I've figured it out. At first I was confused but now all is clear. You see, we ARE running the…
News 3/28/14
Top News

The House of Representatives approves, by an unusual voice vote, a hurriedly presented bill that would delay the mandatory implementation of ICD-10 until at least October 1, 2015. The bill, presented Wednesday and approved Thursday, primarily addresses a Sustainable Growth Rate fix that would prevent the 24 percent reduction in physician Medicare payments that will otherwise occur on April 1. The ICD-10 date change was contained in a single sentence in the bill, which will become law if it’s approved by the Senate on Monday and then signed by the President. HHS has been insisting the deadline wouldn’t change after two previous delays, providers and vendors should have been ready given the generous lead time and remaining six months, and most organizations agreed that it was time to rip the Band-Aid off and just do it. Now a delay gets snuck into an unrelated bill and pushed to approval in less than 24 hours, most likely by politicians who didn’t have a clue about what they were voting for. The bill proves how ineffective Congress can be – they can’t figure out how pay for fixing SGR, so they delay its implementation, and despite HHS claims that ICD-10 is vital, it’s easier to keep delaying it than to reach an actual decision about its merit.
Reader Comments
From The Reverend: “Re: another MU question. Thanks for posting question about the exemption letter. I’m also confused by the statement at the top of the exemption form that, ‘If you successfully met Meaningful Use in 2013, you will be excluded from the payment adjustment and do not need to submit a Hardship Exception Application for Payment Year 2015.’ I betcha this is a brilliant tactic to bring costs for the program under control. Providers current with MU will see an opening to ignore this year’s reporting period since the one percent penalty is off the table and ultimately fewer providers will get that final year payment.” I’m not sure what CMS’s intentions were with its handling of the exemption process, but I bet plenty of providers will take advantage of the reprieve.From Seymour Bush:
“Re: Atlantic article series on EHRs. This gentleman’s comments are a fun counter to industry hype.” According to Nebraska-based family practice doc Creed Wait, MD:
The saying is, “Build a better mousetrap and the world will beat a path to your door.“ The saying is not, “Build a different mousetrap, pay out 19 billion dollars in incentives to use the mousetrap, mandate its use by law and punish those who fail to adopt it. Then shove the world kicking and screaming against their will through your door” … For the federal government to mandate the use of EMRs by every physician out there just because it works at the VA would be like telling the entire world, “OK, we made it to the moon. Now it is your turn. Any country that has not put a man on the moon within the next five years will be bombed. Every country that complies with this mandate will get a check for $1B. For those countries who fail to comply with this mandate, shelling will begin at 1:00 a.m, five years from today.” …The EMR had become the primary influence in the interview. The dynamic had changed. The patient and I were now both in the room to feed the hunger of the software … Physicians used to write their orders and clerks would enter these data into the computer. Under the new mandates, the physician is now a data entry clerk. What’s next? Is each hospital CEO going to be required to spend two hours a day manning the switchboard?
From Dim-Sum: “Re: DoD EHR. DoD looked at Judith’s big Kaiser win, calculated additional funds for development of a down range medicinal solution, and added a chunk for COTS vendors to certify their teams for Tier 1,2 & 3 support. That figure, for all practical purposes, is $5.5 billion USD. The SI prime wants 40 percent of the pie. COTS EHR vendors will want $1.8 billion USD . Does anyone see the math does not add up? To add to the confusion and muffled numbers is the fact that a CMMI 3 firm will come in and state that COTS can’t create or engineer a down range solution, so they will want $500M – are we seeing a trend here? COTS EHR vendors cannot fathom Agile Scrum, let alone CMMI 3 mediocre results, Everyone forgets that software vendors in the US usually charge 16-20 percent of original software list for ongoing annual support — those numbers are included, so the hopes and dreams of the average EHR vendor is shattered. They will have to come down by $0.5 billion, round down their fee so they can recoup recurring revenue of 20 percent ($200 million a year) of the leftover amount to secure a more realistic number of $800 million. Your SI buddies want COTS vendors to be realistic, stop your silly dreams – you never heard of SPAWAR (Latin meaning “Beltway ONLY.”) SIs deserve the cash because they have no idea how to develop competitive software, so they want your knowledge on the cheap, they are program managers, they are the conduit in to the psyche of the DoD. The DoD does not value software, they value stability and sustainability and salute predictability. That is why it is so hard for COTS vendors to believe that the DoD blew $10+ billion USD for the monstrosity they have today and are hoping COTS EHR vendors can save the day.”
From Bill O’Sayle: “Re: FDA recalling McKesson’s anesthesia software. Both Cerner and Epic (for example) now have products to consume medical device data straight into their EMRs (i.e. Cerner iBus). Do you think this means then that EMRs with such capability are now at risk of such a recall? I can’t see Cerner putting their PowerChart install base at risk of a recall just so they (Cerner) can claim medical device integration. But if this is the logic of the FDA, then that seems to be the case, no?” The lab software model is that the instrument interface requires FDA’s approval, but the system that uses its information doesn’t (except for blood banking systems). I’m speculating, without knowing the details, that McKesson’s anesthesia product may have medical device integration built in, which puts the whole product within FDA’s purview. But given my “without knowing the details” disclaimer, I’d be interested to hear from someone who knows more than I.
From HIMSS EHR Association: “Re: EHR Developer Code of Conduct. A correction to Mr. H’s thoughts on the McKesson/FDA matter. The EHRA strongly recommends that all vendors developing EHR products, regardless of membership in the EHRA, adopt the Code of Conduct. However, it is not a condition of membership in the EHRA. The 17 vendors that adopted the Code of Conduct as of February were recognized at HIMSS14. Since then, three additional vendors have adopted the Code. The EHRA is hosting a webcast on Friday, March 28 to educate more vendors on the elements included in the EHR Developer Code of Conduct and the benefits of adoption.”
HIStalk Announcements and Requests
![]() Highlights from HIStalk Practice this week include: Dr. Gregg asks if being OK is OK and notes that the hard part isn’t achieving perfection but learning to be OK with OK. CMS warns EPs of possible system delays as providers submit MU attestation data by the March 31 deadline. The American Academy of Ophthalmology launches IRIS Registry, a centralized data repository that aggregates outpatient clinical data from EHRs. Epic, eClinicalWorks, and Allscripts claim the biggest shares of the ambulatory EHR market. Naval Branch Health Clinic Albany (FL) offers secure messaging services through RelayHealth. AHIMA warns that the use of copy and paste functionality in EHRs should be permitted only in the presence of strong technical and admin controls. While checking out these stories, why not sign up for the spam-free email updates so you won’t miss something important? Thanks for reading.
Highlights from HIStalk Practice this week include: Dr. Gregg asks if being OK is OK and notes that the hard part isn’t achieving perfection but learning to be OK with OK. CMS warns EPs of possible system delays as providers submit MU attestation data by the March 31 deadline. The American Academy of Ophthalmology launches IRIS Registry, a centralized data repository that aggregates outpatient clinical data from EHRs. Epic, eClinicalWorks, and Allscripts claim the biggest shares of the ambulatory EHR market. Naval Branch Health Clinic Albany (FL) offers secure messaging services through RelayHealth. AHIMA warns that the use of copy and paste functionality in EHRs should be permitted only in the presence of strong technical and admin controls. While checking out these stories, why not sign up for the spam-free email updates so you won’t miss something important? Thanks for reading.
This week on HIStalk Connect: Six senators send a letter to the FDA seeking clarification over medical app regulation. Beth Israel Deaconess Medical Center will expand the use of Google Glass by ED clinicians after finishing a successful three-month trial. Reflexion Health raises $7.5 million to expand development of a Microsoft Kinect-based platform designed to support physical therapists and their patients.
I had some site problems over the weekend through Wednesday, which caused some downtime and the temporary disappearance of some posts and comments. Hopefully it’s all fixed now. Geek details: the webhost monitors web traffic and noticed IP traffic containing HIStalk’s server password, leading them to discover a root trojan that would have allowed its creator to take control of the server. That required building a new virtual server and migrating all the settings and large MySQL databases over to an environment containing fresh installs of PHP and Litespeed, which often brings up odd permissions and database problems. It’s been quite a pain – I watched the site and the open support ticket for 15 hours on Saturday alone and slept only a couple of hours, but problems delayed the actual migration until Tuesday evening.
Upcoming Webinars
April 2 (Wednesday) 1:00 p.m. ET. A Landmark 12-Point Review of Population Health Management Companies. Sponsored by Health Catalyst. Presenter: Dale Sanders, SVP, Health Catalyst. Learn the 12 criteria that a health system should use to evaluate population health vendors and to plot its internal strategy, then see the results of grading seven top PHM vendors against these criteria. No single vendor can meet all PHM needs. The most important of the 12 criteria over the next three years will be precise patient registries, patient-provider attribution, and precise numerators in patient registries.
April 16 (Wednesday) 11:00 a.m. ET. Panel Discussion: Documents, EMRs, and Healthcare Processes. Sponsored by Levi, Ray & Shoup. Presenters: Charles Harris, senior technical lead, Duke University Health System; Ron Peel, technical advisor, LRS; and John Howerter, SVP of enterprise output management, LRS. IT department in hospitals implementing EMRs often overlook the role of document-driven workflows. Prescriptions, specimen labels, and discharge orders, and other critical documents must be reliably delivered with minimal impact on IT and clinical staff. This panel discussion will discuss the evolving use of documents in the “paperless/less-paper” environment.
Acquisitions, Funding, Business, and Stock
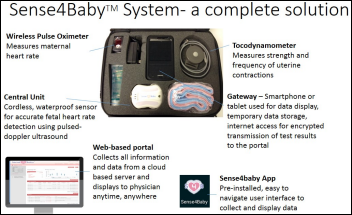
AirStrip acquires the assets of wireless fetal/maternal monitoring provider Sense4Baby and licenses the technology from the Gary and Mary West Health Institute.
Sales

Southern Illinois Healthcare selects CPM CarePoints, ExitCare, Mosby’s Nursing Consult, and Mosby’s Skills from Elsevier.
Gracepoint Management (FL) will implement the Plexus Revenue Cycle Management service from Netsmart across its network of 48 behavioral health and drug and alcohol treatment centers.
People

TeleTracking Technologies hires Susan Whitehurst (Joint Commission Resources) as managing director of consulting services.

Innovative Consulting Group names David Kissinger (Leidos Health) regional VP.

Wellspring hires Matthew Joyce (Stout Risius Ross) as SVP of sales.
Announcements and Implementations

Bradley Healthcare and Rehabilitation Center (TN) begins transitioning to PointClickCare EMR.

Henry Ford Health System (MI) joins the Michigan Health Connect HIE.
Government and Politics
The HHS OIG finds that a federal database for tracking Medicaid fraud isn’t working as intended, with 17 states and the District of Columbia failing to provide information on providers banned from billing Medicaid. The database also contains missing National Provider ID numbers and names of “terminated” providers who are actually dead.
Technology
Medicity earns a patent for its technology for connecting referral networks and another for its technology to centralize communications between providers and patients using cloud-based mobile technology.
Other
Continua Health Alliance announces availability of its 2014 Design Guidelines.
The eHealth Initiative launches its 2020 Roadmap to guide the transformation of the nation’s healthcare system by 2020. The roadmap will focus on recommendations tied to Meaningful Use, system interoperability, care delivery transformation, and a balance of innovation and privacy.
Online second opinion service Best Doctors launches the Medting medical exchange.
Weird News Andy calls this story “dueling paramedics.” A woman being transported by ambulance for possible stroke gets out of the ambulance after the two paramedics started arguing bitterly about a personal issue. WNA also observes the skyrocketing healthcare salaries in Cuba, where huge percentage boosts will give nurses an income of $25 per month, while physician specialists will earn $67 per month, up from $26.
Sponsor Updates
- HealthMEDX hosts its user group meeting next week in Branson, MO.
- CommVault publishes a white paper highlighting findings of a nationwide survey of healthcare IT managers, which suggest that healthcare data from a variety of sources could overwhelm the healthcare delivery system.
- HCS announces that all of its Interactant modules meet ICD-10 standards.
- Craneware hosts a series of one-day user group meetings in advance of its October Revenue Integrity Summit in Las Vegas.
- PDS provides details of its 2014 Tech Conference October 22-23 in Madison, WI.
- Nordic Consulting CEO Mark Bakken will deliver the keynote address at Madison’s startup incubator Gener8tor’s winter premiere night on April 3.
- Wolters Kluwer Health enhances its UpToDate App for the Android mobile platform.
- Kareo CEO Dan Rodrigues discusses his company and the power of cloud computing for small- to medium-sized practices.
EPtalk by Dr. Jayne
Everyone at the hospital is buzzing about the possibility that ICD-10 will be delayed as part of the legislation addressing the Medicare physician payment cut. Both CHIME and AHIMA have come out against the ICD-10 provision, stating that delaying it would negatively impact innovation and health care spending.
Athenahealth’s VP of government affairs, Dan Haley, quickly blogged about it in response. His main assertion is that a delay would only reward vendors who didn’t work hard enough to meet deadlines which have been published well in advance. His secondary point is that for the legislature to delay ICD-10 after the head of CMS has said multiple times that there will be no further delays is akin to a child receiving dessert after his parent had previously told him no.
As much as I’d hate to see my colleagues and their employers suffer when their vendors are not ready, it may take something this dramatic to really thin out the vendor herd. We’ve known this deadline was coming for a very long time and for vendors to still be unable to meet it is inexcusable. We can blame it on MU and the fact that we have a perfect storm of governmental requirements massing to hit us all at once. We can blame it on all kinds of things but the bottom line is that many vendors have delivered despite all those factors.
I don’t have a crystal ball to see how this is going to morph as it works its way through Congress, but it just goes to show that there’s never a dull moment in health IT. Many of my colleagues are already using it as an excuse to stop working on ICD-10 even though the legislation hasn’t been signed. In the words of Julia Roberts as Vivian Ward: “Big mistake. Big. Huge.”
Speaking of mistakes, several readers have written about the issues mentioned in Monday’s Curbside Consult. One of the problems I encountered was an issue with having multiple aliases in a hospital’s patient portal. A reader pointed out that issues like this are not only patient safety issues, but can also play into national safety:
I’m sure you’ve seen the articles about the so-called “Boston Bomber” entering the US undetected because he spelled his name differently than what was on the official watch list (Tsarnayev v. Tsarnaev). Seriously? The CIA was confounded by the unexpected insertion of the letter “y” into a person’s name … a person on a monitored watch list? Seems incredible. If the CIA can’t figure out how to address probable name variances, then I’m not so surprised that your large academic medical center can’t figure out how to fix an alias name in its EMPI.
Other readers sent their own stories of IT systems run amok not only in healthcare, but in other industries as well. The pace of change is so great that little things like accuracy and completeness can’t seem to keep up. As long as the majority of people think technology is the solution to everything, I don’t see things slowing down.
I haven’t mentioned shoes or wine in a while, so I was excited to find this piece about a way to remove the cork from a wine bottle using only a man’s dress shoe. The article contains an engineering explanation of the fluid dynamics responsible for it working. Unfortunately ladies’ heels don’t work well due to the angle of the sole, so Inga and I are out of luck. If you’re looking for a few good laughs, however, make sure you check out the comments section.
Contacts
Mr. H, Inga, Dr. Jayne, Dr. Gregg, Lt. Dan, Dr. Travis, Lorre.
More news: HIStalk Practice, HIStalk Connect







Dr. Jayne,
I think that Dan’s comment was more about marketing Athena than a knowledgeable comment about vendors in general. Most vendors really do seem to be ready, and have been contractually committed to be ready for years.
This is just the typical Athena marketing approach to decry other vendors at every turn in hopes of making themselves look good – whether factually correct or not.
When you pick it up in your blog entry with the presumption of truth, you give it undeserved credibility.
This delay is being put in by the AMA, the AHA and others like it. I know AHIMA likes it, but they represent a coding industry that will make fortunes. This is being pushed by the doctors and health systems. And, if they were smart they’d bring up the obvious 5010 debacle again and force CMS to stand in front of Congress and detail what they did to get ready, how they have tested it, etc. Then get a few payers to do the same.
The medical profession has a right to be afraid, very afraid of this. But the fear shouldn’t be of their vendors who will die if they fail. It should be of CMS who will fail and shrug it off like it wasn’t even a failure in the first place.
From your post:
Athenahealth’s VP of government affairs, Dan Haley, quickly blogged about it in response. His main assertion is that a delay would only reward vendors who didn’t work hard enough to meet deadlines which have been published well in advance.
Follow the money.
Today’s legislation was fully supported by the well-funded American Medical Association lobby as they felt the change would be “too costly” for their doctors. Hospitals be damned.
What isn’t mentioned is the potential the ICD-10 program might eventually eliminate, or greatly reduce the utilization of CPT coding. CPT coding is licensed by the American Medical Association and the AMA earns hundreds of millions of dollars each year in royalties for the usage.
We hear that Tim Thompson is on the move again and out of Baycare
@Reverend – be careful there….. the currently available hardship exemption form is ONLY for penalties due in 2015.
What CMS says is that you won’t be penalized in 2015 if you achieved MU in 2013, which is obvious because the look back is for 2 years. You can still avert the penalty in 2015 if you did not achieve MU in 2013. You do that by attesting to MU for the first time in 2014 before October 1st, or by successfully applying for a hardship exemption for 2014 (using the 2015 exemption form)..
However, after 2015 comes 2016. You will be penalized in 2016 if you don’t attest for MU in 2014, or apply and are granted a hardship exemption for payment year (or rather penalty year) 2016. Those hardship applications require a different application form, which will be made available in July.
I guess CMS wants to stagger the hardship applications, with 2015 coming in first and 2016 coming in after that.
In addition to the ICD-10 delay, the bill delays the new CMS 2 midnight rule and hold off the RACs until 2015.
AHIMA members placed over 6,000 telephone calls to Capitol Hill yesterday re: the ICD-10 delay. Has anyone heard input from HIMSS or HFMA? What are these associations saying? Postponing the conversion from ICD-9 to ICD-10 yet another year would be extremely costly for all of us who have prepared, planned, tested and are ready to proceed.
The conversation about EHRs and physician productivity (or happiness) is important, but it is almost always brought to a halt by hyperbole. For example, with respect tot he Atlantic Article cited above, the author writes:
“I estimate than a CPOE system adds 1-3 hours of work to each day”
Really? You see 14 outpatients a day and it takes more than a minute to write each patient’s orders? What kind of orders are you writing? Are all the patients on home ventilators and TPN?
and
“After one year I was seeing fourteen patients a day, my notes were twelve pages long, [and] the vital signs alone required a half page”
Really? What kind of clinic is this, exactly? How can a single line of text (typical ambulatory vitals) take half a page? What sort of stuff are you inserting into a note that makes it 12 pages?
EHRs have their irritations. But can’t we start from a basis of reality in order to talk about it?
Beth brings up a very good point – while transitioning to ICD-10 is costly and requires significant effort, delaying it at this stage may actually be worse than moving ahead. There are costs associated with putting project on hold. There are costs involved in re-starting projects that were put on hold. And lots of physicians and hospitals have already bought the software and services they need to complete the transition, and those purchases are now useless until the new deadline. This is going to be a major problem for any physician or hospital who actually prepared for the transition. This seems like a very shortsighted move by the AMA and sadly congress went for it.
Are AMA and Congress crafting a bill returning U.S. to Fee-For-Service, MD-centric, disease-focused, pay-for-poor/unsafe care system perpetually on ICD-9 and paper records? String together press releases to see this “platform”.
Has any quality of care initiative sparked the passion and perseverance of AMA opposition to APRN/NP empowerment, ICD-10, EMRs, and even good aspects of Obamacare, e.g. patient engagement and evidence based practice?
On recent ONC HIT Policy (recorded) call, MU “MD burdens” raised related to discharge instructions – a process improvement with clear potential to save $Bs over time and positively impact outcomes for virtually every patient, at every encounter. The burden noted was “cost of a printer” and “having to walk to it”. Yet, AHA and House willing to justify millions of dollars and massive human resources spent and potentially squandered on ICD-10?
We can’t function as a “system” if each stakeholder’s only focus is their own profit and agenda, sabotaging the other, without compromise – and be effective in the mission. This is the antithesis of patient-centered care.
In spite of valid concerns and whatever remaining empathy MDs may have, with this latest move – “win” or lose – I believe they’ve jumped the shark.
I’m dealing with a well known hospital vendor who hasn’t delivered yet so I think it’s more than marketing by athena.
I am an Athena user and I can attest that compared to my colleagues who are on different EMR’s we are waaaaay ahead and ready for ICD 10 and Dan is absolutely right in his assesment. It is no different than ” the hardship exemption” for MU 2 that refers to ” vendors readiness” or …”unreadiness” rather.
Concerning Weird News Andy’s report on “dueling paramedics.”. Life imitates art:
https://www.youtube.com/watch?v=aHdAM3qmrao
It was about Chuckles candy.