There's a typo in your Oracle headline where it says "debilitating wave of layoffs."
Monday Morning Update 3/16/15
Top News
New York Governor Andrew Cuomo signs legislation delaying the state’s mandatory electronic prescribing law for one year to March 27, 2016, the same bill he giddily approved in 2012. “This is a victory for patient safety,” said plastic surgeon Andrew Kleinman, MD, president of the state’s medical society. Assembleyman and pharmacist Roy McDonald says 98 percent of the state’s pharmacies were ready to receive all prescriptions electronically, but the Drug Enforcement Administration and EHR vendors waited until too late to begin their preparations.
Reader Comments

From Jeff Steiner: “Re: Memorial Hospital at Gulfport. I wanted to respond to a story posted about our hospital’s bond rating change ‘due to a Cerner EHR conversion that inflated accounts receivable and jumped AR.’ Memorial Hospital is in the midst of exciting work and tremendous growth. We are undergoing a $65M expansion project spread over the next two fiscal years (with no planned debt). We are living with revenue pressures from Medicare and Medicaid due to changes in their reimbursement methodology. We’re a busy organization and are facing plenty of market pressures and dynamics like so many of our peers. We wanted to add clarity to the ‘100 days in A/R’ comment. This includes a mix of prior non-Cerner systems and Cerner. This snapshot was a 90 day post live look where MHG was on Cerner’s solutions at our fiscal year end. We look forward to our partnership with Cerner and a very productive relationship.” Jeff is CFO of the hospital.
From Castro’s Cousin: “Re: Banner Health. A high-placed source says it will replace Epic with Cerner at recently acquired University of Arizona medical center and clinics. Official announcement won’t drop until summer.” Unverified, but expected.
HIStalk Announcements and Requests
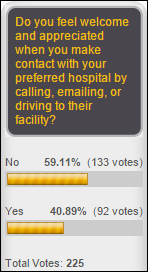
Sixty percent of poll respondents say they don’t feel welcome and appreciated when interacting with their preferred hospital. Donald says the service he gets is good because it’s a rural area, while OutsourcedMom says she feels too welcome, as in “like a spider’s web of financial ruin.” New poll to your right or here: will ICD-10 be delayed again by Congressional action? I get nervous when I see Congress talking about an SGR fix since that is where an unknown politician slipped in the last delay. It doesn’t matter what the experts think should happen – none of the lobbyists who whisper in Congressional ears have a vested interest in wanting the rollout of ICD-10.

Here’s a generous offer from HIStalkapalooza Gold Sponsor Divurgent. Divurgent gets a bunch of tickets in return for their sponsorship, but graciously offered to donate all but a handful of them them to HIStalk readers who might otherwise be unable to attend if we sell out. I will execute their largesse as follows: if you haven’t already signed up to attend, do it here. I’ll guarantee that the first 50 folks to sign up will get an invitation courtesy of Divurgent, with just one exception: I’m not going to give a bunch of invitations to people from the same company just because a secretary was ordered to sign everybody up. You might think, “Nobody would do that,” but at least two companies signed up 30+ people each to attend, which seems ridiculous since the point is to get a lot of readers there, not to have me (and the event sponsors) pay for someone’s company party. Thanks to Divurgent, who clearly is sponsoring the event to support HIStalk rather than for their own benefit.
I have a few spots left for CMIOs (or physicians working in a CMIO-type role) interested in attending a lunch with peers Tuesday of HIMSS week. It’s near the exhibit hall, so the time commitment is minimal unless you just want to hang out. The signup form is here. Thanks to the company that offered to sponsor the lunch even though I turned them down – it was a nice gesture, but I’d rather spend $500 out of my own pocket than to give the impression that I’ll do anything as long as some company pays – I get those offers pretty often and I usually decline.
Last Week’s Most Interesting News
- Apple releases its smartwatch and ResearchKit.
- Stanford University says 11,000 people signed up for one of its research studies within the first 24 hours of the release of Apple ResearchKit.
- Epic’s Judy Faulkner tells a reporter that she will sign over all of her Epic shares to her private charitable foundation when she dies or decides to turn over control, with her intention being to guarantee that the company will never be taken public.
- Two big academic medical centers in the Netherlands stop their implementation of the former Siemens Soarian, expressing concern about how Cerner might handle the product with its Siemens acquisition.
- Oregon finally shuts down its health insurance exchange, which due to technical problems never enrolled a single customer despite its $284 million cost.
- FDA issues draft guidance on using electronic informed consent in clinical studies.
Webinars
March 31 (Tuesday) 1:00 ET. “Best Practices for Increasing Patient Collections.” Sponsored by MedData. Presenter: Jason Bird, director of client operations, MedData. Healthcare is perhaps the last major industry where the consumer does not generally have access to what they owe and how they can pay for their services. Collecting from patients is estimated to cost up to four times more than collecting from payers and patient pay responsibility is projected to climb to 50 percent of the healthcare dollar by the end of the decade. Learn how creating a consumer-focused culture, one that emphasizes patient satisfaction over collections, can streamline your revenue cycle process and directly impact your bottom line.
Acquisitions, Funding, Business, and Stock

The Indianapolis business paper profiles Hc1, which just raised another $14.4 million from angel investors, increasing its total to $28 million. The 100-employee company’s revenue doubled each of the past three years and is expected to triple to $35 million in 2016. The company’s Healthcare Relationship Cloud offers collaboration, CRM, and analytics. I don’t see any healthcare experience on the executive team other than the chief medical officer – most of the folks came over from the founder’s previous company, ChaCha, which offers human-guided, text-message based search using freelancers (seemingly unsuccessfully – it looks like not much is happening there and the company has scaled back over the years). Despite a lack of healthcare background, CEO Brad Bostic seems to get it: “When I order a book on Amazon.com, they treat it like a life-or-death situation if they deliver it to me. But if I go to a healthcare situation, where it actually is life or death, I get treated like a number. This is a really big deal. It’s a big game-changer about, how do you treat patients like individuals?”
Eko Devices receives $2 million in new funding and will begin clinical trials at UCSF of its Eko Core digital extension for analog stethoscopes.
The business paper in North Carolina’s Triangle area profiles seven-employee Polyglot Systems, which raised $1.4 million in equity financing as part of its deal with First Databank to distribute the company’s medication instructions. The proceeds will be used to integrate Polyglot’s product with EHRs.
People

NYU Langone Medical Center names Paul Testa, MD, MPH as CMIO, a position he had held as interim since September 2014.

CTG hires Cliff Bluestein, MD, MBA (Dell Services) as president and CEO.
Announcements and Implementations
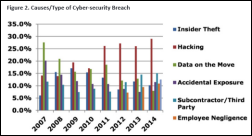
Divurgent and Sensato produce a white paper titled “Cyber-Security in Healthcare: Understanding the New World Threats.” It contains an interesting quote from a hospital CIO: “The reason no one bought your service was that, frankly, if we found out about security holes, then we would have to fix them. It is easier to react after the fact than to convince everyone we need to do something before it happens.”
Privacy and Security
Apple publishes its app store guidelines for HealthKit for human subject research. Apps will be rejected if they store a user’s information in iCloud, fail to include a privacy policy, or provide diagnosis or treatment advice. The app developer must also agree not to use data for advertising or to share it with third parties.
Healthcare IT attorney Nicholas Terry says the White House’s draft wording of the “Consumer Privacy Bill of Rights Act” may have HIPAA implications since it no longer specifically excludes HIPAA covered entities, meaning that health systems could become responsible not just for keeping the information they collect private, but for collecting it responsibly. Terry adds that the FTC’s “data minimization” concept may clash with ONC’s interoperability efforts and could limit selling data to third-party brokers. The proposed policy would be enforced by FTC and the attorneys general of individual states. The bill would also preempt the laws of states that may already have stronger privacy laws on the books given that it doesn’t specifically prohibit selling consumer information to data brokers without their permission.
Other
Philly.com’s story on unemployment in the Malvern, PA area originally contained wording suggesting that Cerner is laying people off after its acquisition of Siemens Health Solutions, but for some reason that section of the story was removed and no Cerner reference remains.
A West Health Institute poll of nurses about medical device interoperability concludes (via the mandatory cute infographic) that almost all nurses say they would spend more time with patients if freed up from dealing with medical devices and think those devices should share data with EHRs automatically, while half of the nurses say they’ve seen a medical error due to lack of device coordination. Nurses, not surprisingly, think their own uninterrupted time is the most important factor in improving patient safety and most of them think that manually documenting device information creates errors and delays. West Health calls for ONC to add medical device information sharing to its interoperability roadmap, for FDA and HHS to recognize open standards for medical device communication and to provide guidance to manufacturers, and for Congress to provide “adequate incentives” for developing and using interoperable medical devices.

Stanford physician and author Abraham Verghese says in his keynote to the American College of Cardiology that doctors should rediscover the humanity of practicing medicine and the non-technical benefits of the medical encounter ritual, saying that EHRs have obliterated the stories of patients as the typical ED physician spends nearly half of their time working on a computer. He explains, “EMR has nothing to do with your heart or your patient’s heart.”

The local paper covers the financial woes of Southeast Health in Cape Girardeau, MO. Billing problems caused by the hospital’s Siemens Soarian implementation as well as that system’s $15 million per year operating cost earned it a bond ratings downgrade in 2013. New CIO Mike Nichols is planning to take advantage of the Siemens acquisition to move to Cerner Millennium. The health system spells their name “SoutheastHEALTH” in the apparently misguided belief that marketing by misspelling is the secret to organizational success. You have to squelch the creatively bankrupt marketing people when they babble nonsense like the words they put in the former CEO’s mouth for the hospital’s annual report: “This is not simply an evolution in name alone. We are a far-reaching network of providers and facilities uniting to provide a regional system of healthcare services.” Sounds good except they’re going broke as they lay people off, with the board chair explaining, “Back here, in the old model, we got paid for doing things. In the future, that’s not how a hospital will be paid. Unfortunately, we are sitting in a spot in the middle, because that model hasn’t been explained to us yet.”

Doctors in France protest health reform, unhappy that under proposed changes they’ll be paid by insurance companies instead of having patients hand over cash directly. They say insurance companies will control both doctors and patients and doctors don’t have the clerical staff to manage the reimbursement paper trails. Patients now pay $25 in cash for a visit and are reimbursed by either the social security system or the patient’s insurance company. A doctor who is leading the protest warns that France’s healthcare system, which he says is the best in the world, will “end up like in the UK” where patients who don’t pay upfront don’t mind wasting the doctor’s time “for any old reason.” He adds, “If we change the system, it will be whichever insurance company pays me, who is responsible. The Social Security service will say to me, Mr. Henry, you are prescribing too many antibiotics. You are prescribing too many pills and sending people for too many tests. They will tell me I have to prescribe less. I will no longer be free to ask the question, what is the best thing for the patient’s health? I will no be longer be independent.”
Sponsor Updates
- Medicity publishes “The Challenges and Benefits of Interoperability.”
- Xerox Healthcare publishes “Survey Says: Your Patient is Unhappy.”
- Voalte asks that “Nurse Leaders, Please Step Up!”
- PMD covers “The ‘Choreographed’ Care Model.”
- Oneview Healthcare highlights the ways in which a “New Study Establishes that Activated Patients Cost 31% Less.”
Contacts
Mr. H, Lorre, Jennifer, Dr. Jayne, Dr. Gregg, Lt. Dan.
More news: HIStalk Practice, HIStalk Connect.
Get HIStalk updates.
Contact us online.








Something of interest I thought I would bring around here is the fact that major news paper media companies are now going to use and some have invested in to begin charging you 20 center to read some articles. The only problem here is that so many news articles are now written by bots, so 20 cents to read bot news and it will be sent to your credit card, so more data for the credit card folks to sell so the behavioral analytic folks can really go nuts with trying to profile you even down to what articles you pay for so we have a “two fer” here. Papers get money and data selling credit card companies get more data to sell as it’s a $180 billion a year business.
Naxnex and I, who’s in the news all the time about how high frequency quants cheat with code figured this out months ago and even MIT not too long ago had an article on the bot news as those journobots can act and react with stock bots:) There’s a big fight and one got busted for releasing news sooner that the public gets is so one more way to “rig”. I don’t fault the news paper media companies as they are looking for money and starving due to the cash rich greedy public companies in a midst of huge stock buy backs that won’t toss a little more ad money to the papers. NYT and WSJ are in on this.
One of the jounobot companies said their software wrote over a billion articles last year and he maybe a bit heavy on the numbers but they are out there in groves, so now I’m careful when I comment as I want a human to read it, not a bot, but either way I’m sure I get profiled both ways:) Just give this some real thought as the parameters of the news can be set to react with what the stock bots do and hammer out tons of articles that could sway trading. Nanex candidly said “where do these bots get their news, they are not out there like an investigative reporter and probably are scanning blogs like ours for content”…it just never stops. I really noticed this when I read several articles on the Supreme Court decision when it was pounding the air waves recently that all the articles really started sounding very similar or the same in content:)
http://ducknetweb.blogspot.com/2015/03/major-us-newspapers-sign-up-and-invest.html
Again we want humans out there and not an entire force of bots, otherwise you might as well just suck up and see what Facebook decides to put in your news feed:) I’m just saying be aware of what you read in the news out there as these bots are getting good and the potential for news rigging is alive and well and probably out there to some degree already. Forbes, ProPublica and AP sure love their journobots. Journobots are ok if they take a spreadsheet or a bunch of other boring stats and make a story for a staff meeting or just some boring stat news and they do a good job there but it’s beyond that now. The most astounding jounobot is LongTail where the creator wrote over 100k books and put them on sale with Amazon, so you know (little satire here) why don’t we just line these bots up to do EMR records next (grin). That comment may come back to haunt me some day:)
Why do you have to post such garbage? MedicalQuack is a good name.
Does anyone else picture MedicalQuack typing up these posts in a basement with cut out magazine words and glue sticks all around her?
France doctors are certainly on to something…I hope they are successful in stopping “progress”.
Truly horrifying stuff, @MedicalQuack. Perhaps you can educate us on the evils of chemtrails next time? Thanks in advance.