RE the AI GLP1 company, Washington Post has an article today by someone who used one of those compounded products,…
News 5/7/14
Top News
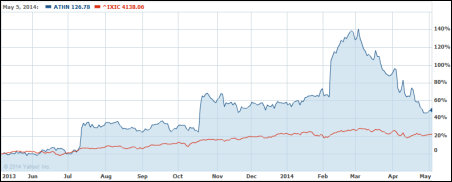
Comments from hedge fund manager David Einhorn send shares of athenahealth down nearly 14 percent Tuesday after he tells investment conference attendees that ATHN is one of a few “bubble stocks” trading at high valuations for no good reason. He added that athenahealth really isn’t a cloud vendor deserving of high share price multiples since its main role is as a business process outsourcer of mundane back-office physician practice tasks. He also said that athenahealth’s promotional videos are full of buzz words and that “Epic’s dominance will only grow” as “the undisputed winner from the fragmented IT market.” He predicted the company’s shares will drop 80 percent. Above is the one-year chart of ATHN (blue) vs. the Nasdaq (red), with shares closing Tuesday as Nasdaq’s fifth-largest percentage decliner.
Reader Comments
From Bratman: “Re: Vonlay acquisition by Huron Consulting. The acquisition price was $35 million, all cash, and was a 1.2 times multiplier on revenue. There were several interested acquirers. The price may have ended up lower since Epic forced the Vonlay owners to modify the terms of the Vonlay-Epic agreement to extend the non-compete for former Epic employees from one year to two years. Epic required this change before it would agree to transfer the Vonlay agreement to Huron. The legality of forcing Epic employees into non-compete agreements they never knew about or agreed to is definitely up for debate and the length of the new non-competes likely makes them unenforceable. Epic seems to be using its power to try to minimize employee attrition and limit the supply of certified third-party consultants.” Unverified.
Upcoming Webinars
May 7 (Wednesday) 1:00 p.m. ET. Demystifying Healthcare Data Governance. Sponsored by Health Catalyst. Presenter: Dale Sanders, SVP, Health Catalyst. Challenged with governing data? This vendor-neutral discussion will cover the need to develop a data governance strategy, including general concepts, layers and roles, and the Triple Aim of data governance (quality, literacy, and exploitation.)
Acquisitions, Funding, Business, and Stock
QPID Health raises $12.3 million in a Series B funding round and adds a board member from New Leaf Venture Partners.
Radiology outsourcer Alliance HealthCare Services acquires the assets of OnPoint Medical Diagnostics, which offers a cloud-based scanner quality control system used by 81 hospitals, for $1 million in cash and two years’ of royalties.

Huron Consulting Group closes its acquisition of Epic consulting firm Vonlay of Madison, WI.
Pittsburgh-based teledermatology technology vendor Iagnosis raises $2.8 million from angel investors.
Xerox will acquire ISG Holdings, which offers workers’ compensation software systems under the StrataCare and Bunch CareSolutions brands, for $225 million.
Sales

Valley General Hospital (WA) chooses Medsphere’s OpenVista EHR for its 68 beds.
Alere Accountable Care Solutions will build a community-wide HIE for Whittier Independent Practice Association (MA).
Emerald Physicians ACO (MA) selects the eClinicalWorks Care Coordination Medical Record.
People

Oneview Healthcare names Jeff Fallon (Fallon Strategy) as president, North America.


ESD hires Cinthia Tenorio, LPN (Lake Health System) as CDI practice director and John Ortego (CTG) as Meditech practice director.

Tracy Gregory (Linguamatics) joins SyTrue as chief scientist.

Patrick Clark (Vonage Business Solutions) joins Wellcentive as CFO.

Accenture CEO Jorge Benitez will retire from the company at the end of August.
Announcements and Implementations
MModal announces enhancements to its Fluency Flex mobile dictation application for iOS devices.
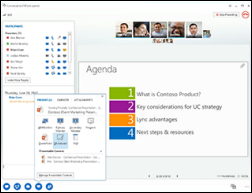
In Australia, Sydney Children’s Hospital Network announces plans to use commodity software for its telemedicine program, including Lync videoconferencing and Skype video calling, both from Microsoft.
RadNet goes live on Nuance PowerScribe 360 at the first of its 250 imaging centers and 27 practices.
Advocate Medical Group of Chicago (IL) implements Forward Health Group’s PopulationManager and The Guideline Advantage.
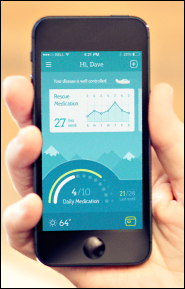
Propeller Health earns FDA approval for the new generation of its inhaler-measuring asthma monitoring system.

St. Joseph’s Hospital Health Center (NY) goes live with Epic.
Zoeticx makes available an API that it says will allow developers access to “any EMR system.”
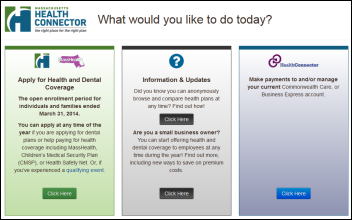
Massachusetts announces that it will abandon its $57 million CGI-built health insurance exchange website and hire hCentive, which developed three other state marketplaces, to build a new one. The state also says that just in case that doesn’t work, it will just join the federal exchange in November. Massachusetts isn’t sure if it will need to ask the federal government for more money than the $174 million it already received since it is disputing its CGI contract, but the “dual track” option it chose (the sequel to its disaster movie) will cost another $100 million.

CMS reports that only 50 doctors and four hospitals have successfully attested for Meaningful Use Stage 2 through (or “thru,” as the slide says) May 1. CMS also reports that it has approved 66 of 72 applications for hardship exceptions.

Michelle Consolazio of HHS tweeted this photo of the HIT Policy Committee thanking outgoing member and Epic CEO Judy Faulkner, who has been replaced as its vendor representative after four years by Cerner CEO Neal Patterson.
The talking heads in this hysterically partisan and sensationalist Fox News program seem exceptionally clueless yet smugly superior about nearly everything, but Jesse Watters (I don’t watch TV, so I don’t know who he is) outdoes himself at the 12:40 mark when talking about the VA wait list controversy by declaring, “They’re still using paper records at the VA. They’re not even computerized yet.” That’s embarrassing no matter what your political persuasion, but of course he only plays a journalist on TV and can’t be expected to differentiate between disability claims forms and medical records.
National Coordinator Karen DeSalvo, MD says her husband, also a doctor, uses a “clunky” EHR. A bit of Googling suggests that her husband is (or at least was) an ED doc at Lakeview Regional Medical Center in Covington, LA, so perhaps his clunky EHR could be identified. I assume it’s Meditech since it’s an HCA hospital.
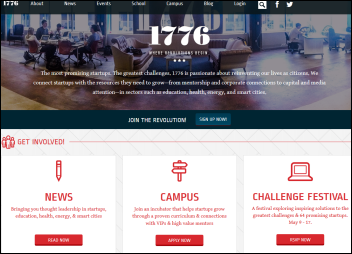
MedStar Health (DC) will co-locate some of its employees in the offices of DC-based incubator 1776, connecting the health system with technology startups to arrange pilot projects. MedStar will also provide education for the 20 percent of 1776’s companies that deal with healthcare.
IBM names 25 finalists in its Watson Mobile Developer Challenge. Those that are healthcare-related include GoGoHealth (telemedicine), Ultramatics (personalized health answers), Ringful Health (patient-physician communication), GenieMD (health management), Biovideo (information for expectant mothers), and Sense.ly/MyIdealDoctor (medical information).
Community Hospital (IN), which is treating the first US patient to be infected with Middle East Respiratory Syndrome (MERS), used its Versus RTLS system (along with video surveillance recordings) to identify employees that had come in contact with the patient, earning a mention on the local TV news report. Hospital CMIO Alan Kumar, MD says, “We can tell down to the second how long they were in contact with the patient, and how long they were in the room, and provide data to CDC.” According to the state’s health commissioner, “MERS picked the wrong hospital, the wrong state, and the wrong country to try to get a foothold.”

Durham County, NC commissioners vote to give Lincoln Community Health Center $500,000 to install Epic, half the amount it requested. The $2 million implementation would allow the clinic to connect with Duke University Health System’s Epic system. Commissioners suggested hitting up Duke for more than the $1 million it offered toward the cost, with one saying, “In the big scheme of what’s been invested at Duke, between $500 million and $700 million, this additional half a million, I would hope they would be able to absorb that and do what needs to be done.”
@venturevalkyrie leading great panel on "Digitizing Care Delivery" at #HEPSummit. pic.twitter.com/CYQmA9fEns
— David Jones (@dajonesjr) May 2, 2014
Investor Lisa Suennen (“Venture Valkyrie”) writes a blog post about the recent Health Evolution Partners Annual Summit that is brilliant in both insight and wit.
And this group of people, who know everything there is to know about how we got into such a healthcare system mess (because they helped create it) and what has got to be tackled to fix it (even if not how to do that exactly) is dealing with quite a conundrum. They are caught in a vortex where they have to straddle the old world and new world—the land where healthcare decisions are mostly still driven by volume and not quite ready to chuck it all for a world based on “value.” … it is impossible to train the entire hospital to act in two completely different ways based on the patient who shows up. You simply can’t run two different workflows and two different case management programs and two different follow-up programs efficiently. Most of the time the actual caregivers in a hospital—physicians, nurses, etc.—don’t even have a clue in what insurance program or risk-pool the patient is enrolled; certainly no one is yet handing out bar-coded wrist bands that tell the caregiver whether to minimize or maximize services, based on the financial motivation (I hope).
Points from the 2014 HIMSS Regional Extension Center Survey, with 37 of 60+ RECs (which have received $677 million in taxpayer support) responding:
- Nine out of 10 say their #1 business issue is staying alive, with several respondents saying financial sustainability isn’t possible or isn’t something they’ve planned adequately.
- One-fourth of the RECS say they won’t be viable by the end of the year, and half of those that say they’ll survive expect state grants to keep them solvent.
- Three-fourths of them want more ONC grants to keep afloat.
- One-fourth of the respondents say they will partner with other RECs to ensure their viability.
- Staffing ranged from two to 80, with an average of 23 FTEs.
- The #1 services priority is providing information services related to business intelligence and data warehouses, while optimizing EHRs and providing Meaningful Use services came in right behind.

Fitch downgrades the bonds of Centegra Health System (IL), blaming its acquisition of physician practices and its EHR rollout (McKesson Paragon, I believe) for “light operating profitability.”

Blue Cross Blue Shield of North Dakota fires its CEO right after the company reports an $80 million loss largely due to problems in its Noridian Healthcare Solutions subsidiary, which developed Maryland’s failed health insurance exchange website. Paul von Ebers had vowed Thursday to improve the organization’s financial position by reducing administrative overhead, which its board took to heart in unanimously voting Monday to fire him effective immediately.
Guess which vendor is looking for a marketing director? Wrong … it’s HIMSS, trying to find someone to help push its many publications.
@deansittig tweeted out a link to an Epic promo-type video by Lucile Packard Children’s Hospital Stanford (CA) that is well done, but I liked the one above better.
Some hospitalists at the annual conference of the Society of Hospital Medicine focus on IT issues, urging their peers to “establish ourselves for the informatics role we have taken” by earning informatics subspecialty board certification.
Weird News Andy intones that “exercise can kill you.” In Portland, OR, a naked man doing pushups in the middle of the street at 4 a.m. is run over and killed by a car, with predictable toxicology results pending. WNA can’t keep his hands off his Oregon as he files another story that he calls, “is there a governor in the house?” as ED doc and Oregon Governor John Kitzhaber jumps out of his limo to perform CPR on a collapsed woman (WNA wonders he couldn’t spare some compressions for Cover Oregon.)
The family of a Miami doctor sues the driver of the Lamborghini in which he died when it crashed into a car stopped at a light at over 100 miles per hour two weeks ago. The driver, the founder of a vodka company, was drunk when he and the doctor left the Versace Mansion after discussing investments. The non-practicing doctor had a vodka company, too, going by the nickname Dr. Vodka.
Sponsor Updates
- Deloitee’s Harry Greenspun, MD is interviewed about mobile health devices on Federal News Radio.
- Strata Decision Technology, MedAssets, and Prominence Advisors are named to Becker’s “150 Great Places to Work in Healthcare.”
- Helen Figge with Alere Accountable Care Solutions discusses how to still meet requirements for MU Stage 2.
- Capsule’s Michelle Grate explores healthcare as a complex adaptive system and explains why it matters.
- Beacon Partners recommends five steps for developing a CDI program as part of preparation for ICD-10.
- Voalte releases a white paper offering three key elements to secure physician texting.
- Advanced Data Systems will integrate Merge Healthcare’s iConnect Network with its MedicsRIS.
- Truven Health reports that premature or low-birth weight infants funded by Medicaid cost nine times more than uncomplicated newborns.
- T-System’s Elizabeth Morgenroth offers three reasons to start documenting for ICD-10.
- Aventura CEO John Gobron discusses awareness computing bringing intelligence to the clinician workflow at the Healthcare IT Institute in Sarasota, FL.
- Cottage Hospital (NH) reports that it has saved over $100,000 in interface fees since going live on Summit Healthcare’s interface engine.
Contacts
Mr. H, Inga, Dr. Jayne, Dr. Gregg, Lt. Dan, Dr. Travis, Lorre.
More news: HIStalk Practice, HIStalk Connect.











I’m calling bs on that Zoeticx claim. I’d love to see them demonstrate direct integration with MEDITECH, Epic, MS4, Cerner, AllScripts and McKesson.
Regarding the death of Dr. Vodka from Miami, I think this is the most head-scratching part of the news report.
“The impact sent the Lamborghini more than 100 yards into the air, according to the complaint.”
What would that car look like if it had been dropped from as high as a football field is long?
Re: “The talking heads in this hysterically partisan and sensationalist Fox News program seem exceptionally clueless…I don’t watch TV…”
It is obvious you do not watch TV or you would know that one of the panelists, Bob Beckel (guy wearing the suspenders), is as Democrat/liberal as they get, and yet he was agreeing with 95% of the points being by the other panelists. Yes, there were a few partisan jabs made toward the end of this clip, but the overall tone of the program was bi-partisan and reflected problems within the V.A. that have persisted across multiple administrations, regardless of party leadership.
I have also found it curious as to why Athena gets such high valuations on Wall St as their model/offering is really just a billing service. Sure, they are attempting to expand into other areas, eg athenaclinicals but not enough to justify such lofty expectations. At some point though, they may become attractive to another as this mkt will inevitably consolidate. And no, I do not subscribe to Epic owning everything, but market will shake out much like the ERP market which now has three dominant players. Epic is the SAP of healthcare and will struggle with similar fate.
And I’m with Chris, that Zoeticx claim is pure bunk.
least nobody here is ‘hysterically partisan’…
Zoeticx – “MEDICAL RECORD APP DEVELOPERS NO LONGER NEED TO WORRY ABOUT DATA PLATFORM OR CONNECTIVITY”
In my experience, App Developers NEVER worry about such things now, leaving the worry to IT and Users. But thanks anyway.
To say Bob Beckel is as liberal as they get is laughable. He’s a “plant” to dump on or otherwise make the other side look bad.
High five–ErinsDad!!! What a hoot! So true…
“Zoeticx – “MEDICAL RECORD APP DEVELOPERS NO LONGER NEED TO WORRY ABOUT DATA PLATFORM OR CONNECTIVITY”
In my experience, App Developers NEVER worry about such things now, leaving the worry to IT and Users. But thanks anyway.”
This place is getting quite partisan itself. Take a look in the mirror. Seems like this site is suffering from what many vendors suffer from…kool aid intoxication syndrome.
“hysterically partisan and sensationalistic”…unnecessary jab at what was an informative spotlight on a tragic situation. I applaud them (and you) for bringing it to light, despite your underhanded critique of their show and political slant.
Has this question been asked before:
Is Weird News Andy, “Weird” News Andy, or “Weird News” Andy?
Just curious.
Jonathan Bush in a difficult position but thought he was effective on CNBC this morning explaining how Athenahealth is different. I would ask HIStalk subscribers, what do you think? Is he just selling AthenaHealth or is he a new breed of market leader?