I was born roughly 2 months after the US space program began (Explorer 1), and I've followed it all my…
Monday Morning Update 3/20/17
Top News
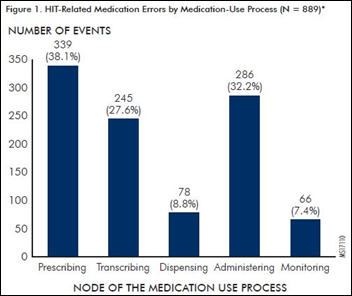
Pennsylvania’s mandatory medical error reporting — which requires submitters to indicate if health IT caused the event or contributed to it – shows an increasing number of HIT-related medication errors. Patients were harmed in eight incidents in the state during the first half of 2016.
Interestingly, the most common cause of dose omissions was system downtime, while the most frequent cause of wrong dosage errors being incorrectly entered patient weight, with one frightening example being a 46 kg patient whose Lovenox dose was calculated based on a mistyped weight of 146 kg.
In another example, a doctor ordered 65,610 mg of aspirin, explaining that she ignored the overdose warnings because she was just re-entering the home med (and in doing so, typed 810 tablets instead of 81 mg daily).
CPOE was involved in half of the incidents, with the pharmacy and eMAR systems each being tied to about one-fourth of incidents.
Reader Comments
From SkidMark: “Re: Epic. Continues its expansion into niche markets by partnering with Acumen Physician Solutions, which is part of Fresenius. Acumen offers a specialty EHR for nephrologists who round in dialysis clinics, but who also visit ESRD patients during their frequent hospital stays. What are the chances the Fresenius will also migrate its 2,500 dialysis clinics from Cerner Soarian to Epic’s legacy or emerging EHR for better integration with their nephrologists?” Fresenius announces that the next version of its Acumen EHR will be “Acumen 2.0 powered by Epic.” Fresenius chose Siemens Soarian in early 2005. It would seem to make sense that choosing Epic for nephrologists would improve the chances of replacing organization-wide Soarian with Epic rather than Millennium.
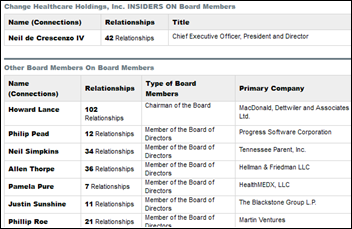
From McChange Pissed: “Re: Change Healthcare’s board of directors. What is McK thinking? They made one bad IT decision after another, starting with Pam Pure, and now she’s back?” Change Healthcare’s board includes Pam Pure, now CEO of HealthMEDX, but she has served on Change’s board since 2012, long before McKesson was involved (when it was Emdeon). Also on the board (for many years, too) is Phil Pead, who was CEO of Eclipsys and chairman of the Allscripts board following its acquisition of Eclipsys, but who later was fired in 2012 after clashing with CEO Glen Tullman, who was fired himself just a few months after. At least Change Healthcare’s management team includes three females among 12 executives (25 percent) vs. just one of eight board members (12.5 percent).
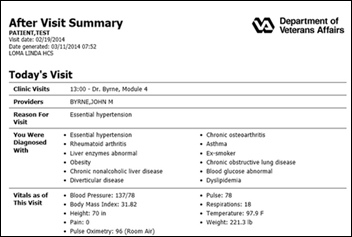
From Springy Insole: “Re: after-visit summary. Have you seen any organization that has a patient-friendly one? The ones I’ve seen are pretty unhelpful and improvements could make a world of difference.” I’ll open it up to readers to weigh in and hopefully provide examples. Those I’ve seen look like they were uncreatively designed by programmers. The above came from the VA’s Robert Durkin, MD, MS, just to give you a refresher of what we’re talking about. While I like the format, I might suggest these changes:
- Indicate which diagnoses were new vs. existing, or perhaps include a date for each diagnosis. In fact, a problem I see with a lot of AVS is that programmers proudly regurgitate everything they have on file about a patient along with boilerplate reference information from third-party products, creating a bulky document that makes it hard to figure out what’s new (a pervasive problem with EHRs in general).
- Don’t mix diagnoses with health indicators, i.e. “ex-smoker” is not a diagnosis.
- Don’t use medical jargon like “vitals.”
- Indicate either the percentile or the risk of each vital sign listed so the patient doesn’t have to figure out what a BMI of 32 means.
- What I would really like to see on all AVS printouts is a few sentences from the doctor that summarize what he or she found, what the patient should be doing, and what the goals are and when those goals will be reassessed. That should be the first set of items on the document, under the assumption that the patient won’t read all of it and thus should see that first. The purpose of an AVS isn’t to print out the information that already exists in the EHR, except of course in the case where lack of interoperability makes the patient the integration engine in handing it off to their next provider.
- It would also be nice to use the summary as some type of agreement between doctor and patient of how they will work together.
- In fact, maybe that’s my takeaway – the AVS should not be considered an efficient but poor substitute for doctor-patient communication. A pretty printout is fine for a Jiffy Lube oil change summary, but a slam-bam medical encounter that results in a handed-over sheet of paper while discouraging patients to ask questions or seek follow-up isn’t ideal. A doctor visit often reminds me of a church confessional – the parishioner quickly states his or her issues and is sent away equally quickly formulated instructions — except that in medicine’s case, the church only offers the confessional while omitting the other important aspects of the church that might have prevented the need for confession in the first place.
HIStalk Announcements and Requests
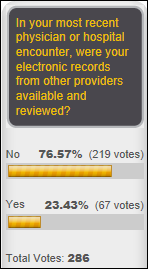
I’ll take the glass-half-full viewpoint in celebrating the fact that 25 percent of poll respondents were able to view their records from other providers in their most recent encounter. Clarence is frustrated that his providers all use Epic, but even as a former Epic employee, he can’t convince the clinicians that they can actually retrieve his information from other sites. Greg’s specialist could access his chart and test results, but he had to tell them he’d had new tests. Brittney was impressed that her urgent care clinic records were not only automatically placed into her PCP chart, but that the doctor even asked about the outcome. Susan says we all need to educate patients and support consumer-mediated health exchange because they don’t realize that we aren’t already exchanging information.
New poll to your right or here: what was your patient portal experience from your most recent provider visit?


Mrs. H in Michigan exclaims, “This is amazing!” in describing how her students are using the listening center we provided in funding her DonorsChoose project. She says they listen to stories every day, write about what they heard, share their thoughts with classmates, and then take the physical book home to read on their own.
This Week in Health IT History
One year ago:
- Apple announces the CareKit developer framework for creating iPhone health apps.
- McKesson announces that it will take a $300 million restructuring charge and lay off 1,600 employees.
- NYC Health + Hospitals President and CEO Ram Raju, MD defends the organization’s Epic go-live date and says a CMIO who quit over the patient safety implications is a disgruntled former employee.
- Several hospitals are hit by ransomware.
- Allscripts and a private equity firm acquire post-acute care EHR vendor Netsmart for $950 million.
- New York’s e-prescribing mandate takes effect.
Five years ago:
- Memorial Sloan-Kettering Cancer Center and IBM announce their collaboration to use IBM Watson for oncology decision support.
- Vocera prices its IPO shares.
- Thomson Reuters puts its healthcare data and analytics business back on the market.
- Cerner breaks ground on its new campus at State Avenue and Village West Parkway.
- HHS launches a developer challenge to use Twitter for real-time public health tracking.
Weekly Anonymous Reader Question
Last week I asked readers to describe the dumbest EHR design flaw they’ve seen recently. I’m omitting vendor names since the point was to show the need for improvement as an industry.
- Click on Labs and there’s a New button, but that means to add a new historical lab – you can’t actually order from there.
- It’s impossible to add reference ranges for in-house labs.
- Free-text drug allergy entry is allowed and users do it all the time despite threats to their unborn children.
- The end user can click one wrong button and delete a global template that cannot be recovered.
- Storage of multiple instances of physiologic variables in different parts of the same database – a heart rate entered by a nurse goes one place, one entered by an allied health provider goes into another data element. When reporting on heart rate, which one does one access?
- Cannot store/send more than one ID for an individual patient visit, which is horrendously inadequate for trying to do conversions, file billing data, and file incoming patient data from another system.
- Approving med refill requests makes no entry in the EHR.
- Half of the home screen is taken up with notifications that list only a category and number. I have to open each one and there may be 10-15 at any time. I just want a list, maybe grouped by category, so I can see them at a glance.
- Can’t put isolation status in the patient header.
- The medication ordering drop-down sorts as strings instead of integers, so doses are listed as 1, 10, 2, 20, etc. How easy is it to generate an order for 10 mg of warfarin instead of 1 mg? Easy enough to be very glad a pharmacist caught the mistake before “the computer” killed someone with massive internal bleeding.
- Does not have a unique identifier to send for bi-directional data flow.
- The lack of design generosity for analysts blows my mind. It’s appallingly easy to hit a key and overwrite something – there’s no way to know what had been there, no undo button, and no way to close a record without saving.
- Our appointment reminder system can send only the patient’s scheduled start time, ensuring that we will run behind schedule. Is it so hard for the system to subtract 10 minutes for follow-up patients and 20 for new patients to calculate the arrival time?
- Tiny icons that can’t be enlarged.
- Scanning in individual TIFF files.
- Two of our systems can’t handle the Daylight Saving Time change in the fall and must be shut down for an hour.
- If you click X next to a patient name when entering documentation, there’s no “do you want to save your work” warning like every single other piece of software in existence.
- When discharging an ED patient, I select instructions, discharge meds, follow-up doctor, and instructions. Back on the discharge screen, the Print button prints an instruction with none of the above listed. I have to jump to another part of the application and reload the page. I’ve had patients leave the hospital without the information and we had to deliver it to them. The vendor’s “reload after selecting” workaround has been in place for 2.5 years.
- The provider master file should be its own app with a cert and minimum staffing recommendation.
- A vendor demonstrated their new enterprise system to a large hospital group and discharged the pregnant male demo patient. The risk manager pointed out the flaw.
- A well-known EHR does not port a female patient’s gyn history into the OB episode when she becomes pregnant, requiring employees to re-document the entire history.
- The vendor sets up two direct messaging solutions, one that’s DirectTrust accredited and one that isn’t. As a result, not all users can exchange messages with other accredited HISPs and they may not know if they are on the “right” HISP.
- If an external user sends a Direct message with a C-CDA and PDF, the HISP drops the PDF attachments because the vendor doesn’t support receiving them. Plenty of EHRs have the same problem, but the killer is that there’s no notice back to the sender that only part of their message was delivered.
- No sandbox for hospital users.
This week’s question, just to lighten things up a bit: What’s the most hilariously clueless one-sentence statement you’ve heard an executive of your organization make?
Last Week’s Most Interesting News
- A GAO report says HHS should question why so many providers say they offer patients access to their electronic information, yet few patients review it.
- Mayo Clinic says its decreasing margins force it to give appointment priority to patients covered by private insurance rather than Medicare and Medicaid.
- ECRI’s #1 patient safety concern for 2017 is EHR information management.
- A House bill would allow employers to require employees to undergo genetic testing and to share their results to earn health insurance premium discounts in corporate wellness programs.
Webinars
March 29 (Wednesday) 1:00 ET. “Improving patient outcomes with smartphones: UW Medicine Valley Medical Center’s story.” Sponsored by Voalte. Presenters: James Jones, MBA, MSN, VP of patient care services and nursing operations, UW Medicine Valley Medical Center; Wayne Manuel, MBA, SVP of strategic services, UW Medicine Valley Medical Center. UW Medicine Valley Medical Center dramatically improved patient outcomes after moving to a smartphone-based platform for clinical communication and alarm and alert notification. Before-and-after analysis shows a reduction in hospital-acquired pressure ulcers and skin integrity events, fall and slip events, and medication errors. By limiting overhead paging, the medical center also created a calmer, quieter environment and improved engagement among nursing and hospitalists. Hospital executives will describe their experience and vision for the future in addressing quality, cost, and the patient-caregiver experience.
Previous webinars are on our YouTube channel. Contact Lorre for information on webinar services.
Decisions
- Henry Ford Allegiance Health (MI) will go live with Epic in August 2017.
- Columbus Regional Healthcare System (GA) switched ERP systems from Infor to Sage in January 2017.
- Bon Secours St. Francis Hospital (SC) moved from McKesson to Cerner in October 2016.
These provider-reported updates are provided by Definitive Healthcare, which offers powerful intelligence on hospitals, physicians, and healthcare providers.
People

The Missouri Health Connection HIE promotes Angie Bass, MHA to president and CEO. I believe she’s the fourth CEO since the organization was founded in 2012.
Privacy and Security
Children’s Hospital of Eastern Ontario notifies 283 people that the medical information of their children was used in a college class taught by one of its employees, who handed out a surgery schedule will full patient information for an in-class exercise.
Houston Methodist Cancer Center notifies 1,400 patients that their email addresses were exposed when an employee used CC: rather than BCC: for a mass email.
A North Carolina radiation oncologist and medical school professor is arrested for issuing fraudulent narcotics prescriptions. Adding insult to injury, State Bureau of Investigation officials who raided his home also arrested his son when they examined his computer and found child pornography. That should create some awkward “remember that day” family conversations.
A Texas woman files a complaint with the state’s medical board and notifies HHS after she says a doctor who performed a “non-surgical tummy tuck” that she complained about on Facebook, after which the doctor allegedly posted near-naked pre-surgical photos and video of her on Facebook and YouTube. The patient claims that Tinuade Olusegun-Gbadehan, MD then threatened her by emailing a link to the video and a message that said, “This video result, when posted as a response to your next slanderous comment about the Dr. O Lift on social media, will be just as damaging to YOUR professional reputation.”
Other
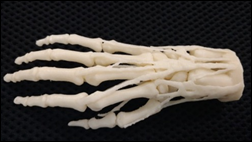
Five VA hospitals create the country’s first 3-D printing network, allowing doctors to design and build prosthetic and orthotic devices as well as to construct anatomic models for study and surgery practice.
A high-profile cardiothoracic surgeon sues Memorial Hermann (TX), which he claims manipulated outcomes data to discredit him after he threatened to move to competitor Houston Methodist Hospital. The doctor – who had served as chair of both the surgery and cardiovascular departments of Memorial Hermann — says Memorial Hermann ordered him to perform surgeries only under the supervision of another surgeon and then presented the information to a roomful of colleagues to smear his reputation even though the underlying data was flawed. “I was coming between administrators and market share,” he concludes, saying he left because Memorial Hermann’s cost-cutting measures were compromising patient care. The hospital stands by its peer review process that uses data from the Society of Thoracic Surgeons.
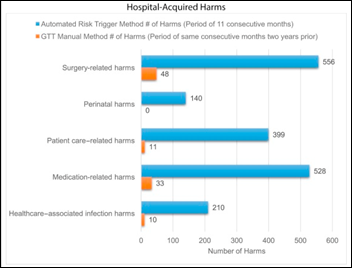
Adventist Health System’s automated, real-time patient harm trigger system – which attempts to identify patient safety issues by reviewing events such as the ordering drugs that might indicate treatment of unreported patient harm – captures a lot more incidents than manual review. The most frequent harms in order of severity were medication-related hypoglycemia, C. diff infection, medication-related bleeding, venous thromboembolism, and post-surgical respiratory complication. The most dramatic increase was for pressure ulcers, which were detected 112 times by the trigger system vs. 0 as previously reported to the PSI 90 regulatory program.
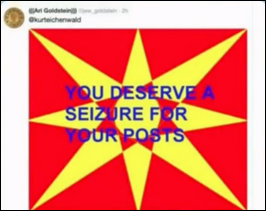
The FBI charges a man with cyberstalking after he uses Twitter to induce an epileptic seizure in a magazine editor who had written articles critical of President Trump. 29-year-old John Rivello knew that Kurt Eichenwald suffers from epileptic seizures and tweeted him a strobe-like animated GIF with a message, “You deserve a seizure for your post.” Eichenwald had an immediate seizure that left him incapacitated for several days and has since received similar animations from 40 other seriously disturbed Twitter users.
Bizarrely sad: a man plugs his iPhone charger into an extension cord and takes the phone into the bathtub with him, with the resulting water contact electrocuting him. The coroner says he will ask Apple to warn phone-addicted people that bringing a plugged-in phone into the bathtub is little different from using a hairdryer there. The man had plugged the extension cord into a hall outlet, which makes me think that he might still be alive had he instead chosen a GFI-protected bathroom jack. Or, if his bathroom indeed had GFI, whether his bypassing of it was perhaps intentional.

Miami authorities try to build a case against a porn star who also operated a cosmetic center where a woman died in 2013 after a botched butt lift procedure. Vanessa Luna (her professional name, which is subtly clever if intentional since her trademark feature is her posterior and thus a “moon” reference is sly) says her clinic just sold Herbalife and cosmetics, but several witnesses say she oversaw illegal cosmetic surgeries performed there. Ms. Luna says she ran Facebook ads for plastic surgery and sold the resulting referrals to reputable doctors, but didn’t do any procedures herself. It wouldn’t be a South Florida story without Medicare fraud, for which the patient had served prison time.
Sponsor Updates
- Versus Technology will exhibit at AMGA March 22-25 in Grapevine, TX.
- Huron recognizes employee performance with 10 senior-level promotions.
- ZeOmega releases the latest edition of its ZeExchange newsletter
Blog Posts
- Busting myths about clinical claim review (Verscend)
- Real World Success Stories in Enterprise Imaging – Case #1: Pediatric Aneurysm (Visage Imaging)
- What We Learned at HIMSS17: Exploring Japanese Heritage and the Impact on Health IT (Vital Images)
- Scalability is the secret sauce. (Voalte)
- What’s Happening with Value-based Reimbursement in 2017 (ZirMed)
Contacts
Mr. H, Lorre, Jennifer, Dr. Jayne, Lt. Dan.
More news: HIStalk Practice, HIStalk Connect.
Get HIStalk updates. Send news or rumors.
Contact us.









The FBI charges a man with cyberstalking after he uses Twitter to induce an epileptic seizure.
This is serious stuff–a felony–attempted murder. Seizures can kill. I hope they lock the bastard up.
Re: NC two for one arrests. I wonder if Hallmark will come up with a line of greeting cards for their future get-togethers?
“Cannot store/send more than one ID for an individual patient visit, which is horrendously inadequate for trying to do conversions, file billing data, and file incoming patient data from another system.”
I don’t see that as a bad thing necessarily. It’s a design decision. Once you know there is one “true” ID, you can rely on it. Make sure you still have the ability to merge if the same patient got in more than once. All the data should file into the same patient. What if you have different providers coincidentally using the same ID for different patients?
“Our appointment reminder system can send only the patient’s scheduled start time, ensuring that we will run behind schedule. Is it so hard for the system to subtract 10 minutes for follow-up patients and 20 for new patients to calculate the arrival time?”
That seems more like a flaw with your process than the system. Sort of like people who set their watches 10 minutes ahead. Just stick to the true time and fix your process. Don’t make your patients show up 30 minutes ahead of schedule and proceed to wait for 45 minutes when they have nothing to do there.
Reading all these EHR design flaws makes me twitchy. I spent a fair amount of the last 10 years designing and supporting EHRs (I even submitted one of the items in the list, and have plenty more where that came from!) The pressure put on Product Development to turn out new features, open new markets, etc. is intense, and its all done at the cost of fixing bugs, cleaning up design, and making changes which are small and easy to do as individual units of work but which would add up to an entire release’s worth of content. For my money? I’d take four months of a “no growth” development cycle to fix them and get rid of the irritants which are “low value” but which really cause doctors and nurses to loathe EHR (which can and should be a seamless experience). I lost a lot of sleep, and even wound up with severe TMJ from grinding my teeth requiring me to puree all of my food for a month, from the stress of being caught between doing what was right by my doctors and nurses — and therefore doing right by their patients — and doing what my director, VP, and CEO said I had to do (or, presumably, lose my job.)
I’m in another line of (HIT-related) work now and while I miss my doctors and nurses terribly (I really, really loved working with them — even the crabby ones) I don’t miss the anxiety of knowing what needs to be fixed and being explicitly told *in writing* that we’re not going to fix it.
I’ll tell everyone what I told my parents years ago:
“To the extent that software does not meet human needs, it will be changed until it does.”
Yes, I know that can take a long time. I’ve been there, marooned on legacy software that isn’t changing, and seeing no hope or timeline for improvement. Never give up!
Change will come. If the legacy vendors of legacy systems are dragging their feet, they will adapt or die. If the problem is governmental regulation, eventually that regulation will change. If the issue is clinicians not engaging with the change process, eventually those clinicians will engage, retire, or be replaced. If the issue is programmers and analysts falling short in some way, eventually they will improve, move on or be fired.
Software is mutable and the customers dollars speak volumes. Unsatisfactory software cannot last forever.
“The lack of design generosity for analysts blows my mind. It’s appallingly easy to hit a key and overwrite something – there’s no way to know what had been there, no undo button, and no way to close a record without saving.”
Oh, that’s Chronicles for sure…
I sometimes hope (as HIT Girl does) for a “no new features” type of release that focuses mainly on making configuration and administration of the EHR easier for project teams. Apple did something similar with 10.6 and it’s always been a well-regarded move.
Epic is actually in this mode right now in that they’re focused on usability. Hard to imagine the publicly traded competitors following suite…