I've figured it out. At first I was confused but now all is clear. You see, we ARE running the…
News 6/17/15
An HHIS OIG report finds that the federal government has paid Healthcare.gov insurance subsidies since January 2014 even though CMS hasn’t finished the software module that verifies the payments owed. Insurers are still submitting estimated claims that the government pays even though it can’t verify their accuracy or whether the enrollees have paid their share of the premiums. CMS sent checks for $2.8 billion in just the first four months of 2014, the period OIG audited.
Reader Comments

From Levi Kittycat: “Re: University of Virginia. Leaving Sunquest and going with Epic Beaker for lab over the next 2-3 years.” UVA posted a Beaker trainer job a few weeks back, so I assume they are indeed going in that direction. I did a quick search and found Beaker analyst positions recently listed at ThedaCare, Stanford, Duke, University of Colorado, PeaceHealth, Sanford Health, UTMB, Thomas Jefferson, OhioHealth, Wellmont, and others. The best-of-breed LIS vendors had better jump quickly onto genomics and personalized medicine before the customer demand for integrated systems shuts them out despite the complaints of the lab people who like having their own systems.
From Ed Hocken: “Re: MModal. Announced in an internal email that chief scientist and co-founder Juergen Fritsch will leave to pursue ‘personal interests.’” Unverified.

From Willow: “Re: Xerox Midas+. Developers have been ordered to work weekends for no extra pay to try to finish development of the in-house replacement for 3M’s APR-DRG coding, which has been dropped to save $3 million per year and must be finished by August.” Mandatory overtime indicates a management failure in overcommitting and underfunding resources assigned to unprofitable work (if it was profitable, they would happily bring in more help). My short stint with a failing vendor many years ago involved the occasional mandatory work weekends, with our clueless leadership exhibiting complete indifference to the family and religious activities they were disrupting through their ineptitude. However, the free market works – if the employees have better options, they are free to seek them (as did quite a few of the best folks at the vendor I worked for). You would hope that the work flexibility extends in both directions so that employees don’t have to burn PTO for occasionally leaving early or taking a long lunch for an appointment (such as a job interview with a better company). I wouldn’t be thrilled with working every Saturday for a few weeks, but it could be worse – at least it’s for a finite product delivery event rather than just offsetting ongoing inadequate staffing.
From NewHavenNighthawk: “Re: Yale New Haven. Big IT management shakeup – Ed Fisher is out and Jimmy Weeks is in.” Former YNHH VP/CTO Ed lists his current LinkedIn position as of May as being in that “between-jobs limbo” of freelance consultant.

From Ben Dover: “Re: Providence Health & Services IT. The former COO and chief of technology and service operations is leaving and his position eliminated after a number of failed projects and clinical system outages. IT has struggled to execute on the system’s affiliations and acquisitions, leading to rumors that it will revert back to the regional model.”
HIStalk Announcements and Requests
My latest gripe: sites that headline stories with Batman-like verbs (Kapow! Powie!) in describing companies that “snag” funding or hackers that “swipe” data. They probably get their coveted clicks for their low-expectation advertisers, although from readers who quickly abandon the story (and possibly the site) after realizing they’ve been baited one time too many by inexpertly written, non-clickworthy stories that were all sizzle and no steak.
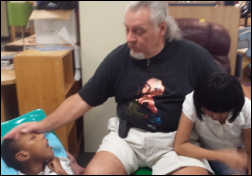
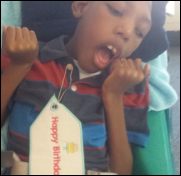
Mr. S sent photos of his South Carolina classroom of profoundly mentally disabled K-5 students, for which we provided (via DonorsChoose and matching funds from Publix) baby wipes, diapers, a blender for preparing food (some of his students can’t eat otherwise), and insect repellent so the kids can participate safely in Special Olympics.
Webinars
June 30 (Tuesday) 11:00 ET. “Value Based Reimbursement – Leveraging Data to Build a Successful Risk-based Strategy.” Sponsored by McKesson. Presenters: Michael Udwin, MD, executive director of physician engagement, McKesson; Jeb Dunkelberger, executive director of corporate partnerships, McKesson. Healthcare organizations are using empowered physician leadership and credible performance analysis to identify populations, stratify risk, drive physician engagement, and expose opportunities for optimized care. Attendees will learn best practices in laying a foundation for developing a successful risk-based strategy.
Acquisitions, Funding, Business, and Stock

CVS buys Target’s money-losing pharmacy business – which includes 1,660 drugstores and 80 in-store clinics – for $1.9 billion. CVS will rebrand the departments as CVS/pharmacy and MinuteClinic. CVS and Walgreens are pulling away from the drugstore chain pack in footprint, technology, and revenue as they diversify traditional drugstore offerings into providing extensive health services in convenient locations. I would expect grocery stores that operate in-store pharmacies (Kroger, Safeway, Publix, and possibly even Sam’s Club and Costco) to pay attention since running increasingly complicated pharmacy businesses isn’t their core competency.

Forward Health Group moves to a new headquarters location in Madison, WI.
Big insurance companies take acquisition aim at their smaller competitors that are still worth dozens of billions of dollars, with UnitedHealth hoping to acquire Aetna, Aetna eyeing Humana, and Anthem and Cigna performing a mating ritual. Reasons: (a) declining employer-provided insurance in favor of exchange and government plans; (b) the need to improve bargaining position with big and expensive market-dominating health systems; and (c) the rise in value-based care.
Former National Coordinator Farzhad Mostshari, MD’s ACO startup Aledade raises $30 million in a Series B round. It will be interesting to watch as heavier investments and the mandatory outsider board seats they require set up a potential clash between idealism and capitalism and the ongoing need for the founder to keep investors and the board happy. The industry rags are covering the story like it’s breaking health IT news, but other than Farzhad’s former job and Aledade’s somewhat related need to assemble information from its physician EHRs, it’s not all that relevant to healthcare IT in general.
CTG will take a $0.09 Q2 earnings charge after failing to convince payers to buy its end-stage renal disease management system that cost over $1 million to develop. CTG will also lay off the non-billable employees working on the product and has revised its Q2 and full-year earnings guidance down sharply. CTG is also considering selling its Buffalo, NY headquarters building. CTG shares are down 48 percent in the past year, valuing the company at $147 million.
Sales

Millinocket Regional Hospital chooses Medhost’s emergency department information system.
Florida Hospital Physician Group (FL) chooses Smartlink Mobile for its Medicare Chronic Care Management services, billing for which at $40 per patient per month requires clinical information exchange, management of care transitions, creation of a patient-centered care plan, and patient access to electronic communication.

Westchester Medical Center Health Network (NY) signs a $500 million deal with Philips for consulting services and medical technologies that “gives us access to the latest in connected digital health technologies, it will be allow us to collaborate on proactive health management and co-create new patient-centered models of care for the Hudson Valley area.” It would be fascinating to see how the actual agreement matches up to the lofty statements in the announcement, and even more fascinating to look back in five years to see how much of the deal was hype.
Weill Cornell Medical College and New York-Presbyterian Hospital sign up for electronic informed consent from Mytrus for clinical trial enrollment in their oncology clinics.
People

Spok promotes COO Hemant Goel to president. He replaces Colin Balmforth, who will “pursue other opportunities.”

Boston Children’s Hospital (MA) promotes John Brownstein, PhD of the Children Hospital Informatics Program to the newly created role of chief innovation officer.

CTG names Alfred Hamilton, PhD (George Washington University) as VP/GM of CTG Healthcare and Life Sciences. He is retired lieutenant colonel in the US Army Medical Department, where he served as a military CMIO and CIO and was deployed to Iraq to support the IT needs of two mobile trauma units.

Don Kemper, who founded Healthwise in 1975 and still serves as its CEO 40 years later, will retire in 2016.
Announcements and Implementations

Imprivata joins App Configuration for Enterprise, which is developing open standards for managing and securing enterprise mobile apps.
Patientco announces the launch of a redesigned PatientWallet, which allows patients to pay bills from any device. The announcement says, without apparent irony, that the product uses “new-and-improved technology.”
Cerner and the Commission on Accreditation of Healthcare Management education announce an awards program and scholarships that will recognize graduate programs that focus on the use of information for healthcare performance improvement.
Incident training in Elgin, IL includes the use of a cellphone app by Augusta, GA-based Global Emergency Resources that allows first responders and hospital personnel to log patient information, including photos and driver license images, so that hospital employees and other emergency teams can monitor progress.
Government and Politics
HHS seeks software developers to become Entrepreneurs in Residence for two development projects: an FDA cancer and hematology data aggregation analysis platform and a CMS system that connects providers to their Medicare interactions.
In England, NHS alerts users that its newly live e-referral service, which replaces the problematic Choose and Book system, has 33 known problems, including system delays, search problems, and reporting capabilities.
The government’s top seven contractors are, in order, Lockheed Martin, Boeing, General Dynamics, Raytheon, Northrop Grumman, and McKesson, which slipped into the defense-heavy list with its $6 billion in drug contracts.
The Senate’s HELP committee convened its second hearing Tuesday, this time on EHR user experience. Vindell Washington, MD, CMIO of Franciscan Missionaries of Our Lady Health System (LA) testified that EHR workflow and documentation requirements are based on outdated paper models and providers should instead be rewarded for patient outcomes. Tim Pletcher, executive director of the Michigan Health Information Network Shared Services, said that health plans and payers have been conspicuously absent from Meaningful Use and patients are still forced to use their portals as are providers who are asked to submit additional documentation, suggesting that health plans be encouraged by HHS to use direct secure messaging. Meryl Moss, COO of the Coastal Medical ACO, urged the government to harmonize quality measures and add data analytics criteria to EHR certification.
Privacy and Security
The FBI is investigating reports that the St. Louis Cardinals hacked into the player performance and scouting databases of the Houston Astros, which had hired the head of its “Moneyball”-type operation who apparently reused his Cardinals password on the network of the Astros, thereby inadvertently enabling the alleged unauthorized access.
A JAMIA article by Dean Sittig and Adam Wright proposes use cases of exactly what determines whether a given EHR is “open” or “interoperable,” which hopefully will squelch the bleating of robotic vendor CEOs who insist on abusing the term to mean “whatever we’re selling at the moment.” The authors also question whether a system is open if its vendor requires those who need access to its system to be certified, to sign a non-disclosure agreement, to pay a license fee, to pay the vendor for custom programming, or to buy documentation. The EXTREME (Extract, Transmit, Exchange, Move, Embed) use cases require the EHR to:
- Export patient records in a format that can be discretely imported into another system that includes enough metadata to make the information usable, with a published dictionary describing how the information is stored and what it means.
- Support the ability for users to send some or all of a patient’s information to another EHR or PHR system via a standard format, allowing the user to choose which information to send and maintaining a usable data structure.
- Respond to data queries 24×7, use a record locator service, send information in a structured format, and send its data dictionary to the receiving EHR.
- Allow a customer to move all of their patient information to a new EHR, preserving metadata and maintaining the existing transaction history.
- Provide read and write API access to clinical and administrative information, such as by using SMART or FHIR services, and store new values provided by the external application.
For more information, see the summary Dean and Adam wrote as a HIStalk Readers Write article.
Here’s a challenge to EHR vendors: is your system open and interoperable based on the definition above?
An interesting article in Wired debates whether “apps” as we know them are obsolete, with both Google and Apple developing technologies that allow apps to be accessed more like services, so that users don’t even need to open one of many apps that reside in their “bag of hammers.” A developer says companies might be forced to sell “powers” rather than “things,” explaining, “There’s a lot of startups that are features masquerading as companies, and they’ll find a better home in this world. For some transactions, it’s ideal. If you can write a perfect API, there’s no longer a need to wrap it up in an app or UI.” The downside is that big companies like Google and Apple will control the entire user experience and compete to lure users into their competitive ecosystems. The author concludes that users may not care since they want results, not services.
Other
A Cerner spokesperson tells me that the Leidos tweet and infographic claiming that “40%+ of healthcare facilities worldwide use Cerner’s EHR system” was, as HIStalk readers pointed out, incorrect (which was pretty clear given that 40 percent of the world’s healthcare facilities don’t have an EHR at all, much less Cerner’s specifically). Cerner says someone probably misinterpreted an analyst’s “global” report title as indicating that it covers the entire world. They’ve asked Leidos to correct the statement. Cerner responded quickly and apologized for the misstatement, which was nice considering they didn’t make the claim in the first place.

Hartford Hospital (CT) says proposed state budget cuts will force it to cut jobs and eliminate programs, with the health system’s CEO calling on residents to demand that Medicaid funding be restored. The most recent tax return I found for the hospital (2012) showed that it earned a $110 million profit, paid the quoted CEO $2.1 million, and had at the top of its one-year compensation list a VP who took home nearly $4 million.
It’s all about perspective: a research article addresses how states are “protecting consumers from unexpected charges,” specifically when they are billed the balance not covered by insurance, such as when they are referred to an out-of-network specialist. That’s something the federal government could address – requiring providers who aren’t covered by a patient’s insurance to state that fact and to provide an estimate of their charges. It’s infuriating to be treated in an ED, where you have no choice in the hospital’s choice of contracted service providers, and to receive out-of-network bills weeks or months later that charge non-negotiated list prices from the ED doctor or even the lab. That’s much more egregious than predatory lending practices if you ask me, especially since the providers dump the responsibility on patients who are usually, by definition, not prepared to sort it all out on the spot.
Dilbert takes on wearables.

Weird News Andy says you have to pay extra for this service at some places. A 21-year-old home health nurse in Florida is arrested after she “decided to take off her clothes and not act normally” in stripping off her uniform and attacking the elderly patient under her care. The local TV station predictably made the non-news item its breathless lead, sending a reporter to report live from the jail’s driveway. Providing competitive snark to WNA this week is @JennHIStalk, who provided the heads-up that a neurosurgeon in Italy plans to lead a team of 100 technicians in transplanting a human head in 2017, with the ailing Russian patient saying, “I hope it will be OK.”
Sponsor Updates
- Culbert Healthcare Solutions becomes a CHIME Foundation Affiliate.
- Frost & Sullivan names Validic a “Healthcare Disruptor.”
- Ricky Caplin, CEO of The HCI Group, is named EY Entrepreneur of the Year in the Florida Health Care & Life Sciences category.
- ADP AdvancedMD offers “ICD-10 billing & coding help – just in the nick of time.”
- AirStrip will exhibit at Connected Healthcare 2015 June 18-19 in San Diego.
- AirWatch by VMware is recognized as a leader in the 2015 Gartner Magic Quadrant for Enterprise Mobility Management for the fifth consecutive year.
- Practice Unite offers “Is your mHealth app HIPAA compliant?”
- Besler Consulting offers an “Update regarding HIPAA Eligibility Transaction System (HETS).”
- Bottomline Technologies will exhibit at ACE June 17-19 in Austin, TX.
- XG Health outlines “XGlearn – Care Management Training.”
- Craneware kicks off a new “value cycle” initiative at HFMA ANI 2015 next week.
- Caradigm offers “The Cultural Shift to Population Health.”
- Commvault offers “Backup-as-a-Service (BaaS) Just Became Easier with Cisco and Commvault.”
- TechOhio discusses startup success with CoverMyMeds VP of Engineering Alan Gilbert.
- Divurgent team members race to support the Children’s Hospital of the King’s Daughters.
Contacts
Mr. H, Lorre, Jennifer, Dr. Jayne, Dr. Gregg, Lt. Dan.
More news: HIStalk Practice, HIStalk Connect.
Get HIStalk updates.
Contact us online.











Can we please stop with this assertion that the ‘free market’ magically works in terms of an employer-employee relationship being a one-on-one relationship where both having generally equal leverage?
No major labor law has been passed in the US since the FMLA in ’93 and almost every U.S. labor law is seeing serious rollback/erosion across the board including overtime, worker’s comp & disability, etc. Hell, more and more workers aren’t even being called ’employees’ anymore but increasingly ‘contractors’ or other similar terminology.
A follow-up on your Hartford Hospital item:
Hartford HealthCare cutting 335 jobs, citing state, federal funding cuts
Hartford HealthCare’s announcement Wednesday said the company planned to eliminate approximately 335 fulltime-equivalent positions, affecting 418 staff members. In addition, the system is considering other changes to programs and services to reduce costs, including consolidations and reductions.
Gov. Malloy spokesman Devon Puglia said the budget required hard choices, but noted that hospitals have been profitable.
“This is a challenging budget year where difficult, often unpopular, choices were absolutely necessary,” he said. “As the state has to find new efficiencies to meet the challenging budget, the hospital industry will also have to find efficiencies to meet the changing industry. With that said, last year, the hospital industry did have one of its most profitable and lucrative years.”
http://ctmirror.org/2015/06/17/hartford-healthcare-cutting-335-jobs-citing-state-federal-funding-cuts/