It's really hard to take seriously these studies targeting "misinformation." Clearly there's some bad stuff out there, like people claiming…
Readers Write 6/25/12
Note: the views and opinions expressed are those of the authors personally and are not necessarily representative of their current or former employers.
HIE Success: Think Google, Not Government
By Orlando Portale
In March 2010, Governor Schwarzenegger named CaleConnect as the new entity that would deploy funds from the Obama economic stimulus package to build out a statewide health information exchange. As was reported recently, the effort has been transitioned to UC Davis.
Make no mistake, this was never going to be an easy task. There are lessons learned for all of us as we plan for our own public or private HIE initiatives.
Shortly after the formation of CaleConnect, I visited with members of the board, including Jonah Frohlich, the Terminator’s right-hand man on HIT. As I indicated to the CaleConnect board back in 2010, “This could turn out to be just another Keynesian economic experiment where money is spent, but nothing tangible is ever delivered.”
Prior to the meeting, I distributed a white paper (click the link to download) to the board outlining specific strategies and potential pitfalls to avoid. Here is its introductory section:
The business sustainability strategies adopted by the California eConnect (CeC) organization are likely to be the same ones employed by other technology startup companies. Success for any startup venture is largely determined by the organization’s ability to rapidly deliver compelling solutions with clear customer value propositions. These solutions must not only meet the functional requirements of the targeted customer segment, but be efficiently delivered and effectively supported. Startup companies that succeed in capturing a given market with compelling solutions are generally rewarded with increased profits and sustained customer loyalty. The path for the successful launch for CeC will be conditional on having the right organizational framework in place, sound business strategies, an understanding of current and future customer requirements, solid solution planning capabilities, financial management expertise, and superior execution. This paper will outline high-level strategies for CeC to consider with regard to achieving a sustainable and successful organization.
When I visited with the board, I stressed the following key points:
- Make sure you clearly define roles and responsibilities of the board of directors versus the CaleConnect executive team. The board should not attempt to micro-manage the effort, rather provide high-level oversight. Leave day-to-day decision-making to the organization’s CEO.
- Don’t line up a burdensome schedule of periodic meetings. A solid, well-understood governance structure will avoid needless conflict later.
- Run the organization like a Silicon Valley startup, not like a branch of state government. Set up shop in Palo Alto, not Sacramento. Think Google, not government. Embrace speed to market, agility, pivoting … everything you would do in a startup company.
- Build out the beta version of the product ASAP. Get some early adopters to test it out ASAP. Iterate on it like crazy. Enlist the beta testers to evangelize your product.
- You are building a product. Treat it like a startup product’s design, build, and delivery effort.
- Your #1 priority should be on the product. Avoid the usual pitfalls of constituent outreach and conference speeches about what might be possible if California had a wired healthcare system. Don’t hype up your stuff until you can demo something.
- When you do get it built, market the heck out of it.
- Don’t waste your time running around the state talking about what might be possible in advance of the product release. Everyone has been pitched endless times about the potential value proposition for health information exchange.
- Everyone will be skeptical, and rightfully so. They have heard it all before. Until you can demonstrate something real, you will have zero credibility.
Unfortunately, as the project unfolded, many of the pitfalls I had warned about were realized.
I continue to believe that a highly agile approach to HIE planning and deployment is greatly beneficial. Remember, think Google, not government.
Orlando Portale is chief innovation officer with a large healthcare organization in Southern California.
Why Windows 8 Might Be the Next Big Thing for Healthcare
By Anthony Hooper
We’ve been following Windows 8 since the developer beta was released at build/windows and it really excites us. Why? Microsoft has a ton of device driver support for Windows XP, Vista, and 7, and most of these drivers will work with Windows 8.
Clinicians want mobility in their day-to-day jobs and they want a device they can carry with them, but one that will also augment and make their day more efficient by allowing them to enter information on the go. Consuming data isn’t the only reason for a tablet any more.
Windows 8 brings a ton of medical device driver support to the table, powerful computing hardware, and a great touch-enabled interface. Finally, a mobile OS that allows health professionals to run their current Windows-based EHR and charting applications, and augment them with metro touch-enabled workflows.
With Windows 8, a clinician can have a single mobile tablet that can be carried during rounds and can be used for taking blood pressure readings without cumbersome dongles. Then, clinicians can return to their desk, switch into desktop mode, and complete many of the tasks they started in the mobile-optimized application.
Unlike iOS, Windows 8 will have a wide variety of hardware manufacturers. This means each hospital or clinic administrator can select the hardware profiles that meet their team’s needs. And it opens the possibility for biometrics hardware and HDP-enabled Bluetooth chipsets.
Anthony Hooper is development manager at Macadamian of Gatineau, Quebec.
Use the ICD-10 Deadline Delay to Maximum Advantage
By Deepak Sadagopan
Just as healthcare providers were getting serious about progressing toward the much-heralded ICD-10 era, the announcement of a potential deferral in the compliance deadline has spawned a new wave of delays and second guessing about how best to apply limited IT resources. Some organizations are freezing ICD-10 budgets and slowing down, or even halting work completely, until a new date is set. While a one-year deadline delay may be productive, it would be a mistake to assume that planning can be halted until this time next year and then resumed – primarily because most organizations are already far behind the curve in preparing for ICD-10.
Any delay or reallocating of internal resources in an environment where healthcare provider budgets are already tight can result in process inefficiencies and, ultimately, higher implementation costs. Many are concerned with how to make the extension beneficial to their organization. Providers should use the additional time to implement a more sound and strategic approach to collaborative testing with their primary trading partners – the most difficult and unpredictable segment of conducting a successful ICD-9 to ICD-10 migration. As it is, most large IT projects typically require more testing time than is usually allocated – and the current status of ICD-10 readiness demonstrates this case is no different. In fact, given that ICD-10 can have a tangible impact on revenue flows, providers should ensure that they work hard to mitigate their risk of disruption with trading partners that account for 80 percent or more of their revenue. Such systematic testing initiatives with key trading partners are essential for achieving the goal of financial neutrality.
Across the industry, we can look at the progress health plans have made to set the future for providers. This newly found year of extra time will be a critical period for internal and external testing. Collaborative testing should focus on maintaining the operational status quo. This means keeping the business neutral with respect to key performance indicators such as claims acceptance rates, support inquiries, electronic claim adjudication rates and aggregate claim reimbursement amounts. Many ICD-10 codes will result in an increase in clinical complexity and document specificity as compared to ICD-9. Through collaborative testing with health plans, both parties will be assured that migrating claims to ICD-10 will allow benefit and payment neutrality.
To test effectively, providers and their trading partners must develop scenarios that reflect use of high-risk codes, specifically claims that use codes expected to have high volumes, complexity, and high dollar values. The key is to minimize the risk to the business by focusing efforts on testing scenarios that could have the most impact.
Successful external testing requires new levels of collaboration and information sharing among providers and insurers. While it may be uncomfortable to collaborate on such testing, failure to do so may lead to big surprises in payments after the transition date, which will cause even greater discomfort for insurance companies and providers alike.
The ICD-10 transition is the most substantial effort the industry has faced. The scale of the project means that the testing required to fully ensure business readiness, as well as benefit and financial neutrality, is unprecedented. For those organizations that have the determination to keep moving forward as if the delay had never been announced, it will undoubtedly end up being a true gift on the testing front. Take advantage of the time afforded to realize a true benefit from the delay. And devote any newfound hours to ensuring that neutrality is achieved.
Deepak Sadagopan is general manager of clinical solutions and provider sector at Edifecs of Bellevue, WA.
Payback is a CPOE
By Daniela Mahoney

Right from the beginning of a project, I elicit the customer’s motivation for deciding to invest in CPOE. For meeting Meaningful Use requirements only? Or for what I like to hear, which is things such as “an organizational initiative for quality improvement,” or “to reach the highest level of patient safety goals” or even, in some cases, “cost reduction and avoidance.”
But if only about the money, we need to understand that the return on investment for a CPOE project — outside of incentive dollars — is difficult to calculate. Baseline costs of essential processes are hard to define, and often a number of benefits do not lend themselves to a quantifiable measurement process (i.e., improved communication across departments). Additionally, many organizations have difficulties measuring their medication errors and adverse drug events.
Although measurable improvement may be detected in well-defined areas, such as the use of expensive diagnostic and therapeutic procedures and compliance with core measures, CPOE should be viewed as an indispensable supportive technology and should be included in the overall quality improvement strategies of the organization.
And just how much will it cost an organization to implement CPOE?
For starters, we know CPOE is 80-85% clinical transformation, rather than tangible software, hardware, or infrastructure. Costs are more about people and processes than implementing technology. There are a few good studies published in the past few years that discuss the financial impacts of CPOE from a cost to ROI perspective.
One well-known study was initiated by the Massachusetts Technology Collaborative (MTC) and the New England Healthcare Institute (NEHI). The study was led by Dr. Bates and his team of physicians and nurses, who audited 4,200 medical charts from community hospitals in Massachusetts over a 12- to 18-month period. Once Dr. Bates’ team completed its work, PricewaterhouseCoopers did a complete financial analysis of the costs associated with each error identified and, if an error had been prevented, to whom the savings would have accrued.
Based on this study, most hospitals that have considered purchasing and implementing CPOE can expect a return on their investment within 26 months, a quick payback. The acquisition cost for a CPOE system was cited as being about $2.1 million, and hospitals could expect annual operating expenses of about $450,000 a year. After breaking even on the initial investment, hospitals with 70% use ratings for CPOE can expect a net savings of about $2.7 million per year.
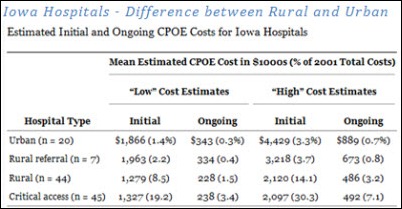
Examples of cost:
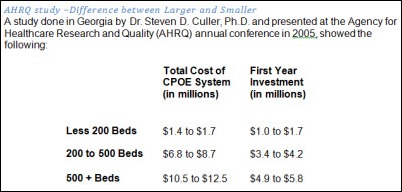
In the example above, averages are from $7,000 to as high as $17,000 per bed as a total cost of implementation. Also, I looked back at the data I have accumulated over the 20+ years to compare the costs for hospitals I’ve worked in and some of the published case studies. Looking at the cost of the implementation per bed, there does not seem to be a significant difference between the larger facilities and smaller ones.
Looking at a range of lows and highs, I am seeing costs varying from $7,550 to $12,000 per bed, depending on how costs were estimated based on the initial project assumptions. In the latter case where the cost per bed is higher, we have accounted for other items as part of the initial capital investment; things such as servers, devices, end-user support staff, and training hours for staff and the entire implementation team members.
CPOE is not an inexpensive endeavor, to say the least. But in the end, it’s cost vs. effectiveness
Organizations will spend a great deal of their initial investment regardless of whether they implement the minimum requirements to meet Meaningful Use or implement to improve quality care delivery for the entire organization. However, one thing is certain: benefits cannot be anticipated if only a handful of providers are using the system and we constantly have to come up with workarounds to bridge the gaps. There are so many benefits to CPOE and real-time clinical decision support.
So I ask the question: what is more important to your organization, cost or effectiveness? This is a critical question to understand and answer to seek because it will help you fully recognize the value of medical technology and the likelihood of adoption by your organization.
We talked about money and the “richness” of CPOE. Why not take this a step further and complement our topic with a nice summer dessert? Extra-rich strawberry ice cream. I guarantee it you will enjoy it, and it will cleanse your palate from the bitter taste this topic leaves behind.
Daniela Mahoney, RN BSN is vice president of Beacon Partners of Weymouth, MA.



Orlando,
One big problemo, they are government, not Google. You can’t be something you’re not.
Although your advise was best intentioned, your premise was flawed.
Big gov is…big gov. It can’t be all the things you suggested.
I agree with Anthony re: “Consuming data isn’t the only reason for a tablet any more.” W8 will be good for further adoption of tablets in healthcare. It is more practical for enterprises, integration and capturing data. Applications can be optimized for touch, pen and voice; but you can also run your legacy applications (assuming they don’t require something nasty like IE6/7). Make W8 (and iPad0 part of your mobile strategy.
The first article speaks very effectively about the importance of clearly defined ROI in an initiative. Let’s extrapolate that to an EMR installation initiative which can be viewed in much the same lense.
The only mention of an ROI in CPOE is “effectiveness.” Yet, the landmark studies on whether CPOE is “effective,” which have come from the US and the UK, show zero correlation between CPOE and better outcomes. In fact, the show greater correlation with negative outcomes. Ad hoc commentary from doctors in the trenches swings either way. Some pro, some con. Alert fatigue, less objective analysis due to a greater inclination to think along the lines of a pre-programmed template than outside the box, orders and thoughts forgotten by the end of the day when the doctor returns to complete encounter, and simple confusion. As one doctor on a very well-known system said, “It’s like driving a car that only turns left.” His neighboring physician on the same system went from 30 patients per day and leaving at 4:30 in the afternoon to 26 patients per day and leaving at 6 PM…. 2 YEARS AFTER THE INSTALL!!!
Folks, sooner or later we’re going to have to get real about expecting systems that deliver a solid, consistent, and measureable ROI – whether it’s dollars or some compelling and measurable improvement to quality…. Or, we’re just living in a government created bubble of “HealthIT”