I've figured it out. At first I was confused but now all is clear. You see, we ARE running the…
News 3/5/14
FCC Chairman Tom Wheeler announces the formation of a task force that will seek ways to increase use of broadband to deliver telehealth, mobile apps, and telemedicine. Heading up CONNECT2HEALTHFCC will be Michele Ellison, a lawyer who runs the agency’s enforcement bureau. Wheeler said in the announcement, “We must leverage all available technologies to ensure that advanced health care solutions are readily accessible to all Americans, from rural and remote areas to underserved inner cities. By identifying regulatory barriers and incentives and building stronger partnerships with stakeholders in the areas of telehealth, mobile applications, and telemedicine, we can expedite this vital shift.”
Reader Comments
From Just Tim: “Re: MU stages beyond stimulus payments. What is the legislative basis to extend the MU program? MU requirements were supposed to run in conjunction with years in which payments were made, not years after penalties kick in. I’d certainly agree that if someone never got to Stage 3, they could reasonably be penalized on an ongoing basis. Otherwise, we’ve just created a large bureaucracy with the power to continue to push unfunded mandates.” Legal scholars and political junkies, the less legislative among us are calling.
From Dim-Sum: “Re: military EHR replacement. Word on the street is that the vendors of choice and partners are as follows. Six service integration (SI) firms will bid Epic. The team that is getting the most news is Leidos/Accenture/Harris. Cerner has a single exclusive SI partner (still doing research to see who that SI is). Allscripts cannot find a partner for their Sunrise. Meditech has the incumbent Northrop Grumman. McKesson walked away from GDIT/Vangent. Siemens has a yet to be named DoD giant. Competitive bids will require an investment by prime and sub software solution firm of about 1.5-2 percent of the total contract value. That means that to win a $5B deal with the DoD, the investment for resources, capabilities, compliance, and regulatory wherewithal (see FISMA, FedRAMP, DIACAP, 508, JITC etc) is $50 million USD. Good Luck beltway bandits and COTS EHR dreamers.” Unverified.
From Brenda: “Re: Washington’s insurance exchange. Add it to the list of those having issues. By the way, I’ve recommended HIStalk to countless people and I’m glad our company has been a sponsor for about a year now.” The Healthplanfinder exchange has 15,000 applications that are stuck because the user-entered information can’t be matched to the state’s Medicaid benefits database or contain incomplete information (hello, programmer edits?) I speculate that the state incurred the wrath of the grammatical gods when it combined “health plan finder” into a single word.
![]() From Charger: “Terrific correspondence from Orlando; much appreciated since I could not attend! I’m sure you have been deluged with coffee mug requests and are out of stock, but may I place an order for one upon receipt of any new inventory? I will gladly swap you one of my local Karl Strauss Brewery pint glasses in return.” Thanks for the generous offer, but sadly all the coveted coffee mugs are gone. Lorre and I are trying to convince Mr. H that the timing is perfect for the opening of an online store featuring HIStalk swag. Beauty queen sash, anyone?
From Charger: “Terrific correspondence from Orlando; much appreciated since I could not attend! I’m sure you have been deluged with coffee mug requests and are out of stock, but may I place an order for one upon receipt of any new inventory? I will gladly swap you one of my local Karl Strauss Brewery pint glasses in return.” Thanks for the generous offer, but sadly all the coveted coffee mugs are gone. Lorre and I are trying to convince Mr. H that the timing is perfect for the opening of an online store featuring HIStalk swag. Beauty queen sash, anyone?
More mug sightings: Investor’s Chair contributor Ben Rooks, who obviously works standing up while looking at green ivy outside his San Francisco office; and Mike Jefferies of Longmont United Hospital, whose Spotify-HIStalk two-monitor setup looks a lot like mine. I still have a few more photos to run next time.
From Dr. Travis: “Re: Nordic’s new office. Thought this was very cool.” I had to clarify with Travis since this is a Midwestern, tailgating, and college thing that much of the country won’t understand: it’s a cornhole platform.
From Ion Exchanger: “Re: HIMSS booth. You had traffic in your booth back in the hall. You should get another exhibitor to give you space free in return for drawing people.” That idea has come up on occasion, although not usually from people offering space. Our first-time exhibitor experience was good, especially since it was a low-rent, homebrew operation designed solely to give Lorre a way to say hello to interested readers and sponsors. I think I’ve decided to do it again in Chicago.
From Dr. Matt: “Re: QlikView. First there’s an Epic partnership and now I find at HIMSS that Health Catalyst offers QlikView on top of their data warehouse. Why are these big players using it?” I’ll let those organizations speak for themselves.
From Doctor N: “Re: HIMSS conference. It was my first one. Only the HIStalk people made me feel valued as a practicing physician. The insults, lack of humility, time away from my clinic, and the lack of vendor understanding of how medicine really works will keep me from returning soon. The sessions could have been done online and the networking conversations were shortened because everyone was in a hurry to get somewhere else. I believe I have seen the American medical industrial complex at its worst. I was surprised at the number of vendor folks who are physicians and how little they know about how we pay for healthcare: SGR (which will worsen matters for providers) and $156 billion being cut from Medicare Advantage plans. They have no clue that I’m not paid for population health and most docs in my community hardly even know the meaning of the term. It is like we are buying the horseshoe, barn, and saddle in the hope that we’ll get a horse for a present. HIStalkapalooza, however, did not disappoint!”
From Spelling CMIO: “Re: a tech solution to HIT spelling problems. As technology professionals, we ought to be able to bring our expertise to bear on the current plague of spelling confusion. I suggest we start to use regular expressions, like: HIM*S* and HIP*A* so that all variants can be brought under the welcoming umbrella of mediocrity. Heck, we could even bust out CM*S to obscure the failure to include ‘and Medicaid’ in the name of our favorite bureaucracy. We could even try E[Pp][Ii][Cc] to free the caps-lock crowd from their yoke of humiliation.” Scanning for “HIMMS” news stories turns up 56, which is pretty sloppy.
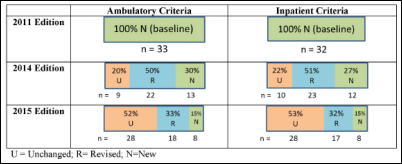
From Frank Poggio: “Re: ONC. Issued new 2015 test criteria while at HIMSS last week. They kept repeating that this new (and extensive at 242 pages) test criteria is ‘voluntary’ for vendors. Here comes another wolf in sheep’s clothing. Do you really think the 2015 Criteria will be ‘voluntary’? How can they generate a revised list of criteria that fixes bugs and not make it required? How can they add something critical to patient safety such as UDI and not make it required? Breaking out CPOE components has been something niche vendors have been asking for since the start. So will those vendors ignore it and stick with 2014 criteria? I have worked through dozens of tests with clients since the inception of ONC and every time they expand or make a test update it soon becomes mandatory by the authorizing testing labs … and with some ATLs sooner than others. I give the 2015 version at most four months before it becomes mandatory.”
HIStalk Announcements and Requests
Listening: new from the all-female, LA-based spacey rock quartet Warpaint, which sounds a bit like Cocteau Twins (and that’s a good thing). I’m also enjoying defunct, brilliant Irish pop band The Thrills.
Some random thoughts I had regarding the HIMSS conference:
- I was surprised and happy that the vendors of much-hyped analytics and population health management products were restrained in their pitch. Many companies talked about those products, but I didn’t hear a lot of wild claims.
- The terms “big data” and “cloud” weren’t repeated reverentially and annoyingly to the extent that might have been expected.
- What is population health management, exactly? It will be whatever payers say it is, no different than “quality.”
- I’m not impressed with “big data” when healthcare is woefully indifferent to “little data.” We ignore evidence-based medicine, warnings for inappropriate or duplicate tests and drugs, and quality measures. We are sloppy about monitoring our supply chain and controlling our labor and materials costs. We pay little attention to the free exchange of information we hold about patients. We don’t like the idea that patients themselves should see our digital secrets. We should be using the information we have to its fullest before trying to tackle giant databases containing even more insights that we’ll ignore. Speak up if your hospital is different.
- I’m not sure if patient engagement was just a token HIMSS nod or a real movement. I don’t see stretched providers getting excited about engaging patients unless government or competitive pressures force them to. It was nice to see patient advocates at the podium, even if only sporadically.
- People are beginning to realize that EHRs aren’t necessarily the center of the universe. Small vendors are creating specific applications that use the EHR, which makes them easier to develop, cheaper, easier to use, and easier to buy since any buyer’s remorse will be several zeroes cheaper than the EHR itself. A question to ask of the dwindling number of EHR vendors might not be what their system does, but what does it allow to have done by other sources? Those companies were in the hall.
- The government has taken a lot of innovation out of the system with Meaningful Use and ICD-10. I said from the beginning that taking MU money means making the federal government your incessantly nagging partner, but with penalties following rewards it wouldn’t have mattered anyway. I got the sense that attendees were more interested in what HHS and ONC say than what vendors were telling them.
- Financial uncertainty as well as a big implementation and optimization ramp-up business has increased the willingness of providers to pay a premium to use consultants since they don’t want to get locked into salaried employees for specific short-life tasks. Consulting companies seemed to be generating a lot of interest.
- Hospitals, like every swollen, inefficient, and political bureaucracy, will do whatever it takes to protect their own interests. They have money and clout and they aren’t just going to happily reduce their profits, headcount, or ambitions to reduce overall healthcare spending. Integrating their acquisitions will be a target market.
- HIMSS is always like a boat show, but this year I’m not sure many boats were sold.
Acquisitions, Funding, Business, and Stock
Telus Health acquires Med Access, a British Columbia-based vendor that claims its EMR is #1 in Canada with 4,000 users.
Clinicient, a provider of RCM and clinical solutions for rehabilitation therapy, raises $15 million in Series C funding from Catalyst Investors and names Rick Jung (Medsphere) chairman and CEO.
Castlight’s IPO could raise up to $140 million based on a revised filing made this week.
Sales
PatientPoint awards Xerox a $28 million contract to work with hospitals and physician practices to introduce PatientPoint’s digital check-in and population health management software and to provide training and support.
Denver Health selects Besler Consulting to assist in the identification of Medicare and Medicare Advantage Transfer DRG underpayments.
UCSF Medical Center will implement Oneview Healthcare’s patient empowerment program at three Mission Bay hospitals.
The University of Miami Health System selects Lockheed Martin to manage its healthcare data, develop predictive models for risk identification, and build automated systems to give providers data at the point of care.
Florida International University’s faculty practice chooses PatientKeeper Charge Capture.
Citizens Medical Center (TX) selects MModal for transcription services and front-end speech recognition.
West Florida ACO will implement eClinicalWorks Care Coordination Medical Record.
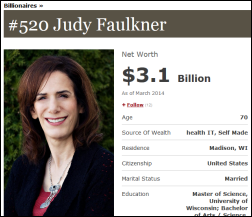
Forbes names Epic’s Judy Faulkner as #520 on its list of “The Richest People on the Planet,” estimating her net worth at $3.1 billion.
People
Accretive Health appoints Patrick Funck (Segwick) SVP/CIO.
HCI Group names Bill Bria, MD (Shriners Hospital for Children) as CMIO and Robert Steele (Sterling Healthcare Initiatives) as SVP of delivery operations.
Greater Houston Healthconnect CEO Jim Langabeer, PhD resigns to return to his previous employer UT Health Science Center, with CTO Phil Beckett, MD named acting CEO.
Carolinas HealthCare System hires Nancy Olson, RN-C, MBA, PhD (Providence Health & Services) as its first chief nurse informatics officer.
Announcements and Implementations
![]() WEDI, in partnership with EHNAC, will create a Practice Management Accreditation Program to review PM vendors in the areas of privacy, security, mandated standards and operating rules, and operational functions. While I am all for having minimum performance standards, is this really the best time to ask vendors to jump through one more hoop to remain competitive in the marketplace? It’s no surprise that we are seeing limited advances in product usability and innovation.
WEDI, in partnership with EHNAC, will create a Practice Management Accreditation Program to review PM vendors in the areas of privacy, security, mandated standards and operating rules, and operational functions. While I am all for having minimum performance standards, is this really the best time to ask vendors to jump through one more hoop to remain competitive in the marketplace? It’s no surprise that we are seeing limited advances in product usability and innovation.
The local business journal profiles St. Francis Hospital (CT), which goes live on Epic next month following a two-year, $120 million transition. Above is VP/CIO Linda Shanley.
Summit Health (PA) implements Wellcentive’s population health management solutions and services.
Ontario’s Group Health Centre goes live on Epic.
Wellmont Health System (TN) transitions to Epic in its physician offices and hospitals.
North Oaks Medical Center (LA) goes live with a two-way interface between Epic and the Masimo Patient SafetyNet remote monitoring and clinician notification system.
GetWellNetwork debuts GetWellNetwork Ambulatory, which is available on mobile and stationary devices and integrates with EHRs to provide personalized information, healthcare tools, and patient pathways.
CoverMyMeds launches an API that enables providers of EHRs, e-prescribing systems, and PM systems to offer an NCPDP standards-compliant electronic prior authorization solution.
John Gomez launches Sensato, which will offer healthcare privacy and security assessments, guidance, and tools.
UC Irvine Health deploys WANdisco and Hortonworks Hadoop data technology to provide real-time information for patient care. They run Allscripts Sunrise, I believe, and an unnamed data warehouse technology described in the announcement as one that “struggles with availability issues as well as the volume and variety of data it can handle.”
Government and Politics
![]() The FDA is seeking a contractor to monitor social media chatter about drugs, medical devices, and other regulated products in order to track conversation shifts following FDA warnings. I found this move especially interesting in light of the heavy Twitter traffic during HIMSS and my realization of the potential value of mined Twitter data. Now I’m wondering if anyone has figured out a way to combine data from social media chatter with old-school opinion polls from phone and mail surveys. That could be powerful.
The FDA is seeking a contractor to monitor social media chatter about drugs, medical devices, and other regulated products in order to track conversation shifts following FDA warnings. I found this move especially interesting in light of the heavy Twitter traffic during HIMSS and my realization of the potential value of mined Twitter data. Now I’m wondering if anyone has figured out a way to combine data from social media chatter with old-school opinion polls from phone and mail surveys. That could be powerful.
ONC releases additional draft electronic clinical quality measures for review and testing for the possible inclusion in the MU and other federal programs.
The front-page story of the March 10 issue of Time says that Healthcare.gov had so many problems that the White House was ready to shut it down and start over right after its launch. It says that it’s not clear even now who was supposed to be in charge of the launch and that people knew upfront that the site’s design was flawed.
Speaking of Healthcare.gov, HHS says it will need $1.8 billion in FY2015 to run the federal health insurance exchange.
Other
A three-year study finds that patient-centered medical homes do little to reduce costs, decrease utilization, or improve care, leading researchers to conclude, “Medical home interventions may need further refinement.”
The use of patient portals for secure messaging does not significantly change the frequency of face-to-face visits, according to a Mayo Clinic study. Weakness of the study are that portal messages were studied in a vacuum rather than in the context of all provider communication, it looked only at the number of visits rather than patient outcomes, and most of the study subjects were Mayo Clinic employees.
Baylor Regional Medical Center announces that it will not accept the Malcolm Baldridge National Quality Award following allegations that it improperly managed a neurosurgeon who is accused of botching surgeries while under the influence of drugs. An extensive profile in the Dallas Morning News paints a disturbing picture of a physician who was labeled a sociopath and serial killer by colleagues. We featured the story in September 2013 with this summary:
A Dallas news magazine recounts the fascinating tale of a newly licensed MD-PhD neurosurgeon whose incompetence left several patients maimed or dead while the state’s medical board couldn’t stop him from practicing. Colleagues called the doctor the worst they had every seen and said his skill level was no higher than a first-year resident as he kept inadvertently slicing arteries causing patients to bleed to death, and in one case the OR team had to forcibly remove him from the OR to prevent him from killing his patient. His marketing team and his 4.5 star Healthgrades.com rating brought in plenty of new patients to his loftily named practice, Texas Neurosurgical Institute. Surgeon readers will be horrified by this recap by a peer who had to clean up one of his messes: “He had amputated a nerve root. It was just gone. And in its place is where he had placed the fusion. He’d made multiple screw holes on the left everywhere but where he had needed to be. On the right side, there was a screw through a portion of the S1 nerve root. I couldn’t believe a trained surgeon could do this. He just had no recognition of the proper anatomy. He had no idea what he was doing.” The article blames the situation on malpractice caps, laws that hold hospitals liable for damages only if their intentions are provably malicious, and a nearly powerless medical board charged more with keeping licensure records and counting CE hours than watch-guarding patient safety.
Mike “PACSMan” Cannavo summarizes HIMSS14 from the imaging perspective in an Aunt Minnie article (simple registration is required.) He tells me that HIMSS rules even though RSNA is a bigger conference because, “The balance of power has definitely shifted from departmental solutions to facility-wide ones and IT and the CIO/CTOs make those decisions here.” Another of his observations:
HIMSS may, and probably will, command the lion’s share of the trade show budgets for VNA and cloud companies from now on. Considering there were more than two dozen vendors playing in this arena alone, plus the majors who showed various central data repository (CDR) solutions, this can affect other trade shows in terms of booth size and revenue. Given that attendance at most radiology-specific shows has been flat or declining and time spent at the shows has declined each year, HIMSS poses even more of a threat.
A group of former senators (Tom Daschle, Trent Lott, John Breaux) forms the noble-sounding Alliance for Connected Care, which will lobby Congress to protect the interests of its big-company members (Verizon, WellPoint, CVS, and Walgreens) as well as patients who benefit from telehealth services. In addition to seeking friendly governmental consideration, the group wants to lift geographic treatment limitations and build the case for telehealth as an effective care delivery mechanism. Surprisingly, HIMSS isn’t among its lengthy list of advisory board organizations. I’m always suspicious of the motivations of retired politicians anxious to make up for the income they lost while holding office, but in this case their announced intentions seem appropriate.
Brian Ahier got a one-on-one interview with National Coordinator Karen DeSalvo at the HIMSS conference. She says everybody has been focused on collecting information via EHRs, but now it’s time to allow patients to participate and acknowledge that “health is more than getting people to a doctor” since only 10-20 percent of outcomes can be attributed to the healthcare system. She clearly has a public health mindset as did her predecessor and she gets a “bravo” for that.
The CFO of Wake Forest Baptist Medical Center (NC) lists reduced Epic expenses as one element of its improved financial performance in which six-month operational losses were reduced from $49.8 million to $23.5 million. The hospital still has high expectations for Epic, saying in a bond ratings agency report, “Management believes that future financial performance must be improved from current levels, and continues to aggressively pursue both short- and long-term strategies to drive growth, reduce cost and leverage our investment in Epic.”
In England, a three-year-old cardiac surgery patient dies when the scheduling system of the hospital to which he was transferred fails to generate his follow-up appointments. According to the hospital’s pediatrics manager, “Samuel’s appointment request must have fallen through the cracks between the old and new system. The new system is now up and running as best as it can be, but as long as there is still humans entering the information there will always be room for error.”
Weird News Andy notes that Banner Health didn’t have a banner day when it inadvertently printed subscriber Social Security numbers on its health magazine’s mailing labels.
Sponsor Updates
- Greenway Medical names Phreesia its Marketplace Partner of the Year.
- Aprima Medical announces that over 1,500 former Allscripts MyWay customers have migrated to its platform.
- PerfectServe introduces automatic electronic PHI filtering capabilities that remove ePHI from the body of messages sent to non-secure mobile devices.
- Lisa Reichard, director of community healthcare relations for Billian’s HealthDATA, writes a fun blog post that includes her top 10 tales and takeaways from HIMSS14.
- Extension Healthcare will participate in the AONE 2014 Annual Conference in Orlando March 12-15.
- The Tennessean interviews Cumberland Consulting Group CEO Jim Lewis about the company.
- Boston Software Systems offers a white paper that examines three steps to a successful migration.
- An HCS case study highlights Christian Health Care Center (NJ) and the benefits it realized following the implementation of HCS Interactant.
- TriZetto Provider Solutions advises customers that it will continue to accept claims in print image, NSF, and legacy formats even after the ICD-10 implementation deadline.
- E-MDs publishes video testimonials from multiple providers.
- Clinithink’s VP of solutions Russ Anderson suggests leveraging the use of Clinical Natural Language Processing to control patient leakage.
- Health Catalyst offers a white paper with keys to a successful data warehouse and analytics implementation.
- Vital Images experiences significant growth across Europe, the Middle East, and Europe.
- CommVault achieves certified integration with its Simpana 10 software and the SAP HANA platform.
- TeleTracking Technologies, Hill-Rom, and GOJO will co-market integrations with the Hill-Rom Hand Hygiene Compliance solution.
- Cornerstone Advisors reports that its staff has grown to 39, a 25 percent increase in the past year.
- Divurgent will provide support to Medsphere clients in their MU, ICD-10, and value-based purchasing initiatives.
- Gartner positions Qlik in the Leaders Quadrant of the 2014 BI and Analytics Platform Magic Quadrant report.
- HIMSS Analytics names Allscripts its first Certified Educator of the EMR Adoption Model.
- The Cleveland Clinic and Dell will offer Epic EMR consulting and implementation services to other health systems and practices.
Contacts
Mr. H, Inga, Dr. Jayne, Dr. Gregg, Dr. Travis, Lt. Dan, Lorre.
More news: HIStalk Practice, HIStalk Connect



























Re: Dr. N’s comment(s): Only the HIStalk people made me feel valued as a practicing physician. The insults, lack of humility, time away from my clinic, and the lack of vendor understanding of how medicine really works will keep me from returning soon.
I’m sorry to hear that you had that experience, Dr. N, and no surprise about your positive HIStalk experience. But, something struck me about your remarks that, although not excusing it, might be worth a thought. You suggested that vendors did not make you feel valued as a physician and seem to lack understanding of how medicine really works. It is possible that you may not be aware that when many of these vendors visit your office and those of your colleagues, they are typically kept at bay by your staff, so struggle to have access to you in order to learn about your practice and workflows. We all understand that your time is precious and you can’t meet with every sales rep that crosses the door.
Again, I’m not intending to excuse rude behavior, but I’m betting that most vendors have a story or two about how they felt disrespected and devalued by physicians and their staff while trying to do their job. I hope you won’t give up on the good things you gained from HIMSS and try again. I have watched this mutual disdain between physicians and vendors for years now. It’s getting a little better, but I think we have a long way to go. There is so much to be gained by all stakeholders in this HIT effort (physicians, vendors, government, and yes, even HIMSS, etc.) recognizing that we all have a role to play and no one is any better than anyone else.
Whaddya say we ALL start tomorrow!??
Hmmm…. let me get this straight. Washington Healthplanfinder is having issues with 15,000 of the more than three quarters of a million applications they have processed? That’s two percent default rate – a miracle given what state’s had to put up with. And 6,000 of those are because the state has the wrong information, not the Healthplanfinder, and another 5,000 because applications are not complete? I am not sure this is actually an issue with the Healthplanfinder as much as it is with the old state database and user error.
@Spelling CMIO: Y*r idea to use wildcards is interesting, but doesn’t go far enough, in my opinion. Th*r are t* many people who can’t be bothered with more basic things d* t* th*r lack of time, education, lack of precision, etc. Substitutions could be made for all commonly made mistakes (their/they’re/there, too/to/two, do/due, …).
Regarding Dr. Matt’s question about QlikView and Health Catalyst… We try to build solutions that are based upon an amalgam (no pun intended) of the best products in the market so that when clients look at our solutions in detail, they don’t see a highly proprietary solution but instead react as if, “This is something that I would build if I had the years of analytics experience and development team to do the same.”
The data visualization market is in very good shape now; better than it has ever been. It will be one of the fastest moving markets in the analytics space of the future, with vendors constantly leapfrogging one another. There are lots of good options out there right now. QlikView is the best overall data visualization tool on the market and Health Catalyst has evaluated every option imaginable– Tableau, Spotfire, Cognos, BusinessObjects, GoodData, etc. You can develop applications in QV about 3x faster than the next best product, which suits an agile development environment, like Health Catalyst. It fits very well with a late binding data warehouse platform, too. QV alone is not a good choice if you are working in a complex data environment with multiple source systems, and you are trying to bind that disparate data together in registries and other complex analytic use cases– you need an underlying data warehouse for those scenarios, with a QV layer on top. Health Catalyst does not use QV for QV’s data integration tools– we use it for data visualization and presentation.
One last comment: A single data visualization tool will not meet the needs of every analytic customer in a healthcare organization– in other words, a tool like QV will meet a large number of those customers, but not all. You need an underlying data warehouse platform that can support other data visualization and presentation tools like Excel, Access, R, SAS, et al.
Hope that helps… let me know if not.
–Dale Sanders, SVP, Health Catalyst
Re: On ‘timing is perfect for the opening of an online store featuring HIStalk swag. Beauty queen sash, anyone?”… that was very funny … and … priceless !!
Re: MU stages beyond stimulus payments. What is the legislative basis to extend the MU program..
The original draft rules for the HiTech act did show only 3 Stages, but when ONC published the final rules for Stage 1 way back in 2010 they specifically said there ‘may’ be more than three stages. Congress in ARRA and the HiTech act never stipulated the specific number of Stages. ONC can be as creative as they want. They are already talking about Stage 4.
To quote Nancy Polosi, who had time to read a 1,000 page bill! Just let the bureaucrats figure it out.
Frank – what does the legislation actually say on it?
ONC didn’t write the law.