LOL @ Ascension. Who knew that outsourcing your entire IT department wouldn't be the best idea? I can't speak to…
News 7/29/15
Top News
An investment firm founded by Harvard professor and disruption author Clayton Christensen invests $8.4 million in ACT.md, a care coordination platform developed by Zak Kohane, MD, PhD and Ken Mandl, MD, MPH from the informatics department of Harvard’s Boston Children’s Hospital, both of whom are also on the company’s board. The advisory board includes Mark Frisse of Vanderbilt and John Halamka of BIDMC.
Reader Comments
From GraySky: “Re: [hospital system name omitted]. Will announce on July 30 that it will spin off several hospitals and its management and consulting company.” Unverified. I’ve left out the system’s name for reasons that will become apparent if the rumor turns out to be true.
From WikiStiki: “Re: Wikipedia’s hot mess entry on ‘electronic health record.’ It really needs to be rewritten.” The page is pretty much a disaster, an unfocused collection of facts (and quite a few opinions) written by people who don’t understand the big picture. WikiStiki offered to rewrite it if a sponsor will help cover some of the cost of her time, so I’m wondering if anyone thinks it’s worth doing. The page is probably read only by non-industry people, but that might make it even more important that it be accurate, timely, and clear (it’s none of those things now).
From Polite Spokesperson: “Re: startups. Another responsibility of startups is to create jobs.” Not true. Companies don’t hire people just to be nice or to bolster the local economy. The last thing I want as an investor or shareholder is for a company to pad its payroll with unnecessary employees since that just makes the company non-competitive. We’re just starting to realize in America that we have more people who need jobs than we have companies who need employees given farm and manufacturing productivity increases caused by technology (not to mention citizens who have prepared themselves poorly for decent jobs). However, I’ll return to your assertion to agree that people who find themselves unemployed or underemployed need to consider an alternative to wage slavery, such as jumping on the 1099 economy by starting a small business or contracting themselves out. People gripe endlessly about their employers, but don’t position themselves to do anything more than find another job working for someone else to be unhappy about. We don’t raise entrepreneurs like they do in hungrier countries, but that seems to be slowly changing. The future of our economy is small businesses, especially those that can turn impressive per-employee revenue.
HIStalk Announcements and Requests
Here’s how a monopoly behaves from an example I was reading about. Electric companies whose customers install solar panels are required by law to buy back any excess energy that customer generates, allowing solar customers to lower their monthly electric bills to a very low rate that will eventually offset the high cost of the initial installation. Electric companies, alarmed at the possibility of widespread consumer choice, are now lobbying to change the laws to not only eliminate the requirement that they buy customer-generated power, but they also want to charge those customers more than their actual electricity usage because they see solar users as freeloaders who use their grid without paying their fair share (the entitlement attitude is rampant among utilities). Electric companies are worried that as more customers use less of their product in favor of cheaper alternatives, they will have to spread their high fixed costs over fewer and fewer full-paying customers, feeding the cycle all over again as solar panels become even more cost effective. That’s the same problem the post office can’t figure out. You might well find similarities in healthcare. Government and monopolistic organizations never graciously accept getting smaller and instead find more desperate ways to protect their government-granted fiefdoms against declining market demand.
My Medical Records Saga Update
A reader asked for ideas about how hospitals and providers could respond more effectively to patient requests for electronic copies of their records. Send me your thoughts via this quick online form (it saves you from having to compose an email) and I’ll summarize them. My main takeaway is that records requests go to the hospital’s HIM department, which is usually clueless about anything electronic such as the hospital’s patient portal and not all that user friendly when it comes to patient requests. It’s also bizarre that a business case even exists for release of information companies to place themselves between patients and providers, but that’s another issue. Meanwhile, here’s what I came up with.
- Records requests should be automated via online form for folks who have that access and technical knowledge. PDF downloads, scanning, and faxing are not reasonable.
- ID verification should be by "what you know" rather than "what you have." No scanned driver license or form — just DOB, last four digits of SSN, address, etc. Or, use SMS messaging to send a text message to a mobile phone number and then use the generated coded to validate that the phone number is active and in possession of the requester.
- The request form (hopefully online) should be tailored specifically to patients requesting their own information, with a separate form available for other entities making similar requests.
- The form should not require medical record number (hospitals are ridiculous in making it the patient’s job to memorize their assigned MRN).
- The form should provide information for using the provider’s portal. It should offer a phone number or email address for signing up or getting a password/userID reminder (providers should like the idea of increased portal usage) and should compare paper copies, online access, and an electronic download and how to request each. It’s not reasonable that the HIM department handles medical records requests without having any knowledge or interest in their own employer’s patient portal that might be more appropriate for the patient’s needs.
- The request should open some sort of help desk ticket so it can be tracked by the patient. I can imagine patients giving up in frustration unless someone feels pressure to close the ticket to the patient’s satisfaction (possibly measured by a follow-up survey link).
- The form should include the records charges and how those are calculated. I really don’t see how a provider can justify charging for an electronic copy that surely already exists in their systems, but naturally hospitals rarely turn down the chance to create a charge.
If you want to critique your own provider, here are some ideas. Email me your experience. You don’t even need to actually make the records request – just see what’s involved.
- Is information about record requests available online where it can be easily found by patients?
- Is the form or process easy to understand?
- How does the provider validate the requestor’s ID?
- Does the request spell out what the patient will be charged for copies? Does it involve a “per page” figure that doesn’t make sense for electronic records?
- Does the request form indicate that data can be sent electronically or does it offer only paper copies?
- Does any step involve a physical trip, a fax machine, or information the average patient won’t have (like MRN)?
- Does the request form indicate the existence of a patient portal, explain why that might be a better option than requesting records copies, and describe the steps needed to gain access to it?
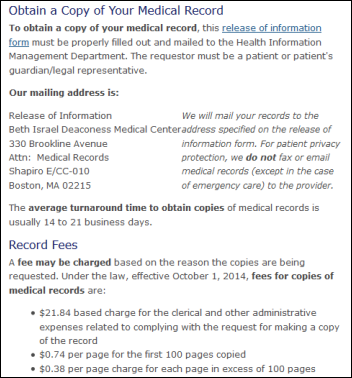
I decided to randomly choose a hospital and see how they handle records requests from patients. This is from Beth Israel Deaconess Medical Center, which accepts requests only via a mailed form and offers only paper copies of records, taking up to 14-21 business days (it’s odd to count business days in seven-day full-week increments) and costing the requestor around $600 (!!) for copies of a full chart. The “internal only” portion of the form suggests that the patient must produce a photo ID. I bet John Halamka’s IT group has nothing to do with this process and he’s probably not even aware of it since the chasm between HIM and IT is wide in hospitals.
I’ve noticed that other hospital sites say that HIPAA prevents them from providing records without the patient’s signature, meaning electronic requests can’t be accepted. I’m not so sure this is true, but perhaps a HIPAA expert can weigh in.
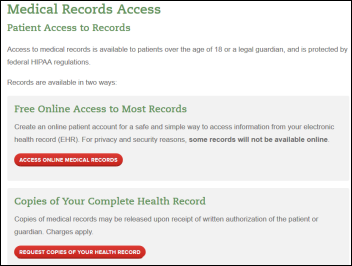
Florida Hospital’s medical records page tells patients upfront that they can get a lot of their information from their portal, to which it provides a link. Every hospital should do this. Hospitals need to get with the 21st century and realize that the HIM department is no longer the obvious and sole gatekeeper for patient records requests. All of this presumes a patient has Internet access and capability – I can only imagine the roadblocks they would find calling the hospital switchboard.
Webinars
July 29 (Wednesday) 11:30 ET. “Earning Medicare’s New Chronic Care Management Payments: Five Steps to Take Now.” Sponsored by West Healthcare Practice. Presenters: Robert J. Dudzinski, PharmD, EVP, West Healthcare Practice; Colin Roberts, senior director of healthcare product integration, West Healthcare Practice. Medicare’s new monthly payments for Chronic Care Management (CCM) can improve not only patient outcomes and satisfaction, but provider financial viability and competitiveness as well. Attendees will learn how to estimate their potential CCM revenue, how to use technology and clinical resources to scale up CCM to reach more patients, and how to start delivering CCM benefits to patients and providers by taking five specific steps. Don’t be caught on the sidelines as others put their CCM programs in place.
July 30 (Thursday) 3:00 ET. “De-Silo Your Disparate IT Systems Around the Patient with VNA.” Sponsored by Lexmark. Presenters: Steven W. Campbell, manager of diagnostic applications and interfaces, Piedmont Healthcare; Larry Sitka, VNA evangelist, Lexmark. The entire patient record, including both DICOM and non-DICOM data, should be available at the point of need. Disparate, aging systems that hide data inside departmental silos won’t cut it, nor will IT systems that can’t integrate medical images meaningfully. Learn how Piedmont Healthcare used a vendor-neutral archive to quickly and easily migrate its images and refocus its systems around its patients.
Previous webinars are on the YouTube channel. Contact Lorre for webinar services including discounts for signing up by Labor Day.
Acquisitions, Funding, Business, and Stock
NantHealth founder Patrick Soon-Shiong, MD takes cancer drugmaker NantKwest public Tuesday in the biggest biotech IPO in several years at a $2.7 billion market cap. He bought Conkwest less than a year ago for $48 million, renamed it, and kept 60 percent of shares, valuing his newly IPO’ed holdings at $1.6 billion or 33 times what he paid for the company a few months ago.
Small practice EHR vendor Kareo raises $55 million.
Israel-based home telehealth sensor vendor TytoCare raises $11 million in a Series B funding round.
Sales
Prestige Emergency Room (TX) chooses Wellsoft’s EDIS.

Covenant Health (TN) chooses Strata Decision’s StrataJazz for decision support and budgeting.

UF Health Shands Hospital (FL) selects Lexmark’s vendor-neutral archive.
The Banner Health Network (AZ) ACO chooses eClinicalWorks EHR and population health management systems.
Abbeville Area Medical Center (SC) will implement Medhost’s EDIS.
People

Jason Friedman (Ascension Information Services) joins Oneview Healthcare as VP of solutions.
Announcements and Implementations
Stella Technology announces Inspector of Quality Healthcare Data, developed with New York’s HealthElink HIE to evaluate the quality of HIE-collected data.
Government and Politics
ONC awards $29.6 million in grants to 12 state entities to expand adoption of HIEs, $2.2 million to Academy Health to create population health strategies, and $6.7 million to six colleges and universities to update HITECH’s workforce development curriculum.
Privacy and Security
A security researcher finds a flaw that lets hackers take over Android phones by simply sending a self-destructing text message, meaning all they need is the victim’s cell phone number to launch a Stagefright trojan attack that can’t be detected or prevented.
Other
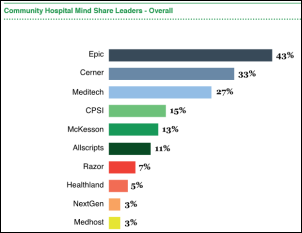
A new report from Peer60 finds that 20 percent of community hospitals are planning to replace their EHRs, with the major complaints being poor usability and missing functionality. Meditech is the dominant product, followed by McKesson Paragon, Cerner, and Healthland, but the hospitals are focusing on Epic, Cerner, and Meditech in considering new systems.
Fortune magazine seems to have dumbed itself down considerably in the past few years, but it also seems to believe its readers are getting stupider along with it as it sleuths out an under-the-covers scrappy healthcare startup called McKesson (#11 on the magazine’s own list of largest US corporations). John Hammergren surely grimaced at the writer’s obvious lack of industry knowledge in trying unsuccessfully to pose insightful questions.
In Canada, Nova Scotia stops further hospital EHR rollout amidst physician complaints about inefficiency, lack of consistency between practice and hospital EHRs, and worries that practices maintain information that they don’t share. The province issued a “One Person, One Record” RFP in April 2015 with hopes of replacing the three hospital EHRs it had previously approved, use of which the government says is “beyond what we can sustain in a province the size of Nova Scotia.”

A study finds that hospital checklists, which delivered dramatic clinical results when first introduced several years ago as described in Atul Gawande’s “The Checklist Manifesto,” often fail to deliver similar results when rolled out on a broad scale. A 101-hospital study that found no improvement after checklists were mandated suggests that the problem isn’t the concept but rather its implementation, which is dependent on rollout methods, localization, and staff resistance. In other words, as is often the case, hospitals manage to mess up projects that seem foolproof via their stubborn culture of accepted mediocrity and lack of accountability.

The CEO of UMass Memorial Health Care (MA) says the system will spend $700 million over 10 years to implement Epic, its largest capital expense ever. He adds that Epic cost 10-20 percent more than its competitors, but 500 employees voted Epic as their top choice following demos.
QPID Health posts a pretty funny video called “Squirrelnado 2, the QPID Edition” that has some fun pop culture references that include, “You’re going to need a bigger nutcracker” and the “Nut Bucket Challenge.”
Former Stanford hospitalist turned concierge medicine provider ZDoggMD creates a superb, non-humorous (angry, in fact) video called “Ain’t the Way to Die.” It should serve as a call to action for the half of my recent poll respondents who unwisely haven’t created an advance directive. You might as well do it right now since insurance companies are increasingly requiring it since they otherwise have to eat the cost of long-term ventilator care that patients probably don’t want anyway. I keep watching it over and over. A sample of the lyrics:
Let me go, I’m leaving you—no I ain’t
Tube is out, you put it right back, here we go again
It’s so insane, ’cause though you think it’s good, I’m so in pain
I’m more machine than man now, I’m AnakinBut no advance directive, I feel so ashamed
And, crap, who’s that nurse? I don’t even know her name
You lay hands on me, to prolong my life again
I guess you must think that this is livin’…
Weird News Andy is fascinated that new guidelines for healthcare mobile device security were published by NIST just as the DEA investigates the explosion of an apparent meth lab running inside NIST’s headquarters, leading WNA to question the security of NIST’s immobile devices. He also likes the article description of NIST as "the federal agency responsible for setting standards for precise measurement of just about everything.”
Sponsor Updates
- An imaging site reviews the VA Midwest’s deconstructed PACS project that includes an imaging viewer from Visage Imaging, vendor-neutral archive from Lexmark, and a work list module from Medicalis.
- Zynx Health adds Android support to its ZynxCarebook mobile care coordination solution.
- Video clinical pathways vendor ViiMed will use InterSystems HealthShare to integrate with provider EHRs.
- Voalte will hold its inaugural Voalte User Experience conference (VUE15) in Sarasota, FL on November 10-12.
- AirStrip CEO Alan Portela pens “A Ray of Hope from Washington? Don’t Rush Meaningful Use.”
Contacts
Mr. H, Lorre, Jennifer, Dr. Jayne, Dr. Gregg, Lt. Dan.
More news: HIStalk Practice, HIStalk Connect.
Get HIStalk updates.
Contact us or send news tips online.







RE: From WikiStiki: “Re: Wikipedia’s hot mess entry
If you or anyone decides to re-write it, make sure to cite all your sources using URL’s to other websites or you will probably get reverted. Additionally, if someone is sponsoring you, I would disclose that on the article’s talk page just to be safe. If any statement about the sponsor or their line of business happened to make it to the article that would be a no-no.
“A new report from Peer60 finds” The link embedded in “finds” doesn’t work. “Page not found” on http://www.peer60.com. A search on peer60.com for “community hospital ehr” doesn’t find the related article, either.
[From Mr H] Sorry, they changed the link, I’ve discovered. I changed it in the post. It should be:
https://www.peer60.com/community-hospital-ehr-2015/
Re: Electric companies. I live in a small country where the government owns and runs the only electric company, so everyone has to use it. Electricity is extremely expensive here, which means many people do not have it in their homes at all. A young couple tried installing solar panels on their house to supply their entire neighborhood since there would be plenty of excess, and the government moved swiftly to outlaw solar panels. The couple had to take the panels down. The “hypothetical” scenario you described is perfectly accurate.
Regarding checklists which “often fail to deliver similar results when rolled out on a broad scale”, isn’t this the pattern for most management fads? They appear to be an important innovation when initiated at a site that is having significant problems, but when applied to a relatively problem-free site the cost-benefit ratio does not look so favorable.
Nant…