering wheel). In China, a car show model who is demonstrating Nissans’s emergency braking system by standing in front of the moving car is run over (with only minor injuries despite being thrown 10 feet) after the demo driver – who was not familiar with the system – pushes its button twice, turning it on and then off again.
Sponsor Updates

- Docent Health assembles bags and lunches for Boston-based charity Bridge Over Troubled Waters.
- The American Association of Critical Care Nurses chooses Kathy Douglas, RN, MHA, chief clinical officer of Abililty Network’s ShiftHound, for its Pioneering Spirit award.
- CSI Healthcare IT provides at-the-elbow support for MaineHealth’s Epic go-live.
- Besler Consulting releases a new podcast, “Lessons learned from the introduction of a physician incentive compensation plan.”
- CapsuleTech and Dimensional Insight will exhibit at the International MUSE Conference May 30-June 2 in Dallas.
- Spok executives will speak at several industry events.
- Direct Consulting Associates will exhibit at the SIIM Annual Meeting June 1-3 in Pittsburgh.
- The American College of Radiology – a National Decision Support Co. partner – wins the ABIM Foundation Creating Value Challenge for its Radiology-Teaches initiative.
Blog Posts
- Hiring the best executives and professionals, monetarily guaranteed to be retained for 1 to 2 years (Direct Consulting Associates)
- EHealth Partnership Unites Ontario Hospitals on MEDITECH (Video Series) (Meditech)
- Specialists Training Specialists (Optimum Healthcare IT)
- Interactive Patient Care Platforms (Sphere3)
- State of the Union Address (AdvancedMD)
- Impressions of a very busy Health IT Expo 2017 in Paris (Agfa Healthcare)
- A Day in the Life of “Death by a Thousand Clicks” (Arcadia Healthcare Solutions)
- Hybrid Cloud is Now the Preferred Option Within Healthcare (Datica)
- Have You Adopted Electronic Prescriptions for Controlled Substances? (Caradigm)
- Prescription Nonadherence: An Infographic (CareSync)
- Growing Pains: A Practical Approach to Managing Your Application Portfolio During Organizational EvolutionGrowing Pains: A Practical Approach to Managing Your Application Portfolio During Organizational Evolution (CTG)
- Healthcare On-Demand: An Experience with Epic MyChart (Culbert Healthcare Solutions)
- 3 Takeaways from the New England HIMSS Spring Conference (Dimensional Insight)
Sponsors named to Modern Healthcare’s “Best Places to Work in Healthcare” 2017 list:
- Cumberland Consulting Group
- Divurgent
- Encore, a Quintiles Company
- Hayes Management Consulting
- Healthfinch
- Impact Advisors
- Imprivata
- Nordic
- PMD
- Santa Rosa Consulting
- The Chartis Group
Contacts
Mr. H, Lorre, Jenn, Dr. Jayne, Lt. Dan.
More news: HIStalk Practice, HIStalk Connect.
Get HIStalk updates. Send news or rumors.
Contact us.








Re Vaporware: I don’t want to be rude, but where are you getting your information as it isn’t accurate on my experience. Cerner has been delivering on interoperability for a VERY long time, ,they have always been willing to build an interface into and from any system or EMR. As for Beth Israel Deaconess, i don’t recall that they ever even used Cerner Millennium. I believe that AthenaHealth actually bought their home-grown system and has been re-branding it. So where is Cerner even used there? Maybe the Lab if anywhere…
As for the Genesis project, Millennium is being interfaced to more than 40+ 3rd party systems and that was part of the original delay, building out those interfaces and standardizing the data, so to say when are they going to deliver..they have already delivered and dozens of hospitals and IDN’s.
With all do respect, I think you may be commenting due to a bad experience or perhaps allegiance to another EMR provider. I could not care less what EMR a hospital has, as I have worked on all of them (Cerner, Epic, Athena Health and Sorian). I don’t have an allegiance one way or another, but I want the truth to come out instead of speculation or “rumors”.
Now, on a larger scale, interoperability is subjective in a way. The Hospital Leadership has to want to integrate all of their systems, so to say that Cerner or Epic is bad at interoperability is not entirely true…What decisions were made when that EMR was implemented? You need to take that into consideration before saying “this system sucks or doesn’t talk to other systems”. That very well could have been a decision made by hospital leadership. Now, there are systems that are notorious for not playing well with others (eClinicalWorks I am looking at you).
I believe they were just referring to the BIDCO approved EHR list (athenaClinicals, Centricity, eClinicalWorks, Epic, NextGen, and WebOMR).
Interesting that you call out eClinicalWorks as a bad egg but they are in the group.
I, on the other hand, want to be a little bit rude.
Honestly, Vaporhead? Do you understand the sentences that are formed from the words you reference?
“Beth Israel Deaconess Care Organization includes nine hospitals and 2,600 physicians. To become a member of BIDCO, an organization must have a BIDCO-approved EHR, which include athenaClinicals, Centricity, eClinicalWorks, Epic, NextGen and WebOMR, which is a BIDCO-built EHR.”
Those six (granted, you CAN count) are the list of EHRs from which Beth Israel requires its BIDCO members to choose. It has absolutely nothing to do with being willing or able to spit out data to be used by an as-yet-not-live “platform for cloud-based real-time analytics with the goal of improving population health.”
Please take your disgruntled, Cerner-apparently-done-you-wrong trolling elsewhere. Better yet, spend your energy on common vocabularies, standard payload formats, or universal patient/provider health ID initiatives to help transform interoperability in the healthcare industry. Assuming you’re interested in making things better, of course…
C/E: No hard feelings on the rudeness. I got my info from the BIDCO article, but Mr. H. edited the link out. My sense from the article is that they’re talking about taking in info from OUTSIDE EMRs, not necessarily EMRs or other systems that Beth Israel purchased. Maybe someone from BIDCO could comment on ‘why no Cerner’? They surely have physician users in Boston.
Similarly, on Genesis, I was asking for the truth, so maybe we’re on the same team after all. That said, “building interfaces” to third-party systems within MHS isn’t what I’m asking about. Since you seem to have those facts … Can they get an outside CCD from a multi-vendor network? Are they live with CommonWell? Carequality? What organizations in their community are they exchanging with? What’s their volume?
Regarding hospital leadership’s role, I partly agree, but it would be hard to argue that BIDCO or MHS doesn’t care about interoperability. (FWIW, eClinical is on BIDCO’s “willing and able” list.)
Good Reader: Look like Mr. H. also edited by paraphrasing to “willing and able.” The words I read were from BIDCO’s CIO, Bill Gillis. Maybe your beef is with him:
“We only allow folks to come into BIDCO if they are on one of six EHR platforms with very robust data delivery mechanisms and are from vendors that are open and willing to work on interoperability so we can exchange information between those systems.”
If BIDCO has to pull teeth to get a CCD sent across town from Cerner-using docs, then Cerner had dun-a-lot-more-people-wrong than me.
C’mon, VapoRub, I read WELL, so there’s no reason to take issue with Gillis’ statements. Let’s break it down. One. More. Time. (Seriously… this is the last time I’ll respond.)
1. BIDCO requires the use of one of six EHRs.
2. Those EHRs have robust interop capabilities.
3. The vendors that supply those EHRs are willing to work with BIDCO.
4. Stop.
From that point forward, you’re inferring that means no other EHRs can meet the data submission requirements, no matter how hard BIDCO has slaved away at trying. It’s like hearing someone say “This SAAB has four wheels.” and concluding that, against all odds, Sweden produced the only car in the world with four wheels. Either you really did score 17 in the ACT Reading section (if so, I apologize) or you have an issue with Cerner.
Believing that the interop an organization utilizes is equivalent to what their EHR is capable of only demonstrates your ignorance of our industry. The healthcare organizations decide which interop functions they wish to utilize and when. For example, Commonwell, Document Exchange, Sharing CCDs with Patients, Directed Exchange, ePrescribing, Orders&Results Delivery, Immunization Registering, etc. are available to all Millennium implementations. It’s up to each organization to turn them on.
As an aside, they all seem to turn on Claims Submissions at go live. Priojrities, I guess.
MHS Genesis specific: Based on recent past history, do you actually believe the DoD is going to sign up for Commonwell on Day 1? This is their venture into commercial software territory, Vapes, they gotta crawl before they run. (It should be embarrassing to everyone in HCIT to think that the exchange of standardized documents is “running”, by the way.)
In working on the vendor side of things for a number of years with a number of different companies I think it is pretty evident what is happening with interop….
Almost every vendor at this point has “committed” to exchanging data. The realities are that most of these vendors are still in the process of trying to make this work..even with something as simple as exchanging a ccd across disparate systems. Some can do it with certain vendors and not others due to the fact that MOST software vendors have multiple versions creating the task of having to build out multiple connections/mappings.
Someone said it but the question to ask a vendor is how many live sites do you have sharing CCD’s/patient data, what is the volume of transaction, and what kind/format of data do you get. There are a few vendors right now doing very well with this simply because they have newer systems built with this in mind.
A lot of time a vendor in the community is favored simply because they have built an interface or connection to a large local care setting. Let’s say a major outpatient EMR vendor built a connection to the large epic shop down the road. That interop would work, and that vendor may be seen in the community as a leader in interop. End users essentially only know what functionality they have. The reality is that could potentially be the only connection in the entire country for sharing data between those two vendors, as it was built for a specific one off purpose…but end users don’t see that aggregate. Most just know whether they get data or not with their systems.
Long story short…every vendor is going to tell you they can connect and share info, and they all do in some capacity in some areas of the country, but no one has mastered it yet. Be sure to ask the questions around your specific care settings and communities!
Well Reader: In fairness, I consider BIDCO to be an open question, since they haven’t weighed in. Your answer is certainly plausible, but by my logic, not likely. It seems true, at face value, that BIDCO values gathering the data – so when the largest EMR company in the world isn’t on its list, it begs many questions. Does it cost too much? Is the data junk? Is it simply not adopted? Maybe BIDCO just forgot Cerner.
MHS, on the other hand, I would expect to get one of the “newer systems” that Sergeant F is describing and YES as a paying customer of this $9b bait & switch I expect it to go live on what was promised by the Cerner dog & pony crew. Why is it that BIDCO can get a record from athena, but MHS can’t? Can MHS or Cerner really defend Genesis going live WITHOUT CommonWell turned on? You’re kidding with that question, right? You can call it industry ignorance, but i call it vaporware.