I tend to think that tests of ability (rounds, in this case), ought to stay close to real-world situations. Therefore,…
News 5/11/12
Top News
Government investigators applying statistical tools to sift through HHS data find $5.6 billion in questionable Medicare billings from 2,600 pharmacies, many of them in the Medicare fraud hotbed of Miami. Some beneficiaries received hundreds of prescriptions each year (two patients received more than 1,000 prescriptions per year), while pharmacies in Baltimore, Detroit, and Tampa had unusually high narcotics dispensing. CMS administrator Marilyn Tavenner said she agrees that oversight should be improved, but doesn’t want CMS to be flooded with false leads, especially since the report does not provide examples of proven fraud.
Reader Comments
From Not a Smurf: “Re: insourcing in healthcare. What do you think about this book’s premise that American workers are being left unemployed because of the importation of RNs and MDs to work at American hospitals & other healthcare settings?” I assume we do import a lot of doctors and nurses. I’ve worked in rural hospitals where we had basically no American-born physicians, creating odd communities of extended families of doctors from mostly India, the Philippines, and Colombia taking care of people who had never been more than 50 miles from home and who often couldn’t understand a word their doctors said. Those docs were smart enough (or maybe just more ambitious) to have chosen procedure-based specialties like surgery, radiology, and cardiology instead of the lower-paying general medicine and pediatrics. And, to open their own practices instead of working for someone else. We had some horrible ones that were certainly harming patients with their obvious incompetence, but I don’t know that the numbers were disproportionate to some equally bad good old boy docs who didn’t pay much attention in their med school classes. I agree with the premise that we have more foreign healthcare workers than you might expect, but I don’t see that as necessarily bad. Foreigners usually take jobs that Americans either aren’t smart enough to do (engineering, computer science) or are too lazy to do (farming, restaurant work). I don’t buy the idea that foreign docs and nurses are stealing desirable jobs from equally qualified and willing American candidates. In the backwater places I worked, you couldn’t pay enough money to get American docs to move there from the more desirable cities — it was foreign-born docs or none at all. The supply of doctors and nurses is artificially limited by schools and licensing boards to keep incomes high anyway, so I like the idea of breaking that monopoly. We’re going to need a lot of healthcare people to care for entitled baby boomers. All the docs I know are keeping plenty busy no matter where they were born. But as I gaze down from high on my soapbox, I’ll ask: what do you think?
From ORISpilot: “Re: Andrew Brearton, CIO of St. Joseph’s Health Center in Toronto, Ontario. Resigned today due to ‘health reasons’ and will be replaced by an interim CIO until a full-time replacement is found.” Unverified.
From Pickle_Juice: “Re: heard two rumors. Partners is dumping their Soarian install in favor of Epic. Lifespan in Providence, RI is switching from Siemens (I think they were Invision, tried Soarian, but pulled back to Invision) to Epic.” Rumor #1: true. Partners has indeed chosen Epic as vendor of choice, but I haven’t seen a definitive list of what they’ll be replacing (knowing Epic, probably everything possible, but the business apps weren’t mentioned in the e-mail from the Partners CEO that was forwarded to me). Rumor #2: not true yet. I asked Lifespan SVP/CIO Carole Cotter (above) and she says Lifespan is considering five vendors, with the incumbent Siemens being one of them. The selection will take several months.
From Joey: “Re: Partners. This is a dream sale for Epic. The private offices are latched onto Partners as part of their IPA, so Epic’s sale goes far beyond the hospital itself. Partners will tell them that to stay in the IPA, they will have to get on Epic, and they will.”
From Eagle Driver: “Re: St. Luke’s in Kansas City. Just heard a wild rumor that they’re going Epic. I think they’re McKesson inpatient, Allscripts outpatient. No real information, but maybe you can check with your sources.” VP/CIO Debe Gash says they’re evaluating products, but haven’t made a decision yet. The fact that they’re evaluating products says a lot (are any Horizon customers not actively looking?)
From Blue Dog: “Re: [hospital system name omitted]. Re-evaluating their EHR strategy for owned practices in over 100 cities. [product name omitted] was picked in 2010, but has been an epic (no pun intended) failure, with no successful implementations and three botched ones. They are moving to athenaclinicals for at least a quarter of future installs. Hospital and vendor staff can’t get along and hospital leadership is so frustrated with the IT department that it’s beyond reality. Huge internal struggle. Many of the EHR issues are actually related to IT issues.” Unverified, with names removed for now. The CIO didn’t respond to my inquiry, but I’ll allow a bit more time.
HIStalk Announcements and Requests
![]() This week on HIStalk Practice: ONC launches an Health IT Dashboard. Sermo says its iConsult app is a hit with physicians. ONC publishes a guide to privacy and security for physician offices. A Tennessee practice agrees to pay $4.36 million to settle a fraudulent claim lawsuit. ChartLogic makes a big EHR sale to a 25-provider group in Arizona. Dr. Gregg shares a juicy (and unconfirmed) rumor about his EHR vendor. It’s all good stuff, but I think Dr. Gregg’s piece is particularly thought provoking. Sign up for e-mail updates when you stop by. And thanks for reading.
This week on HIStalk Practice: ONC launches an Health IT Dashboard. Sermo says its iConsult app is a hit with physicians. ONC publishes a guide to privacy and security for physician offices. A Tennessee practice agrees to pay $4.36 million to settle a fraudulent claim lawsuit. ChartLogic makes a big EHR sale to a 25-provider group in Arizona. Dr. Gregg shares a juicy (and unconfirmed) rumor about his EHR vendor. It’s all good stuff, but I think Dr. Gregg’s piece is particularly thought provoking. Sign up for e-mail updates when you stop by. And thanks for reading.
![]() We are always looking for interesting and fun content for HIStalk Practice, including contributions from providers, consultants, road warriors, or other ambulatory HIT enthusiasts. We can’t promise fame and fortune, but our other regular contributors will likely tell you that Mr. H and I are highly appreciative, occasionally offer constructive feedback, and every now and then send amusing off-the-record information. Drop me an e-mail if you are interested.
We are always looking for interesting and fun content for HIStalk Practice, including contributions from providers, consultants, road warriors, or other ambulatory HIT enthusiasts. We can’t promise fame and fortune, but our other regular contributors will likely tell you that Mr. H and I are highly appreciative, occasionally offer constructive feedback, and every now and then send amusing off-the-record information. Drop me an e-mail if you are interested.
Thank you very much to those 45 generous readers who have contributed to the hat-passing I’m doing to support the four young daughters of Tim Dodson, a long-time HIStalk reader who passed away suddenly last week at 34. He was an Epic analyst with Children’s Medical Center (TX). I’ll leave the Donate button in the right column of this page for a couple of days, also mentioning that two readers (Ed Marx of Texas Health Resources and Dave Shaver of Corepoint Health) have offered to do as I did and match $250 in contributions dollar for dollar, just in case you need to be convinced to slide off the fence. I’ll be sending the money to the fund that’s been set up for the girls shortly and will give you the total. I’m sure I speak on the family’s behalf in saying that they appreciate any and all support, both emotional and financial.
Acquisitions, Funding, Business, and Stock
MEDSEEK announces that private equity firms Silver Lake Sumeru and Essex Woodlands will finance a management buyout of the company. CEO Peter Kuhn says the change will allow the company to accelerate the expansion of its platform.
e-MDs reports a 20% increase in revenue and a 10% increase in employee count over the last year, also saying the company was profitable in 2011 and that it invested 40% of its annual revenue in R&D.
Enterprise data management vendor CommVault announces Q4 numbers: revenue up 27%, adjusted EPS $0.29 vs. $0.25. The $2.4 billion market cap company has never done an acquisition.
Vocera turns in its first quarterly report after its April 2 IPO. Its Q1 results: revenue up 26%, adjusted EPS $0.06 vs $0.07. Full-year 2012 was given as $100-102 million in revenue and non-GAAP earnings of $2.5-$3.0 million. Shares that were IPO priced at $16 are now at $23.35, including a 7% jump after the earnings announcement.
Ireland-based startup Cara Health is profiled in an Irish publication for its Patient Journey Record readmission avoidance software that will be aimed at the US market. Recently discharged patients are called by telephone and their responses to specific questions are linguistically analyzed and compared to a database of key phrases that may predict a need for readmission, allowing earlier intervention. Clinical trials of the software found that 30-day readmissions were reduced by 51%.
UK-based hospital patient care software vendor Ascribe engages William Blair & Company to explore its strategic alternatives, with speculation being that the investment banker might find a US buyer.
Nuance announces Q2 numbers: revenue up 22%, adjusted EPS $0.43 vs. $0.32, beating expectations. Healthcare revenue was up 24%.
Greenway reports Q3 results: revenue up 52%, adjusted EPS $0.08, beating revenue expectations and with year-ago quarterly EPS not stated due to tax changes.
Sales

Banner Health Network and Aetna expand their ACO relationship to include HIE technology from Medicity for population health management and patient services.
Lutheran Healthcare (NY) selects Merge Healthcare’s iConnect solutions as its enterprise imaging platform.
Dossia (NY) selects NexJ Connected Wellness platform as part of a NYC Health Department pilot program to give patients PHR access.
People
Cognosante appoints John Calabro (OK HIE Trust) as leader of the company’s HIE practice.
EHR provider Spring Medical Systems promotes Mark Benvegnu to president and CEO. He will continue as chairman of the board.
iSALUS Healthcare, developers of OfficeEMR, names Chuck Dietzen MD (Timmy Global Health – above) chief medical officer, Randy Kidd (Stratice Healthcare) EVP/CIO, and John Brady (Stratice Healthcare) EVP/chief marketing officer.
The National Council for Prescription Drug Programs elects First Databank VP Thomas R. Bizzaro to its board of trustees.
Scott West (STC/SeeBeyond/Sun Microsystems) joins NextGate as SVP of global sales.
Announcements and Implementations
Michigan Department of Community Health, Michigan Health Connect, and Michigan Health Information Network activate real-time electronic reporting of public health information to the State of Michigan’s Care Improvement Registry using Medicity’s platform.
Baptist Health South Florida deploys Centrify Suite for access management and centralized user management.
BCBS of North Carolina and SAS announce their collaboration, with BCBSNC using SAS database analytical tools to identify patients who could benefit from specific interventions and to allow the insurance company to target its offerings and communications.
PDR Network and the iHealth Alliance announce a drug safety certification program for EHRs and e-prescribing platforms. Products earning a PDR Certified seal must contain full FDA drug labeling for prescribers, drug alerts and warnings (safety alerts, boxed warnings, recalls, and REMS Communications), adverse drug event reporting, and patient education content, all updated at least weekly.
Veriphyr donates its patient privacy breach protection service to Gillette Children’s Specialty Healthcare (MN).
M*Modal launches its cloud-based speech understanding platform and M*Modal Fluency Direct for enabling speech in EHRs.
Government and Politics
In compliance with the HITECH Act requirement, CMS publishes the names, NPI numbers, business phone numbers, and addresses of Medicare EPs and hospitals that have successfully demonstrated MU as of March 2012. If you happen to need a free list of 44,000 providers or almost 1,000 hospitals, the lists can be downloaded in either CVS or PDF file formats.
HHS issues final rules to streamline reporting requirements for hospitals and to retire older versions of e-prescribing transactions for Medicare Part D. The regulation changes are expected to yield over $1.1 billion in savings the first year.
The Utah Division of Occupational and Professional Licensing puts its upgraded disciplinary action database online, including records of physicians, nurses, pharmacists, and other licensed healthcare professionals.
I’m impressed with The Health Datapalooza taking place in Washington, DC on June 5-6, put on by the Health Data Initiative. Speakers include some VC guys, the CEO of Aetna, Matt Miller of NPR, the executive editor of Wired magazine, former Senate Majority Leader Bill Frist, Todd Park (US CTO), Kathleen Sebelius (HHS Secretary), Atul Gawande (physician author), Dominique Dawes (former Olympian), and Farzad Mostashari (ONC). Sessions look interesting. Hospital guys like me find it hard to get time off to run around to conferences, so if you’re going and want to be my on-the-ground reporter there, let me know.
Speaking of government conferences, I’m excited that EHR design guru and HIStalk contributor Dr. Rick saw my mention of the May 22 ONC/NIST EHR usability conference and has decided to attend (and to provide a post-conference report, I assume.)
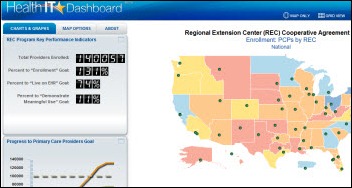
ONC announces its Health IT Dashboard, with geographic maps covering its various grant programs and HIT adoption.
Other
Imprivata announces the results of its Fifth Annual IT Trends Survey, including findings that single sign-on, virtual desktops, and remote access are the top three enablers for engaging physicians to adopt CPOE.
Speaking of Imprivata, here’s their latest cartoon (insert your own orthopedist joke here). If you’re a Scott Adams wannabe, submit your cartoon ideas here.
Finding it hard to keep track of which vendors have acquired which other vendors over the years? Check out this acquisitions family tree, graciously offered to HIStalk readers by Constantine Davides, senior analyst with Boston-based JMP Securities. It could be turned into a fun HIT trivia game, with questions such as, “ What was the coding solution vendor that Cerner bought a few years ago?” or, “What vendor bought Intelus?” I bet it will jog some good stories out of Vince for future HIS-tory presentations.
Here’s another video in honor of Nurses Week, this one recommended by a reader since it makes her think of her sister, a pediatric oncology nurse, and her patients.
University of Miami’s medical school will lay off up to 800 employees because of state budget cuts and reduced payments from struggling Jackson Health System, which itself laid off more than 900 employees earlier this year.
An employee of Waukesha Memorial Hospital (WI) is charged with embezzling $1.5 million from the hospital by submitting invoices from his wife’s painting company. Management got suspicious five years later at the large number of invoices paid to a single company, then determined that nobody had seen anyone doing any painting other than hospital employees. The employee told investigators that he wanted to make restitution, saying he estimated he owed the hospital $100K. When shown the deposited checks for $1.5 million, he said, “So I guess I probably owe them more.”
Sponsor Updates
- A group from the University of North Carolina Hospitals wins a prize for their abstract on LVAD at the UNOS Transplant Management Forum. Their work was sponsored by OTTR Chronic Care Solutions. Above are Paul Kenyon of OTTR, Randy Watkins of UNC Hospitals, and Tim Stevens of Providence Sacred Heart Medical Center & Children’s Hospital (WA) and chair of the OPTN/UNOS Transplant Administrator’s Committee.
- Bloomberg Businessweek profiles Digital Prospectors Corp.
- At this week’s Healthcare IT Institute Conference, Aventura SVP Brian Stern discusses comprehensive solutions to change the way clinicians work with HIT.
- Passport Health reports that more than 50% of the facilities listed on Thomson Reuters Top 100 Hospitals for 2012 use Passport’s eCare solution for RCM.
- Orion Health announces the release of Rhapsody Integration Engine V5.
- Medicomp Systems offers a free webinar May 24 and 30 on navigating future demands in healthcare.
- Practice Fusion profiles Andrew Bronstein,MD, an orthopedic surgeon who uses its EMR.
- Emerson Hospital (MA) goes live on the Intelligent Forms Suite from Access, launching its forms on demand functionality from Meditech.
EPtalk by Dr. Jayne
An article published in the Journal of the American Medical Informatics Association demonstrates that linking a personal health record medication review tool to the provider’s electronic health record can reduce potentially harmful medication discrepancies. The trial was cluster-randomized and included 11 primary care practices using the same personal health record. Over the 18-month study period, some practices received an intervention that provided access to a medication module capable of prompting patients to review their medications and identify potential discrepancies.
Now that the comment period for Meaningful Use Stage 2 is over, there seems to be a preponderance of medical associations commenting against it. Nearly 100 groups joined the American Medical Association in sending a 37-page letter to CMS Administrator Marilyn Tavenner. Highlights:
- Non-participants in Stage 1 should be surveyed to identify barriers to participation prior to finalizing Stage 2 requirements.
- New core measures (or Stage 1 menu measures moved to core in Stage 2) should be evaluated for “evidence of efficacy, administrative burden, costs to physicians, and technological standards.”
- Measures assessing elements outside a physician’s control (such as patient use of technology) should be avoided.
- Providers should not have to meet all 20 core measures plus clinical quality measures. Allowing providers to opt-out of a few would allow them to achieve MU with a good faith effort.
- MU rules should only apply to Medicare/Medicaid patients.
- Disparate health IT programs need to be synchronized so that providers are not penalized for participating in one over the other.
Interesting note: state medical societies not signing include California, Montana, and New York. Major organizations not signing include the American Academy of Family Physicians and the American College of Physicians.
The American Medical Association Journal of Ethics (online at virtualmentor.org) publishes an editorial discussing the need for physicians to counsel patients on material they obtain from the Internet.
HIMSS13 calls for both proposals and reviewers are still open. If you have a great story to tell, now’s the time to ensure your boss has to fund your trip to the Big Easy.
For my friends in clinical engineering, Fluke introduces a new device for simulating vital signs during patient monitor testing and calibration. I noticed the website says it’s 17 pounds lighter than its predecessor, which apparently also had the ability to simulate the new onset of a hernia.
We’re wrapping up National Nurses Week, so if you haven’t taken the time to thank a nurse (or several), you still have a couple of days to do so. On further thought, how about making it part of your everyday routine?
Contacts
Mr. H, Inga, Dr. Jayne, Dr. Gregg.
More news: HIStalk Practice, HIStalk Mobile.





















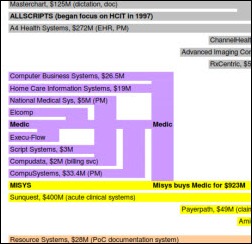




That vendor family tree is awesome. For kicks he should have included a big red line for Epic. Not sure if the joke about family trees without branches applies.
Another thumbs up for the family tree – though the Medical Manager genus is missing? It’d also be interesting to do a couple of the big claims clearinghouses, as they seem to change names every year too.
Family tree: Look at the top. The single lines for Epic and for eCW get dwarfed by the firework fountains that follow them, but they’re there.
Re: Insourcing Health Care – Having worked for several years with community health centers and FQHCs, I can tell you that were it not for foreign-born docs, they would not be able to provide the compassionate and competent care that they do to so many who need it. There is already a shortage of primary care providers, and getting them to work in centers which are more often than not either in rural areas or poorer urban neighborhoods is challenging enough. Add to that salaries which are on the lower end of the scale and you can understand why they oftentimes must take what they can get, though they will still only hire those that will fulfill the mission. Considering that our healthcare costs are so tilted towards caring for those with chronic conditions, and the populations that health centers serve tend to have multiple chronic conditions, these docs are a blessing.
RE: Not a Smurf comments on Insourcing. I couldn’t agree with your quite succinct response of the issue. I grew up in a farming town of 15,000 that had 10 “foreign” familes including my own, all but one were headed by a physician. My father was the only anesthesiologist when we moved in 1980. Despite almost twice the pay of the big city, half the work and 1/3 the cost of living it was over 10 years before they could get a second doc to join him. Even then it was another immigrant family as they could not successfully recruit an American born MD. Having been highly involved on a state level with the AMA, I do have to place some of the blame on ourselves. Whether stated or not, it is AMA’s belief in limiting the number of docs to keep compensation high. I think this will hurt us in the long run as political pressure to ramp up primary care combined with the increasing number of midlevel providers will force the substitution of docs by other types of providers-not necessarily a bad thing. But in the end the artifically created limited demand will be broken and compensation will drop for all, leaving the AMA and other governing boards searching for even more exotic ways to increase physician pay.
It would be nice to see the Republican politicians go after the AMA for artificially increasing the salaries of high end doctors in the same way that they do for labor from other unions.
There are a lot of factors involved but given the stats on similar patient outcomes, can we really say that our training of Docs or their value here is that much greater than in other countries which pay less than half.
Can’t help but wonder if the two stories on Miami (800 layoffs, 5.6 bil in fraud) have a correlation. Not direct mind you – but stealing, even if it is from the government, has implications on some real people. I guess while 800 sounds like a lot, 8% could be healthy cuts… just won’t feel like that to those working on their resume.
Re: Pickle Juice reporting Epic wins is hardly headline worthy. Epic has executed nicely and will continue taking share from Cerner, Meditech, McKesson et al until i) Siemens delivers its integrated Soarian offering ii) Cerner, Meditech and Allscripts make acute ambulatory integration magic from separate solutions or iii) Epic follows Meditech’s lead and begins updating their platform and incurs the same problems for the same reasons….
Re: Cucumber Salad – Epic is actually not taking share from MEDITECH. Epic has been gaining share against McKesson and Allscripts but MEDITECH’s share has between 27% and 28% at least since 2007.
If you have any actual data which would show your point, please post it. The same “Epic is great” marketing is PR whether Epic pays for it directly and calls it “marketing” or not.
Dear “Not a Smurf” and Cog,
There are a number of issues addressed in “Insourced”. In order to provide health workers to rural communities we need to recruit and train young people from those communities. The evidence is so strong on this that it’s one of the strongest points in the WHO’s rural retention guidelines. http://www.who.int/hrh/retention/guidelines/en/index.html
Unfortunately, nursing and medical schools are currently set up to accept metropolitan young people rather than rural young people and most students get no exposure to rural practice. We need to change the way health professional schools recruit and train students.
I agree with you when you say that almost no amount of money will lure a metropolitan to health workers to rural areas. Also, once more foreign trained health workers have finished their initial jobs in the US, they are more likely to work in metropolitan areas than US workers. Although it’s cheaper in the short term to recruit foreign workers, it’s more cost effective in long term to train and retain rural US citizens. This is the subject of a recent peer reviewed article: http://www.ncbi.nlm.nih.gov/pubmed/22361802
@Coincidence: The 2 Miami stories are unrelated. Much of the Medicare fraud in South Florida happens as a result of identity theft, fraudulent clinics, and even organized crime. Jackson is just a typical sad story of a county hospital in a poor area that’s struggling for funding to stay afloat. It is also UM’s primary teaching hospital, and UM has not built up enough of a sustainable presence otherwise in the region to be a referral center of choice for paying patients.
A big thank you, Constantine Davides, for the outstanding family tree of EHR/EMR vendors / products. Having been an HIT professional for 30 years, I always maintained that gaining an understanding of a product’s ancestry is essential for any technology buyer in today’s market. Do you have the time / willpower to 1) maintain and 2) do same for PACS and / or other complementary EHR systems???
The “family tree” was well done, but left out the whole Medical Manager/VERSYSS/PCN/Emdeon/WebMD, etc. portion…lots of limbs there, a few have broken off along the way.
The family tree is perhaps the most insightful HIT industry graphiic to come along.
Edward Tufte would be pleased.
After years of hearing bloggers speculate (pontificate) about why certain vendors fail and others have customers flocking to them, it is now visually obvious. Purer blood line (i.e. less acquistions to delete your product line gene pool) is the path to success. Ex. Epic, Meditech, eClinical, Athena,….
It should be clear from this graphic why Mckesson, GE and now Allscripts are having problems. Integrating that many different products with different core code and data structures limits the ability of these vendors to deliver successful solutions.
One might speculate that through this lens it is easy to understand Mr. Tulman’s emerging troubles.
Email from Jim Noga CIO sent to staff right before CEO email mentioned ending Soarian relationship, CEO email that was forwarded to you did not mention this.
Great family tree…
but where is QuadraMed (Compucare, Mysis (Perse), PDS, Sched pkg from FL?, Coder andd MPI from……etc)
I am sure there are many more…everybody should add to it then we can print it out on the side of a big hot air ballon!