Giving a patient medications in the ER, having them pop positive on a test, and then withholding further medications because…
Monday Morning Update 8/18/14
Top News

Epic President Carl Dvorak testifies at an ONC HIT Policy Committee interoperability governance subgroup hearing. Some of his points:
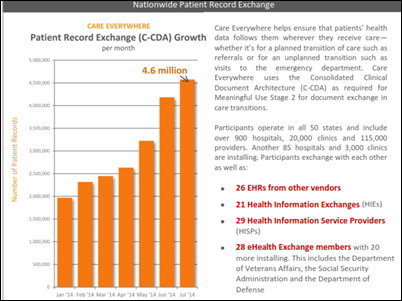
- Epic’s Care Everywhere exchanges 4.6 million C-CDA documents each month with 26 non-Epic vendor systems, 21 HIEs, 29 HISPs, and 28 government agencies. Its connections to other organizations carry 20 billion transactions annually to 88 public health agencies, 18 research societies, 51 immunization registries, and 17 research registries. This, Dvorak says, portrays a broader definition of interoperability than just exchanging patient summary documents.
- Dvorak said providers who receive Meaningful Use money should be required to participate in a national list of exchange-ready participants.
- Epic recommends that Meaningful Use Stage 3 add eHealth Exchange standards for unplanned transitions of care.
- Epic suggests allowing multiple trust verification services since DirectTrust is too expensive for some organizations.
- Dvorak says data exchange should be simplified for data used only for patient treatment and not for the “payment and operations” part of HIPAA where information is often sold or redistributed to business associates.
- Epic says ONC should give patients control of information sharing with a simple opt-in/opt-out option and let patients who want finer control to use their own personal health record instead.
- Epic customers are reporting that state and local HIEs are demanding payments that exceed their connectivity value and that some are trying to pass laws requiring providers to pay their full fee just to access state immunization registries. Epic says immunization and public health reporting should be free to users and paid for by the states, and providers in states that refuse to do so should get an exemption from those Meaningful Use requirements.
- Epic urges ONC to be wary of “political agendas and commercial competition” in assessing interoperability, adding that if ONC wants to get a true picture, they should encourage health care systems to voluntarily report their interoperability statistics directly to ONC.

Also testifying at the subgroup meeting, CORHIO Executive Director Morgan Honea said one practice was quoted $50,000 to connect to its network. He also said independent providers and small health systems should get Meaningful Use money for connecting to HIEs since they have little incentive otherwise.

Tim Burdick, MD, CMIO of OCHIN, said that data are tethered to one EHR and one patient portal, giving an example of a cancer patient who has to log into the patient portals of six organizations to see her information, then send messages to the other five asking them to update their EHRs. He says that most of the 22 states in which OCHIN operates have their own technical standards and they are often outdated, vague, or impractical (example: data standards for immunization registries required 15 different interfaces.) He said that his organization struggles with connecting to specialized registries as MUS2 requires because not only is every state different, some registries are run by drug and device companies and require each participating doctor to pay a monthly fee or make them agree that the patient data they submit can be sold or used for any purpose. He says it’s hard to match Direct addresses to specific providers because some of them work for multiple organizations and it’s not clear whether each role has its own Direct address or what happens when that doctor stops working at that location. He finished by suggesting that ONC rate organizations that are using HIE best practices, which he calls “Yelp for HIE vendors.”
Reader Comments
From HIErarchical: “Re: new insurance company-sponsored HIE in California. This has CalRHIO 3.0 written all over it. The program came from the president of UCLA, where former CalRHIO head Molly Coye, MD is chief innovation officer. She has surfaced to restart what was thrown out in 2010.” CalRHIO’s ambitious California-wide RHIO plans were thwarted in early 2010 when the state created a new entity that paired CalRHIO with a competitor with whom it had fought over HITECH money. CalRHIO, like former National Coordinator David Brailer’s Santa Barbara project, talked a lot but accomplished little – it brought one county’s EDs online. The chair of the newly created Cal Index HIE, which is funded with $80 million from Blue Shield of California and WellPoint’s Anthem Blue Cross, is the president of UCLA’s health system.
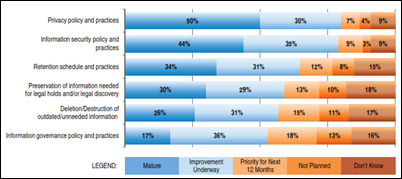
From Information Governor: “Re: information governance. I’m curious whether organizations have an information governance policy as described by a recent AHIMA white paper.” AHIMA recommends that hospitals define information as a critical business asset that is managed using published standards and the appropriate resources. Two-thirds of survey respondents said their organizations haven’t developed that kind of strategy. The most interesting part to me was the information life cycle management of electronic information, including accuracy, access, protection against loss, preservation for legal holds, managing data deletion, and plan for technology obsolescence. Actually, maybe even more interesting was the section on information controls: documentation requirements, downtime planning, data definitions, software testing, how information is corrected, and how data quality is measured. The survey went out only to AHIMA members, which may have skewed the results. Leave a comment if you’d like to describe your organization’s efforts.

From Lodi: “Re: EMRs and quality improvements. You are a hospital IT person. Why do you always question study results proving that EMRs improve care?” Because the studies prove no such thing. It’s appalling to me that the people who conduct those studies, many of whom have a vested interested in being EMR cheerleaders, misstate their results as proving causation rather than correlation. Clueless reporters then add another layer of obfuscation by writing punchy but flat-out wrong headlines. I believe that hospitals using EMRs have better outcomes. I also believe that hospitals that have bigger profits, prettier buildings, cafeteria sushi bars, and showcase helicopters also have better outcomes. I’m throwing down a challenge to anyone who claims EMRs improve outcomes: show me your data.
HIStalk Announcements and Requests
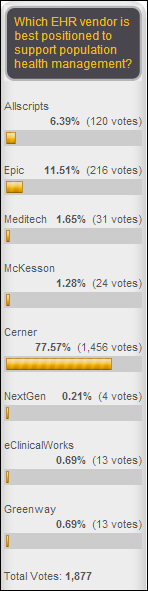
Cerner handily won the vote of which EHR vendor is best equipped to support population health management, although the IP addresses of respondents suggest that a huge percentage of the nearly 1,500 votes it received came from inside the company. Cerner contacted me to say they didn’t encourage ballot box stuffing, but non-Cerner voters nonetheless left scathing poll comments upon seeing the results, one of whom suggested giving the win to Epic by default (who also had some homers clicking away, with 62 of its 216 votes.) Let’s move on to a new poll to your right or here: is it a good deal for Cerner to buy the Siemens HIT business for $1.3 billion? Vote and then click the Comments link to expound further. Add some insightful comments and I bet some healthcare publications will use the results for further articles since information is otherwise scarce.
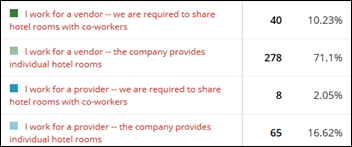

I asked readers whether their employer requires them to share hotel rooms for group travel. The results: only 12 percent of respondents said yes, which is about the same percentage as reported in other national surveys. The numbers were the same for both vendor and provider employees. My thoughts:
- Vendors theoretically save their customers money by forcing the rank and file to share rooms, but the frugality often ends when executives are involved as the lavish salaries and stock options dwarf the cost of a few hotel nights. Customer costs never go down, and it’s likely that customers of the room-sharing vendors pay just as much.
- I would bet anything that company executives don’t share rooms. I’m not a fan of policies that only apply to people in the trenches.
- A better option would be to book single rooms in cheaper hotels and provide group transportation to the event’s location.
- The “two same-sex people should be comfortable and safe as roommates” idea is a dated concept that makes incorrect and stereotypical assumptions about sexuality and body image.
- A shared employer isn’t enough reason for me to be comfortable with forced cohabitation with someone I barely know.
- I’m a big fan of asking employees if they will share rooms instead of insisting they have to. That gives people who are uncomfortable with the idea for any reason a discrete way to opt out.
- Lawyers would salivate at the chance to represent someone exposed to sexual harassment or violence because of employer-mandated room sharing.
Last Week’s Most Interesting News
- Epic hires a lobbying firm, breaking from its long-held claim of having nobody assigned to sales, marketing, and government relations roles.
- Free EMR vendor Practice Fusion raised the ire of practice customers and hopefully the awareness of other cloud-based system users in reminding those customers to insist on access to local copies of their data for downtime situations.
- A survey of ACOs finds that most have only basic IT systems.
- Massachusetts says it will spend more money to fix its struggling health insurance exchange website rather than move to Healthcare.gov.
Webinars
August 27 (Wednesday) 1:00 p.m. ET. Enterprise Data – Tapping Your Most Critical Asset for Survival. Presented by Encore, A Quintiles Company. Presenters: Jonathan Velez, MD, FACEP, CMIO, Hartford Healthcare; Randy Thomas, Associate Partner, Encore, A Quintiles Company. This first of a webinar series called “It’s All About the Data” will describe the capabilities provider organizations need to become data driven. The presenters will provide an overview of the critical role of an enterprise data strategy, creating the right data from source systems beginning with implementation, real-world data governance, how to avoid “boiling the ocean” with an enterprise data warehouse, and the role of performance feedback to transform analytics insights into improved outcomes and efficiencies.
Acquisitions, Funding, Business, and Stock
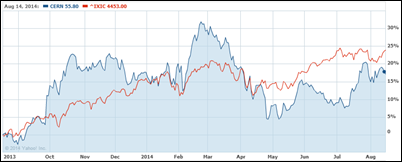
Cerner shares (blue) are up nearly 12 percent since the company announced that it will acquire the healthcare IT business of Siemens on August 5, but they still lag the Nasdaq (red) over the past year.
People

MModal announces that CEO Duncan James will resign from the company, which exited Chapter 11 bankruptcy two weeks ago. MModal has also brought in a new board.
Government and Politics
The New York Times reviews the government’s Medicare fraud efforts that cost $600 million per year, concluding that the 90 percent of fraud isn’t caught because HHS doesn’t manage the private recovery audit contractors it uses very well. The article says hospital pushbacks and extensive appeals have nearly completely shut down recovery efforts and cases can take up two years to get in front of a judge. It also notes that RAC bounties are so high that the companies paying fraudulent claims are sometimes the same companies paid to investigate them.
I missed this: Health Information Technology Exchange of Connecticut died a quiet death on July 1, 2014 when a new state budget bill repealed the creation of several quasi-public agencies, of which HITE-CT was one. Nobody seemed to notice or care, so that probably says it all.
In Canada, B.C. Emergency Health Services drops its $2.8 million ambulance electronic patient care record a year after it was supposed to go live, saying that, ”the vendor was unable to meet our business requirements.” The vendor was Interdev Technology.
A study of 2011 California data finds that hospitals charged between $10 and $10,169 for the same lipid panel lab test. The same author previously found that the list price for an uncomplicated appendectomy prices ranged from $1,500 to $187,000. Nobody pays list prices except the uninsured, who obviously wouldn’t be able to afford the ridiculous prices even if they wanted to pay. Healthcare prices are even more irrelevant than the inflated nightly rates listed on the back of hotel room doors.
In a relevant story, a man who went to the ED of for-profit Bayonne Medical Center (NJ) to have them look at a finger he had cut days before is billed $9,000 for a tetanus shot and a bandage. The hospital’s CEO says it went out-of-network for the insurance company because of low payments and that it needs high ED charges to survive. The insurance company says the CarePoint Health-owned hospital is deliberately gouging consumers by dropping out of networks since New Jersey law requires the insurance company to pay for ED services anyway. The insurance company settled with the hospital for $6,640, and after the local TV station picked up the story, the hospital wrote off the balance owed by the patient. It’s ridiculous to put in-network verification responsibility in the hands (no pun intended) of a patient seeking emergency treatment, or to ask every employee who walks in the door whether they are in-network since hospitals always have private doctors and contractors running around who issue their own bills.

The top 10 executives at the non-profit Blue Cross and Blue Shield of Alabama made more than $1 million each in 2013, doubling their 2011 pay. The president and CEO made nearly $5 million.
Contacts
Mr. H, Lorre, Jennifer, Dr. Jayne, Dr. Gregg, Lt. Dan, Dr. Travis.
More news: HIStalk Practice, HIStalk Connect.
Get HIStalk updates.
Contact us online.





The “two same-sex people should be comfortable and safe as roommates” idea is a dated concept that makes incorrect and stereotypical assumptions about sexuality and body image.
Thanks for making this statement. I was thinking it, and observed a conversation by Allscripts employees on this very topic, but wasn’t sure if it was appropriate yet to say aloud.
Based on your coverage, the US medical care system is going from bad to worse in terms of price gauging and other financial engineering programs, all made easier by experienced IT specialists and hospital IT billing and record systems.
Now I know why there are smiling mugshots on you blog.
I would like to see the smiling million dollar Highmark execs. Get their mugshots.
Amen to your response to @lodi.
Do you think @carl_dvorak’s comments are self serving?
And why should the vendor exec be in a direct position to establish US national policy re:HIT??
Not only is Massachusetts going to spend ANOTHER $18 million, I mean the taxpayers to fix their exchange, the other bug news is that 400,000 people will have to re enroll into the health exchange because they were put on state aid when the original site crashed. So the Massachusetts taxpayer will continue to pick up the costs of these fiasco’s. Gov Deval Patrick is in complete denial of the problems, because in the end, it is not his money that he keeps spending to meet POTUS mandates.
Regarding the downtime of cloud based EMRs and the comment in a recent HIStalk post stating that clinics must wish they had an in-house server when the cloud EMR goes down, do in-house client-server EMRs never go down? I think there have been plenty of examples of client-server EMRs going down. What is the difference between either type going down? For the providers, its the same thing. I think I would rather have a cloud based system go down. The vendor is responsible for bringing it back up and has specialists working on it immediately. In an in-house server, the provider office has to wait until a tech is available and has to pay for the service him/herself.
Love the use of XKCD :). Good stuff.
“Nobody pays list prices except the uninsured, who obviously wouldn’t be able to afford the ridiculous prices even if they wanted to pay. Healthcare prices are even more irrelevant than the inflated nightly rates listed on the back of hotel room doors.”
I did a stint as an uninsured stay-at-home mom during my children’s early development years, and I found this to be contradictory to my experience. I had an ER visit to learn about my first kidney stone, where I was given an ultra-sound and confirmed the size of the two stones and referred to a urologist, all for a grand total of $6,000. (For some perspective, we paid for a nifty new “4D” ultrasound of our baby just a few months earlier for $200. It included a DVD copy and a massage.) The hospital worked with me and wrote off the majority of the charges, such that I was left with a bill for $300, if memory serves. Fast forward five years, I am employed and paying for insurance coverage and seeing a urologist who refers me to the lab for urinalysis and KUB x-ray. Two different labs offered each test, but both quoted me around $500 each for each test, which would go toward my insurance’s annual out of pocket maximum. HOWEVER, if I wanted to pay cash, both labs were willing to accept $50 for each test. How is this not criminal? I dread the public reaction as more people go to use their newly minted insurance cards and learn the racket that is called healthcare.
“Nobody pays list prices except the uninsured, who obviously wouldn’t be able to afford the ridiculous prices even if they wanted to pay. Healthcare prices are even more irrelevant than the inflated nightly rates listed on the back of hotel room doors.”
That may have been true years ago, but with millions of people moving to high deductible health plans out of necessity, the cost (if not the “list prices”) of services is shocking a lot of people. My brother is a small business owner with a HDHP. During a routine annual checkup with his GP, the doctor offered to remove some ear wax he noticed. The ear wax removal showed up on his bill as a $180 charge, which he was forced to pay out of pocket because he wasn’t at his deductible limit yet. A lot of people are in for a rude awakening as the ugly side of U.S. healthcare becomes more apparent to more people.
I love the entertainment about room sharing at Allscripts. I experienced many years of it at Allscripts and never enjoyed it but always understood it. It works out ok as long as you don’t play room roulette. I always thought of it as the ability to have more associates participate for less spend. Clients love to interact with associates. Especially those on the front lines and not just sales and exec’s.. Clients also like companies that are being responsible with spending.
Having said all that and now working for another employer that doesn’t require this and I am enjoying my personal space.
Allscripts lets you buy the other half of your room , or select a specific room mate — might want to get your information straight, son.