RE the AI GLP1 company, Washington Post has an article today by someone who used one of those compounded products,…
Curbside Consult with Dr. Jayne 5/21/12
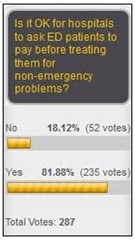
Mr. H posted the results of a recent poll asking whether it’s OK to ask emergency department patients to pay before treating them for non-emergent problems. The vast majority of HIStalk readers responding thought it would be OK.
Since I’ve spent the better part of the last week working the ED, I have to say I agree. Normally I don’t work this many shifts, but the combined stresses of recent changes in our nursing ratios that resulted in some “blue flu” among the nursing staff seems to have inspired an unusual number of call-ins among the medical staff as well. (Either that, or my partners just want to get a jump on their summer vacations.)
Most of my shifts were on the lower acuity side of the ED, which suits me just fine. The full-time docs can handle all the gunshots, “fit for confinement” exams, strokes, heart attacks, and major trauma, thank you very much. I’m perfectly happy to handle fractures, asthma exacerbations, lacerations, and minor trauma. This week, however, we had a boom in patients who simply should not have been in the ED.
This was a bit of a bummer from an electronic documentation standpoint. Our recent upgrade brought us the ability to have condition-specific defaults, and I had spent a fair amount of time building out my personal templates for the conditions I typically see. I did not, however, spend any time building templates for problems that might be best handled at home with a wet paper towel and a nap. The highlight reel:
- A teenager with an insect bite. His mother wrote a note giving permission for a neighbor to bring him in. He noticed the bite in the morning before school when it wasn’t bothering him at all, but mom decided at 10 p.m. that she wanted to know what kind of insect it was that bit him. Unfortunately, I am not an entomologist.
- A high school senior with mild sunburn who wanted to know what she could put on it to make it go away before graduation (which was the next day.)
- An adult male with a 0.5 cm lump on his arm that had been there for six months. That prompted him to arrive at 1 a.m. “just to get checked out,” although he couldn’t say why he was coming in NOW.
I’m pretty sure that if someone in the waiting room would have told them it would be a minimum of a two and a half hour wait and a $200 charge, these three musketeers (and the dozens like them) would probably have chosen to go home. I wish we could have a seasoned registered nurse stationed in the waiting room, administering simple first aid and counseling patients to follow up with a primary physician or a walk-in clinic in a day or two rather than using scarce ED resources. While I was dealing with them, we had an elderly woman with a complex fracture of her upper arm, several patients with lacerations, and a chap with a knee the size of a grapefruit that needed my attention.
Unfortunately, fallout from the Emergency Medical Treatment and Active Labor Act (EMTALA) makes it difficult for us to employ creative strategies to reserve the ED for appropriate use. Becoming law in 1986 as part of the COBRA legislation, EMTALA seemed like a good idea at the time. Although EMTALA was intended to ensure that patients presenting with emergent conditions were not turned away for inability to pay or other discriminatory reasons, the unintended consequence is a generalized fear of saying “no” to anyone who walks in the door.
The Code specifically defines an “emergency medical condition.” More than half of my patients this week failed to meet that standard, yet they had full visits anyway. We had to document each visit in detail, including a full review of systems, counseling on advance directives, nutritional screening, and more. (We also had to arrange transportation home for the mom who brought her daughter by ambulance for a splinter, but that’s another story entirely.)
I wasn’t in practice prior to 1986 so I can’t say what it was like, but I can’t imagine it was as chaotic and soul-sucking as it is now. I was, however, in the trenches when E&M Coding appeared on the scene, and I experienced first-hand the ridiculous make-work that ensued.
Looking at the track record for federal meddling in health care, it’s hard for me to think that the changes occurring as a result of Meaningful Use will turn out well in the long run. I may have Certified EHR Technology and full command of the Meaningful Use program. I can cite all the measures verbatim even after a couple of glasses of wine. I have more timely access to old charts (which are now actually legible) and better drug interaction checking, but other than that, the benefits still seem elusive.
How do you think we’ll feel in 25 years when we look back at Meaningful Use? E-mail me.



I agree with the sentiment that the ED should not be used as substitute for primary care, and that the current system is set up to foster the abuse of the emergency department for this purpose. That said, I don’t see a suitable alternative to providing indiscriminate treatment to all patients, regardless of their ability to pay, who present at the ED. Once you go down the track of requesting payment preemptively, some very sticky questions arise. Such as: Who determines who needs to pay ahead of time and who doesn’t? What happens if a patient can’t pay, has no insurance, and has a non-emergent but still serious condition?
As a career ED Doc, the anecdotes make me laugh. But I have to say that I got mellower about “abuse” of the ED the older I got. There’s nothing wrong with a co-pay; obviously those who can’t or won’t front the money get treated just the same, without regard to that decision. Here’s the deal: there is no way to sort out anyone without actually seeing them. One has a bug bite; the next has necrotizing fasciitis (and the next 9,999 are bug bites again, sure…). Those who plan their lives pay for those who don’t; those who are fortunate pay for those who have been struck by misfortune. One thing for sure about Meaningful Use: it drives sales for CEHRT but it has almost nothing to do with quality care, quality clinicians or–God help us–meaningfully using the health system itself. I laughed when John Halamka’s recent blog about the importance of integrating the EMR run sheet with the ED used an image of an EMR run sheet which showed a patient whose problem was probably caused by intoxication and who was coming to the ED for difficulty walking. Other history was “unknown.” http://geekdoctor.blogspot.com/2012/05/cool-technology-of-week_18.html The best healthcare software in the world doesn’t change the patient population, so just have fun and realize people are people. There but for the grace of God go I…
Like most other countries in this world we need to multiple level health care system. People are now believing that even if they don’t work for something that they deserve the very best. I had a Dean of a local university tell me a party that everyone in this country deserved the best quality of healthcare. I don’t agree. Everyone in this country should be entitled to basic healthcare. In my opinion the US provides to much free care especially to people who come across the borders only for healthcare that they can not get in their own country. Are we to provide free healthcare to the entire world. I don’t believe that is reasonable or practical. We can’t afford the system we have now for our citizens let alone providing care to the entire world.
The next question is should everyone get the same level of healthcare. I don’t believe so. In France they have a two level system. The basic (national) system is paid by the government. This is covered by taxes. There is also another system where people can purchase the next level of healthcare service. If a patient wants Cadillac service then they can purchase commercial insurance. Manny other countries have this same system.