RE the AI GLP1 company, Washington Post has an article today by someone who used one of those compounded products,…
Readers Write: Are You Ready for the Quality Payment Program?
Are You Ready for the Quality Payment Program?
By Kory Mertz

With the start of the New Year, the first performance period for the Quality Payment Program (QPP) has officially started. The QPP, part of the MACRA legislation, was passed with strong bipartisan support in Congress and sends a clear signal of the federal government’s accelerating effort to move to value-based payments.
QPP creates two new tracks for Eligible Clinicians (ECs), as program participants are called: the Merit-based Incentive Payment System (MIPS) and the Alternative Payment Models Incentive Program.
MIPS
MIPS consolidates and sunsets three programs focused on ambulatory providers: the Physician Quality Reporting Program, the Value-Based Payment Modifier, and the Medicare EHR Incentive Program for eligible professionals. In 2017, ECs can receive a maximum payment adjustment of plus or minus 4 percent based on their performance in four categories. ECs who are new to Medicare or who bill less than $30,000 or see fewer than 100 Medicare beneficiaries during a year will be exempt from MIPS.
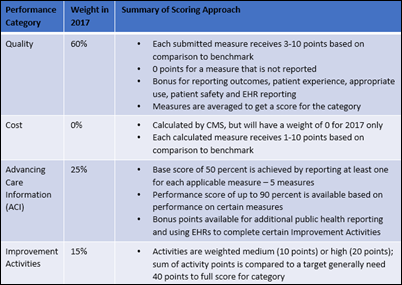
In response to significant feedback from the provider community, the Centers for Medicare and Medicaid Services (CMS) has simplified the requirements and made 2017 a transition year to help ECs get used to participating in MIPS. Providers have three general approaches they can take:

Alternative Payment Models Incentive Program
The second track of QPP is focused on increasing EC participation in Alternative Payment Models (APM) (i.e. Accountable Care Organizations, bundled payments, etc.) by offering a 5 percent bonus and exemption from MIPS for ECs who participate in an Advanced APM and meet certain participation thresholds. In 2017, ECs must have at least 25 percent of their Medicare payments or 20 percent of their Medicare patient panel in a CMS Advanced APM to receive the bonus and MIPS exemption. ECs who meet lower payment or patient thresholds have the option to be exempt from MIPS. CMS maintains the list of qualifying Advanced APMs here.
Moving Forward
The overarching framework created in the legislation and initial rulemaking completed by the Obama Administration will continue unchanged in 2017. The Trump Administration will have a chance to put its own twist on the QPP in 2017 by filling in the program implementation details through sub-regulatory guidance (much like CMS has done with the Meaningful Use program) and in 2018 and beyond through rulemaking to establish future program requirements. If Representative Tom Price is confirmed as the Secretary of the Department of Health and Human Services, he may accelerate efforts to reduce provider burden and simplify the QPP.
As providers prepare to participate in the first year of QPP and HIOs prepare to support providers’ success, they should keep the following in mind.
- While APMs have gained significant attention in recent years, CMS anticipates that the vast majority of providers will participate in MIPS in the early years of the QPP.
- Providers just beginning to think about the QPP requirements should generate reports to determine which providers are likely to be an EC during the performance period and which will fall under the low volume exclusion; map out the existing TIN/NPI structure of the organization to help support decision making around group versus individual reporting; and undertake a scan across the organization to determine existing Advanced APM participation by ECs. If an organization participates in an Advanced APM, a report should be generated based on all participating providers to determine if participants will qualify for a bonus and MIPS exemption under the APM track.
HIOs have the opportunity to position themselves to support providers’ success in QPP. HIOs should ensure they have functionality that aligns with program requirements, including:
- Implement certified tools to collect and submit electronic quality measures to CMS to support ECs and help them achieve bonus points for the quality performance category.
- Support ECs success with a variety of ACI measures including HIE (send and receive); view, download and transmit; and submitting information to public health and clinical data registries. A key consideration in determining which measures to support include the existing exchange environment the HIO operates in, if certified technology is required to meet the measure, whether the HIO’s technology meets the requirements (i.e. providing machine readable C-CDAs), and the ability to provide ECs necessary audit documentation.
- Support improvement activities. For example, “Ensure that there is bilateral exchange of necessary patient information to guide patient care that could include one or more of the following: Participate in a Health Information Exchange if available; and/or use structured referral notes.” A key consideration for supporting improvement activities is whether the HIO has the ability to provide ECs with necessary audit documentation.
Kory Mertz is senior manager of Audacious Inquiry of Baltimore, MD.


Nope and proud not to be.
MACRA is a shameful crazy complex program that no one, not even CMS can “estimate” how providers will be paid. Its a sad joke as this was touted as less of a burden.
And tweeted over and over and over by CMS leaders that “we listened” to reduce burden, etc. Did they?
They continue MU with a new name.
They continue PQRS with a new name
They continue resource use (CMS has NO idea how to attribute a “cost” to a specific MD)
They ADDED CPIA (oh thats less of a burden to add yet another reportable regulation?)
All of these have some unreadable calculus to determine how you are doing.And AAPM’s ? You need to hire a policy expert, attorney, accountant, and numerous other consultants to even get
close to that game. More risk for MDs? Puhlease.
Those of us that have not already been driven out by these ridiculous “value” reporting ideas, will fight at every point to get them thrown out. One way or another, they are destined to fail just like MU PQRS and other before them.
And if we don’t play, you can penalize us out of practice, but then you will have no one left to abuse.
What’s your solution to making healthcare great again? Go back to the 1990’s when Medicare costs were out of control? It’s not like physician practices were doing a great job of providing high quality healthcare at an affordable price? As Mr. Trump and his fellow Republicans are finding out – it is easy to nitpick, way tougher to provide solutions.
Government is the problem not the solution to health care.
Our government is run by and for corporations, not the people. That is the problem.
Re: VFJ – so are you saying you’re opposed to the Constitution ? First 3 words of the US Constitution “WE THE PEOPLE”. Looks like we agree that the actions of the government are the problem…. Corporations will by definition be better organized than individuals and no matter the laws that organization will give them more say and power in government than one individual. Again, government is the problem not the solution to health care.
http://constitutioncenter.org/interactive-constitution/preamble
RE:PM_From_Haities I think you missed the entire point of what VFJ said. The constitution is an old outdated piece of paper. The principles in which it represent are valuable. The problem is those values are no longer truly represented by our government because corporations control the government (not the people).
The point is policy is being created that is influenced by corporations and for corporations. These policies are not establishing Justice, insuring domestic Tranquility, providing for the common defense, promoting the general Welfare, nor securing the Blessings of Liberty to ourselves and our Posterity,
Learn how our government actually functions, not how it was “designed” to function 223 years ago. Words on paper mean nothing, action is everything.
Exactly why government is the problem not the solution to health care!