You are so absolutely right. But all these issues were there before AI became a big thing. Sothis is all…
Monday Morning Update 11/24/14
Top News

Beth Israel Deaconess Medical Center (MA) will pay $100,000 to settle a state complaint over the 2012 theft of a laptop that contained the health information of 4,000 employees and patients. The attorney general said the hospital broke the law in failing to encrypt the device. CIO John Halamka says the hospital has since started encrypting all devices and requires employees to verify annually that their personal devices are encrypted.
Reader Comments

From Sam Lawrence: “Re: CommonWell. I read through their website to understand what exactly they offer and was unsuccessful. Tons of reference to ‘services’ and appears to be written entirely in vague marketing-speak. What can the two endpoints exchange? CCDAs? Discrete data? If so, what data? Can it be viewed and pulled directly into the EHR at either end? Do users have to query for data or is it passively making connections behind the scenes? Maybe this is coming, but instead of some fluff quotes, I’d like to understand what the provider actually gets and how it’s helpful.” Their website has specific use cases and refers to documents that members receive, so I assume it’s really just non-members who are still in the dark. CommonWell gets a pass for their hastily prepared HIMSS13 publicity rush, but for a group that talks a lot about transparency and openness, they aren’t very good at either when it comes to explaining their business model, technology, and the status of their offering to the industry as a whole (they’re kind of like Epic in that regard, in fact). The latest announcement looked like a committee-edited PR fluff piece. I suppose that’s inevitable when you ask several EHR vendors to collectively agree on anything. Loftily stated benefit to mankind notwithstanding, I fully expect that McKesson and Cerner expect to make money or gain competitive advantage from their participation, so I would just like them to say so.
From Donald: “Re: health IT consulting. We’re seeing a huge downturn. Rates are down a bit and opportunities are way down. Every consultant and recruiter I’ve talked to says the same thing.”
From Mr. Ron Anejo: “Re: health IT consulting. The market is dead. Very few large implementations remain, providers aren’t chasing MU $, and uncertainty surrounding possible repeal of the ACA has Medicare heavy hospitals and health systems freezing spending. In speaking with many consultants, they’re terrified because recruiters are no longer calling them 10 times a day with offers and aren’t sure how long they will be without work. Supply (consultants) definitely outweighs demand for services right now — consulting firms should be able to drive down pay rates and hospitals should push for lower rates.”

From Deborah Kohn: “Re: ICD-10 phase-in. I contacted Sue Bowman, AHIMA’s Senior Director, Coding Policy and Compliance (Public Policy & Governmental Relations), who confirmed and articulated what I suspected. Per Sue: It’s not just a matter of accepting both code sets – someone has to process the codes, be able to analyze and compare data, etc. With different providers on different code sets, it would be a nightmare. And there is also the matter of coordination of benefits. Our healthcare delivery and reimbursement systems are too inter-connected to allow different entities to use different code sets for the same date of service.” CMS is abound with botched, expensive IT projects (Healthcare.gov being just the most visible one), so I wouldn’t be optimistic that the checks will keep flowing without interruption. Here’s a free tip for mainstream reporters looking for a big story: start sleuthing around in the spring to see how confident CMS’s contractors and project people are about their ICD-10 readiness and how thoroughly they’ve tested. I bet they, like providers, just moved on to something else while waiting out the year-long delay.

From Jello Biafra: “Re: CareTech Solutions. Has it been sold to Mr. Madhava Reddy?” Weekend confirmation is hard to get, so I’ll stick with facts: (a) the Federal Trade Commission approved on November 20 the acquisition of CareTech Solutions, Inc. by Madhava Reddy; (b) Madhava Reddy is president and CEO of IT/BPO outsourcer HTC Global Services; and (c) both companies are located in Troy, MI.

From Dan: “Re: Dr. Oz. Invites fans to send him questions via Twitter, getting gems such as ‘I just got my flu shot — when can I expect to develop autism?’" America’s favorite daytime TV huckster doctor should have known better to take to the Twitterverse given the flack he takes for touting bizarre miracle drugs and refusing to have his children vaccinated. My favorite questions asked of him: (a) “What has been your most profitable lie for money so far?”; (b) “Is snake oil gluten free?”; and (c) “Why have you not been censured or fired from Columbia Surgery for conduct unbecoming a physician, scientist, and gentleman?”
From The PACS Designer: “Re: Office 365 sharing. The Garage Series for Office 365 ProPlus highlights a nice upgrade called shared computer activation, which can enhance productivity for multiple users of any computer.” It uses Remote Desktop Services to allow multiple users to connect to the same remote computer simultaneously to run Office 365 ProPlus programs like Word or Excel. It was announced using hospital nurses as an example.
HIStalk Announcements and Requests
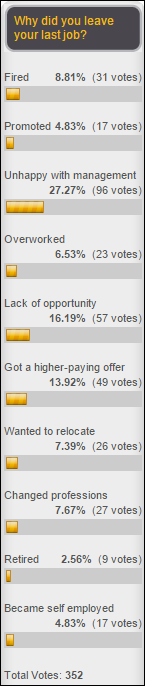
Most poll respondents left their most recent jobs because of problems management could have resolved, with 50 percent saying they didn’t like management, were overworked, or lacked opportunity. A surprising 9 percent said they were fired from their last position. New poll to your right or here for hospital or practice people: how much IT consulting will you use in 2015 vs. 2014? Vote and then click Comments to explain – I’m curious about what seems to be a consulting downturn and I’d like to learn more.
Some interesting comments from last week’s poll:
- Laid off. Other hand-picked layoffs included people who had worn out their welcome at the company after on-the-job injury, bereavement, and of course, cancer.
- Competition was eating our lunch nationally, and their response was to constantly cut staff and raise prices; classic short-term thinking.
- The software company where I worked for many, many years sent me to India to train developers. After I returned, the company decided they didn’t need the experienced local staff and our jobs were outsourced to India.
- I left, not because I was unhappy or underpaid at my last job, but because I saw an large challenge in my new job… this new job came a’-calling and the offer was intriguing. Essentially the same money, but in a warmer climate. The job though was to start a program from scratch, accelerate it as quickly as possible. I wanted to see if I could do it.
- When I turned in my notice, management went after me. They contacted Epic to look into if I might be trying to go into consulting. Epic found I was. My management told them to blackball me in an attempt to get me to stay. The job which I was to start in a few weeks disappeared. The site and recruiter were told by Epic that they could not do business with me since I was leaving an active installation, which was untrue.
- Individuals in management roles tended to be those who stuck with the company the longest, rather than individuals who were talented or forward-thinking. There was no official training that management received, as far as we knew, so most managers didn’t know how to grow their team members or keep them at the company (most managers had no idea how to handle HR issues either, like what to do when an employee told them they wanted to quit).
I was frustrated at not being able to see a journal article because it’s behind the paywall of a for-profit journal publisher. My conclusion: journals should continue providing a service in vetting and editing submitted research articles, but perhaps the authors should pay a submission fee and let everybody read the resulting article for free. That would serve several purposes: (a) it would reduce the number of crap articles that are accepted only because the journal is desperate for content; (b) journals could stop accepting ads if they haven’t already, or they could all start running ads as long as the editorial process is separate; and (c) human knowledge would be diffused to everyone, not just high-paying subscribers. That’s especially true of articles written from government-sponsored research or by government employees: why should I as a taxpayer have to pay to see them? It’s the author that gets bragging rights and personal benefit, so let them pay. I’d also like to see an impartial panel of experts grade the methodology, originality, and applicability of each article, which might shame sloppy authors or journals into not wasting reader time.
Listening: new from Gerard Way, the former singer of My Chemical Romance. Not bad, although MCR was a lot better.
Last Week’s Most Interesting News
- CVS Health announces plans to open a 100-employee technology development center in Boston that will create consumer-engaging technologies and work with health-related startups.
- EHealth Initiative’s “2020 Roadmap” calls for the federal government to refocus Meaningful Use on interoperability, get EHR vendors to offer API access to their systems, and align federal agency interoperability efforts.
- Cleveland Clinic creates Adeo, a for-profit company and website that will sell software developed by it and academic medical centers in the Healthcare Innovation Alliance.
- Emdeon announces that it will acquire consumer engagement tools vendor Change Healthcare for $135 million.
- A Salesforce blog post describes how Johns Hopkins Healthcare is using its platform to manage high-risk patients, seemingly confirming a big healthcare push by the company.
- UPMC takes a $9 million gain by selling a procurement systems software company it created to a private equity firm.
Webinars
Webinar recordings recently added to YouTube:
Improving Trial Accrual by Engaging the Digital Healthcare Consumer.
Cerner Takeover of Siemens, Are You Ready? Vince and Frank have hit over 1,000 YouTube views in four days, giving them a good shot at surpassing Dim-Sum’s all-time record.
Government and Politics

Karen DeSalvo tweeted out this farewell photo with Jacob Reider in a nice gesture. They have something in common: both are doctors who used to work full time for ONC.
Technology
US News profiles Health Heritage, developed by NorthShore University HealthSystem (boy, do I hate that multiply conjoined words name created by marketers run amok – why create a dumb name that 99.9 percent of your customers couldn’t spell in a bar bet?). It’s a genomic decision support system that combines family history to information from Epic, developed by the founder of Apache Medical Systems. Of 3,000 people who signed up and downloaded their NorthShore information, 13 percent were flagged as being high risk for cancer.
Other
An Advisory Board survey lists the reasons doctors are worried about retail clinics:
- They will siphon off the profitable and more easily managed simple cases.
- Patients don’t understand the value of provider continuity and will seek convenient access instead.
- Retail clinics will move up the food chain in offering ever-expanding services that threaten the medical group model.
My reaction as a patient:
- If a practice can’t survive without cranking through expensive but mindless sore throat and fever encounters that trigger an automatic (and often clinically inappropriate) antibiotic prescription, then we have too many practices.
- Providers haven’t in most cases demonstrated the value of continuity to their patients, treating each encounter like an impromptu hooker visit where the patient describes what they have and what they want in 10 furtive minutes of bartering and eventual consummation of a clumsy balance of compassionate care and bare-knuckle capitalism.
- If retail clinics can threaten the overpriced, underperforming, and often patient-indifferent healthcare system and that system refuses to change, then I’ll happily go to Walgreens or CVS where I get treated like paying customer and can park for free close to the door. I feel perfectly safe as long as the provider (whether it’s a PA, NP, or telemedicine doc) knows when to turf me off to experts when they’re in over their head.
It’s really odd to me that retail clinics made a big splash, were seemingly on the verge of extinction, and now are seen as a big threat to entrenched providers (the “odd” part being why it took so long).

Florida’s Blue Cross Blue Shield company installs a HealthSpot telehealth kiosk in its Miami center to allow members to access doctors from Miami Children’s Hospital. HealthSpot even did a nice job Photoshopping MCH’s logos onto stock photos of its device.
In Canada, a Montreal newspaper’s editorial says Quebec’s EHR project is “an abysmal failure,” adding that its health minister agreed in an interview. The project was supposed to cost $500 million US and be finished by 2010, but is now targeting a $1.4 billion cost and 2016 completion date. The editorial blames the variety of EHRs that were approved (nine for practices, four for hospitals) that can’t exchange information.

Weird News Andy says this article on the privacy-invading possibilities of 90-minute DNA criminal profiling creates should also have addressed potential medical uses, such as finding genetic disorders that mimic MS or identifying people with genetic sensitivity to warfarin or chloroquine.
Contacts
Mr. H, Lorre, Jennifer, Dr. Jayne, Dr. Gregg, Lt. Dan, Dr. Travis.
More news: HIStalk Practice, HIStalk Connect.
Get HIStalk updates.
Contact us online.



re: journal articles behind paywalls — I’ve had some success in finding such articles using the google scholar search engine; just search on the full name of the article’s title. Note that sometimes it takes a week or two for the article to show up, after some kind person “hosts” the article – often in another country. Try: http://scholar.google.com/schhp?hl=en#
I don’t understand AHIMA phase in for ICD10 answer. When I send in my claim for payment, I have NO idea what the hospital or other consultants are using as ICD9 codes. So why not carry both sets, they can accept ICD9 or 10 and make payments based on either. Sorry they will have to do some programming to get the data matched but hey, its better than a hard date with no end to end testing.
Re: retail clnics – they’re as close to concierge medicine as some folks will get. That also has the practices nervous.
Also – I can’t tell you the last time I felt hassled by the front office, financial, or checkout staff of a retail clinic. My practice visits – well… I find joy in askng for costs at check in, refusing to provide ID, fill out forms, and asking for my notes at check out.
I mean what’s the point in having a practice, staff, and an established patient if you’re not going to use them meaningfully. Forget the emr – I love getting on webmail and getting some work done on the exam room pcs while I wait. Best way to screw with the staff.
“Re: health IT consulting.” Nothing lasts forever. Healthcare IT consultants needed to keep an ever-watchful eye on the future. Our special niche is no different than the greater job market. One must be able to adapt to changes or end up unmarketable.
Regarding the HIT consulting market, if your business is mostly Epic, the market is not in your favor. There is plenty of business out there regardless of what the government does. To remain relevant in any business the senior leadership team has to be looking out 6 to 9 months into the future. It’s about having the right services, right people and list of positive outcomes for clients that helps sustain your business. As with any industry demand and focus changes.
With many of the firms up for sale or saying the business is drying up, their heads were down counting their cash and not looking forward. I look forward to the day of some normalcy back in the market.
Re: retail clinics
There is so much packed into this situation and your comments, which is neither good/ bad or right/ wrong, but illuminating about the need to pay primary care differently–and what happens when you do.
Under FFS and the need for face-to-face visits to get any revenue at all, the practice never got paid enough to for encounters that generated a lot of work beyond the exam room: acutely ill patients who needed the health care system mobilized now; chronically ill/ complex patients who needed many parties coordinated. Getting paid “too much” for simple cases balanced that out, so that at the end of the day/ week/ quarter/ year, the enterprise could keep the lights on and the participants motivated.
Retail clinics peeling off the higher margins face-to-face visits breaks that model. They don’t claim to handle the negative margin cases, and don’t really want to, despite gestures in that direction. And if the result is more conveniently getting a face-to-face visit for problems that don’t require that visit (and an unnecessary Rx/ placebo treatment that, surprise, is sold one aisle over), then no real efficiency is created.
If we get to population payments into primary care enterprises and don’t mandate a face-to-face encounter to trigger revenue, then we begin to rationalize things. What is more convenient than going to the retail clinic and its great mall parking? Not having to go anywhere to be under the care of your doctor/ clinic.
With recent developments in lab tech and other “mobile health” devices, there could still be great utility in health services in retail locations. Moreover, the primary care organization that manages a health care budget for a population might still want the services of retail clinics in many use cases. Indeed, the future may entail owning as little brick and mortar as possible.
The real distress here is the need for all of us to move on to a model that gets primary care off of the FFS model.
@JR Bak, Re: Retail clinics – BINGO.
“One of our most important obligations to the American people is to report information and data accurately,” HHS Secretary Burwell.
Perhaps there’s room for everyone to take that seriously; seems for the more marketing-minded, there’s the preferred view from 10,000 feet up and words like “Folks”, “Innovative” and “Interoperability”.
IMHO: if you don’t cry about accuracy, you don’t know what it feels like to be accurate, or put another way: 1st clue you’re inaccurate is when it doesn’t hurt and you stop crying… so if you can say “Accuracy” with a smile, welcome to marketing.
I’d hate to be a company that didn’t exhibit drop-dead accuracy for at least a decade, but in light of what it takes, I’d hate to be a company that did. (either way, I’m a hater)
Re: CommonWell and Sam Lawrence’s questions,
Sam, the full specifications of CommonWell’s services (and use-cases ) are available on the CommonWell website: http://www.commonwellalliance.org/specifications/
I will try to address your specific questions to save you the trouble of reading the specs!
CommonWell endpoints exchange documents, using the standard IHE XCA protocol. Typically vendor members are exposing and exchanging CCDAs, but they can chose to expose and exchange any document. At present, discrete data must be encoded into the CCDA for exchange, but as soon as FHIR is widely deployed, CommonWell plans to offer direct exchange of discrete data, optionally bypassing the CCDA.
Each vendor member is responsible for integrating access to CommonWell services into their products. Typically access to CommonWell is provided inside the EHR’s regular clinical workflow, and usually supports “data reconciliation” options to pull data out of the CCDA and into the local EHR. The mechanisms to do that are controlled by the each individual vendor.
Each vendor can decide when to query CommonWell. It can be “on demand” or it can be triggered by external workflow, such as an appointment schedule. That’s up to the vendor to decide.
CommonWell’s value comes mainly from the patient identity management service (enrollment and MPI) and the record locator service (RLS.) These two together make it as easy as possible to provide access to a “virtual” distributed health record (albeit, currently limited to documents.)
CommonWell is open to any EHR vendor. The CommonWell pilot is finished, and they are just now deploying production services so the network is still fairly small, though expected to rapidly expand.
I hope that helps,
David McCallie MD / SVP Cerner