RE the AI GLP1 company, Washington Post has an article today by someone who used one of those compounded products,…
News 1/16/15
Top News
PwC adds Google to its Department of Defense EHR bidding consortium that is pitching the VA’s VistA. Google joins, PwC, General Dynamics IT, DSS, and Medsphere. Google’s contribution would be collaboration and search tools, which seems to be more sizzle than steak as PwC tries to make VistA sound sexier to the DoD, whose contempt for that system is legendary. The group has also put up a web page to make its case.
Reader Comments

From Weird News Andy: “Re: Iowa health insurance startup, the second-largest co-op in the country and heavily funded by the federal government, fails. The key is in this quote: ‘CoOportunity Health’s pool of people was larger than expected, was sicker than expected, so their risk became much greater than the funds that were available.’ That’s an economics lesson. Sicker people spend more and choose the one that saves them the most money, so you end up with a pool of sicker, more expensive members. If the founders of the organization did not see this going in and did not charge enough for their service, the fault is theirs. But then if they charged more, fewer people would select them and …” That’s a big problem with medical insurance. The fingers of insurance company actuaries fly over their Excel worksheets in their attempt to assemble a customer base that includes lower-risk, healthier patients to offset the expensive ones so they can bid competitively. However, individual patients sign up expecting to use more services than they’re paying for, to the point of not even buying insurance until they’ve accumulated enough problems to make it worth their while. It’s like a buffet restaurant eyeballing prospective diners at the door in trying to choose a profitable mix of picky eaters and starving chowhounds for a predetermined price, but their downfall is that few picky eaters will pay for an all-you-can-eat buffet knowing they’re subsidizing those who inhale everything in sight.
From RVA: “Re: concierge medicine. My PCP is moving to concierge practice, saying he doesn’t want to use Epic and that he can’t provide good care because his face is always in the computer ((FYI, he cashed his MU check). The concierge company touts their USB chart that allows you to take your important clinical information anywhere — apparently MyChart was not good enough (the guy sitting next to me joked that when they run out of USB drives, they’ll switch to 8-track tapes). He has approximately 1,200 patients (mostly Medicare) and a poorly-managed practice. They showed a scary video about how doctors are ‘forced’ to give up their practices and referenced the use of ‘mid-level providers’ in a negative way. A lot of people ate it up and started pulling out their checkbooks – oh, he has limited capacity, so it’s first-come, first-served at $2,500 per year. I’m worried that we’re creating a class system where those who can’t afford the fee get less than premium care.” It’s tough to ignore economics by suggesting that those who pay less should receive equally generous, excellent, and responsive healthcare services, even though we as decent people wish that were possible. All of us working in healthcare expect to be paid, so unless we turn it back over to the nuns and counties that ran hospitals as true non-profits using cheap and volunteer labor, those days are likely gone. The ED is the last foothold of healthcare democracy, where everybody is treated the same based on need, but then again, it’s a cost cesspool for that reason and hardly a poster child for open access to all. Healthcare economics is like a balloon – squeeze it in one place to cut costs and another part bulges out as providers who are understandably unwilling to reduce their personal standard of living figure out new ways to charge for their services. We’re at three tiers now: (a) those who use ED and public clinics or who don’t buy insurance because they don’t see the immediate value; (b) the large middle class who have insurance but are getting hit hard by out-of-pocket costs and sometimes facing bankruptcy because of huge and often questionable bills, with that group subsidizing the first one by paying excessive charges and taxes; and (c) those whose assets are adequate to self-insure and whose time is valuable enough to make it worth finding the best and most customer-friendly providers who don’t take insurance. It’s unrealistic to expect the care and outcomes to be identical across all three groups. It’s also reasonable to expect people in the middle group to move down rather than up, and it’s the loss of that group that threatens to implode the system. It’s just like the tax system: some percentage of people pay nothing, the wealthy pay a low overall percentage because of their small numbers and large accounting tricks, and those in the middle foot most of the bill.
HIStalk Announcements and Requests
Last year right before the HIMSS conference I supported Donors Choose by offering companies a large, short-term banner that appears beside the HIStalk title on every page, using the proceeds to fund a bunch of projects for classrooms in need. It felt good and it was fun, so I’m doing it again this year. Contact Lorre if you’d like to book the most prominent ad on the page and help needy students in the process. Like last year, I’ll write up the projects we funded and share the student comments and photos that result.

I followed through on a reader’s suggestion of an HIStalk Book Club sort of thing where I review an HIT-related book and invite readers to share their thoughts. I reviewed Eric Topol’s “The Patient Will See You Now” and next up is “America’s Bitter Pill.” Read along, add your thoughts, and suggest what book I should read next. I have a copy of John Halamka’s “GeekDoctor: Life as a Healthcare CIO” that HIMSS sent me in return for completing a survey, so maybe that should be next.
I’m sure we’ll see this at the HIMSS conference: every hip meeting now includes a “graphics facilitator” who documents everything on a flipboard, compelling attendees to proudly tweet out photos of the drawing afterward. I don’t want to attend a conference where a cartoonist understands the presenter better than I do.
Here’s one last appeal for you to complete my once-per-year HIStalk reader survey, which takes just a couple of minutes but helps me immensely.
This is a fond farewell to Agilum Healthcare Intelligence, whose marketing person told us, “I’ve never even heard of HIStalk” in declining to renew their sponsorship after many years. They’ve been supporters for a long time and I appreciate it. I also appreciate the service of the marketing guy, who though he has zero health IT experience, is a former Army infantry captain who led a field artillery battery in Iraq, according to his LinkedIn profile.
This week on HIStalk Practice: Telehealth reimbursements are set to go live in New York. Tulane University Medical Group implements eCW’s CCMR. Etherapi takes advantage of the Kaiser strike in California. HHS breaks down its own silos, and enjoys flying first class. Dr. Gregg looks into the future of healthcare IT, circa 2037. Third-party patient portals go head to head with vendor-specific options. Thanks for reading.
This week on HIStalk Connect: 23andMe finds a new source of revenue as it closes a $60 million deal with Genetech in which it will use its dataset to support Parkinson’s disease research. Athenahealth acquires cloud-based inpatient EHR vendor RazorInsights, and confirms that it will move into the hospital space. Augmedix raises $16 million to scale a promising Google Glass-based telecharting business.
Acquisitions, Funding, Business, and Stock

Todd Cozzens of Sequoia Capital is featured on Fox Business’s “Opening Bell” live from the JPMorgan Healthcare Conference. He mentions his firm’s investment in Health Catalyst (analytics) and MedExpress (retail clinics). A Forbes profile of Sequoia Capital mentions its 40-plus year history, including its 1980 investment in Apple’s IPO (the founder thought the 22-year-old Steve Jobs “looked like Ho Chi Minh”) and its recent gains from Airbnb, Dropbox, and WhatsApp. The firm’s partners make a fortune, apparently, as the article mentions a 2003 fund that returned gains of 41 percent per year for 11 years, with the firm’s partners pocketing $1.1 billion as “Sequoia is turning its own partners into billionaires while keeping outside investors purring.”

I mentioned that Athenahealth has acquired small-hospital EHR vendor RazorInsights for a rumored $40 million to give it an inpatient foothold. I really like what RazorInsights is doing in giving small hospitals an inexpensive, cloud-based system that covers both clinicals and financials, but I don’t see the benefit to Athenahealth in buying a four-year-old company with only a couple of dozen small customers. RazorInsights has much larger competitors (Meditech, CPSI, Medhost, NTT DATA, McKesson Paragon, etc.) with established infrastructure and most hospitals have already spent their money on a Meaningful Use dance partner, some of them even choosing to run Epic or Cerner as provided by another hospital (or to be acquired by those hospitals). Athenahealth has choked on its previous acquisition Epocrates, which is highly regarded but is stumbling even more than before under Athenahealth’s ownership. I think Athenahealth wants desperately to crack the inpatient market (after insulting that market for years), realizes it doesn’t have the expertise to build a new hospital system from scratch, and decided to spend money instead of time to get a name-plated product quickly to market and then ramp it up. The challenges are many:
- RazorInsights is small for a reason and not being owned by Athenahealth may not be it.
- Both product and company scalability are unknown.
- Few big companies have low-enough overhead to profitably roll out products to cash-strapped 25-bed hospitals.
- Expected synergies may (as they often do) prove to be elusive.
- Companies have been historically lured into unwise acquisitions because the product aroused them technically and filled a perceived immediate need at high expense (Allscripts buying Eclipsys).
I think Jonathan Bush will talk this up as though Athenahealth is the next Epic (or Salesforce or whatever high-flying comparison comes to mind), but the acquisition is just another distraction as the company tries desperately to keep its Wall Street plates spinning in the air despite concerning profits and a year-long share price stall.

Aetna announces that it will raise its minimum wage to $16 per hour in April and will offer an enhanced insurance plan for employees who participate in wellness programs starting in 2016.
Two former NantHealth executives file a whisteblower lawsuit against billionaire doctor Patrick Soon-Shiong’s company, claiming that NantHealth is “engaged in a multitude of fraudulent activities,” violates HIPAA requirements, has failed mock FDA audits, and offers products that harm patients. Stephanie Davidson (former SVP of professional services) and William Lynch (former senior director of marketing) also claim that several customers were prepared to stop using the company’s Clinical Operating System, citing an internal report that characterized that product as “10 years behind in technology capability” that “runs on LUCK.” The pair claims that NantHealth’s marketing material is misleading and that Soon-Shiong’s charitable foundation defrauded Medicare by donating millions to a hospital that would then use CMS matching funds to buy NantHealth’s products. NantHealth’s responds that the employees, who are in a romantic relationship and had worked for the company for only a few months, demanded that NantHealth pay them $2 million to prevent them from launching a pre-IPO smear campaign after NantHealth fired Davidson. Perhaps it’s not a coincidence that the lawsuit was filed just as Soon-Shiong gave the company’s investor pitch at the JPMorgan Healthcare Conference.

Craneware says second-half sales for 2014 increased 10 percent and its board is confident of meeting 2015 expectations.
Sales

Good Shepherd Health System (TX) chooses Strata Decision’s StrataJazz for decision support and cost accounting.
Healthfirst (NY) selects InterSystems HealthShare as its HIE and clinical portal.
Providence Health & Services expands its relationship with Kyruus, which offers a doctor web search tool. That’s how I would describe their business, anyway, but if you don’t get enough buzzwords, here’s theirs: “Kyruus is an enterprise healthcare provider solutions company that helps health systems optimize their Patient Access, Referral Management and Care Coordination operations. Leveraging the cloud and a proprietary Big Data approach, the company enables the integration of massive amounts of information to create a single source of truth of providers. Kyruus helps health systems create customizable protocols for referral and scheduling across all channels of patient engagement to improve patient access and patient experience.”
People

Ralph Keiser (Deloitte) joins Recondo Technology as chief growth officer.

John Glaser (Siemens Healthcare) joins the board of the American Telemedicine Association.

Hayes Management Consulting hires Gay Fright (Coastal Healthcare Consulting) as VP of strategic services.

Huntzinger Management Group promotes David DiChiara to CFO.

Sachin Jain, MD, MBA (Merck) joins care plan CareMore as chief medical officer. He worked for ONC for a short time a few years ago. He said in a talk last week that most health IT startups offer products that are interesting but not really useful because (a) they’re trying to make a quick buck, and (b) they are mostly run by young, prosperous, healthy people and develop products in the context of their peers rather than for the sick, expensive patients that need help. He also said HITECH came about because everybody knew EHRs were good for patients, but hospitals put the interest of their resistant doctors first because they’re the ones who admit patients.

Ken Pool, MD, co-founder of OZ Systems and co-chair of the HL7 Public Health and Emergency Response Work Group, has died, according to a posting on the group’s listserv.
Announcements and Implementations
An article by Brad Swenson of Winthrop Resources Corporation suggests that the total cost of ownership of hospital EHRs should use a 10-year forecast rather than the more common five or seven years. It quotes The Valley Hospital (NJ) VP/CIO Eric Carey, who used a 10-year timeframe to make an upgrade-or-buy decision: “We felt no one should be replacing an EHR platform in less than 10 years unless a catastrophe happens. Also, probably the most expensive part of an EHR project is the army of consultants, staff, and project managers you need to have to pull everything together. Our implementation has involved 20 FTE over at least one year. Most organizations can’t afford to do that more than once.”
McKesson announces Paragon Community Plus, a package that includes its Paragon system, implementation, training, and remote hosting.
A House Committee on Energy and Commerce work group creates a draft policy that would require HHS to pay for telehealth services at the same rate as in-person visits within four years.
Innovation and Research
Philips gives MIT researchers access to the de-identified records of 100,000 ICU patients who were monitored via its eICU program. The records, which represent about 10 percent of all US adult ICU beds, include vital signs, medication orders, lab results, and severity of illness scores.
Technology

Google stops public sales of Google Glass and moves the product from its research lab to a separate business unit led by former fashion and eyewear designer Ivy Ross. Companies and developers will still be able to buy Glass units after the January 19 cutoff date. Google was supposed to release a new version of Glass in 2015 but hasn’t provided specifics. People seem to think this is the beginning of the end for Glass, but I’m not so sure: it desperately needed a reboot, graduation from beta status, and design help for its ugly form factor (which is true of most things Google), so perhaps this is its graduation into the real world, or even away from the consumer market and into the enterprise one.
A guest newspaper article by the CEO of a Missouri public policy organization says the state is still #49 in economic growth despite being one of nine labeled as “the corporate welfare kings of America.” He says of the Missouri’s $1.6 billion subsidy of Cerner’s $4.3 billion new campus, “If Cerner needs a corporate pleasure dome, it should pay for it on its own nickel.”
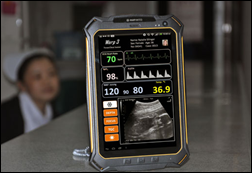
I thought sure this was a spoof since it was heavy with Star Trek puns and one of the pictures features a nurse wearing a 1970s-style cap, but apparently the just-started IndieGoGo campaign for the $3,500 Warp 3 Medical Tricorder is for real. It’s not the X-Prize, Scanadu-type consumer Tricorder, though – this China-based one will be just for doctors and will provide vital sign, ultrasound, and EHR functions.
Other

The local paper says that MultiCare Health System (WA) is not only represented on the advisory group IBM and Epic put together to help make their case to the Department of Defense as it selects its $11 billion EHR, but MultiCare will also serve as the pilot site should the IBM-Epic bid be chosen.

A physician’s New York Times editorial observes that 24 of the 141 medical schools in America are now named after big donors, causing graduates to be “embarrassed that there was a rich person’s name on their diploma, with the university name tucked below in small print.” Naming rights cost from $8 million (East Carolina University’s Brody School of Medicine) to $200 million (UCLA’s David Geffen School of Medicine, above).
Sponsor Updates
- Imprivata integrates its Cortext secure communications platform with the Citrix XenMobile enterprise mobility management solution.
- HealthTronics selects AirWatch for enterprise mobility for its 500 employees.
- ZeOmega is named as one of the 100 fastest-growing Dallas companies.
- John Stanley of Impact Advisors is quoted in a San Diego newspaper’s article on the pros and cons of EMRs.
- Divurgent will participate in the HIMSS East Tennessee Summit in Knoxville on January 22.
- DataMotion covers the important role e-mail plays in file sharing in its latest blog.
- CompuGroup Medical will participate in the Critical Care Congress in Phoenix, AZ from January 17-21.
- CommVault expands its relationship with NetApp to offer integrated data protection solutions.
- TechGig outlines CitiusTech CEO Rizwan Koita’s predictions for 2015 healthcare technology trends.
- CareSync publishes a new blog on the importance of taking charge of a family’s health records.
- Dignity Health VP/CMIO David Lundquist, MD offers insight into how to keep patients in mind when discussing the future of healthcare at AirStrip’s Mobile Health Matters blog.
- ADP AdvancedMD offers “4 surefire signs you need a new EHR for MU2 and beyond” in its latest blog.
EPtalk by Dr. Jayne

It’s been a strange couple of weeks for me. We’re getting ready to go through some major changes at our hospital and everyone is on edge. Teams are being consolidated and it feels like the directors and VPs are playing a giant game of “Go Fish” only instead of cards, they’re playing with people. This comes right on the heels of our hospital’s push to reduce the number of accrued vacation days on the books, which had almost half of our employees taking significant time off during the last month or so.
Everyone is overworked and cranky as we try to make decisions based on forecast scenarios and half-developed plans. Sometimes we start to feel not only like the sky is falling, but that the world is burning down around us. We imagine it can’t possibly be this bad in other places. It’s difficult to reach out to colleagues at other organizations because we don’t want to admit that our own organizations are in frantic disarray.
It was in that frame of mind yesterday that I was trying to catch up on the ridiculous thing that is my inbox. I’m on staff at another hospital that’s not part of my health system. I almost got whiplash doing a double take at one of the emails I received. It was discussing the final steps of a system conversion they’ve been working on for years. They’ve been running dual platforms for the last six months during the transition and are finally pulling the plug on the legacy application.
Despite the robust features of the new system, the email wording left something to be desired. “Many fixes and enhancements have been done to NewApp to make it usable.” The email was sent out under the CMIO’s banner. Knowing him as I do, I’m pretty sure that’s not what he intended. I forwarded it to one of my colleagues – not as a way to humor ourselves at someone else’s expense, but as a confirmation that the people at our competitor across town are likely under the same pressures as we are. No matter how hard and how many long hours we work, things are falling through the cracks.
I thought about how fortunate I’ve been that during most of my time as a CMIO I’ve been surrounded by colleagues who are competent, confident, and motivated. I’ve always felt like they have my back and in turn I’ve had theirs. Over the last year and a half, however, it seems that everyone has been stretched thinner and thinner. We’re to the point where we can barely support ourselves, let alone each other. Although we’re certainly experienced in delivering the impossible, it’s become harder and harder to make it a reality.
Looking at the last few months in particular, not only has our energy been sapped, but we’ve lost some of our support structures. Our standing team meetings have been fragmented as we’re pulled in countless directions by competing demands. Those were our opportunity to update each other on our projects, potential risks, and needs. We received feedback and encouragement as well as ideas to remove blockers or handle difficult situations. Colleagues who had been in similar situations provided pointers and tips and lists of “gotchas” to look for.
I should have taken that email as a warning to stay vigilant. By the end of the day today, I watched one of my key projects go off the rails. In hindsight, I should have seen it coming, but I didn’t. Although ultimately it’s no one’s responsibility but mine, I can’t help but think that if we weren’t all so scattered and overwhelmed that someone else might have picked up on subtle signs that I missed. I spent most of the day with an impending feeling of doom and heartburn that made me want to eat a box of chalk.
I realized that given our current state of being overextended, under-resourced, and fatigued that it’s likely this isn’t going to be the last time something like this happens. This is an uncharted place that I’ve never had to operate in before. I’m officially working without a net and it doesn’t feel very good. But given the state of our industry today, I’m sure I’m not alone.
Do you have tips for how to work without backup? Email me.
Contacts
Mr. H, Lorre, Jennifer, Dr. Jayne, Dr. Gregg, Lt. Dan.
More news: HIStalk Practice, HIStalk Connect.
Get HIStalk updates.
Contact us online.







Why are you thanking someone that clearly shared insider information on athenahealth? I don’t know if you or the insider traded on that information but sharing that information was illegal. I’m sure it tickled your ego to have an inside scoop but wrong is wrong, and should not be thanked.
[From Mr H] I don’t know if they are an insider or if they made any trades since the report was anonymous and quite possibly purely speculation on their part, but all I did was make a mental note and tweet out that an unnamed company was rumored to be making an unnamed acquisition. I don’t invest in individual stocks — I’m a mutual fund man. I only mentioned it to encourage readers to send me anonymous information that I CAN use. But you are right – while I appreciate that readers send me stuff, I don’t want anyone to think that I want insider information on publicly traded companies, so I’m removing that item and you were right to call me out on it.
Re: MultiCare
I believe the pilot (IOC in DoD terms) is Madigan Army Medical (whom MultiCare already shares records with), regardless of who wins the bid.
Love for Epic these days is like love for Reagan in the 80’s. Don’t get it on either end.
HAHAHAHA NantHealth. I know, I shouldn’t laugh since, if true, these system deficiencies could end up harming patients. But ever since our Chief Innovation Officer convinced our organization to enter an agreement with NantHealth for not-yet-developed technology that will only integrate with our EHR data in their wildest dreams, I’ve been waiting to see the company go down. I just don’t see how someone can trust a promise and a charming billionaire doctor over proven EHR technology that, while certainly having its flaws and limitations, actually works on a day-to-day basis.
Hip hip hooray to Aetna! There may be hope for us yet…