RE the AI GLP1 company, Washington Post has an article today by someone who used one of those compounded products,…
Monday Morning Update 5/16/16
Top News

John Halamka revisits his criticism of the proposed MACRA requirements, specifically suggesting that HHS focus on rewarding three specialty-specific outcomes at a time, allowing each specialty to choose those three outcomes and giving doctors free rein to use whatever technology they need to achieve them.
Halamka also suggests limiting EHR certification to basic care coordination interoperability functions:
- Sending a summary of care to a recipient listed in a national provider directory.
- Querying a record locator service and retrieving a common data set.
- Sending a care summary to a patient-provided address.
- Populating a relevant registry.
- Interacting with a prescription drug monitoring program.
Reader Comments

From Mister F: “Re: MD Anderson / Encore’s $50 million contract. Trace the relationships of current MDACC leadership > Encore leadership > Healthlink. It’s fraternity-based procurement behavior. If someone had the time to create the map of Healthlink alums in provider leadership roles, those in services (vendor) roles, and the subsequent contract awards, it would look pretty interesting.”
From Mark: “Re: Qardio’s real-time blood pressure and scale monitor that was just launched. Do MDs really want this ‘continuous’ information? Is this a billable service? How will MDs replace lost income with fewer patient visits?” Technology companies anxious to get a foothold in the lucrative healthcare market often confuse their limited sensor and analytics capabilities with what will work in real life to improve oucomes. Doctors don’t have the time or interest to monitor a patient’s self-measured vital signs, which have minimal diagnostic or therapeutic value (ask any nurse how often they ignore inpatient vital signs monitors without clinical consequence). It’s a situation similar to companies convinced that the biggest problem in medicine is lack of accurate diagnosis and offer technology to assist where assistance usually isn’t needed, not to mention that diagnosing from data alone ignores that art of medicine. It’s rarely healthcare professionals that come up with these ideas, and when it is, they’re usually ignoring the practical practice of medicine hoping nobody will notice and buy their product anyway.
HIStalk Announcements and Requests
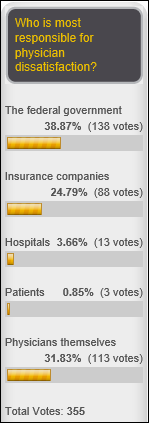
Poll respondents say it’s the federal government and doctors themselves who are most responsible for physician dissatisfaction. Some respondent thoughts:
- Ann Farrell says MACRA is crazily complex, but adds that doctors have been self-centered for decades in denying their quality statistics and failing to lead the charge on patient safety. She welcomes income-focused doctors to the world in which RNs and other employed professionals live — KPI games, stagnant wages, job loss, unrealistic productivity goals, and dwindling respect.
- Frank Poggio says doctors have been their own worse enemy since the start of Medicare, first fighting the concept but then jumping on the bandwagon when Part B was introduced, making many specialty doctors millionaires but not helping PCP who found that, “When you go to the bed with the devil, you wake up in hell.” He adds that doctors have an image problem both with patients and with payers because of the way they practice.
- Meltoots (who is a doctor) says the profession may be seen as whiny, but physicians are being beaten senseless with constantly changing regulations, fighting with insurance companies, patients who can’t pay their large deductibles, board certification headaches, and RAC audits. He says everybody should be paying attention if it’s so bad that John Halamka is on the ropes. He or she adds, “It takes 14 years of training just to make a fresh new me and another 17 of practice experience that is truly invaluable to my abilities as a surgeon. With my low costs and my quality numbers, CMS and ONC should be begging me to stay on board and not be penalizing me 2 percent because I cannot do MU. And with MACRA, it looks like they want to ratchet me down 9 percent. Look at my costs per patient, co-morbidities, and readmit rate and tell me I’m a bad deal for CMS. No chance.”
New poll to your right or here: would you recommend the hospital or medical practice where you had your most recent medical experience as a patient? Overachievers are welcome to click the Comments link on the poll after voting to explain.
I’m annoyed that Yelp, Tripadvisor, and LinkedIn are forcing website readers on mobile devices to open their proprietary app to continue reading. Not only do I resent being forced into their walled gardens, they often launch the App Store instead of handing off smoothly to their app that I’ve already installed.


Ms. Hardy and her Pennsylvania class of 18 elementary school students are “incredibly grateful” for the document camera, dry erase lapboards, and computer speakers we provided in funding her DonorsChoose grant request. She has students show their math answers on the whiteboard so she can easily see which ones need extra help. She reports that the document camera makes the students more eager to share their work and allows the visual learners to see lessons and materials modeled for them in their preferred learning style.
Last Week’s Most Interesting News
- Theranos shuffles its board and its president steps down.
- MD Anderson attributes its $160 million year-over-year drop in net income to its Epic implementation.
- NantHealth files for an initial public offering.
- McKesson loses a Horizon hospital to Cerner and a 14-hospital Star and Horizon group to Epic.
- HHS Secretary Burwell acknowledges to the ACP that Meaningful Use has been “burdensome” and “inflexible” for doctors and reinforces HHS’s interoperability agenda.
- ProPublic’s online narcotics prescribing database that was intended to call out questionable prescribers has the unintended consequence of being used to identify those prescribers by drug-seekers.
Webinars
None scheduled soon. Contact Lorre for webinar services. Past webinars are on our HIStalk webinars YouTube channel.
Sales

Doctors Community Hospital (MD) chooses the Summit Express Connect interface engine to manage all EHR connections.

Lincoln Surgical Hospital (NE) selects Access Passport for Web-based electronic forms integrated with Meditech.
Announcements and Implementations
ZeOmega releases Clinical Assessment Protocols for its Jiva population health management platform.
Penn State Health (PA) signs up for virtual ICU monitoring from Mercy Virtual.
Privacy and Security
The creator of the Tor anonymous Web browser (which powers the “dark Web” hacker haven) warns that medical identity theft is fast becoming the primary form of identity theft. He mentions that an unnamed healthcare organization is developing anonymous online drug tests, health services, health chat, and research questionnaires. He defends anonymous browsing as being similar to encryption in initially being used by people trying to hide something, but eventually becoming mandatory for secure, Web-powered commerce.
Children’s National Health System (DC) warns that its outsourced transcription provider, Ascend Healthcare Systems, misconfigured a server and thus allowed access by FTP to the information of 4,000 patients over a one-week period in February 2016. The health system stopped doing business with Ascend in mid-2014 and notes that Ascend failed to meet its contractual obligation to delete its data.
New Scientist magazine, which exposed England’s NHS data sharing agreement with Google two weeks ago, finds that neither Google nor the Royal Free London NHS Foundation Trust have requested ethical approval. It also notes that Google’s recently acquired DeepMind app has not been registered as a medical device. Royal Free defends sending Google the fully identifiable information of 1.6 million patients each year, saying that patients give their implied consent when their information is used by IT companies related to direct patient care.
Technology
Entrepreneur profiles India-based ICliniq, which offers an online doctor consultation app that uses a bot running on the WhatsApp-like messaging program Telegram. The company also offers a standard Android version.
A LinkedIn article by Cyrus Maaghul describes out-of-hospital use cases for blockchain technology that include tracking drug development, clinical credentialing, population heath data analysis, insurance risk pooling, telemedicine, and remote device monitoring. He’s head of product and technology for Phoenix-based PointNurse, which offers virtual visits with nurses for patient navigation, referral, consultations, disease management, and remote monitoring.
A Memphis man’s LifeVest wearable heart monitor and defibrillator saves his life when his heart stops beating in his sleep. The device has a 98 percent first-shock success rate for patients at risk for sudden cardiac arrest. The device first earned FDA approval in 2001, although I don’t recall hearing about it until now.
Other
Scripps Health’s Q2 financial report shows that its Epic project will cost $309 million in capital and $361 million in 10-year operating cost, although it expects to save $211 million of that by retiring applications that Epic will replace.
The New York Times notes that people who buy medical insurance via Healthcare.gov or state exchanges are often treated as second-class citizens even though their policies are issued by the same big insurers as employer-provided plans. Many providers don’t accept exchange-issued policies, provider networks are narrower and geographically limited, and some policies offer no out-of-network coverage at any price. The article notes that exchange-issued policies often omit high-priced providers that have local clout to set high prices, such as Memorial Sloan Kettering being left out of every exchange-sold plan even though New York employers would not find that acceptable for their employees. The article also observes that many of the doctors listed in insurance company directories aren’t accepting new patients even though federal law requires insurance companies to keep their provider directories current.
Direct-to-consumer teledermatology websites made a lot of mistakes when diagnosing and treating fake patients. In 62 encounters with 16 websites:
- None of the doctors asked for the patient’s ID.
- Two-thirds of the sites assigned a doctor without giving the patient a choice, mostly without disclosing the doctor’s licensure status. Some of them used offshore doctors who aren’t licensed in California where the study was performed.
- Only one-fourth of the doctors asked who the patient’s PCP was, and only 10 percent offered to send them records.
- Patients were rarely offered warnings about the risks of the drugs prescribed during the encounter.
- Clinicians diagnosed correctly most of the time when shown a photo in which the condition was obvious, but failed to ask good questions otherwise.
- The doctors missed significant diagnoses such as secondary syphilis and gram-negative folliculitis.
- The treatments ordered didn’t always follow guidelines.
The study’s authors note, however, that those same doctors might have performed equally poorly during in-person sessions, so maybe it’s not teledermatology itself that’s the problem. They suggest that while direct-to-consumer medicine can be be effective, the clinicians should be part of the practice or health system the patient already uses rather than randomly selected contractors of third-party sites.
UPMC reports that it paid six of its executives at least $2 million in its most recent fiscal year, including $6.43 million to President and CEO Jeffrey Romoff. CIO Dan Drawbaugh made $1.57 million.
TV consumer reporter John Stossel complained about poor customer service while he was hospitalized for lung cancer, but now he offers his solution: high-deductible insurance that forces consumers to shop carefully. Maybe he missed the recent research that found that what actually happens is that people just skip getting care rather than shopping more carefully for it. He also takes a logical leap in assuming that people paying more out of their own pockets will create an environment he describes as: “When patients shop, doctors strive to please patients rather than distant bureaucrats. More doctors give out their email addresses and cellphone numbers, and shorten waiting times. Their bills are easier to read because the providers want customers to pay them!” A lot of Americans now have high-deductible plans, so he as an investigative reporter should be able to fund examples where his idea has actually worked.
Sixteen VPs/SVPs of Wheaton Franciscan Healthcare will lose their jobs in its merger with Ascension Health, among them SVP/CIO Greg Smith.
The family of comedian Joan Rivers settles the medical malpractice lawsuit they brought against the New York city clinic where she died during a routine endoscopy. The suit claimed that the gastroenterologist performed a laryngoscopy despite the concerns of the anesthesiologist, while a CMS investigation found that the clinic failed to keep proper medication records, didn’t record the patient’s weight, failed to obtain informed consent, and allowed staff to take selfies with Rivers before she died.
Vince and Susan move along with their 2016 vendor review, covering small vendors in Part 4.
Weird News Andy says this man’s heart’s in the right place, even if it’s the wrong place. A patient’s complaint of right-side chest pain radiating to his right shoulder is found to have situs inversus, a rare condition in which all of the major visceral organs are on the opposite side of normal.
Sponsor Updates

- Huron Consulting Group employees lead nearly 100 events during its annual day of service.
- ESD offers a discount on automated testing solutions to CHIME members.
- T-System will exhibit at the MIHIMA 2016 Annual Meeting May 18-20 Bay City, MI.
- Talksoft is chosen as Greenway’s Intergy Partner of the Month.
- Visage Imaging will exhibit at ACR 2016 May 16-17 in Washington, DC.
- Zynx Health announces the winners of its 2016 Clinical Improvement Through Evidence Award.
- Experian Health and PatientMatters will exhibit at the HFMA Florida Spring Conference May 15-18 in St. Petersburg, FL.
- Red Hat announces the agenda and keynote speakers for Red Hat Summit 2016, June 27-30 in San Francisco.
- The SSI Group will exhibit at the Rural Hospital Alliance of Mississippi meeting May 18-20 in Orange Beach, AL.
- Streamline Health will exhibit at the 2016 Michigan HIMA Annual Meeting May 18-20 in Bay City, MI.
Blog Posts
- National Nurses Week 2016 (TeleTracking)
- Adding a mobile ultrasound program … but how? (UltraLinq)
- The Financial Impact of 2017 Medicare Advantage Payment Rules (Verisk Health)
- The Sweetest Match: Clinical and Coding Professionals (VitalWare)
- Patient safety requires close collaboration. (Voalte)
- On Death’s Door: My Patient Experience (Xerox Healthcare)
- GPS for Corporate Wellbeing ROI (West Corp.)
- Don’t Just Manage Denials; Prevent Them (ZirMed)
- 2016 Nurses Week – Culture of Safety: It starts with You (PatientSafe Solutions)
- Change Management: the Secret Ingredient in Successful Implementations (Sagacious Consultants)
- Say Thank You to a Labor Nurse (PeriGen)
- Survey Finds Healthcare Executives Credit IT with Improving Care (Phynd Technologies)
- The Beat Goes On: Medicare’s Newest Acronyms, MACRA, QPP, MIPS, and APMS (PMD)
- Combating Medical Errors with Interoperability (Surescripts)
Contacts
Mr. H, Lorre, Jennifer, Dr. Jayne, Lt. Dan.
More news: HIStalk Practice, HIStalk Connect.
Get HIStalk updates.
Send news or rumors.
Contact us.









Mark’s question about patient monitoring (now continuous monitoring) is spot on. Main things remotely monitored are glucometer, scales, and BP readings, with some SPO2 and spirometer. NONE of these have a demonstrated ROI and in one double blind study, the results of monitored vs unmonitored returned about a 1% difference in outcomes and cost (admittedly, this was only one study).
I can say this as I’ve worked in the industry selling these devices/solutions that report the data back to the physician or to a call center that monitors the patient data and takes interventive steps when something is out of whack.
At the most, one reading daily of any of these items is enough to spot trends. Weight gain in COPD/CHF patients and BP rise being the most critical. No way does anyone need a running graph of data especially on 3x per day blood sugar readings.
The factor most overlooked is what Mr. H said in reply. Not only do doctors or their staff not have time to look at all these readings (and if you have 100 diabetics in your practice being monitored it could mean 300 or more data points per day to consider), they don’t want the liability of having received the data, not looked at it, thus not acted upon it, and having the patient crash. Lawsuit city.
It is a good thing to have these readings, trend them over time and use them at the next appointment to adjust meds and patient attitudes/activities. Even then, we couldn’t prove you even got a dollar back for each dollar spent – and that ignores the extra doctor and staff time consumption.
Rebuttal to Mr. F: Encore and MD Anderson. The news reported just isn’t true. Encore did not lead the MD Anderson go-live efforts–that was Santa Rosa. Just because it’s a small industry (and almost every consulting company has close ties to leadership) doesn’t mean it isn’t competitive.
I think he said Encore led the Implementation, not the go-live. There is a difference you know.