RE the AI GLP1 company, Washington Post has an article today by someone who used one of those compounded products,…
News 11/8/13
Allscripts reports Q3 results: revenue down 8 percent, adjusted EPS $0.05 vs. $0.23, missing estimates on both. By GAAP standards, the company lost $48.9 million in the quarter. The company also announced that it has fired Cliff Meltzer, EVP of solutions development since July 2011, and will pay him severance that includes his expected one-year salary and bonus totaling $900,000. A reader’s rumor suggests that former Jardogs CEO Jim Hewitt, named Allscripts SVP of development after the the company acquired Jardogs in March 2013, will replace Meltzer. I interviewed Hewitt in June 2012.
Reader Comments
![]() From HerkyHawk: “Shoes. A Symantec representative was wearing these shoes at the Virginia HIMSS meeting. They serve a dual function: conversation starter and castrator for when she gets angry.” Readers often send me photos of fun shoes, for which I am thankful. This shoe earned a rare mention on HIStalk because its owner clearly understands that shoes offer so much more than foot protection.
From HerkyHawk: “Shoes. A Symantec representative was wearing these shoes at the Virginia HIMSS meeting. They serve a dual function: conversation starter and castrator for when she gets angry.” Readers often send me photos of fun shoes, for which I am thankful. This shoe earned a rare mention on HIStalk because its owner clearly understands that shoes offer so much more than foot protection. 
HIStalk Announcements and Requests
![]() A few goodies you may have missed from HIStalk Practice this week include: the implementation of HIT in practices reduces the demand for physicians. CMS says it’s not appropriate to charge patients a fee to access their records online. A reader worries about ZocDoc and HIPAA compliance. Lawmakers consider phasing out fee-for-service billing in favor of rewards-based models. The government shutdown delays the release of the 2014 Medicare physician fee schedule. Jaffer Traish of Culbert Healthcare Solutions discusses EHR clinician adoption and change management. Dr. Gregg shares a post-Halloween nightmare. Julie McGovern of Practice Wise offers advice for providers seeking a replacement EMR product. Micky Tripathi’s “Pretzel Logic” post is called Have Sympathy for Your Vendor. Thanks for reading.
A few goodies you may have missed from HIStalk Practice this week include: the implementation of HIT in practices reduces the demand for physicians. CMS says it’s not appropriate to charge patients a fee to access their records online. A reader worries about ZocDoc and HIPAA compliance. Lawmakers consider phasing out fee-for-service billing in favor of rewards-based models. The government shutdown delays the release of the 2014 Medicare physician fee schedule. Jaffer Traish of Culbert Healthcare Solutions discusses EHR clinician adoption and change management. Dr. Gregg shares a post-Halloween nightmare. Julie McGovern of Practice Wise offers advice for providers seeking a replacement EMR product. Micky Tripathi’s “Pretzel Logic” post is called Have Sympathy for Your Vendor. Thanks for reading.
HIStalkapalooza planning has begun for the February 24 event at the HIMSS conference in Orlando. It’s too early to announce the sponsor, venue, and other details (registration won’t start until right after New Year’s) but I always get requests from companies asking about co-sponsoring it along with the primary sponsor. The previous sponsors have always declined to share the limelight, but this one is OK with the idea and has a plan for providing exposure and recognition at the event because it’s going to be really big and impressive. Let me know if your company is interested.
Acquisitions, Funding, Business, and Stock
Verisk Analytics reports Q3 results: revenues up 10 percent, adjusted EPS of $0.62 vs. $0.54, missing analyst estimates on both measures. The company noted that its “healthcare business delivered growth that was below” plan, but it remains “enthusiastic” about the longer-term outlook.
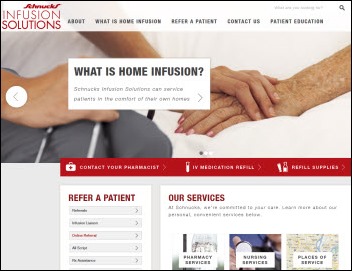
Midwest grocery chain Schnucks follows its competitor Walgreens by opening its first 6,500 square foot IV infusion center, offering patients free Internet access, a TV, a snack bar, and evening and weekend appointments. The center’s pharmacist and two nurses can either infuse the medications on site or prepare them for home administration.
Sales
In England, BT selects Harris Corporation to supply clinical portal solutions for health and social care organizations across the NHS.
The California Office of Health Information Integrity awards contracts to Humetrix, UC San Diego Department of Emergency Medicine, and the Santa Cruz HIE to participate in a PHR demonstration project.
Huntsville Memorial Hospital (TX) selects StrataJazz from Strata Decision Technology for cost accounting, operating budgeting, long-range financial planning, and capital planning.
Mammoth Hospital (CA) chooses the MEDHOST emergency department information system.
People
Coker Group hires Jeffrey T. Gorke (Castle Gate Management) as SVP of practice management.
VA’s acting CIO Stephen Warren is named executive in charge of the office of information and technology and CIO.
Capsule names Didier Argenton (Siemens Healthcare) as VP of international sales.
Patricia Sengstack, DNP, RN, formerly deputy CIO of NIH and currently president of the American Nursing Informatics Association, is hired as chief nursing informatics officer of Bon Secours Health System (MD).
Announcements and Implementations
Software Testing Solutions will provide automated testing services for Sysmex WAM decision support software for the clinical laboratory, validating the system’s rules, application settings, and workflow practices.
Surescripts adds 12 Epic health systems to its national clinical network, including Swedish, UCSD, UCSF, and Community Health Network.
pMD expands its charge capture secure messaging feature with real-time alerts and direct text messaging.
Government and Politics
CMS CIO Tony Trenkle will leave the agency, according to an internal email sent to CMS employees.Trenkle oversaw $2 billion in annual IT products and services, including the development of the healthcare.gov website. Dave Nelson, the current director of the office of enterprise management, will serve as acting CIO.
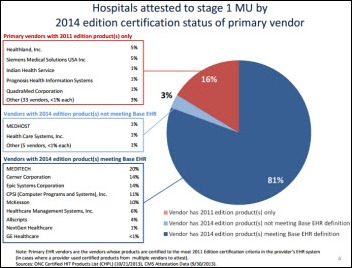
CMS paid $16.5 billion in EHR incentive payments to over 325,000 EPs and hospitals through the end of September. Customers of Meditech, Cerner, and Epic account for almost half of all hospitals that have attested for Stage 1 MU; customers of Epic, Allscripts, eClinicalWorks, and NextGen represent almost half of all EPs that have attested for Stage 1.
USO CEO Sloan Gibson, the President’s nominee for the VA’s deputy director position, says in his nomination hearing that he will focus on the agency’s disability claims backlog and the integrated EHR (i-EHR) project of the VA and Department of Defense.
The Military Retirement and Compensation Modernization Commission, reviewing the failure of the VA and Department of Defense to create a single EHR, floats the idea of combining the entire health systems of the VA and DoD into a single organization, with former Senator Bob Kerry stating, “If [VA and DoD] can’t work together, put one of them in charge. Pick your poison, I don’t care which one. Create a unified command with DoD or put VA in charge.” Former Indiana Congressman Stephen Buyer agreed by saying, “If you had one chief information officer in charge of budget and line items for both, this problem and many others would not be an issue.”
I signed up on Healthcare.gov this week just to see what all the fuss was about. I have to say it was a pleasant experience – the much-criticized identification system worked great and the entire process to get quotes took maybe five minutes. Once I saw the prices I’m glad I have hospital-subsidized medical insurance. I wasn’t as pleased with the site when I logged back in later – it seemed to be confused that I had requested quotes without buying insurance, and I kept getting warnings about pending messages when there weren’t any. Trying again just now, all I got was a blank screen with no options, and clicking the “Get Insurance” tab just took me back to the default page.
Other
Jackson Health System (FL), planning how it will spend the $830 million it will get from a just-passed property tax referendum, says it will upgrade rather than replace Cerner with the $130 million that is intended for EMR-related improvements.
An investigative report finds that financially struggling Lifespan (RI) paid its now-retired CEO $8 million in 2011, raising his 14-year total compensation with the organization to $39 million.
HIMSS, trying to ensure that FDA doesn’t regulate EHRs as medical devices, proposes to HHS a “risk-based oversight framework” that would consider the risk when used as intended and the cost vs. benefit of oversight. It makes sense – HIMSS points out that non-clinical IT that has no patient safety implications doesn’t oversight. They also don’t want vendors to be solely responsible, with surveillance and reporting responsibilities to be shared among vendors, providers, and government. They suggest that vendor responsibility ends once their control of their product ends, such as when users customize it.
Weird News Andy is at a loss for all but one word: unbelievable. A man claims that city police in Deming, NM pulled him over for rolling through a stop sign at Walmart, then decided from his posture and previous behavior that he was hiding drugs in his anal cavity. A judge issued a cavity search warrant but the local ED doc refused to do it, saying it was unethical. The man was then taken to Gila Regional Medical Center, which obliged by performing two sets of x-rays, two rectal probes, three enemas, and a colonoscopy, all without the man’s consent and with no drugs were found. The hospital is adding its own version of anal intrusion to the story by not only billing the man, but threatening to turn his debt over to collectors.
Sponsor Updates
- Informatica achieves top marks for customer loyalty, overall quality of products, and product reliability in the 2013 Data Integration Customer Satisfaction survey.
- Halim Cho, director of product marketing for Covisint, will discusses the importance of cloud identity and access management at the November 20 Gartner Identity and Access Management Summit in Los Angeles.
- Intelligent InSites VP Marcus Ruark presents on the value of operational intelligence at this week’s Data Intelligence for Health Care Conference.
- QuadraMed will add Health Language terminology management solutions to its QCPR platform.
- Bottomline Technologies hosts its second annual Healthcare Customer Insights Exchange this week in Del Mar, CA.
- Airwatch secures additional office space for its UK facility to accommodate recent growth.
- Verisk Health publishes its schedule of events through the end of the year.
- Vocera’s chief medical officer Bridget Duffy offers ideas for improving patient satisfaction scores.
- eClinicalWorks CEO Girish Navani predicts that patient engagement and population health management will become essential components of EHRs.
- Predixion Software publishes a white paper on embedding predictive analytics into software.
- PGA Championship winner Jason Dufner gives Greenway employees a putting clinic.
- Hayes Management Consulting provides details on its monthly webinar series.
- HIStalk sponsors named to the Thomson Reuters 2013 Top 100 Global Innovator list include 3M, AT&T, Fujifilm, GE, NTT, and Xerox.
- PeriGen hosts a November 13 webinar on labor progress as part of its inaugural webinar series on excellence in perinatal care.
- ZirMed’s Betty Gomez discusses risk mitigation strategies for ICD-10 at next week’s WEDI 2013 Fall Conference in Maryland.
EPtalk by Dr. Jayne
News flash: CMS requests public comments on potential Clinical Quality Measures for Stage 3. The measure specifications are published on the CMS website for your review. If you don’t have any exciting social plans for the weekend, I’m sure it will be a good read. The comment period closes on November 25.
You know you’re a clinical informatics propeller head when you find a quote like this one funny. It’s gone somewhat viral in the health care IT universe since being shared on Twitter last week. I have a medical student working with me this month and he almost spit his coffee when I turned my laptop so he could read it. It’s true, though – lots of people are talking about doing it, but the realities of actually doing it are very different.
My own health system has a vision of big data. They’re spending loads of money building various analysis platforms since they never met a homegrown application they didn’t like. There is a herd of project managers and marketing types that has embarked on a road show to extol the virtues of big data. It’s exciting to hear them talk to groups of physicians about the vision for the future, when they will bring together data from our EHR with payer and community data and use it to change the world.
Call me cynical, but rather than pin all our hopes for the future on a project that is just getting started, perhaps it would be a good idea to go ahead and use what we already have to start changing how we practice. We’re fortunate to have selected an ambulatory EHR that has robust reporting capability. It also can automatically send patient-specific tasks to the care team when test results are overdue, when preventive services need to be scheduled, or when clinical values are out of range. A couple of years ago we bought additional hardware to be able to run over 250 clinical reports and tasks from them, but the servers are largely sitting idle.
Why is this happening? My theory is this. Unlike a certain baseball field in Iowa, if you build it, they may not come. Our physicians are deathly afraid of these reports and what they represent. They’re worried about liability – specifically, the liability of having these patient care tasks and not having the staff to work them. They’ve been told that having a report that they don’t take action on is riskier than having no report, so they have not allowed us to enable them for their practices. They feel trapped in a Catch-22 — if they can demonstrate higher clinical quality they hope to negotiate better reimbursement for their services, but they can’t demonstrate quality because they can’t afford the staff to drive it.
It’s easy to say that physicians should cut their take-home pay and hire more staff, but it’s not realistic. In our group, primary care physicians make less than half of what their subspecialty peers make and typically work longer hours in the office and hospital. The bulk of our primary care growth has been with younger physicians who are still paying off student loans debt that is higher than the mortgage on a McMansion. Our starting salary for most new primary care physicians is barely more than IT managers make.
This brings me to the point of why I have a medical student working with me. He’s in his fourth year and is a smart cookie, but is no longer sure he actually wants to be a physician. He sees the long hours that his faculty preceptors put in and the sacrifices their families have made and doesn’t feel it’s worth it any more. So, with over $180,000 in student loan debt, he’s looking for a way to leverage his clinical knowledge and critical thinking skills in the healthcare field. Unfortunately, learning about the complexities of the Meaningful Use program, the transition to ICD-10, billing requirements, documentation standards, the plethora of audits that we face, and the overall anarchy found in the healthcare system may be driving him out of medicine altogether.
One of the more challenging aspects of working with him has been trying to help him make sense of everything. Much of what we deal with defies logic and pushes the bounds of reason. When I delivered his mid-rotation evaluation, I asked what part of our time together he enjoyed most and he said it was the more IT-focused meetings we’ve had. We’ve been through some highly technical discussions the last few weeks about server virtualization, hardware and operating system upgrades, backups, redundancy, and off-site storage. I asked him what he found appealing about that and he said it was the fact that it was logical and made sense.
I’ve got another two weeks with him, so there’s hope, but it’s been interesting to see his reaction to the things that CMIOs deal with every day. At best I want to convince him to complete an internship so he can be fully licensed and will have more options than if he decides not to pursue additional clinical training. But in the mean time, I’m sure I can come up with plenty of sticky hardware and infrastructure issues to keep him occupied.
Do you work with medical students? What do they think about healthcare IT? Email me.
Contacts
Mr. H, Inga, Dr. Jayne, Dr. Gregg, Lt. Dan, Dr. Travis.
More news: HIStalk Practice, HIStalk Connect.
















Re: Med students and informatics. I am an informaticist but interact with med students as a clinician. I have found that the interest from med students is not tremendous, but have always chalked that up to them being overwhelmed with just learning how to be doctors. I would love to see informatics more deeply integrated into the med school curriculum, but at the same time I have to acknowledge that the curriculum is already so jam-packed with add-ons to the basics of medicine that it may not serve anyone well to cram informatics in there as well.
Dr. J,
Your comment:
“My own health system has a vision of big data. They’re spending loads of money building various analysis platforms since they never met a homegrown application they didn’t like. There is a herd of project managers and marketing types that has embarked on a road show to extol the virtues of big data. ”
…reminds my of my last Readers Write ” Big Data the next Big HIT Boondoggle?”
http://histalk2.com/2013/09/09/readers-write-big-data-the-next-hitemr-boondoggle/
Thanks for posting about Patricia Sengstack! It’s nice to see a woman on the people page for a change. 🙂
We used to call Cliff “the ghost” because we never saw or heard from him during the time I worked on Allscripts’ development team. I am amazed that he’s getting almost $1,000,000 in ‘go-away’ pay considering he didn’t really do anything at all in his 2+ years there.
A really big task for Mr. Hewitt. I know Jim as a pragmatic leader that gets projects done. It will be interesting to see if he can get a large development organization working together.
Everyone is partying once the news came out …… especially the remote employees he required to move into offices and Malvern, PA and other offices that were closed . In his arrogance, he created such a debacle within the organization that no one trusts the word of upper mangement. Many, many talented Developers and Testers left (and are leaving) who knew the Sunrise product very well. Very sad so many peoples lives were affected by this bad decision and that he gets rewarded for this.