Thank you for the mention, Dr. Jayne — we appreciate the callout, the kind words and learning more about the…
News 8/30/13
HHS and the Illinois attorney general announce that they will investigate the July 15 theft of four unencrypted Advocate Medical Group desktop computers that contained the medical information of 4 million patients, announced last week. An HHS spokesperson signaled the financial exposure the medical group is facing in describing the “high-profile actions that have sent clear messages to the industry that we expect full compliance with privacy and security rules.” Advocate admits that the information should never have been stored on the hard drives. Obviously encryption technology would be throwing off some impressive ROI right about now, which might be something to consider if your organization hasn’t implemented it.
Reader Comments
From Ron Mexico: “Re: [executive’s name omitted]. Leaving Allscripts, heading to Fletcher Allen to increase its ROI on Epic.” Unverified, so I left the name off for now, even though it’s obvious because he already works at Fletcher Allen part time.
From HIS Junkie: “Re: Sutter’s Epic downtime. To deploy Epic over a broad environment you have to create a ‘Citrix monster.’ That’s a classic sledgehammer solution to a legacy problem, far more likely to fail than a state-of-the-art system that is truly Web developed and deployed. One would think a competent competitor could really leverage that … but then where’s the competent competitors?” Speaking of Sutter, here’s the official response to our downtime inquires from spokesperson Bill Gleeson:
Sutter Health undertook a long-planned, routine upgrade of its electronic health record over the weekend. There’s a certain amount of scheduled downtime associated with these upgrades, and the process was successfully completed. On Monday morning, we experienced an issue with the software that manages user access to the EHR. This caused intermittent access challenges in some locations. Our team applied a software patch Monday night to resolve the issue and restore access. Our caregivers and office staff have established and comprehensive processes that they follow when the EHR is offline. They followed these procedures. Patient records were always secure and intact. Prior to Monday’s temporary access issue, our uptime percentage was an impressive 99.4 percent with these systems that operate 24/7. We appreciate the hard work of our caregivers and support staff to follow our routine back-up processes, and we regret any inconvenience this may have caused patients. California Nurse Union continues to oppose the use of information technology in health care but we and other health care provider organizations demonstrate daily that it can be used to improve patient care, convenience and access. While it’s unfortunate the union exploited and misrepresented this situation, it comes as no surprise given the fact that we are in a protracted labor dispute with CNA.
HIStalk Announcements and Requests
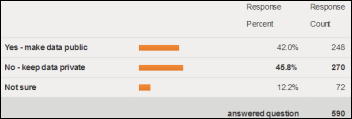
![]() Highlights from HIStalk Practice this week include: Physicians are split when it comes to publicly sharing Medicare payment data. New York physicians are required to consult an electronic prescription database before writing scripts for controlled substances. The benefits of a practice’s ACO participation reach beyond the patients covered by the ACO. MGMA offers online scheduling tools for its annual conference. More than 90 percent of office-based physicians accept new Medicare patients, which is about the same percentage that accept new privately insured patients. The AMA urges CMS to prohibit insurers from paying physicians less than contracted amounts when reimbursing providers with plastic or virtual credit cards. Doximity says it has more physician members than Sermo. I look at the Stage 2 dilemma, highlighting the recommendations of various professional organizations and offering my opinions, namely that CMS should keep the January 2, 12014 start date but extend the deadline for meeting Stage 2 requirements. You won’t find any of these stories – and others – on HIStalk so keep reading HIStalk Practice if you like staying current with happenings in the ambulatory HIT world. Thanks for reading.
Highlights from HIStalk Practice this week include: Physicians are split when it comes to publicly sharing Medicare payment data. New York physicians are required to consult an electronic prescription database before writing scripts for controlled substances. The benefits of a practice’s ACO participation reach beyond the patients covered by the ACO. MGMA offers online scheduling tools for its annual conference. More than 90 percent of office-based physicians accept new Medicare patients, which is about the same percentage that accept new privately insured patients. The AMA urges CMS to prohibit insurers from paying physicians less than contracted amounts when reimbursing providers with plastic or virtual credit cards. Doximity says it has more physician members than Sermo. I look at the Stage 2 dilemma, highlighting the recommendations of various professional organizations and offering my opinions, namely that CMS should keep the January 2, 12014 start date but extend the deadline for meeting Stage 2 requirements. You won’t find any of these stories – and others – on HIStalk so keep reading HIStalk Practice if you like staying current with happenings in the ambulatory HIT world. Thanks for reading.
Welcome to new HIStalk Platinum Sponsor InterSystems. The company is a global leader in software for connected care. Its products empower healthcare professionals with the information they need to make the best clinical and business decisions. HealthShare is a strategic platform for healthcare informatics, enabling information exchange and active analytics across a hospital network, community, region or nation. Cáche is the world’s most widely used database system in healthcare applications. Ensemble is a platform for rapid integration and the development of connectable applications. InterSystems has more than 35 years of experience as a trusted partner serving thousands of physicians, hospitals, and health systems around the world, including Johns Hopkins, Kaiser Permanente and Memorial Care; five statewide HIEs; and the national health systems of Sweden and Scotland. The company’s technology is also used by over 100 leading healthcare software vendors in their solutions, including 3M Health Information Systems, Epic, and GE Healthcare. Thanks to InterSystems for supporting HIStalk.
A YouTube cruise turned up this video about InterSystems. I thought I knew the company pretty well, but I learned a lot about them.
On the Jobs Board: Staff Engineer (Java), Clinical Applications Consultant, Project Manager.
CareTech Solutions will present “Using Infrastructure and Application Monitoring to Assure an Optimal User Experience” on Thursday, September 19, 2013 at 1:00 p.m. Eastern. The presenter will be John Kaiser, senior director of the Pulse IT monitoring service. The abstract:
It’s time for hospital IT monitoring to mature – from reactive to predictive. Supporting the highly-complex healthcare technology environment with only individual monitoring tools or relying on an application vendor to identify system degradation is not the most effective means to providing users with a reliable, optimal IT experience. A comprehensive monitoring solution includes eyes on servers, network, application performance, and real user monitoring. CareTech Solutions will discuss an integrated approach to comprehensive monitoring of both the infrastructure and applications, with an emphasis on delivering a consistent solution based the hospital’s IT maturity level. The target audience is CIOs, CMIOs, CNO, IT directors, and IT analysts.
Acquisitions, Funding, Business, and Stock
The healthcare IT business unit of Tennessee-based Parallon Business Solutions, itself a subsidiary of Hospital Corporation of America (HCA), merges with Vision Consulting to form Parallon Technology Solutions, with Vision President Tim Unger taking the CEO role. Parallon Business Solutions has 24,000 employees and provides services to 1,400 hospitals and 11,000 non-acute care providers.
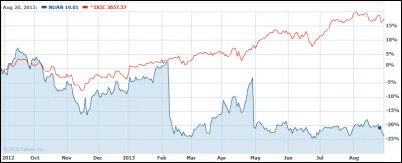
Carl Icahn boosts his stake in Nuance to 16.9 percent of the outstanding shares, according to an SEC filing Tuesday, saying he may want to talk to the company about adding his slate of nominees to the board. Above is the one-year NUAN share price in blue vs. the Nasdaq in red.
Sales
Blessing Physician Services will deploy Phytel’s population health management suite.
Rideout Health (CA) will roll out Perceptive Software’s Enterprise Content Management solution integrated with its McKesson Paragon HIS.
People
McKesson Specialty Health and the US Oncology Network appoints Michael V. Seiden, MD (Fox Chase Cancer Center) CMO.
Physician RCM provider MedData promotes Ann Barnes from president to CEO.
Announcements and Implementations
Australia’s Noarlunga Hospital activates Allscripts Sunrise Clinical Manager.
Novant Health (NC) reports that 343 of its physician clinics are now live on Epic’s PM platform and 316 are live on EHR. The five-year project was completed three years ahead of schedule and under budget.
Humana and Centene join Verisk Health as founding members of its pooled data initiative, which uses Verisk’s database of cross-payer information and analytics to identify illicit billing practices.
Hawaii Advanced Imaging Institute upgrades to RamSoft’s PowerServer RIS/PACS/MU radiology workflow application.
Home device manufacturer Bosch Healthcare and health content vendor Remedy Health Media announce a partnership to develop and sell products for remote patient monitoring.
Government and Politics
ONC opens the Behavioral Health Patient Empowerment Challenge to highlight existing technologies to help patients manage their mental health or substance use disorders.
A Washington Post article says that the Department of Veterans Affairs was paying bonuses to its disability claims employees despite a mammoth backlog, thereby encouraging them to game the system by pushing the tough claims aside to boost their numbers. It does point out that employees were handling high claims volumes even though the number of claims made the backlog grow.
Other
![]() Skyline Exhibits provides trade show stats that vendors might use to justify for exhibiting: (a) 81 percent of trade show attendees have buying authority; (b) the top reason for attending is to see new products; and (c) building brand awareness is the highest marketing priority for most exhibitors. Marketing execs may very well need to look for justification considering that a 10×10 booth at HIMSS costs about $4,000. Tack on drayage, shipping, travel, trinkets, and personnel and you’re at $20K in no time.
Skyline Exhibits provides trade show stats that vendors might use to justify for exhibiting: (a) 81 percent of trade show attendees have buying authority; (b) the top reason for attending is to see new products; and (c) building brand awareness is the highest marketing priority for most exhibitors. Marketing execs may very well need to look for justification considering that a 10×10 booth at HIMSS costs about $4,000. Tack on drayage, shipping, travel, trinkets, and personnel and you’re at $20K in no time.
![]() Coming to a baby shower near you: a smart sock from Owlet Baby Care that monitors a baby’s vitals and sleep position and includes a four-sensors pulse oximeter, an accelerometer, a thermometer, and a transmitter to send data to a smartphone or computer. The company’s cofounder says the device does not require FDA clearance, though a version that includes an alarm system for oxygen levels will. Owlet is seeking $100K in crowdfunding.
Coming to a baby shower near you: a smart sock from Owlet Baby Care that monitors a baby’s vitals and sleep position and includes a four-sensors pulse oximeter, an accelerometer, a thermometer, and a transmitter to send data to a smartphone or computer. The company’s cofounder says the device does not require FDA clearance, though a version that includes an alarm system for oxygen levels will. Owlet is seeking $100K in crowdfunding.
![]() Here’s a story of interest to anyone in charge of their organization’s encryption efforts. UT Physicians (TX), the medical group practice of the UTHealth Medical School, notifies 600 patients of a potential data breach after the theft of an unencrypted laptop. Unlike similar thefts at other organizations, UTHealth has a comprehensive encryption policy that covers more than 5,000 laptops. The stolen laptop was overlooked, however, possibly because it was attached to an electromyography machine in the orthopedics department and is considered more of a medical device than a standard computer. The laptop included patient names, birth dates, and medical record numbers, but no financial information.
Here’s a story of interest to anyone in charge of their organization’s encryption efforts. UT Physicians (TX), the medical group practice of the UTHealth Medical School, notifies 600 patients of a potential data breach after the theft of an unencrypted laptop. Unlike similar thefts at other organizations, UTHealth has a comprehensive encryption policy that covers more than 5,000 laptops. The stolen laptop was overlooked, however, possibly because it was attached to an electromyography machine in the orthopedics department and is considered more of a medical device than a standard computer. The laptop included patient names, birth dates, and medical record numbers, but no financial information.
Researchers in Canada find that the use of RFID badges raised the handwashing compliance of nurses from 33 percent to 69 percent. Their study appears in the current issue of CIN (Computers, Informatics, Nursing). I wasn’t familiar with that journal even though it’s been around in various forms since 1983, but it looks decent.
Fourteen-hospital Baptist Memorial Health Care Corp. lays off 61 employees, including pharmacists and nurses, but urges them to reapply for 500 open positions, many of those newly created to support its Epic rollout.
If you’re a fan of evidence-based medicine or Coldplay, you’ll like this video, which was tweeted by Farzad Mostashari.
Spectrum Health (MI) fires several employees after one of them takes a picture of an ED patient’s rear and posts it to Facebook with a caption of, “I like what I like.” The health system fired the employee who took the picture and all of those who gave it a Facebook Like, including an ED doctor.
Marin General Hospital (CA) asks the FBI to investigate a possible scam that shut down the phones in labor and delivery and the ED last week.
Liviam announces its Facebook-like site for long-term hospital patients, which offers the CareStream timeline, a dashboard from which the patient can request help, a blogging tool, and an events calendar.
New York prescribers issuing prescriptions for pain meds must first check an online registry of pharmacy-reported filled narcotics prescriptions as of this past Tuesday, implemented to help curb the abuse of addictive drugs.
Sponsor Updates
- Truven Health Analytics offers free access to Micromedex iPhone apps for customers outside the US and Canada. Truven also announces enhancements to its Unify Population Health Management solution, which is deployed in partnership with CareEvolution.
- Iatric Systems announces that its Meaningful Use Manager and Public Health Syndromic Surveillance products have earned 2014 ONC HIT certification.
- IHS names Merge Healthcare the leading provider of vendor-neutral archive solutions in the world and in the Americas.
- iSirona adds Singapore-based telehealth services provider myHealth Sentinel as a reseller.
- The Massachusetts eHealth Institute awards Aprima Medical a $101,000 grant to advance the interoperability of EHRs with the state’s HIE.
- Besler Consulting releases a review of the FY2014 Hospital Inpatient Prospective System final rule.
- InstaMed achieves Phase III CAQH CORE certification.
- EClinicalWorks names HealthNet (IN) the winner of its Improving Healthcare Together video contest. Auburn Medical Group (GA) and Open Door Family Medical Centers (NY) took second and third places.
- Aspen Advisors shares details of the ICD-10 preparation services it delivered to East Jefferson General Hospital (LA).
- Dearborn Advisors discusses the need for healthcare organizations to optimize their EHRs in order to thrive in today’s regulatory climate.
- API Healthcare highlights the importance of meeting the needs of an aging workforce.
- pMD announces that its mobile charge capture solution will support iOS 7, which has a possible September 10 general availability.
- Visualutions will resell Wellcentive’s Advance to FQHCs.
- RazorInsights will showcase its ONE Enterprise HIS solution at the 15th Annual HIS Pros Buyer’s Seminar next month in Rosemont, IL.
- Medicomp hosts its annual strategy update webinar September 18 and 19 and opens registration for MEDCIN U sessions November 3-5 in Reston, VA.
EPtalk by Dr. Jayne
It’s quite a challenge to try to keep up with Mr. H and Inga in finding newsworthy items each week for EP talk. Between our day jobs and our staggered publishing schedules, it’s easy to be scooped by another member of the HIStalk crew. In the spirit of mixing things up, we’ll be taking EPtalk in some new directions. I may write up an interesting product, discuss a recent journal article, or respond to something I’ve seen in social media. Since EPtalk runs with the news each week with a slightly different audience than Curbside Consult, I may do some multi-part pieces to allow reader responses to influence the next week’s piece.
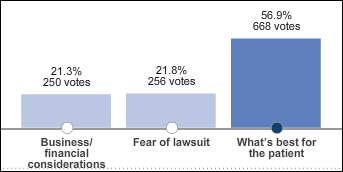
Yesterday, @ONC_HealthIT tweeted a recent Wall Street Journal Health Blog piece that asked readers what doctors use as the basis for care decisions: business or financial considerations, fear of lawsuits, or doing what is best for patients. I was gratified that with over 1100 votes, 56 percent of respondents believe we want to do right by patients. The other two options tied at 21 percent.
I’ve spent a good part of my career working in emergency departments and urgent care situations. I have to agree that fear of lawsuits can be an important driver. Financial considerations are also important, but there are many nuances other than what this survey can capture. Case in point: at one of the hospital-owned urgent care centers where I moonlight, the leadership issues a monthly report that looks at our utilization. On the surface, this aims to encourage us to provide more cognitive medicine and perform less defensive medicine.
Although thoughtful practice is a nice goal, I’d be kidding myself if I thought the report was aimed at encouraging us to use our brains rather than tests. The fact of the matter is that our population is largely uninsured, with Medicaid and Medicare closely behind. The hospital has been hemorrhaging money for the last decade despite extremely good management. It’s largely due to payer mix and other external economic factors in the community. Across our department, the Family Medicine physicians have much lower service utilization than do the Emergency Medicine physicians, and I think it’s partly due to the way we see the patient population
As a family doc, I’m used to seeing patients quickly in the office, treating their self-limited problems, and moving on. There’s a relationship between the patient and the physician. We tend to think that if the patient is becoming worse or not improving, they’ll be back. We don’t feel that pressure to try to cover all eventualities while they are in front of us, although it’s become that way with the advent of the Patient-Centered Medical Home, Accountable Care, and other initiatives where every visit has become a preventive/full-service visit as we try to cram as much as humanly possible into each encounter.
I really try not to order tests if I can make the diagnosis based on clinical history and physical examination. Not just for cost reasons, but also because tests are not without risk. Even a simple urinalysis can give false positives that lead to unnecessary follow-up, including not only financial cost but the burden of patient anxiety.
I’m also not afraid to play the bad guy with patients when it’s indicated. I don’t care if your husband’s primary doc gave him antibiotics for his viral illness. Just because you came to the urgent care and have the same symptoms, you’re not going to get them from me. I don’t care if your copay was $50, it’s not the right thing to do. It’s likely you’ll mark me down on your patient satisfaction survey, but I’ve reached a point in my career where I simply care less about satisfaction scores than I do about quality care and antibiotic resistance. You’ll get my empathy, sympathy, and some symptomatic treatment, but no Z-pack for you.
My peers that trained in emergency residency programs tend to order more X-rays for vehicular trauma even if the clinical story isn’t that impressive. Maybe it’s fear of being sued or maybe it’s just the way they’ve been habituated from working in higher acuity and trauma centers rather than the ambulatory office. Maybe because there was that one case where they missed something and it came back at them later. It’s definitely harder to try to help a patient understand why decision support rules say it’s OK to not order an x-ray than it is to just shoot a film, and sometimes I order those films too. None of us is perfect and medicine still has some art to go along with the science.
The most interesting thing about the utilization reports, though, is that over the last year, they have done very little to drive any of physicians at the high end of the test ordering spectrum into a lower bracket. Right now, the only “incentive” provided is seeing your name on the report and where you fall against your peers. Some docs may consider these reports the way I see the physician satisfaction numbers – as something that’s not on the top of their list for the many things we have to worry about when we’re seeing patients. Others may need education or potentially something more tangible before their behavior will change.
The bottom line, though, is that defensive medicine is alive and well regardless of steps towards tort reform, provider education, and other interventions. I’ve been doing some thinking about the other 21 percent as well. I’d liked to have seen the “financial considerations” choice expanded to include other options but you’ll have to tune in to the next post for those thoughts.
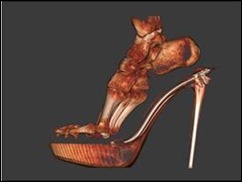
I’ll still throw in the occasionally newsy tidbit especially if it involves both shoes and technology. A new CT scan technology by CurveBeam called pedCAT shows what the foot and ankle actually look like when weight bearing. I was fascinated by the YouTube clip from the Royal National Orthopaedic Hospital. Since I was hobbling around this afternoon due to a loose heel on my favorite pair of pointy-toed mules, it’s a sure bet that my scan would have more than one ICD-10 code associated with it. I’m leaning toward “Unspecified soft tissue disorder related to use, overuse and pressure” and “Grief reaction” since I ultimately had to pronounce said mules dead at 6:59 p.m.
Contacts
Mr. H, Dr. Jayne, Dr. Gregg, Lt. Dan, Dr. Travis
More news: HIStalk Practice, HIStalk Connect















With regard to Citrix and Web:
HIS Junkie, if you think for one second pure web is immune from failure, you’ve got another thing coming. Talk about a vector for unexpected malware and unstable changes coming through browser updates.
Citrix helps cure a MAJOR problem with Windows and creates a way more reliable environment than even pure web servers. It way more reliable than browser based systems at this point.
The vulnerabilities on web servers will be memorialized in song and poems of the next generation. It’s the stuff of lore.
Get off your bandwagon and on with life. Sutter hit a problem with Citrix Provisioning Services and they had rational backups in place that actually were used despite the false press the California Nurses Union put out. Could they have prevented it with better load testing or something – who knows.
Anyways, any dummy knows that:
Windows thick clients have problems.
Citrix has problems.
Web servers (all makes, models and versions) have problems.
Vendors have problems.
Servers have problems.
Data centers have problems.
Network providers have problems (and back-hoes to deal with).
Power companies have problems.
Sutter’s events were unfortunate, but not unprecedented.
When it happens on your watch, I’m sure you’ll find a way to excuse it. When it happens on someone else’s watch, it’s sort of sporting to try to create a competitive differentiation over it.
Let them learn from it and move on.
It’s a good thing football season is starting next weekend so all the armchair quarterbacks can get back to what they do best.
Responder – if there were a giant LIKE button – I would LIKE your response 100x over.
Right on point – but ultimately that is what this blog is about – rumors and hypocritical judgements. Goes along with the rest of our society and “news” sources.
Re: sutter downtime
It was very disappointing to see the Califirnia Nurses Association’s media blitz regarding the sutter downtime. Many issues in the article raises quetions about their stance including;
* complaining that nurses need to bill correctly. All of us who work in healthcare from nurses, doctors, pt, IT, dietary have to figure out ways to provide quality care while running a hospital like a business. We can not continue on the path we have been on. As Mr. H mention- how can hospital pay the salaries nurese want if they do not bill for services.
*complaining that nurses have to use an EHR- As a patient or a potential employee, I can not envision going to an institution that did not have an EMR and nurse were not documenting real time. While they may not be perfect, at least the information is oonline where multiple clinicians and support people have access to the data and something is not missed becasue it is on a paper chart.
* I am curious how the union feels about patient engagement? The move towards patient engagement means that nurses need to be a prime member of the care and share documentation with the patient. You need an EHR and portal to do that.
i am so disappointed in the complete lack of trying to work with the industry to improvie healthcare instead of trying to hold it back by very misleading media reports.
The article indicates the Advocate Medical Group Breach involved stolen unencrypted desktop computers, not laptops. The big 2011 Sutter Breach (approximately 4.2 million patients impacted, resulting in billions of dollars of potential liability in class action suits) was also the result of a stolen unencrypted desktop computer.
I have worked with many Healthcare Systems across the country and while many/most are now encrypting laptop computers, not many are encrypting desktop computers due to the cost and effort involved and the fact that laptops are more likely to be stolen or lost than desktops.
If we have more big breaches caused by stolen unencrypted desktops, some may need to revisit their desktop encryption decisions. Having a policy that says don’t store EPHI on unencrypted devices may not be enough when CMS comes knocking.
#sutter
“We appreciate the hard work of our caregivers and support staff to follow our routine back-up processes, and we regret any inconvenience this may have caused patients.”
That is all well and good, but when my doctors face the blank computer screens and the nurses are sitting waiting for the back-up downtime process to activate, patients are not inconvenienced. Their therapies are delayed and some of them die or deteriorate because of the delays. Let’s call a spade a spade, and stop the euphemisms.
At one hospital, they can go 2 hours with blank screens before it is considered a downtime.
Responder, you make a lot of grandiose statements without any evidence to back them up (e.g., “It [sic] way more reliable than browser based systems at this point.”).
No doubt Citrix reduces the administrative burden on desktop IT support, but it does so by adding an extremely complex layer on top of it. Not too dissimilar to protecting your car like this: http://bit.ly/145Gs2g
I’m not opposed to using Citrix – it’s a godsend for supporting legacy products – but let’s try to stay balanced about the pros and cons of different technologies.
CNA has done some good work in the past but is now notoriously uncompromising and farcically anti-IT. Some of their literature is laughably ill-informed, reflecting antiquated thinking. This is ironic given that commercial EMRs were born in CA with RNs at El Camino Hospital a huge part of the success.
This is not to say RNs don’t have legitimate concerns with EMRs (as their largest user group) or that all HIT vendors respect RN’s role and critical thinking. But CNA needs to move into the 21st Century and get behind good technology that supports nurses, not continue to rail against EMRs which only makes them look out of touch and petty.
Thank you ‘Foaming’. I could not have said it better.
Another layer of complexity = more points of failure.
Responder – I did not say that web systems do not fail, only that another layer adds to the probability. If you had a choice of installing a syst with the layer or without the extra layer…which would you select?
Would Farzad talk out of both sides of his mouth??
Cute video, but If he believes so strongly in EBM then please explain this. In 2009 your boss Kathleen Sebelius issued a report from the U.S. Preventive Services Task Force, an outside independent panel of doctors and scientists, (which she created at the urging of the White House). Their report found that mammography screening of women under 50 years that do not have a family history of breast cancer was not only a waste of money but created false positives that were potentially dangerous to the patients, and therefore the screening s/b stopped. She ignored their recommendation and told the Komen foundation that the government would keep paying for screening for these women. Why? The evidence from five studies they reviewed was clear- but the politics over rode the science, that’s why.
Get real Dr. – if our own government tells us one thing then turns around and does the complete opposite when lobbyists lean on them…how can you expect the front line care giver to sign on to you mantra?? You should call it EBPM, evidence based political medicine.
See: http://articles.washingtonpost.com/2009-11-20/opinions/36770211_1_mammograms-task-force-male-dominated-medical-establishment
So, just to be clear, web servers are comparable to Citrix servers.
Web servers are routinely hacked at banks, federal agencies and businesses.
How many reports of Citix farms being hacked?
Web servers are tons more complex and fragile.
Server -> web server -> client
Server -> Citrix server -> client
It’s all the same architecturally. But web servers are way more difficult to manage and they do also go down or suffer if they lose contact with a provisioning service it ldap server for example.
Dr Jayne, sorry to hear the mules died…,maybe time for an end of summer hand painted interlude with Roberto Cavalli…and another ICD10 code or two.
http://www.luisaviaroma.com/index.aspx?gclid=CKWn-pXJqLkCFSVgMgodJEcALg#ItemSrv.ashx|SeasonId=58I&CollectionId=918&ItemId=1&SeasonMemoCode=actual&GenderMemoCode=women&CategoryId=&SubLineId=shoes
FYI, a citrix implimentation is just another layer over a web server. Enterprise Web servers are quite easy to administer – the challenge is when your ‘web application’ requires client side executables and applets to function, which means it is not truly a web app.
Server -> web server -> client
Server -> web server -> Citrix server -> client
@Cdff: love the handpainted shoes, although 110mm is probably more than I can stand (pun intended!)