Thomas told me when he submitted his article that it was OK if I didn't run it because people generally…
News 3/17/17
Top News
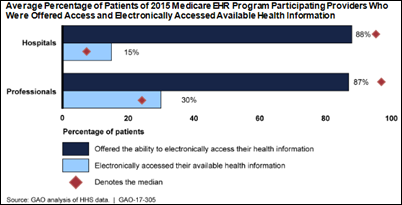
A GAO report says HHS should investigate why few patients access their electronic medical information even though 90+ percent of hospitals and practices claim to offer such access.
The report suggests that patient portals are the most common method by which patients look up their information, most commonly that of the provider’s EHR vendor. The report notes the limitations of portals:
- Patients must often use multiple portals for their multiple providers, meaning they have to go through the sometimes laborious setup more than once and maintain multiple sets of login credentials.
- Longitudinal data across providers isn’t available.
- User interface design is often poor.
- Each provider’s portal may be set up to display a subset of the available information that may be inconsistent, such as one portal showing prescriptions and another not.
- New information is not always available consistently, such as recent lab results that may not be posted every time depending on which lab processed the sample.
- Portals don’t usually display historical vital signs and weights that the patient could use for trending.
The percentage of patients who review their health information varied widely depending on which EHR the organization used. Of the top 10 vendors (which were not named in the report), the percentage of patients who reviewed their information ranged from 10 percent to 48 percent.
The report suggests that providers provide portal brochures, promote the portal during each interaction, make computers available in the hospital or practice, send reminder emails, reward clinical staff, or offer patients prizes or discounts for using the portal.
Reader Comments
From Inquiring Mind: “Re: Soffet. We’re converting to Cerner Patient Accounting and the reference site mentioned a product called Cerner Charge Integrity from Soffet. We’ve searched HIStalk and haven’t found it. Where can I find this mythical company and product?” Some pretty impressive Googling (if I do say so myself) turned up Softek Solutions, which offers EHR performance and revenue integrity solutions for Cerner sites.
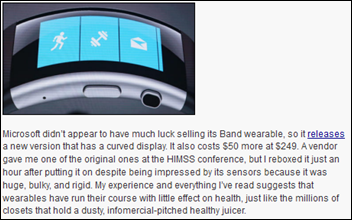
From Shoulda Shorted: “Re: fitness trackers. You wrote in 2015 that fitness trackers had run their course. I sent that comment to my broker when Fitbit was trading at $35, but I should have also shorted shares – they are now at $6.” I also now see that Microsoft has killed off its poorly designed Band tracker that I had panned after trying it, with its demise going unnoticed due to indifference. My take today: the only fitness tracker that will ever be consistently used will be built into your phone, with any required sensors being effortless and invisible. Nobody wants to wander around like Dick Tracy with a big old gadget on their wrist or risk embarrassment after missing a fad shift in still wearing one of those once-ubiquitous but now-defunct Livestrong yellow rubber bands. My weekend poll might ask how many trackers you’ve owned and whether you still use one (my early 2014 survey found that 37 percent of respondents claimed to use their tracker at least five days per week, “use” being loosely defined). The early-market churn as companies rushed supposedly improved products to market and convinced consumers to change brands created the illusion of ongoing demand, but there’s only so much to be gain health-wise by counting steps and most Americans don’t really want to take a lot of steps anyway. At least you can hang clothes from unused treadmills.
HIStalk Announcements and Requests


Readers funded the DonorsChoose grant request of Ms. H in Indiana, whose seventh graders are using the scientific calculators we provided to perform complex experiments in calculating the volume of cylinders using popcorn.

Lorre’s post-HIMSS specials for new sponsors of the site and of webinars ends when March does, so interested companies have a couple of weeks to speak up before we slack off during those lazy, hazy, crazy days of summer.
I was reading a questionably authoritative article that proclaimed that data centers will be obsolete within five years because of the cloud. I think they missed the fact that data centers aren’t going away – they’re just being centralized. What has changed is ownership and the length of the cord attaching the end user. As I often say, the cloud is just someone else’s computer, although that’s a flip response if a vendor really offers a “cloud” – a pool of interchangeable, commodity servers that are physically touched only when installed and discarded and that are managed collectively, spun up quickly via software, scalable, and are sold as a metered service. It would be interesting to know which health IT vendors are truly operating in this type of cloud vs. just parking the same old server in their own building instead of one owned by the customer. And speaking of Dilbert (which I wasn’t, except to include the strip above), Scott Adams is putting together a list of startups that could lower healthcare costs and is seeking submissions in case you work for one of those.
Listening: new from Norway-based but American-sounding Beachheads, jangly, hook-laden power pop that defies your toes to stop tapping even with a pleasant soupcon of the punkish minor chords that I require.
This week on HIStalk Practice: CaptureRx expands, relocates in San Antonio. Southwest Behavioral & Health Services implements EnSoftek IT. Compulink develops EHR for pain medicine providers. Primaria Health launches ACO in Central Indiana. Ingenious Med CEO Joe Marabito calls out lack of vendor support for physicians. Price, Verma reassure governors of their commitment to Medicaid. MGMA takes CMS to task for lack of 2017 MIPS eligibility information.
Webinars
March 29 (Wednesday) 1:00 ET. “Improving patient outcomes with smartphones: UW Medicine Valley Medical Center’s story.” Sponsored by Voalte. Presenters: James Jones, MBA, MSN, VP of patient care services and nursing operations, UW Medicine Valley Medical Center; Wayne Manuel, MBA, SVP of strategic services, UW Medicine Valley Medical Center. UW Medicine Valley Medical Center dramatically improved patient outcomes after moving to a smartphone-based platform for clinical communication and alarm and alert notification. Before-and-after analysis shows a reduction in hospital-acquired pressure ulcers and skin integrity events, fall and slip events, and medication errors. By limiting overhead paging, the medical center also created a calmer, quieter environment and improved engagement among nursing and hospitalists. Hospital executives will describe their experience and vision for the future in addressing quality, cost, and the patient-caregiver experience.
Previous webinars are on our YouTube channel. Contact Lorre for information on webinar services.
Acquisitions, Funding, Business, and Stock
CareDox, which offers a free EHR for K-12 public schools, raises $6.4 million in a Series A funding round, increasing its total to $13.5 million. The company is vague about how it makes money, but it appears to sell de-identified student information and to send care reminder-type advertising messages to parents.
First Databank acquires Polyglot Systems, which offers the Meducation patient medication instructions product line.
FDA-approved EKG app vendor AliveCor raises $30 million to add AI-powered EKG analysis to its service.
Livongo Health, the diabetes monitoring and coaching company led by former Allscripts CEO Glen Tullman, raises $52 million in a Series D round, increasing its total to $143 million.
McKesson is rumored to be selling its San Francisco headquarters building for $300 million. The company previously announced plans to sell and then lease back the 38-story building.
Sales
Hawaii’s leading health plan HMSA selects Sharecare’s consumer health and messaging platform for a statewide rollout and also makes an unspecified investment in the company, started in 2010 by WebMD founder Jeff Arnold and TV’s Dr. Oz. Sharecare acquired the population health business of Healthways in July 2016.
Mount Sinai Health System (NY) will use Salesforce Health Cloud to coordinate and manage care of Medicaid Performing Provider System.
People


Influence Health hires Dave Morgan (Recondo Technology) as CFO and Rupen Patel (NCR) as CTO.

Former Acting CMS Administrator Andy Slavitt (and our HIStalk Industry Figure of the Year) joins the Bipartisan Policy Center as senior advisor.
Announcements and Implementations
Mayo Clinic says that its tighter margins have forced it to start giving appointment priority to privately insured patients over those covered by Medicare and Medicaid. Mayo had a $475 million profit in 2016. What’s most surprising is that Mayo announced publicly what most health systems do privately – market to those with private insurance and, all things being equal, give them smoother passage through the system without affecting clinical outcomes. Perhaps there’s a market for a targeted patient dissatisfaction program to keep the low-paying customers away without actually banning them.
IBM Watson Health licenses AI-powered medical imaging analysis software from Israel-based MedyMatch Technology, which IBM will offer to EDs for assessing patients with suspected head trauma or stroke.
Government and Politics

The White House’s budget proposal, which would cut NIH funding by 19 percent, would also move HHS’s AHRQ into the National Institutes of Health.
Privacy and Security
A phishing employee awareness test by BayCare Health System (FL) creates headaches for the tax collector’s office when appropriately wary workers call to verify the phony government-looking email. The health system expected unsuspecting employees to click on links as the email instructed, which would have automatically presented them with a lesson on why their actions were inappropriate.
Other
A second Dallas death is attributed to a “ghost call” problem in which 911 callers can’t get through because the lines are overloaded by calls from T-Mobile cell users who didn’t actually dial 911. The Dallas-only problem seems happen when someone completes a 911 call, then sometime later the cell service thinks the call didn’t go through and tries again. The city admits that a six-month-old died while his babysitter was on hold with 911 for 30 minutes last week, with records indicating that 360 callers were waiting on hold at one point in the day.
A federal judge dismisses a lawsuit brought against Amtrak by Temple University Hospital that demanded payment of $1.63 million for treating a passenger injured in a May 2015 derailment. The passenger was covered by Medicare but the hospital didn’t submit its claim in time to collect the $269,000 that Medicare would have paid.
I mentioned last time that a new app measures the percentage of time men vs. women speak in a meeting, but here’s one I like better. Woman Interrupted allows measurement of “manterruption,” when a male interrupts a female who is speaking. I’m sympathetic since there’s nothing that drives me crazier (and often into pouty silence) than when someone of either gender repeatedly interrupts me, either in a one-to-one or group setting. It’s usually one of two extreme personality types: (a) an egotist (often the highest-ranking person in a meeting) who thinks they possess super-human insight into what needs to be said; or (b) someone so lacking in self-confidence that they have to talk over someone else to feel validated. I’m pretty sure those interrupters hate being interrupted themselves (since everybody does), so I always wonder if I should just say, “I’m going to leave now since you’ve turned our dialog into monolog and thus rendered my presence superfluous.” For the app, I suggest a Nuance-powered enterprise version that maintains speech profiles on every employee so it can provide a meeting recap indicating: (a) how much time each person talked; (b) how many times they interrupted someone or were interrupted themselves; and (c) who the primary interrupters are on the rudeness leaderboard. Perhaps it could also record which ideas each person argued for or against and then reconvene the groups six months later to see whose thoughts most closely aligned with the eventual reality and then automatically remove the chatty but wrong ones from future invitations.
Sponsor Updates
- Billings Clinic Hospital (MO) goes live with Versus Wi-Fi RTLS asset tracking.
- InterSystems posts its HIMSS17 presentation by Mental Health Center of Denver VP & CIO Wesley Williams, MD.
- Intelligent Medical Objects, Kyruus, Meditech, and PerfectServe will exhibit at AMGA 2017 March 22-25 in Grapevine, TX.
- Liaison Technologies will exhibit at the SCOPE Spring Conference March 19-21 in Atlanta.
- LifeImage publishes a new primer, “Image Sharing: Is It Missing From Your Enterprise Imaging Strategy?”
- Gartner names LogicWorks a leader in its 2017 Magic Quadrant for Public Cloud Infrastructure Managed Services Providers.
- MedData and The SSI Group will exhibit at the HFMA Texas State Conference March 26-29 in Austin.
- Netsmart will exhibit at the NAPHS Annual Meeting March 20 in Washington, DC.
- News: NTT Data awarded contract by the CDC
- NVoq will exhibit at the ACC Annual Scientific Session & Expo March 17-19 in Washington, DC.
- Experian Health will exhibit at HFMA KY March 30-31 in Lexington.
- Reaction facilitates a study on the ways in which independent physician referrals represent millions of dollars in revenue for hospitals.
- Harris Healthcare will exhibit at the NYONEL Annual Meeting March 19-21 in Tarrytown, NY.
- Sagacious Consultants releases the latest edition of Sagacious Pulse.
- Sunquest will exhibit at ACMG 2017 March 22-24 in Phoenix.
- Surescripts will exhibit at the Patient Adherence and Engagement Summit March 21-22 in Philadelphia.
- Sutherland Healthcare Solutions releases a new case study featuring Palomar Health, “Turning ICD-10’s Transition from Anticipated Calamity into a Resounding Success.”
Blog Posts
- How Analytics Can Help in a Value-Based World (Dimensional Insight)
- #JointheConversation on Analytics (Experian Health)
- AIDS Resource Center of Wisconsin – Making a Difference in HIV Outcomes (Forward Health Group)
- Why Aren’t You Leveraging Analytics? (Optimum Healthcare IT)
- Real World Success Stories in Enterprise Imaging | Case #1: Pediatric Aneurysm (Visage Imaging)
- Technology Evaluation Tools for a Complex Hospital Acquisition Process (Sphere3)
- Epic Workqueues and Revenue Cycle (Impact Advisors)
- What’s in Your Tech Stack? (Influence Health)
- CNO conversation #1: How do you handle overtime? (Infor)
- Certificationology: The Art of Making Healthcare Payment Security Decisions as Conspicuously as You Choose Your March Madness Bracket (InstaMed)
- Key Pharma Industry Trends to Watch for in 2017 (Liaison Technologies)
- Are You Ready for the CMS Emergency Preparedness Final Rule? (Live Process)
- How to Migrate to AWS in 30 Days (Logicworks)
- The Early Bird Gets the Bundled Payment Program Worm (Medecision)
- EHR “Go Live” Isn’t the End … It’s Just the Beginning (Netsmart)
- The Benefits and Challenges of Staff Augmentation (Parallon Technology Solutions)
- Too Big to Succeed? (CloudWave)
- Is the EHR a secret weapon for success under risk? We think so. (Advisory Board)
- Putting the “Long” in Long-Term EHR Training (PatientKeeper)
- The Path Forward for Enterprise Imaging (Lexmark Healthcare)
- How Pharmaceutical Companies Could be Affected by the AMA’s Prior Authorization and Utilization Management Reform Proposal (Point-of-Care Partners)
- Marking One Year of Success in Financial Services and Healthcare (Salesforce)
- Why It’s OK to be a Dinosaur in Patient Communication (Solutionreach)
- The Growing Need for Notifications (Summit Healthcare)
- How to grow capacity and tame complexity in the genetics lab (Sunquest)
- Using Actionable Intelligence to Improve Patient Safety (Surescripts)
Contacts
Mr. H, Lorre, Jennifer, Dr. Jayne, Lt. Dan.
More news: HIStalk Practice, HIStalk Connect.
Get HIStalk updates. Send news or rumors.
Contact us.








I hate interrupting people but have poor sense of when the other person is done.
… Or maybe we don’t look at out patient portals because after we get done with our care, we’d prefer not to think about it any more. One might say, “Who wants to sit around looking at lab values and diagnoses? Isn’t it the doctor’s job to figure it out and give us good advice?”
RE: A GAO report that says HHS should investigate why few patients access their electronic medical information. May I add my two cents?
I have a handful of doctors across different health care organizations and settings, ranging from small private physician practice to large academic institutions. I recall seeing one doc who did not use the EHR (Allscripts) in the exam room. So when I checked out and was handed the Clinical Summary for that day’s visit, it had nothing documented that was of any interest to me, just the day’s VS, Meds, etc. What I wanted from the visit was the ‘meat’ of the provider’s exam, assessment, evaluation and recommendation. Perhaps, if I remembered to request that summary 3-4 days later, the ‘meat’ would have been included, but by then, I’m on to the rest of my life.
My PCP is part of an academic institution now using Epic. I can download my records from their portal, but this too does not contain useful info for me. I can relate to all those physicians who receive a consult report with nine pages of not very useful information.
And finally, I have another provider who does not use a portal at all, so unless I fill out a release of info following the visit, I get nothing.
Perhaps HHS should convene a focus group of patients who can share what information THEY would be interested in receiving????
Saying that the Cloud is just someone else’s computer is like saying “There is no such thing as the grid, it’s just someone else’s generator.” While technically true, it ignores the efficiencies, distribution, redundancy and ubiquity afforded by the electricity grid.
Agree 100% The big reason cloud isn’t someone else computer is how the cloud is typically managed. If you take your current infrastructure physical-to-virtual all the servers and put them in the cloud you’re effectively just on someone else’s computer.
However, if you leverage say Google’s App Engine or any number of AWS services that provide substantial redundancy and scale ability the whole picture around cloud changes. For example, a modern designed SaaS offering has almost no limit to the amount of data (e.g. the limit is so far beyond what a hospital would actually use it effectively has no limit) it can handle in comparison to a hosted EHR. The challenge is most cloud initiative are just physical-to-virtualing their infrastructure which results in only a small amount of savings and benefit.
The comparison of switching from generating your own electricity to plugging into the grid is very real. I have a server setup that would have cost atleast $50K and likely required 1-2 FTE to maintain that has cost a total of $100 and no FTE in Google’s cloud. It’s a game changer, but the challenge is it will also eliminate whole department at any major hospital system so it will take forever for them to realize those savings.
The answer to “why don’t patients access their medical records” seems really obvious to me — we don’t need to. I have no particular interest in looking up my cholesterol levels from two years ago, or the visit note from the podiatrist I visited in January. Unless I have a specific need for specific data, what possible “in the realm of normal” reason would I I have for looking up my medical data? If I’m tracking something my “wellness” (*gag*) I’m probably doing it using some fun little gamified phone app that gives me stickers when I exercise three days in a row.
That aspect of MU certification always irked me and I agree with the physicians (my clients) who were equally annoyed by it, calling it “social engineering” that they are inexplicably on the hook for. Looking up historical medical records is not part of our daily life, and there’s no reason for it to be.
Regarding accessing medical records via a portal; obviously the current respondents do not have a critical disease where this information is very very helpful to understand my current status.
Having Stage 4 cancer means that there are a lot of tests and procedures that are completed and access to the outcome/findings is most helpful to me. And yes, I look at lab results that are 2 years old; I find it very helpful to be able to track my progress. I look and re-look at many of the results and will continue as long as I can.
My frustration is with health systems that have multiple applications which means multiple portals. This requires a lot of set up work to get access and many times I am unable to locate anyone who can help me.
If you are in good health, I understand that you would not access your medical information since there may not be any information that would help you. If you are in good health, please consider patients who are not prior to responding to this.
RE: BayCare Phishing – We have had similar backfires on phishing tests that were (luckily) only focused internal to the organization. My best guess is that these types of tests come en masse and alert staff. I’m hoping to find a way to send e-mails in a “trickle” attack and avoid any major alarms from sounding. However, it should be a best practice to not involve any external agencies in the fake scam, especially those that are unaware.
Portal mess.
Yet another fine example of the so called “leaders” at ONC that have no idea what they are doing. Its always, “doesn’t this sound good” with no evidence of success, trials, burden, cost or any knowledge of how care is actually delivered. Its pathetic. Asking EVERY MD to have a portal, all with different logins, different interfaces, and different outputs, is just plain idiotic.
Then after mandating that MDs are somehow responsible to have a % of their patients to use them, download info, or send secure messages at some rate, its also ridiculous. Forced policy markets NEVER work. But apparently these arrogant leaders at ONC/CMS feel they know better. Its always buzzword care, “sounds good” policy. Never a thought about actual costs, burden, outcome or even evidence that there is any possibility of improvement. There has been some minor “talk” about cost and burden, but no action. It seems that the regs are still piling on, more complex and more costly and more burdensome than ever. We need a REAL front line MD leader, not sycophants like AMA or other organized med society, but real MDs to stop this mess. We are driving MDs out daily. Its all fun and games until there are none left. And that is coming.
Regarding the GAO report on why so few paitents access their records.
For many patients there is limited value to accessing their medical records. If the patient visit was due to an acute condition such as a flu virus, muscle strain, sprain or surgery treating an acute condition such as appendicitis the problem is resolved quickly. There is limited need or useful information for the patient to view in a medical record.
Those with chronic conditions may find value in reviewing their medical records. A percentage of these chronic patients may make notes during their visits precluding the need to access a portal.
I would access a portal to view my annual physical lab results, if it meant avoiding a follow up visit to the practice.
As to the 48 percent access to users of one EHR. I doubt this is the result of the software desgn. Some medical practices have physicians send messages that require patients to login to their records to view. These are not clinically important messages just generic follow up courtesy messages to game the system. Note in the study, higher results at larger group practices where they have staff to implement such a program.
Thanks for bringing attention to interrupters.
Previously, one might assume it is just themselves being overly aware. Realizing it is a problem for others too via (a) an egotist or (b) someone so lacking in self-confidence is beneficial.
Faced with a consistent “manterruption” this week, I spoke with the person (even though higher title in the hierarchy) after the meeting to inform him that it was inappropriate. Surprising to me, he knew. He offered an apology of sorts.
It was good to confront this.
I like the suggestion to leave the meeting though too!
Would be nice if Tim Thompson at Baycare would work on getting Cerner to add value for us instead of these fake traffic ticket emails… the IS leadership has become an internal joke at BayCare leaving confidence and morale at an all time low… management through fear continues and no one speaks up… plenty of good folks have left…