TBF the anti-hate non profit was funding undercover investigators trying to being down the KKK & has done successfully for…
Readers Write: Fund Healthcare Modernization and Innovation – Retire Legacy Applications
Fund Healthcare Modernization and Innovation – Retire Legacy Applications
By Julie Lockner
The American Recovery and Reinvestment Act of 2009 (ARRA) provided the healthcare industry incentives for the adoption and modernization of point-of-care computing solutions including electronic medical and health records (EMRs/EHRs). Now that these funds have been allocated and invested in new information systems, hospital and patient care provider CFOs are checking in on the return on those investments. Many are coming up short.
These mega EMR/EHR applications are taking longer than planned to implement leaving a number of legacy applications running in parallel. In addition to hardware and software maintenance costs for both environments, costly resources with skills to maintain aging technology platforms drain IT budgets – funds needed to support new systems.
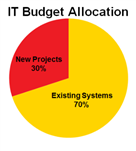
This challenge is not unique to the healthcare industry. A recent survey [1] of companies with over 50 IT staff shows that on average, 70 percent of the IT budget is spent on existing systems. If half of the applications are redundant, this represents a major opportunity for cost savings or reinvestment.
Why are so many legacy systems still running? An industry research report [2] indicates the #1 reason is that users still want to access data. As creatures of habit, many hospital staff continue to use familiar systems to look up patient information and records out of convenience. Unfortunately, this comes at a cost.
Another reason is because entire legacy data sets are not always migrated to new systems. Data with assigned records retention schedules require collaboration between stakeholders and compliance teams. Without a programmatic approach, application retirement projects can be significantly hampered.
Many providers have overcome these hurdles and successfully implemented an application retirement strategy while migrating to a new system saving millions.
For example, the nation’s largest children’s hospital expects to save $1.8 million annually from retiring legacy applications. Their IT modernization program replaced applications running on aging platforms such as HP Turbo Image, SQL Server, Oracle, and MUMPS with an EPIC implementation. Patient clinical data needed to be retained for compliance reasons, so they deployed an application retirement strategy that allowed them to keep that data and eliminate dependencies on legacy systems and applications. Hospital staff was given online, convenient access to data in a secure archive and compliance teams could track retention.
Key to success, they claim, includes a platform with the following capabilities:
- Archive support for a variety of data types, systems and platforms
- Automated validation to confirm data had been completely and correctly archived
- Ability to assign retention policies during or after the archive process
- Automate data purge workflow when retention periods expires with legal hold support
- Mask sensitive data in case a clinical trial is reopened
[1] NCC survey companies with over 50 IT staff
[2] Enterprise Strategy Group Research Report, Application Retirement Trends, October, 2011
Julie Lockner is vice president of product marketing for Informatica.



Thank you for writing this article. I can’t tell you how many times I have tried to explain to healthcare provider organizations the importance of developing and enforcing (with modifications over time, if needed) a strategy for decommissioning systems as part of an Information Governance plan. From a data / records management perspective, even when a new system is acquired, a retention schedule for the new system’s data should be developed and enforced. In your article, you emphasized the cost benefits achieved from decommissioning systems, As a HIM professional, who should be part of this team, I emphasize the legal and compliance benefits — whereby just one court case or regulatory audit without such a strategy can cost millions. I’ve seen it!
Unfortunately this article skims the surface of the challenge of managing legacy applications. Ms. Lockner has missed an educational opportunity regarding CFO’s “checking in on the return…”. We should not simply accept that it is “OK” to look for financial benefits a year after implementing an EMR: it is not unusual for IT investments—particularly EMR functionality—to require a 6-7 year period to see a financial return, and even then only with complementary management and workflow changes (David Bates et al had a great article on this some years ago). As a former CIO, I can say that a 70/30 split between existing and new projects makes a lot of sense—you can’t overwhelm an organization by constantly introducing new projects. Not sure any CFO would applaud the $1.8M annual savings when compared to the likely $100M cost of a implementing a new EMR environment. Also, labeling SQL Server and Oracle as “aging platforms” seems a stretch. These platforms are constantly evolving, and actually support many of the capabilities that Ms. Lockner cites as “key to success”. Interestingly, the ESG Research Report that Ms. Lockner cites apparently didn’t note the special challenges of the health care industry, in which the data retention requirements are real and often based in legislation and government rules (she also didn’t mention that she was a co-author of the report, and that it is only available for $3500!). The main point is that getting rid of “legacy” applications is neither straightforward nor as easily accomplished as Ms. Lockner seems to suggest.
Am I the only one that’s confused by this?
“For example, the nation’s largest children’s hospital expects to save $1.8 million annually from retiring legacy applications. Their IT modernization program replaced applications running on aging platforms such as HP Turbo Image, SQL Server, Oracle, and MUMPS with an EPIC implementation.”
Replace MUMPS with EPIC?
Um, doesn’t EPIC run on MUMPS?
Lynn Vogel and JustAClinician raise important points.
However, I maintain that relatively few healthcare provider organizations recognize the importance of developing strategies for decommissioning systems and include them as part of their Information Governance plans. Without, the legal and compliance risks can be significant.
Great article! Thanks for sharing.
Great comments – in an article that only scratches the surface on the benefits of implementing an application retirement strategy, there is definitely more detail to every story. In this use case, the versions of Mumps, Oracle and SQL Server deployed in these legacy environments were older versions no longer supported and the applications running on top of those databases didn’t run on the latest, supported versions. Yes, EPIC is implemented on top of a version of MUMPS – but that doesn’t mean that older legacy systems run on or support the latest versions of databases. These older versions of databases only support older versions of operations systems and hardware. Anyone in the IT industry for any length of time recognizes the challenges this poses from a support perspective. The risk of not being able to access or run a report because an aging system stopped working and you can’t find a consultant who even remembers how to run the application poses incredible risks. And – given that healthcare applications are commonly run on proprietary platforms, data portability is a bigger challenge.
This ROI I touched on showed that by implementing an archiving solution for a department that moved regulated data to an application and technology independent platform, they could eliminate costs of about $1.8M immediately and annually (which is roughly $12.6M or $1.8M X 7 years to implement an EHR, or 12.6% the cost of implementing a large EHR – using a comment previously pointed out) while maintaining legal compliance and access to data that multiple stakeholders required. Now that may be a drop in the bucket compared to what this hospital is investing in a new EPIC implementation, but given that this was just for one department, think of the potential impact it could have rolling out these best practices and use those savings to fund the rest of the EPIC implementation that fell out of scope. This point is worth the debate – thank you for your comments and I am happy to share more about how others are saving $10M annually in other industries. I would rather this money go back into giving hospitals funds that they could reinvest in innovation that can save lives – what would you do with $10M?
A great article on a topic that hasn’t received meaningful coverage in recent years. I recently helped a health system client discover that almost 25% of their existing applications “in operation” (350+) could be effectively decommissioned right away. They are not alone; too many IT shops carry unnecessary cost, complexity, and liability because this isn’t a high enough priority.
CIOs: Start decommissioning that old application of yours the same day you do the project kickoff for that shiny new one!