Amazing that the takeaway is that its easier to buy a gun than to get credentialed as a physician is…
News 12/2/15
Top News
The Health IT Policy Committee’s API Security Task Force held its first meeting Monday, co-chaired by Josh Mandel (Harvard Medical School) and Meg Marshall (Cerner). The group is charged with identifying privacy and security issues with open APIs. Its next meeting is this week.
Reader Comments
From Frying Burrito Brother: “Re: DonorsChoose. Our company would like to donate and I don’t see instructions.” I have matching money left, which I will apply to your donation made as follows:
- Purchase a gift card in the amount you’d like to donate.
- Send the gift card by the email option to mr_histalk@histalk.com (that’s my DonorsChoose account).
- I’ll be notified of your donation and you can print your own receipt for tax purposes.
- I’ll pool the money, apply the matching funds, and publicly report here (as I always do) which projects I funded, with an emphasis on STEM-related projects as the matching funds donor prefers.
From Equine Hindquarters: “Re: EHR databases. You wrote a long time ago that they should all use the same basic schema and compete on additional tables as well as their UI.” I’ll update my suggestion as follows. Each EHR should contain a basic set of tables with a universal format so that any authorized party can retrieve patient demographics, visits, medication lists, etc. That eliminates the need to convert proprietary tables or run the query through an HIE that may or may not be translating correctly. That also places onus for the data accuracy and completeness on the EHR vendor, who is best equipped to manage that task. Those interoperability tables would be separate from the existing EHR tables to avoid exposing proprietary information or methods. It’s like exporting a CCDA or other document except that it resides permanently in the vendor’s database with real-time updates and could be accessed via standard APIs with minimal effort or system knowledge. The vendors know their own systems, so let them populate these standard tables instead of forcing everybody who needs access to their patient information to figure it out for themselves.
From Pippi Longstocking: “Re: Microsoft Lync. Does anyone know of an acute care facility that has fully converted to it? If so, how was HL7 addressed and is backup and stability similar to a traditional communication platform?”
HIStalk Announcements and Requests
Welcome to new HIStalk Platinum Sponsor Spok (pronounced “spoke”). The Springfield, VA-based company is a market leader in critical communications solutions – clinical alerting and notification, secure hospital communications, physician and nurse scheduling, paging, and contact center technologies. The company chose its new name in 2014 following the 2011 acquisition of Amcom Software by USA Mobility. The Spok Mobile secure texting app allows users to send images and video along with text, with full logging and HIPAA compliance. Spok Critical Test Results Management helps meet National Patient Safety Goal #2 in quickly sending radiology and lab results to the right clinicians on their mobile devices, accelerating the treatment plan and discharge process as appropriate and protecting against malpractice lawsuits. The FDA-approved Spok Messenger sends mobile alerts from nurse call systems while routing non-clinical requests to the appropriate team member. Paging remains relevant as an essential part of critical healthcare communications due to its high reliability and low cost and Spok offers both wide-area and onsite versions of it. Thanks to Spok for supporting HIStalk.
Here’s a YouTube video case study that describes Banner Health’s use of Spok solutions to create patient-centric communications.
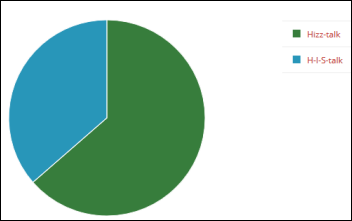
I’m among the one-third minority who pronounce the name of this site “H-I-S-talk” rather than the “Hizz-talk” preferred by two-thirds of 335 poll respondents. Dean says he doesn’t like turning acronyms into words and was baffled when people at his previous employer pronounced “URL” as “earl,” which reminds me of my annoyance at people pronouncing Joint Commission back in its JCAHO days as “jayco,” which makes no sense at all but is at least less annoying than lowbrow humorists who gleefully turn FHIR into tediously non-clever “fire” puns. Two respondents offered a variation I hadn’t though of in “hisstalk.” At least nobody said they incorrectly assume that: (a) the “his” is the opposite of “hers,” or (b) the name has a religious connotation.

Mrs. Jarrell from Louisiana reports that her seventh graders are learning about integers as they use the math manipulatives and electronic quiz tools we provided via DonorsChoose.
I get a bit queasy when I see how HIMSS advises its vendor members on how to sell their products to its provider members, as evidenced by the pitch for its recent webinar that gets me going in several ways:
- It uses “social” as a synonym for “social media,” which it is not (although I’m at least happy it’s not the retch-inducing “sosh”). It also bleats out “leverage” and “utilize” instead of the less-pompous and perfectly serviceable “use.”
- It pitches the use of social media to “generate excitement about your brand before and during HIMSS16 utilizing its expert team,” with the expert team to be “utilized” being that of HIMSS Media, which seems to have happily eliminated the firewall between alleged news reporting and for-hire pitching. I’ve yet to experience tweet-induced excitement about a company, especially when the tweets in question emanated from those folks.
- It claims that screwing around with Twitter and Facebook will result in “transforming yourself from a vendor into a trusted advisor.” That’s asking a lot from simply assigning some 20-something kid to post unoriginal, corporate-approved thoughts that decision-makers will never read because they have far better things to do than monitoring Twitter. It’s usually a really bad idea to make a vendor your “trusted advisor” unless the advice you seek is that you should buy whatever they’re selling.
- It reminds me that HIMSS makes millions from pimping low-paying provider members to high-paying vendor members while also selling itself. I like some of what HIMSS does, but the emphasis on its own bottom line keeps increasing. They’re almost as bad as AAA, which bombards me trying to sell insurance, car repair, vacations, sponsor-supported products, credit cards, and even used cars when all I want is roadside assistance and maybe an occasional hotel discount.
Webinars
December 2 (Wednesday) 1:00 ET. “The Patient is In, But the Doctor is Out: How Metro Health Enabled Informed Decision-Making with Remote Access to PHI.” Sponsored by VMware. Presenters: Josh Wilda, VP of IT, Metro Health; James Millington, group product line manager, VMware. Most industries are ahead of healthcare in providing remote access to applications and information. Some health systems, however, have transformed how, when, and where their providers access patient information. Metro Health in Grand Rapids, MI offers doctors fast bedside access to information and lets them review patient information on any device (including their TVs during football weekends!) saving them 30 minutes per day and reducing costs by $2.75 million.
December 2 (Wednesday) 1:00 ET. “Tackling Data Governance: Doctors Hospital at Renaissance’s Strategy for Consistent Analysis.” Sponsored by Premier, Inc. Presenters: Kassie Wu, director of application services, Doctors Hospital at Renaissance; Alex Eastman, senior director of enterprise solutions, Premier, Inc. How many definitions of “complications” (or “cost” or “length of stay”…) do you have? Doctors Hospital at Renaissance understood that inconsistent use of data and definitions was creating inconsistent and untrusted analysis. Join us to hear about their journey towards analytics maturity, including a strategy to drive consistency in the way they use, calculate, and communicate insights across departments.
December 2 (Wednesday) 2:00 ET. “Creating HIPAA-Compliant Applications Without JCAPS/JavaMQ Architecture.” Sponsored by Red Hat. Presenters: Ashwin Karpe, lead of enterprise integration practice, Red Hat Consulting; Christian Posta, principle middleware architect, Red Hat. Oracle JCAPS is reaching its end of life and customers will need a migration solution for creating HIPAA-compliant applications, one that optimizes data flow internally and externally on premise, on mobile devices, and in the cloud. Explore replacing legacy healthcare applications with modern Red Hat JBoss Fuse architectures that are cloud-aware, location-transparent, and highly scalable and are hosted in a container-agnostic manner.
December 3 (Thursday) 2:00 ET. “501(r) Regulations – What You Need to Know for Success in 2016.” Sponsored by TransUnion. Presenter: Jonathan Wiik, principal consultant, TransUnion Healthcare Solutions. Complex IRS rules take effect on January 1 that will dictate how providers ensure access, provide charity assistance, and collect uncompensated care. This in-depth webinar will cover tools and workflows that can help smooth the transition, including where to focus compliance efforts in the revenue cycle and a review of the documentation elements required.
December 9 (Wednesday) 12 noon ET. “Population Health in 2016: Know How to Move Forward.” Sponsored by Athenahealth. Presenter: Michael Maus, VP of enterprise solutions, Athenahealth. ACOs need a population health solution that helps them manage costs, improve outcomes, and elevate the care experience. Athenahealth’s in-house expert will explain why relying on software along isn’t enough, how to tap into data from multiple vendors, and how providers can manage patient populations.
December 9 (Wednesday) 1:00 ET. “The Health Care Payment Evolution: Maximizing Value Through Technology.” Sponsored by Medicity. Presenter: Charles D. Kennedy, MD, chief population health officer, Healthagen. This presentation will provide a brief history of the ACO Pioneer and MSSP programs and will discuss current market trends and drivers and the federal government’s response to them. Learn what’s coming in the next generation of programs such as the Merit-Based Incentive Payment System (MIPS) and the role technology plays in driving the evolution of a new healthcare marketplace.
December 9 (Wednesday) 1:00 ET. “Looking ‘Back to the Future’ on Clinical Decision Support and Data Warehousing.” Sponsored by Health Catalyst. Presenter: Dale Sanders, SVP of strategy, Health Catalyst. Dale will use a 2006-era slide deck (complete with old-school graphics) on using an enterprise data warehouse in clinical decision support, as it was originally presented to several masters-level informatics classes nearly 10 years ago. Some of the information in the “time capsule” will be laughably wrong, while some will still be relevant. Either way, reviewing the past will help inform the future. A highly interactive Q&A will follow.
December 16 (Wednesday) 1:00 ET. “A Sepsis Solution: Reducing Mortality by 50 Percent Using Advanced Decision Support.” Sponsored by Wolters Kluwer Health. Presenter: Stephen Claypool, MD, medical director of innovation lab and VP of clinical development and informatics for clinical software solutions, Wolters Kluwer Health. Sepsis claims 258,000 lives and costs $20 billion annually in the US, but early identification and treatment remains elusive, emphasizing the need for intelligent, prompt, and patient-specific clinical decision support. Huntsville Hospital reduced sepsis mortality by 53 percent and related readmissions by 30 percent using real-time surveillance of EHR data and evidence-based decision support to generate highly sensitive and specific alerts.
December 16 (Wednesday) 1:00 ET. “Need for Integrated Data Enhancement and Analytics – Unifying Management of Healthcare Business Processes.” Sponsored by CitiusTech. Presenters: Jeffrey Springer, VP of product management, CitiusTech; John Gonsalves, VP of healthcare provider market, CitiusTech. Providers are driving consumer-centric care with guided analytic solutions that answer specific questions, but each new tool adds complexity. It’s also important to tap real-time data from sources such as social platforms, mobile apps, and wearables to support delivery of personalized and proactive care. This webinar will discuss key use cases that drive patient outcomes, the need for consolidated analytics to realize value-based care, scenarios to maximize efficiency, and an overview of CitiusTech’s integrated healthcare data enhancement and analytics platform.
Contact Lorre for webinar services. Past webinars are on our HIStalk webinars YouTube channel.
Acquisitions, Funding, Business, and Stock

Allscripts announces a share buy-back of up to $150 million.
Sunquest Information Systems will move its Tucson, AZ headquarters to an office building on the north side. Google Maps indicates that it’s a 26-minute drive between the offices, just in case you’re an employee trying to assess your quality of life impact. I’ve had my hospital commute involuntarily changed a few times by an office move, where the folks in charge seemed surprised that most employees weren’t thrilled about wasting more hours driving every week just to stare at the same cubicle walls moved to a further-flung part of town. My limited analysis was that somehow the new building was always closer to the wealthier neighborhoods where hospital executives lived and featured an even nicer version of Mahogany Row on whose plush carpet the peons rarely trod except as guests at their own termination.
Blue Cross Blue Shield of Michigan acquires insurance company software vendor IkaSystems, which has some executive team members who have worked for various health IT vendors.
Sales

University of Chicago Medicine (IL) chooses Valence Health to support its clinically integrated network, the 30th such organization to implement the company’s unified clinical information solution.

Skagit Regional Health (WA) chooses Epic at an estimated cost of $72 million over five years. ECG Management Consultants, which managed the selection, says Skagit will displace Meditech in the hospital and NextGen in its clinics.
People


Online second opinion provider 2md.MD hires Kirk Rosin (Aetna) as chief strategy officer and Kristin Herrera (UnitedHealthcare Global) as chief growth officer.

Florent Saint-Clair (DR Systems) joins Dicom Systems as EVP.

CTG promotes Amanda LeBlanc to VP/chief marketing officer.

Kate Crouse (Smart Exec Tech LLC) is named network CIO at Kings County Hospital – Central Brooklyn (NY).

Vital Images names Paul Markham, DBA (Origenetics) as VP of marketing.
Rob Senska, Esq., MBA (Somerset Medical Center) joins Besler Consulting as director of compliance services and associate general counsel.
Announcements and Implementations
Yale-New Haven Hospital (CT) implements Mobile Heartbeat’s MH-Cure clinical smartphone app, with three-fourths of its physician users saying it has improved patient workflow and safety.
Naunce and the National Decision Support Company announce their collaboration to support ACR’s Imaging 3.0 by offering NDSC’s ACR Select appropriate use criteria along with Nuance PowerScribe 360 and PowerShare Network.
National Decision Support Company also announces that it has signed an exclusive agreement with Cerner to make its ACR Select imaging appropriate use criteria available to Millennium users.
Craneware will demonstrate a new version of its Pharmacy ChargeLink solution at the ASHP Midyear Clinical meeting, which includes predefined formulary mapping to Epic Willow and Cerner PharmNet.
Privacy and Security
In Canada, a former administrative assistant of Alberta Children’s Hospital is charged with 26 counts of inappropriately accessing patient records. She had already been fired for snooping.
Technology
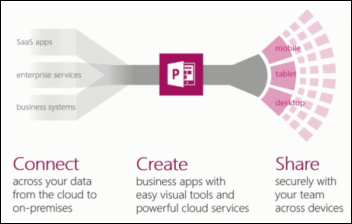
Microsoft announces PowerApps, which it says will allow non-technical employees to create apps that work on any device by using Office-like templates, a drag and drop workflow designer, and connections to cloud and on-premises services such as Salesforce, Dropbox, and databases. That would be pretty cool if it works as described since subject matter experts typically struggle when trying to move handy, Office-powered workgroup apps to web or mobile environments without technical help.
Other
The US Supreme Court declines to hear the case of a retired Texas veterinarian whose license was suspended for offering online pet advice in yet another clash between Texas professional boards and telemedicine providers. The vet says the state’s requirement that he physically examine an animal before offering telephone advice violates his free speech rights. He was offering only advice, not the writing of prescriptions.

WakeMed (NC) blames its $50 million FY2015 loss on major expenses that include its Epic implementation, construction of a new 61-bed hospital in Raleigh, and running a care management program, but says the numbers are deceiving because the investments will pay off later. Meanwhile, neighboring Duke University Health System, which reported $355 million in profit on $3 billion in revenue, says its Epic-related financial hit from last year is history and Epic is now delivering the expected results. UNC Health Care System made $119 million on $3.2 billion in revenue.
Coca-Cola’s chief science and health officer retires following a New York Times report that described how the company secretly funded a non-profit that urged Americans to exercise more instead of drinking less soda as advocated by what Coke called “public health extremists.” The CEO of the non-profit, which has since shut down, accepted honoraria and travel expenses from Coca-Cola before he formed the group. He’s a professor at the University of Colorado School of Medicine, which returned Coke’s $1 million donation following the article’s publication. Coke also paid $500,000 to University of South Carolina, which says it’s not giving the money back.
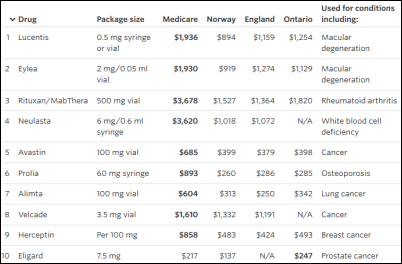
A Wall Street Journal investigative report finds that Americans provide most of the global drug industry’s profits because of pharma’s political clout, an unwillingness by Americans to limit use of expensive drugs regardless of proven therapeutic benefit, laws that prohibit Medicare from negotiating drug prices, the fragmented US healthcare system in which lack of a single government buyer allows drug companies price their products however they like, and demand-generating direct-to-consumer advertising that most countries don’t allow.
In the Cayman Islands, the former board chair of the health services authority is on trial for defrauding the public after the HSA awarded a patient swipe card contract to a firm in which he held partial ownership. Witnesses testified that the technical committee’s choice of Cerner angered him to the point he a sent a copy of Cerner’s proposal to the owner of eventual winner AIS Jamaica, with whom he planned to open a pharmacy business.
Facebook CEO Mark Zuckerberg announces in a letter written to his newborn daughter Max that he and his wife Priscilla Chan, MD will give away 99 percent of their Facebook shares – worth $45 billion today – via a foundation that will focus on personalized learning, curing disease, connecting people, and building strong communities.
A KPMG survey finds that 80 percent of organizations report their ICD-10 transition as smooth, although its methodology of surveying 300 attendees of an ICD-10 webinar is lazy.
A tiny observational study finds that doctors who enter information into the EHR during patient visits not only communicate less as you might expect, but also argue more with their patients and earn lower satisfaction scores. That may mean that those doctors don’t communicate well, but it could also indicate that the observations made involved patients who were sicker or newer, thus requiring more data entry and less catering to the patients’ every whim. The most telling aspect would be how the computer and monitor were positioned in the exam room, which heavily drives patient perception as being either exclusionary or participatory.
Websites that offer estimated medical procedure costs, including those run by insurance companies, often give consumers incorrect cost information that leaves them paying higher-than-expected expenses out of their own pockets, according to an NPR review. Reasons include health systems that quietly buy other providers and increase their prices, use of historic or aggregated prices, and not knowing exactly what procedures a doctor might perform during a visit or how the doctor will code and bill it. Price transparency is also nearly non-existent as prices are hidden inside non-public contracts between payers and providers.
Weird News Andy enjoyed the programmer jokes I ran recently and offers “Mr. Boole Comes to Tea” in a belated celebration of George Boole’s 200th birthday.
Sponsor Updates
- Anthelio Healthcare Solutions will exhibit at the HIMSS Gulf Coast Chapters event December 4-5 in Birmingham, AL.
- Capsule will exhibit at the IHI National Forum on Quality Improvement in Health Care December 6-9 in Orlando.
- Divurgent ranks amongst CIOReview’s 50 most promising healthcare solution providers.
- Fujifilm debuts an updated version of Synapse RIS at RSNA.
- Visage Imaging is demonstrating Visage Ease mobile imaging results enhancements at RSNA.
- Healthfinch will exhibit at The Institute for Healthcare Improvement Annual Conference December 6-9 in Orlando.
- Huntzinger Management Group interviews client ProMedica CIO Rose Ann Laureto about the organization’s Epic go live.
Blog Posts
- 4 Reasons Private Physicians Should be Thankful That They’re Employed (AdvancedMD)
- 16 Tweet-imonials We’re Thankful for This Season (AirWatch)
- Update: The CCJR is distinctly different from other bundled payment models (Besler Consulting)
- The Roadmap to HIT Success Part 1: 5 Guiding Principles for Use Case Development (Burwood Group)
- Go Big or Go Home: The Importance of Scale in Population Health (Caradigm)
- Bringing Up Baby with Healow (EClinicalWorks)
- Chronic Care Management – Are you getting paid for the work already being done? (Galen Healthcare Solutions)
- 6 Ways to Avoid Squandering Consulting Hours (Galen Healthcare Solutions)
- HIMSS EMRAM Site Visit Presentation – 4 Key Questions (The HCI Group)
- Pharmacy’s Role in Reducing Readmissions: New Findings (Healthcare Data Solutions)
- The Business Case for Patient Engagement: Convenience and the Wild Card (Healthwise)
Contacts
Mr. H, Lorre, Jennifer, Dr. Jayne, Dr. Gregg, Lt. Dan.
More news: HIStalk Practice, HIStalk Connect.
Get HIStalk updates.
Contact us or send news tips online.












“Each EHR should contain a basic set of tables with a universal format so that any authorized party can retrieve patient demographics, visits, medication lists, etc.”
Epic (for example, but probably Cerner, IDX, etc.) uses Cache and it does not use tables. So this suggestion doesn’t work unless you’re mandating that they switch to a relational database (which would probably bankrupt them due to having to re-write much of their core software).
There is a lot of optimization (performance) and abstraction (allows things like upgrades to happen more easily) that happens. If you were to mandate standardization that means doing away with all those optimizations as you’d be coding to the lowest common denominator. The difference is something like your system on the same hardware supporting 1000 or 10000 users. Or an upgrade having an 9 hour outage as opposed to a 90 minute outage. There are real benefits that would be impacted. Standardization should really be at the API level. What needs to happen is the various levels of features being documented and supported by the API. You should standardize what data values are contained in a patient’s chart, encounter, claim, etc., and make sure there are API’s that can pull all those values in a documented format. At some point you’d have to limit or support the limiting of the transfer rate of those API’s as well. I can imagine some vendor trying to drain the entire 5TB database from another vendor on a live system on a Tuesday at 10 AM and slowing the system down for everyone, and then complaining of not being allowed to inter-operate when the system can’t handle it.
Technical requirements should really not come directly from people who are not technical. I wouldn’t imagine recommending to a doctor standardizing on a procedure of which I know almost nothing about. You can specify high level requirements that can do what you are trying to do through low level requirements. Mandate the intentions, and leave the implementation details to those that have the know-how.
As a correction to AC, Epic already provides – and has provided for a long time – a standard framework that extracts the Cache database into a relational structure. It’s call KBSQL (not sure what the KB stands for). It allows you to query the Epic database with SQL statements. One means of doing so is through web service calls.
Now these tables don’t conform to any industry standard – since there isn’t one – but that’s not to say they couldn’t should one come along (I won’t hold my breath).
As a long time employee of Sunquest Information Systems, I am excited about the move to the new office building on Sunrise. The company is making a long term commitment to the employees creating a professional environment to work. The property itself is larger allowing growth and the much needed space to build education theaters, demo/workflow labs and resource libraries.
I’ve worked at Sunquest for more than 25 years and am really looking forward to the new office. During the dark days of being private equity owned, little was done for employees. It’s exciting to see the new changes here and the office looks really beautiful with the extra windows and access to nature.
@ AC, not really, that’s not what he’s saying – the tables don’t have to be the db layer of the application and it doesn’t have to require any change in underlying scheme that drives functionality. They can produce and stand up RD tables without compromising their application, as long as they make it an extra component. No software would need wholesale rewriting – just accommodation for RD structure in addition to cache.