Challenger exploded on lift-off when the O-rings failed. Columbia disintegrated on reentry after one of the heat shield tiles were…
Monday Morning Update 11/23/15
Top News
The Department of Defense notifies the House Appropriations Committee that it has met the federal requirement that it share records with the VA. The demonstrated solution was the Joint Legacy Viewer, a combined visual view of the information stored in separate DoD and VA systems. The DoD and VA spent several billion dollars trying unsuccessfully to integrate their systems, finally settling for a questionable level of “interoperability” in putting information from their respective systems on the same user screen.
Reader Comments
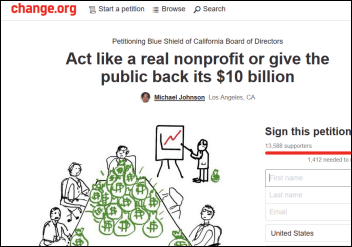
From Concerned Insider: “Re: Blue Shield’s lawsuit against its former executive. This has far-reaching implications on several issues – non-profit status, corporate corruption, and H-1B visas – all of which hinder healthcare efficiencies.” The non-profit insurer Blue Shield of California sues its former policy director, who launched a public campaign after his departure criticizing the company for running itself like a for-profit company and providing too little value to the public. Michael Johnson says he won’t back down from his demand that Blue Shield either provide $500 million per year in community benefits or return the $10 billion in assets it holds. Blue Shield claims Johnson is exposing confidential company information, which the company discovered after having forensic analysis of his laptop performed while he was still an employee. California revoked Blue Shield’s tax-exempt status earlier this year and ordered it to pay back taxes. The organization has 5,000 employees, a payroll of $426 million, and $9 billion in annual revenue. Healthcare is full of theoretically non-profit organizations that pay multi-million dollar salaries, hold fortunes in assets, and predatorily acquire competitors to protect their market position.
From CIO Boy: “Re: webinars. I might be a geek, but since I found the HIStalk webinar channel on YouTube I’ve watched several of them just to see what’s going on.” I’ll offer a confession of my own – I sometimes bring up the channel on my Roku streaming player and watch previous HIStalk webinars on the living room TV with surround sound. I don’t explore the Roku menus often and didn’t realize YouTube was an option.
From Court Watcher: “Re: Epic’s lawsuit against Tata. The court called Tata’s employees ‘hackers’ and Tata’s arguments ‘meritless.’ Any lawyers want to give an opinion?” A Wisconsin court denies a motion from India-based Tata Consultancy to dismiss Epic’s claims that Tata used its confidential information and trade secrets. Epic claims that Tata’s employees, working as consultants to Kaiser Permanente, misrepresented themselves as customer employees in gaining access to Epic’s UserWeb, after which they downloaded Epic’s proprietary information from India. The court rules that the actions of Tata’s employees meets the definition of inside hacking and leaves it to other courts to assess Epic’s claims of damages. It’s a pretty big deal for a huge, international company to be labeled as a hacker rather than a hackee.
From FlyOnTheWall: “Re: Cleveland Clinic. Warns patients accessing its medical records to expect inaccuracies and incomplete documentation. Lowering the bar much?” The clinic warns patients that its clinician documentation isn’t written for them, may make it seem that their doctor is uncaring or grammatically challenged, that records may contain boilerplate information or facts collected for reasons other than patient care, and that references to weight or alcohol consumption aren’t personal. I admire their honesty, but I hope public pressure doesn’t turn otherwise meaningful notes into the cheery, falsely complimentary drivel that’s in the summary notes of dogsitters and daycare centers.
HIStalk Announcements and Requests
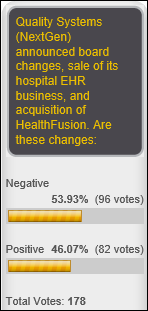
It’s a respondent toss-up as to whether the flurry of recent Quality Systems changes are positive or negative. New poll to your right or here: should federal privacy laws be expanded to include everybody instead of covered entities only?
Welcome to new HIStalk Platinum Sponsor Wolters Kluwer Health’s POC Advisor. POC Advisor combines evidence-based clinical decision support with advanced clinical and change management consulting services to help detect and treat sepsis. It’s built on the proven Sentri7 infrastructure that is used by 400 hospitals, integrating CDS products (UpToDate, Lexicomp, Medi-Span, Provation clinical content, Language Engine, and surveillance engine) into a clinician-friendly mobile interface and cloud-based rules engine. Hospitals define sepsis-related detection and treatment alerts and then POC Advisor brings in vital signs, nurse notes, and lab results from the EHR via HL7, applying hundreds of rules to send targeted, multi-disciplinary care alerts. The addition of change management supports the integration and use of POC Advisor and sepsis protocols, resulting in a greater than 50 percent reduction in sepsis mortality in partner hospitals. Thanks to Wolters Kluwer Health and its POC Advisor platform for supporting HIStalk.
I found this YouTube video that introduces Wolters Kluwers Health POC Advisor.
Red Hat is supporting HIStalk at the Platinum level. The Raleigh, NC-based company believes that open, hybrid technology is the future of IT and that open source is the operating system for the cloud. Red Hat supports architecture that is modernized, standardized, and virtualized, offering Red Hat Enterprise Linux Server and the Red Hat Enterprise Linux OpenStack Platform for building public or private clouds. Red Hat Satellite allows enterprises to keep Red Hat infrastructure running efficiently and securely, offering complete life-cycle management (provisioning, configuration management, software management, and subscription management) in a single console that offers an average payback period of seven months and allows enterprises to identify and respond to vulnerabilities. The company offers a December webinar titled “Creating HIPAA-Compliant Applications Without JCAPS/JavaMQ Architecture.” Thanks to Red Hat for supporting HIStalk.
Here’s a great video of Red Hat CEO Jim Whitehurst opening the company’s summit a few months ago in Boston as he talks about economic change and how companies operate in the Information Age. He points out that Uber owns no cars, Facebook creates no content, Alibaba owns no inventory, and Airbnb owns no real estate.


Mrs. Hatley from Washington says her kindergartners are enjoying the listening center we provided via DonorsChoose, learning the basics of reading as they following along with narrated stories. Also checking in is Ms. Perkins, whose Louisiana elementary school students are using the iPad and math manipulatives we provided to make math fun.
I received two emails from the same conference last week, one urging me to register and the other issuing a call for speakers. It reminded me of scalpers who stand outside of a sporting event carrying two signs, one saying “Have Tickets” and the other saying “Need Tickets.” It’s all about the arbitrage.
Listening: new from Jeff Lynne’s ELO, which grabbed me instantly with its moving first track that sounds like a cross between the classic Electric Light Orchestra and the Beatles (it’s at 18:30 in the video). It’s the first ELO album since 2001 and the best since their mid-1970s prime. Rolling Stone positively gushed at the band’s first live US performance in 30 years, which required security to ask Paul McCartney to refrain from dancing in the aisle. Purists might debate whether this is ELO or just Jeff Lynne with some stellar pick-up players who are replacing former ELO members who left or died, but whatever it is, I’m a fan.

I’m fascinated by what’s going on with the Healthcare.gov marketplace as insurance companies back away following huge losses. The country’s biggest insurer, UnitedHealth Group, was saying just a month ago that it would expand ACA coverage but now says it will lose $600 million on ACA-issued policies this year and will scale back its participation even after implementing big premium increases. I talked to a friend who sells individual and company medical insurance, who made these points:
- Insurance companies have greatly reduced their 2015 plan choices. UnitedHealth Group pulled many of its plans offline early last week, including most of its Silver-level plans, which my friend says customers can still buy, but not via Healthcare.gov – she has to call the company (with hours-long wait times) to get a paper application form. Apparently the laborious process allows the company to meet the government’s requirement of offering such plans that it doesn’t really want to sell while making it difficult enough that few people will buy them.
- Insurers have raised their deductibles from around $1,500 last year to $6,500 this year. Read that again: the insurance company pays nothing until the patient has spent $6,500.
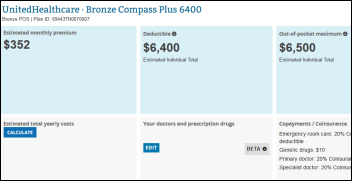
- I ran a Healthcare.gov cost estimate for a 50-year-old, non-smoking male in Chattanooga, TN whose income precludes a federal subsidy. UHG’s Bronze-level plan costs $352 per month with a $6,400 deductible and a $6,500 out-of-pocket maximum. That means a single ED visit or hospitalization will cost the insured their full $6,500 plus what they already paid for their annual premium, or nearly $11,000 cash out of pocket for the year. That’s for an individual, not a family. The hospital implications are enormous since they now have to attempt to collect the money owed to them by someone who almost certainly doesn’t have that kind of cash lying around. These days, having insurance doesn’t mean being free of the risk of medical bankruptcy.
- Healthcare.gov can’t ask any demographic questions except whether the applicant smokes, their age, and where they live. Prices vary considerably by state based on claims experience as well as local market provider competition.
- Some of the plans I pulled up online have as few as 4-5 doctors who participate in a given area.
- Co-insurance has become a lot more common in addition to deductibles, meaning patients keep paying a fixed percentage of billed costs until they hit their out-of-pocked maximum. Many available plans don’t offer a fixed doctor or ED visit co-pay – the insured patient pays a percentage that is usually around 30 percent instead of the formerly common $20 per PCP visit or $250 per ED encounter. That will put a lot of pressure on providers to collect those large amounts.
- Insurance companies have changed their prices, coverage, and availability hugely from last year, forcing consumers to change plans.That means starting over with new providers, trying to find doctors that are accepting new patients, and wiping their medical records slate clean as lack of interoperability means their new doctors will hand them the ubiquitous clipboard on which to provide their medical history.
My friend’s conclusions:
- Employer-provider medical insurance offers better coverage for a lot less money than Healthcare.gov or other individually sold plans, even if your employer sticks you with a higher cost.
- The ACA is providing a lot of unpleasant surprises to both insurance companies and their customers, as too few young and healthy people are signing up to offset more expensive customers who are catching up on medical treatment after years of not having insurance to foot the bill.
- ACA addressed availability of insurance, not healthcare costs, and the coverage and premiums are reflecting that.
- Insurance companies keep armies of accountants and actuaries busy trying to find ways to reduce risk and increase profit. Selling directly to individuals who sign up only if they expect their medical expenses to exceed their cost of insurance means someone has to pay. Employer-provided plans give companies a broader risk pool and often require big employers to accept some of the risk of their employee population, which helps control medical utilization and cost.
- Rapidly increase drug costs have forced insurance companies to make dramatic formulary changes, especially for specialty drugs, with some companies requiring a $250 deductible and 30 percent co-pay for drugs like Humira that can cost several thousand dollars per month. Lack of generic competition has also caused some insurers, such as UHG, to require patients to try other products for which they’ve negotiated a better price even though the patient response may not be the same.
- Most of those who don’t have Medicaid, Medicare, or employer-provided insurance aren’t likely to be able to afford either the insurance or their out-of-pocket costs. That means middle-class people who are self-employed or who work for companies that don’t provide insurance are taking the biggest hit.
- People can buy expensive medical insurance and still go broke trying to pay their portion of their medical expenses.
I’m interested to see how the government assesses penalties for people who don’t buy insurance. That should be coming as people file 2015 taxes. I suspect many folks will simply continue to not buy it and won’t be penalized, especially the younger, healthier people upon whose participation the entire ACA is built.
I’m not sure where this free-market experiment is going, but I suspect that the political backlash will be significant and the calls for healthcare price controls and/or universal coverage will get louder even though it’s political suicide to suggest either. As health economist Uwe Reinhardt says, “Of all the conceivable ways to finance healthcare, Americans have found the dumbest way to do it.”
Last Week’s Most Interesting News
- The concept of offering individual medical insurance coverage via Healthcare.gov took blows as insurance companies announced that losses have forced them to scale back their offerings, raise prices significantly, and consider pulling out of the Affordable Care Act insurance marketplace completely.
- Venture capital firm Andreesen Horowitz launches a $200 million investment fund that will focus on digital therapeutics, tech-enabled biology, and computational medicine.
- A federal judge dismisses charges and scolds the Federal Trade Commission for taking action against a lab services provider that was driven out of business by the FTC’s claims of security deficiencies that were based on the accusations of a security services company whose services the lab company had declined to purchase.
- Connecticut’s attorney general states that, contrary to published reports in Politico, his office is not investigating Epic or anyone else for “information blocking.”
- A Kentucky hospital is notified by the FBI that keystroke-logging software had been running within the hospital for years, potentially exposing anything information the hospital entered via the keyboards of the infected computers.
Webinars
December 2 (Wednesday) 1:00 ET. “The Patient is In, But the Doctor is Out: How Metro Health Enabled Informed Decision-Making with Remote Access to PHI.” Sponsored by Vmware. Presenters: Josh Wilda, VP of IT, Metro Health; James Millington, group product line manager, VMware. Most industries are ahead of healthcare in providing remote access to applications and information. Some health systems, however, have transformed how, when, and where their providers access patient information. Metro Health in Grand Rapids, MI offers doctors fast bedside access to information and lets them review patient information on any device (including their TVs during football weekends!) saving them 30 minutes per day and reducing costs by $2.75 million.
December 2 (Wednesday) 1:00 ET. “Tackling Data Governance: Doctors Hospital at Renaissance’s Strategy for Consistent Analysis.” Sponsored by Premier, Inc. Presenters: Kassie Wu, director of application services, Doctors Hospital at Renaissance; Alex Eastman, senior director of enterprise solutions, Premier, Inc. How many definitions of “complications” (or “cost” or “length of stay”…) do you have? Doctors Hospital at Renaissance understood that inconsistent use of data and definitions was creating inconsistent and untrusted analysis. Join us to hear about their journey towards analytics maturity, including a strategy to drive consistency in the way they use, calculate, and communicate insights across departments.
December 2 (Wednesday) 2:00 ET. “Creating HIPAA-Compliant Applications Without JCAPS/JavaMQ Architecture.” Sponsored by Red Hat. Presenters: Ashwin Karpe, lead of enterprise integration practice, Red Hat Consulting; Christian Posta, principle middleware architect, Red Hat. Oracle JCAPS is reaching its end of life and customers will need a migration solution for creating HIPAA-compliant applications, one that optimizes data flow internally and externally on premise, on mobile devices, and in the cloud. Explore replacing legacy healthcare applications with modern Red Hat JBoss Fuse architectures that are cloud-aware, location-transparent, and highly scalable and are hosted in a container-agnostic manner.
December 3 (Thursday) 2:00 ET. “501(r) Regulations – What You Need to Know for Success in 2016.” Sponsored by TransUnion. Presenter: Jonathan Wiik, principal consultant, TransUnion Healthcare Solutions. Complex IRS rules take effect on January 1 that will dictate how providers ensure access, provide charity assistance, and collect uncompensated care. This in-depth webinar will cover tools and workflows that can help smooth the transition, including where to focus compliance efforts in the revenue cycle and a review of the documentation elements required.
December 9 (Wednesday) 1:00 ET. “The Health Care Payment Evolution: Maximizing Value Through Technology.” Sponsored by Medicity. Presenter: Charles D. Kennedy, MD, chief population health officer, Healthagen. This presentation will provide a brief history of the ACO Pioneer and MSSP programs and will discuss current market trends and drivers and the federal government’s response to them. Learn what’s coming in the next generation of programs such as the Merit-Based Incentive Payment System (MIPS) and the role technology plays in driving the evolution of a new healthcare marketplace.
Contact Lorre for webinar services. Past webinars are on our HIStalk webinars YouTube channel.
Acquisitions, Funding, Business, and Stock

Turing Pharmaceutical, which in August promised to reconsider its 5,000 percent price hike for the old but critical drug Daraprim following massive public and political backlash, will offer hospitals a discount of up to 50 percent based on usage, which would still leave them paying nearly 30 times the pre-Turing price. The company won’t offer any other discounts, maintaining the full 50-fold increase in effect for patients who take the drug at home. Meanwhile, Turing is planning another funding round that will value the company at $500 million, with an IPO to follow. Former hedge fund manager turned Turing CEO Martin Shkreli also acquired majority control of a struggling biotech company last week.
Shares of Castlight Health keep dropping, having lost 90 percent of their March 2014 IPO price in valuing the company at $380 million at last week’s closing share price. The company lost $20 million in the most recent quarter on revenue of $19.5 million.

Arizona-based lab testing vendor Sonora Quest, jointly owned by Banner Health and Quest Diagnostics, will open lab draw stations in Safeway grocery stores. Safeway spent $350 million reconfiguring 800 of its pharmacies to add Theranos draw stations, but backed out after Safeway executives questioned the methods and validity of Theranos tests. Sonora Quest has also taken advantage of the Theranos-backed change to Arizona law that allows consumers to order their own lab test, but unlike Theranos, Sonora Quest will perform tests without a doctor’s order only for tests it believes the average consumer can understand.
Sales
Cook County Health & Hospitals System chooses Chicago-based Valence Health to provide claims approval and payment services for its Medicaid managed care plan in a contract worth $72 million.

Children’s Hospital & Medical Center (NE) chooses Strata Decision’s StrataJazz for decision support and cost accounting.
People

Arthur Harvey is named VP/CIO of Boston Medical Center (MA).

IBM promotes Kyu Rhee, MD, MPP to chief health officer for Watson Health.
Announcements and Implementations
Martin Ventures-backed Lucro announces an innovation solutions marketplace that features a catalog of participating companies and user-provided ratings. Bruce Brandes is founder and CEO.
Lexmark Health and Center for Diagnostic Imaging announce a National Image Exchange for participating sites.
Interbit Data announces the NetRelay secure messaging solution.
Glytec earns a patent for its software-driven automated insulin administration method.
Government and Politics
Hawaii’s health department issues an RFP for an online medical marijuana inventory and sales tracking system that will allow tracking “from seed to sale.”
Privacy and Security
The Washington Post seems surprised that HIPAA covers only providers, meaning patients are on their own when it comes to sending their information or wearables information to non-provider websites and public databases. The article says that OCR hasn’t taken action on 60 percent of the HIPAA complaints it receives, either because they weren’t filed quickly enough or because HHS has no authority over the accused entity. A woman who used a paternity test kit that reported results on a public web page filed an HHS complaint when she noticed she could see everybody’s results and not just her own was quoted in the article as saying, “It was shocking to me to get that message back from the government saying this isn’t covered by the current legislation and, as a result, we don’t care about it.” I’m not sure what she expects OCR to do, but perhaps she should be contacting her elected representatives to consider whether medical privacy laws should be extended to all organizations and not just providers (thus my poll this week).
Technology
FDA approves Medtronic’s MyCareLink Smart Monitor, which sends a patient’s pacemaker data over their smartphone to a database that physicians can review.
Other
Athenahealth removes its Epocrates Bugs + Drugs app from the app store. It was announced in 2013 to criticism that it contained obvious errors and offered no evidence of rigorous testing or peer review. The company hadn’t updated the app since January 2014.
The bond ratings agency of Baptist Health (KY) affirms its A+ rating, but warns that its profitability and liquidity will decline in FY2016 due to its Epic implementation, investments in population health management, an unfavorable payor mix, and the subsidies it providers to its physician group. It adds, however, that Epic will produce positive returns in 2017-2018.
Sponsor Updates
- Impact Advisors offers a white paper titled “The New World of the Health System CIO: Consumers, Consolidation, and Crooks.”
- Experian Health recaps its successes in the first half of 2015.
Blog Posts
- Flashback Friday: ACEP Scientific Assembly 15 (T-System)
- Carilion Clinic Recognized for Taking Command (TeleTracking)
- Supporting Actionable FWA Investigations with Deep Data (Verisk Health)
- The Joint Commission & Trinitas Regional Medical Center Publish ‘Leading Practice’ on Portable Panic Alert System (Versus Technology)
- RSNA 2015: Faster. More Powerful. Enterprise Imaging. (Visage Imaging)
- Catalytic Communication (Voalte)
- 6 Ways to Avoid Squandering Consulting Hours (Hayes Management Consulting)
Contacts
Mr. H, Lorre, Jennifer, Dr. Jayne, Dr. Gregg, Lt. Dan.
More news: HIStalk Practice, HIStalk Connect.
Get HIStalk updates.
Contact us or send news tips online.










RE high cost of insurance bought on the exchange, my guess is that there will be a big increase in use of urgent care centers that only charge a fixed price when you go there. I have co-workers who prefer to go to places like that even with our pretty good employer-based insurance. I think lots of people would rather pay a $49 or $79 flat fee instead of $300 out of their deductible that their local provider affiliated with a large medical center charges.
Patients shuffling their insurance plans means lots of new patient visits for PCPs. Entering a new patient’s medical history into the EHR is a arduous task requiring a great deal of time, especially for the nurses and PAs. I wonder how this will impact PCP offices and wait times once patients’ new health insurance plans kick in early next year?