"A valid concern..." Oh please. Everyone picks the software they like and the origin of that software is an afterthought.…
News 6/20/12
Top News
CMS says that as of the end of May, more than 110,000 EPs and over 2,400 hospitals had been paid a combined $5.7 billion in EHR incentives from Medicare and Medicaid. That’s about 48% of all eligible hospitals and 20% of eligible Medicare and Medicaid providers.
Reader Comments
From Jenny: “Re: Catholic Health Initiatives. The group is installing Cerner, but the Tacoma-based Franciscan group received permission to install Epic in five hospitals and will go live in April 2013.” Verified.
From Pillsbury DB: “Re: Lahey Clinic. They were installing Allscripts in the ambulatory environment and had a best-of-breed approach using Orion for the inpatient setting. I’ve attached an old case study. Instead of implementing a true EHR product, they decided to pull data using Orion into a clinical data repository. Paper-based data was scanned and indexed into PDFs which were also available using Orion portal. This worked for clinician viewing, but made it impossible to implement CPOE. They were also scanning millions of records per year requiring many FTEs to perform the function. When HITECH hit, they had no hope of meeting any stage of MU. To compound the problem, the Allscripts implementation was about a year behind and way over budget.” Above is an extract from the Orion Health case study from last year. I guess MU did reduce the interest in EMRs based on scanned documents quite a bit.
From The PACS Designer: “Re: Microsoft’s Surface tablet. The new challenge to the iPad has arrived in the form of a tablet PC called Surface. One unique aspect of the Microsoft Surface is the keyboard in cover of the tablet. While it won’t really be any threat to the iPad, it may draw interest from PC users who are more comfortable with a traditional keyboard versus an on screen keyboard.” Microsoft has been short on innovation lately (decades), but I don’t get why they used the Surface name on a tablet when it’s already being used by their coffee table gesture thingy. And unlike Apple, Microsoft is selling futures once again since nothing’s ready to ship. They won’t get bold on the pricing because they won’t want to diminish the already iffy prospects of the Ultrabook laptops, so you’ll be able to buy a me-too tablet running probably buggy software for double the price of iPad right as businesses give in and let people bring in their own at zero expense to the enterprise. Apple started failing dismally after firing Steve Jobs and returned to prominence only after they hired him back, but Microsoft’s problem is that Bill Gates isn’t coming back.
HIStalk Announcements and Requests
I’m doing some traveling for the hospital over the next few days (to a vendor location home to a great many HIStalk readers, in fact), so given the difficulty in achieving my usual prodigious output given limited time and connectivity, Inga is handling the brunt of the HIStalk chores. I’ll chime in with whatever is interesting to me as I have time. If you’ve tried to get in touch with me, hang in there until the weekend when I can get caught up.
Acquisitions, Funding, Business, and Stock
Shareable Ink secures $5 million in series B financing from Lemhi Ventures. As part of the deal, Lemhi Ventures’ managing partner Tony Miller will assume the role of chairman of the board.
ESO Solutions, a provider of EMR software for the EMS and fire services industries, raises $4 million from Austin Ventures.
North Bridge Growth Equity invests $30 million for a minority interest in Valence Health.
Sales
Missouri Health Connection and the NY eHealth Collaborative select the InterSystems HealthShare platform for their health information networks.
St. Luke’s Hospital (IA) chooses Amcom Software for smartphone communications and Web-based on-call scheduling.
WakeMed Health & Hospitals (NC) contracts with MobileIron to provide mobile device security and enable the organization’s BYOD program.
The Newfoundland and Labrador Centre for Health Information sign agreements with Telus Communications and Orion Health to provide technology for a province-wide integrated EHR.
Allscripts Enterprise EHR customer Summit Medical Group (NJ) signs a long-term contract for Allscripts Managed Services.
People
Bulletin News names Nick Tabbal (Resonate Networks) VP of analytics for its Bulletin Healthcare subsidiary.
PerfectServe hires Robin Borg (Optum) as VP of human capital.
Beacon Partners names Fernando Martinez PhD as national director for enterprise assurance services. He was previously with Jackson Health System (FL).
MyHealthDIRECT adds HealthWays VP and COO Tom Cox and SSB Solutions chairman Jacque Sokolov, MD to its board of directors.
Announcements and Implementations
Geisinger Health System and Merck announce a multi-year collaboration to develop solutions that facilitate shared decision-making between patients and physicians and improve patient adherence, engagement, and care delivery.
Corniche Hospital becomes Cerner’s first client in the United Arab Emirates to achieve full closed-loop medication administration. Meanwhile, Royal Berkshire NHS Foundation Trust goes live this week on Cerner Millennium after a three-month delay.
Government and Politics
The HIT Policy Committee’s Quality Measurement Workgroup and the HIT Standards Committee’s Clinical Quality Workgroup ask for input on ways in which Stage 3 MU may advance the delivery of high-quality care in diverse care settings.
The White House recognizes 82 providers for their successful implementation of EHR at a Health IT Town Hall in Washington, DC.
HHS awards $772 million to 81 providers, tech firms, and local organizations to advance healthcare innovations that lower costs and improve quality.
VA officials tell lawmakers at a House Veteran Affairs Committee hearing that it has processed fewer than 800 benefit claims despite investing $491 million in new technology. The current backlog is 913,690, which includes 575,773 claims older than 125 days. The VA originally promised a system-wide rollout of its Veterans Benefits Management System this year, but performance issues have pushed full implementation until the end of 2013.
The Military Health System issues an RFI for a system to track lab work within its integrated EHR.
Joe Goedert writes a Health Data Management article describes pending federal legislation that could be the first steps toward regulation of healthcare IT.
Other
The US Supreme Court refuses to consider an appeal by former McKesson Chairman Charles McCall to overturn his 10-year prison sentence for scheming to inflate company revenue.
Lehigh Valley Health Network , Cedars-Sinai Health System, Kaiser Permanente, Palmetto Health, and HCA make the top 25 in Computerworld’s list of 100 Best Places to Work in IT 2012.
The local paper highlights Greenwich Hospital’s (CT) recent $30 million implementation of Epic, which replaces Meditech and will eventually connect with other Yale New Haven Health System facilities.
UnitedHealthcare tops AMA’s fifth annual National Health Insurer Report Card, which considers the insurance billing and payment accuracy of seven of the largest commercial health insurers. Error rates on paid medical claims dropped from 19.3% in 2011 to 9.5% in 2012, saving health systems $8 billion in unnecessary administrative work to reconcile errors.
New from Ross Martin MD: The Money Machine, which he says appropriately describes your financial hamster wheel, whether it’s the usual problems or EHR adoption or whatever.
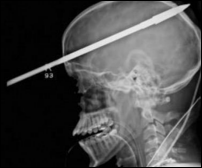
Weird News Andy admires the dry analysis of a doctor describing a 16-year-old accidentally shot through the head with a three-foot-long stainless steel fishing spear: “It’s a striking injury, something you don’t see every day … the first obstacle is to not be distracted by the obvious sensational aspect of the injury.” The spear missed most everything important in the boy’s head, doctors removed it, and he’s expected to make a near-full recovery.
WNA also finds this story interesting. A man told by a hospital that his cancer left him with just months to live, along with his wife, rack up $80,000 in debt to complete a hastily compiled bucket list, giving away $30,000 worth of goods, selling their house at a loss, cancelling their health insurance, and traveling the world. The man even takes up smoking again, figuring he has nothing to lose. He then waits to meet his maker, vowing to kill himself if the pain became unbearable even as he questions why he seems so healthy. Finally his hospice worker told them the hospital had made a mistake but didn’t tell him – he’s fine.
Sponsor Updates
- Greenway pilots integration between its PrimeSUITE EHR/PM product and Microsoft HealthVault.
- ICA Informatics exchanges direct messages and trust agents with Cerner, Max MD, Mirth, NitorGroup and Techsant Technologies at the ONC Direct Summit.
- Capsule says that within the last six months it has added or updated more than 70 devices to its device integration list.
- Johns Hopkins’ director of enterprise services discusses his hospital network’s use of Imprivata’s SSO technology.
- The NY eHealth Collaborative announces that Stephen J. Dubner and Dr. David J. Brailer will be keynote speakers at its October Digital Health Conference in NYC.
- Emdeon hosts educational presentations on cost containment challenges at this week’s America’s Health Insurance Plans Institute conference in Salt Lake City.
- Picis announces a strategic partnership with billing and PM provider Anesthesia Business Consultants.
- All Imaging Systems partners with UltraLinq Healthcare to provide cloud-based storage services to UltraLinq clients.
- Medicomp and technology partner Northrop Grumman announced Northrop’s Clinician App integrated with Medicomp’s MEDCIN engine at last week’s Government HIT conference in DC.
- The 400-physician Rees-Stealy Medical Group (CA) lowered transcription costs $800-900,000 annually (80-90%) within 10 months of adopted Nuance’s Dragon Medical voice recognition software.
Contacts
Mr. H, Inga, Dr. Jayne, Dr. Gregg.
More news: HIStalk Practice, HIStalk Mobile.






>>> CMS says that as of the end of May, more than 110,000 EPs and over 2,400 hospitals had been paid a combined $5.7 billion in EHR incentives from Medicare and Medicaid. That’s about 48% of all eligible hospitals and 20% of eligible Medicare and Medicaid providers.
This data is iwrong… let me review the actual numbers, published by CMS here: https://www.cms.gov/Regulations-and-Guidance/Legislation/EHRIncentivePrograms/downloads/Monthly_Payment_Registration_Report_Updated.pdf , updated monthly.
There are 2 groups of “providers” included in those that have been paid. There are 49,051 that are in the “Medicaid Eligible Professional” group. I usually refer these as the major crazy ones- these are physicians that willing to accept Medicaid patients ad nauseum, even though the payments for this group of patients barely covers overhead, and on top of this they are willing to get into a MU situation where they will lose massive amounts of money on technology, per license, per year, indefinitely. These doctors should not be discussed in any “meaningful way.”
That leaves the 123,921 that have been paid under the “Medicare Eligible Professional” group which also lose money treating the low-paid, more complicated Medicare patients. Of these, 77% are physicians. Another bit of important data is that there are about 624000 physicians in actual clinical practice as per the AHRQ – http://www.ahrq.gov/research/pcwork1.htm . There are 952000 physicians in the USA, as per the article “Medical Schools Can’t Keep Up,” WSJ, 4/12/2012.
If you do the math:
1. 123,921 x 0.77 = 95,419 physicians that have been paid.
2. 95419/624000 x 100 = 15% of all physician clinicians have been paid.
3. 95419/952000 x 100 = 10% of all physicians have been paid to date.
The 10% number is at par to what the CDC have found in their annual updates (historically 9-10% not only have an EHR but are using it in a meaningful manner).
What they also don’t tell you is that this is:
1. Many physician clinicians have closed down their office practices to be employed due to MU, lowering the number of active physician clinicians available for MU, which will increase the percent of physicians that have been paid, but unfortunately in a deleterious manner. This was mentioned in the following article: “Why Are Primary Docs Thinking About Leaving Medicine?” (http://thehealthcareblog.com/blog/2012/03/22/why-are-primary-docs-thinking-about-leaving-medicine/ )
2. This is really as good as it’s going to get- when we get to phase II of MU with the even more onerous demands physicians will drop out so the participation will likewise decline.
3. The future of HIT is not what we have today. Smart physicians will hold off buying into an EHR, allowing for costs to come down, interfaces to improve, and productivity as well as usability to increase. There has recently been a big debate on this after the NEJM recently came up with 2 editorials, one of which was titled: “Escaping the EHR Trap—the Future of Health IT.” They can be downloaded from here: https://www.box.com/s/f523651ebb227da7158b
4. The citation that “The EHR Incentive Programs have really helped jump-start the use of electronic health records by health care providers all across the country.” (Dr. Mostashari) is only correct in that physicians are using basic EMRs more and are partially using EHR systems. Unfortunately, the MU program is in trouble and is a house of cards waiting to collapse. It’s a waste of taxpayer money and I’m not really sure that this growth in EMR was really jump started by any MU big government bureaucracy when only 10% of doctors have taken part and been paid for the easiest portion of these mandates.
Dr. Borges’s seemingly mean-spirited dismissal of doctors who choose to treat Medicaid patients (“major crazy ones” and “These doctors should not be discussed in any “meaningful way””) makes it hard for me to take any of the rest of his commentary seriously. If he wants to participate in a “meaningful way” in a debate about MU and EMRs, I don’t know that disparaging his peers is the best place to start.
Allscripts loses another big customer in Lahey?
Oh boy.
Bravo Dr. Borges. MU froze innovation, skewed the adoption curve, and once bitten/twice shy it’s now going to take much longer to get ambulatory care to a place where we truly can have interoperable records.
Look at Shahid Shah’s fantastic article about interoperability:
http://radar.oreilly.com/2012/06/health-it-system-integration.html
Re: I guess MU did reduce the interest in EMRs based on scanned documents quite a bit.
After working with electronic document management systems since the late 1980s, I cannot believe that some EMR products continue to be based on scanned documents! Shame on those vendors promoting their products as such!
Analog document and film capture (scanning) has always been and remains a complementary solution to EMRs/EHRs and PACS, respectively — for analog documents/film received from the “outside” (due to the current stage of health information exchange), for important drawings that are handwritten on paper napkins, for consents and other forms that yet employ eSignatures, etc.
On the other hand, woe to the EMR product vendor or provider organization that has not yet developed / installed and / or interfaced, respectively, all the EMR structured data functionality — so that the organization has no choice but to scan paper-based medical record documents and analog photographic film.
Maybe the above was the situation at Lahey Clinic!
Aside from the pot shots at doctors who dare to treat the poor and elderly, it is hard to take Dr. Borges analysis seriously when his first data point (952K physicians in the US) is lifter from a 2010 (not 2012) WSJ article and is 140K more than the reports from the AMA or any other credible source.
The anti-EMR crowd on here is very passionate, but operate in like politicians – fast and loose with the facts, lots of emotionally charged but unsubstantiated claims.
I am sure the adoption and the effectiveness of the program is overstated – however that doesn’t mean that Dr. Borges claims are any more valid.
Loved the story about the guy with the pericardial effusion, apparently attributed to malignancy. In the States he’d have got his bucket list done and ended up with more money than he started after a little intervention by the tort system.
Ok- I’ll call the Medicaid-accepting providers the “Mother Teresa types”- politically happy, Really?
Thanks for the cudos, Ben!
Deborah, I’ve heard that Dan Steele’s SRS MU certified EHR is pretty good. If it’s as good as his posts,I certainly wouldn’t pass it up.
Wouldn’t it be more politically correct to use solid base data?
McCynical, when it comes to treating the poor and elderly, I’ve been there, done that, and still do. Including these physicians into a MU incentive program, thus compounding their losses by turning them into unpaid data-entry clerks is criminal. Shame on President Obama and his cronies for forcing that on these doctors!
The data that I cited is solid and well-referenced. You can’t get any better than that. The only problem with the WSJ article is that it is 2010 data- in reality, if you follow the growth curve of physicians, the actual numbers is now most likely much more than a million. (In 2009 there were a total of 785,326 physicians– see https://www.aamc.org/download/181238/data/state_databook_update.pdf ). You’ll be hard pressed to find anything for 2011 or 2012 (census data is put out infrequently- just Google it). BTW, why in the world would you think that the AMA’s data is any better than the WSJ’s data?
I’m not “anti-EMR” but I am anti-government interference in healthcare and anti-government using its power to take what little wealth physicians have to enrich another group (EMR vendors). Heck, in my office I use an EMR- one that I programmed using Visual Basic and it’ll go head-to-head with anything out there, especially when it comes to usability and productivity. When I’ve had to interface it with another system, like Office Ally (for electronic billing), I did that in less than 2 weeks time. Heck, the DOD and VAMC systems spent years trying to interface their systems and last year called it quits! They had all the money in the world and the backing of the US Government, yet they still couldn’t do it. My EMR also not only does PMS (eBilling) but also does all of my chemotherapy.
But don’t say that I don’t use “solid base data” because I do. You shouldn’t discount it so quickly just because it doesn’t jive with your biased viewpoint/reasoning. Heck, why don’t you come up with numbers that back up what Sebelius is spewing out from the HHS podiums? Let’s see numbers showing that 20% of physicians have been paid by the government.