I was born roughly 2 months after the US space program began (Explorer 1), and I've followed it all my…
Monday Morning Update 1/12/15
HLM Venture Partners, which made several health IT investments in its first three funds, is raising up to $150 million to launch a fourth fund. Its portfolio companies include Nordic Consulting, Aventura, Medicalis, Phreesia, and Teladoc.
The investment challenge, it seems to me, is that in the frenzy to throw money at unproven healthcare IT startups, we’re well past the wheat and deep into the chaff. It’s good that demand for new technologies seems strong, but too many no-name companies confuse the market and many of them will fizzle out quickly. Companies that are thrown together purely to chase money usually don’t find it and there’s only so much proven management talent to go around. Incubators and accelerators are encouraging a lot of shaky startups that will experience the inevitable Darwinism. Still, a few of them will avoid enough minefields to get market traction or sell out to a bigger player.
Reader Comments
From Frustrated Surgeon and Developer: “Re: big health IT. Epic and Cerner are using strong-arm techniques to counter any move to interoperability. Congressman Dave Camp (MI) testified before Congress that he was being pressured by lobbyists paid for by Epic to remove interoperability from MU 2 ( and now 3) to secure their business position. Cerner said they weren’t interested in interoperating with my cloud-based system that several hospitals are using. APIs and licensing fees never came up — they just won’t do it. Cerner’s representative to ONC’s Jason Task Force is pushing hard to stop MU 3 interoperability requirements. We should not look to Epic and Cerner to open the doors. We need a HIE which Epic, Cerner, and all other permitted applications should use. It’s the data, not the application.” Unverified. I searched the Congressional Record for Epic-related comments by Dave Camp (who is now retired) but didn’t see anything relevant, although the search isn’t exactly Google quality.
From Jack Gutenberg: “Re: HIStalk book club. You should invite readers to read along and add their comments to yours.” I like the idea. I’m just starting Eric Topol’s “The Patient Will See You Now” in case anyone wants to start it along with me and then add their comments once I’ve posted mine. I’m not only interested in critiquing the book itself, but also discussing the interesting ideas inside. Books I’ve summarized here previously include “Connected for Health,” “Your Medical Mind,” “Safe Patients, Smart Hospitals,” and “Where Does It Hurt?”
From The PACS Designer: “Re: Windows 10 browser. Rumors have been swirling for months about the next version of Windows 10 and its browser style since Internet Explorer and Bing have such a small market share compared to Firefox. The leaked browser is called Microsoft Spartan.”
HIStalk Announcements and Requests
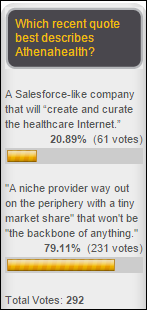
More than three-fourths of poll respondents agree with a popular stock expert’s characterization of the Athenahealth as a “bubble stock” that won’t be “the backbone of anything” rather than the company’s stated high-flying ambition to be the Salesforce of healthcare. New poll to your right or here since I ask every year: what are your HIMSS15 attendance plans compared to HIMSS14?
Ready for your input: the HIStalk reader survey and HISsies nominations. Thanks for participating. I’ll also randomly draw three reader survey responses for a $50 Amazon gift certificate.
I was thinking about Uber’s surge pricing model, where the app tells you in real time that local demand is high and you’ll have to pay more. I’m frustrated when I get that message, but it makes perfect sense from a supply and demand point of view. When cars are in short supply, the higher price does two things: (a) it allows price-sensitive consumers to seek alternatives to Uber such as taking a cab or walking, increasing Uber car availability for those willing to pay more; and (b) it encourages more Uber drivers to get out on the road and start picking up fares. (obviously it does a third thing: it raises Uber’s profits, so you have to trust them to proclaim surge pricing only when they really are swamped). An Uber model would work in medicine if it were a pure science instead of an art and if people actually paid cash for their services – you could have doctors willing to provide telemedicine consults at a given time and price via an Uber-type service and let patients decide what it’s worth to them, with an app setting the intersection of supply and demand. That leaves those unable to pay out of the picture, but medicine is already heading toward a two-tier system where cash-paying patients have better options anyway.
Last Week’s Most Interesting News
- IBM and Epic enhance their DoD EHR bid pitch by announcing that they’ve already installed an Epic model instance in a DoD-hardened environment for testing and also formed an advisory committee.
- Walgreens adds health management, real-time health coaching, and wearables connectivity to its website and mobile app, offering users reward card points for using the tools to meet their health goals.
- The AMA says EHRs, ICD-10, prior authorization, and Medicare fraud detection are barriers to care that it will target in 2015.
- Sue Schade of University of Michigan Hospitals and Health Centers wins the Gall CIO of the Year award.
- Analytics vendor Inovalon files for a $500 million IPO.
- Allina Health and Health Catalyst announced an analytics technology and quality improvement partnership, explained by Allina President and CEO Penny Wheeler, MD in my interview.
- Only 24 percent of respondents to my poll said their impression of HIMSS is positive.
Webinars
January 13 (Tuesday) 1:00 ET. “The Bug Stops Here: How Our Hospital Used its EHR and RTLS Systems to Contain a Deadly New Virus.” Sponsored by Versus Technology. Presenter: John Olmstead, RN, MBA, FACHE, director of surgical and emergency services, The Community Hospital, Munster, Indiana. Community Hospital was the first US hospital to treat a patient with MERS (Middle East Respiratory Syndrome). It used clinical data from its EHR and staff contact information from a real-time locating system to provide on-site CDC staff with the information they needed to contain the virus and to study how it spreads. Employees who were identified as being exposed were quickly tested, avoiding a hospital shutdown.
Acquisitions, Funding, Business, and Stock
Francisco Partners makes an unspecified investment in Olathe, KS-based revenue cycle solutions vendor eSolutions.
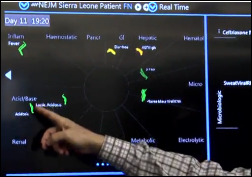
The Columbus paper profiles Lyntek Medical Technologies, whose PatientStorm Tracker software provides a weather radar-like display of an inpatient’s overall condition. It’s being beta tested by OhioHealth Riverside Methodist Hospital. Founder and pulmonologist Lawrence Lynn, DO says the outdated fire alarm model of medical monitoring systems doesn’t provide useful information until vital signs hit specific limits. He adds, “You can be in the hospital dying of sepsis with a smartphone in your pocket that can detect the pattern of a song just by listening to it, but this sophisticated-looking monitor above you can’t detect a single pattern of evolving death.”
Sales
Atlantis Health Group chooses Influence Health’s Navigate population health management solution.
People

UMass Memorial Medical Center (MA) appoints Pam Manor, RN, MSN, DNP (St. Francis Hospital) as chief nursing informatics officer.

William Hersh, MD (Oregon Health & Science University) is named the winner of the 2014 HIMSS Physician IT Leadership Award.


Streamline Health promotes David Sides, who has been with the company for five months, to president and CEO. Sides, on the left above, replaces Bob Watson, who will leave the company to become president of NantHealth but will remain on Streamline Health’s board. NantHealth announced in November that it will use Streamline Health’s analytics product in its system.
Government and Politics
The American College of Physicians urges Congress to: (a) repeal Medicare’s SGR formula; (b) continue Medicare’s 10 percent bonus for primary care; (c) restore the Medicaid program that pays primary care physicians no less than Medicare rates; and (d) provide relief from “burdensome and unrealistic” Meaningful Use requirements and “other excessive regulatory burdens.”
An opinion piece slated for publication in Academic Medicine examines whether it’s ethical for medical students to use an organization’s EHR to track their former patients so they can match outcomes to the students’ original diagnosis and treatment. The authors conclude that the benefits outweigh the harms. I couldn’t agree more – it’s hard to believe that an intelligent argument could be made otherwise. The opportunity would only arise in teaching hospitals and I see no potential ethical or HIPAA conflicts since patients understand that their treatment has an educational component. The practice should not only be allowed, it should be mandatory, and perhaps not just for medical students. Medicine (and ancillary fields) are literature-based and that always involves aggregated, de-identified research, but what could be more educational than seeing how your care decisions impacted a particular patient’s life and whether your actions were ultimately right or wrong? The patient has to live with the impact, so why shouldn’t the professionals who made those decisions? It would also be interesting to look at a patient’s overall perception of health and well-being (perhaps via a self-survey with results trended over time) instead of just a problem list if we’re really interested in improving their lives and not just their medical conditions. We have to leave the “treat ‘em and street ‘em” mindset behind.
The Wall Street Journal runs an essay by Eric Topol, MD titled “The Future of Medicine Is In Your Smartphone” in which he again predicts that technology will alter the patient-physician relationship, reduce costs, and empower patients. He thinks that doctors will still have a role, just not as today’s paternalistic “priestly class.” He has vested interests, however, even going beyond pitching his new book: he lists consulting engagements with Google, AT&T, Walgreens, Quanttus, and Sotera Wireless. A skeptical WSJ commenter weighs in: “I am in atrial fibrillation, now what? That is the rub. All these carnival barkers for the utopian vision of the smartphone/connected world are simply exhausting. For all its many benefits, the Internet is rife with misinformation when it comes to healthcare and the burden is now shifting to the consumer to sort out what is real and what is bogus.”
Ebola vaccine researchers face a surprising challenge: a sharp drop-off in the outbreak could make it hard to find enough victims to test new vaccines.
Sponsor Updates
- HCI Group CMIO William Bria, MD will present at IMN’s HealthIMPACT Southeast on January 23 in Tampa.
- Passport/Experian Health will exhibit and present at the HFMA Region 11 Healthcare Symposium January 11-14 in San Diego.
- nVoq releases a case study on the success Teleradiology Specialists (AZ) experienced with its SayIt cloud-based speech recognition technology.
- SCI Solutions VP of Business Development Bill Reid shares his thoughts on price transparency and how to equip patients with the right tools to understand the financial consequences of care.
- Netsmart will participate in the New York Coalition of Behavioral Health Agencies conference on January 27.
- Patientco outlines three healthcare finance game-changers for 2015 in a new blog.
- MedData will participate in the ACEP Reimbursement Trends and Strategies in Emergency Medicine Conference in Las Vegas from January 13-15.
- RazorInsights will exhibit at the Texas Hospital Association Annual Convention in Austin January 22-23.
- PMD recaps the previous week in healthcare in a new blog post.
- Nordic Consulting offers a new white paper, “Beaker Lab: Planning for Meaningful Use Stage 3.”
Contacts
Mr. H, Lorre, Jennifer, Dr. Jayne, Dr. Gregg, Lt. Dan.
More news: HIStalk Practice, HIStalk Connect.
Get HIStalk updates.
Contact us online.





The thought of many VC firms “throwing lots of money” at start ups that are sure to fail is absurd. Healthcare IT is replete with opportunities to improve interoperability, workflow, patient satisfaction and physician use. Epic and Cerner physician use and EMR offerings are clearly “first generation” design with significant limitations. Compound this with their arrogance regarding interoperability and you have a near perfect setting for next generation solutions.
This guy is totally bogus.
Both Cerner and Epic sat at ONC last week and championed interop.
This guy may have and idea for an app that might help and could make a buck or two only if Cerner and Epic did a bunch of hard work to enable their pure genius in their products.
When does this end? Whey doesn’t Mr. Frustrated Surgeon and Developer create an EMR of his own and do the work necessary to be successful.
Are we destined to become a nation of whiners and lame complainers?
… sorta like how Zoho has dislodged Microsoft’s Office Suite.
Regarding Uber and healthcare: The comment “That leaves those unable to pay out of the picture, but medicine is already heading toward a two-tier system where cash-paying patients have better options anyway.”
Medicine is not heading toward a two tier system , if it was I would jump on board. Health care has and always will be a multi-tier system. The wealthy get the best of the best and the rest is trickle down healthcare like trickle down (aka leak on you) economics. I know this because I have been in health care for several decades and how we care for the sick hasn’t changed. I have watched how hospitals and physicians have given phenomenal care to the wealthy, adequate care to those with adequate insurance and ignored the poor until they got caught – then give barely adequate care.
Medical professionals are not inherently equipped to properly navigate medical information systems, just because the information is not contemporary. Which is to say that data abstraction, reporting mechanisms and oversight of data governance do not automatically disappear when a service provider desires retrospective awareness because of previously performed activities. Since researchers, administrators and medical professionals currently conform with regulations and constraints, it would seem logical that service providers align themselves with current operations and not rely on past performance to justify data investigations. I believe conversationally it boils down to “Who owns the patient data?”
Perhaps “Training” facilities could train service providers on these topics rather than circumvent information mechanisms by broadly brushing things aside. Perhaps (who would know?…) contemporary limits to data access are there for a reason that was learned the hard way and might be easily taught, rather than hardly learned.
About Uber-ization: “consumerization” is hitting health care in (at least) two ways right now– in people picking plans with varying degrees of patient responsibility; and once a deductible-structure is selected, in the consumption of services.
Both are a bit weird, as far as rational economic agents go. Patient responsibility should be framed as a kind of “first dollar” responsibility. The catastrophe occurs and maximum-out-of-pocket kicks in. That being said, it appears that for many that MOOP is still a bankruptcy event, that demands negotiation. So, a certain kind of calculation occurs.
Agency in the consumption of services operates under a similar convoluted logic. What is the cost of the *next* service I am consuming. What is the perceived benefit? How is the limitation of risk, both financial and medical, valued as a benefit? If I roll the dice, and forego a service because of its immediate cost, how much does the cost for the (unlikely) occurrence of the remote adverse event fall on me, the agent doing the choosing. And, when I meet the deductible, does my thinking change? Rationally, it probably should.
So, uberization is an interesting notion for medicine. Does it really apply, except in niche use cases?
On the somewhat scary side, what happens in a true public health emergency and capacity doesn’t match demand? How does surge pricing on very, very brick and mortar-based services help? How do ICU beds or ventilators “surge”? There is a process for handling these situations, but it is called “triage”– a form of rationing.
Perhaps niche is unfair. The segment of current service where capacity could surge is probably not small, but how much of it is truly essential, and how much of it would survive if primary care was paid on a population basis?
Stray thoughts, about real opportunities to rationalize medical care…
Randy Bak, MD JD
If “medicine is already heading toward a two-tier system where cash-paying patients have better options anyway”, should we just give it another uber push in that direction?
Or should we maybe step in front of the train (tank)?
Echoing what was said above, I’m surprised that anyone would say that Cerner is in any way “countering” moves toward interoperability, since they’ve been a fully participative, committed member of CommonWell since before day 1. Dr. McCallie has been a vocal supporter of interoperability and his colleagues have been an indispensible part of the development of the platform.
Uber is a ridiculous comparison as is Amazon or a host of other incredibly poor and nonsensical analogies to the healthcare system. We are already at a two-tier system according to a Bankrate survey:
“Only 38% of those polled said they could cover a $500 repair bill or a $1,000 emergency room visit with funds from their bank accounts, a new Bankrate report said. Most others would need to take on debt or cut back elsewhere.”
Just look at the wealth measurement numbers from the McKinsey or Fed report from last year. We’re already at a level of wealth inequality that ranks us towards the bottom of the OECD too.
http://www.economicgreenfield.com/2015/01/09/financial-condition-of-many-americans/
Re: Frustrated Surgeon and Developer:
If you have a best-of-breed lab system and Cerner, you will know how much they DO fight interoperability. The LIS conforms to MU, using HL7 2.5.1 to properly format required elements to outbound DOH systems. The LIS has successfully interfaced to the state department of health, but somehow, Cerner refuses to take the same data for MUAR as they are on older HL7 and will not budge. Their answer: you have to convert to the enterprise Cerner LIS to meet MUAR.
It makes no sense to convert our ability to meet laboratory MURR Stage 2, going backwards in HL7 and in LIS technology. Cerner must not only get in the CommonWell sandbox (talk), but they should also ACTUALLY play with others (action). Hard to believe? Not really… especially if you live with it.
“Internet Explorer and Bing have such a small market share compared to Firefox”
Okay, ‘yes’ Bing has a small market share compared to Google, but Firefox has only 15% of the browser market share compared to MS Internet Explorer’s 58%. With Chrome steadily advancing, Firefox is fading into obscurity.
jamadan
TPD stands corrected IE is not small market share, but many who have IE that they got from Microsoft use other browsers so that 58% share is questionable.