I was born roughly 2 months after the US space program began (Explorer 1), and I've followed it all my…
Monday Morning Update 4/2/12
From HMSUser: “Re: HMS CEO departure. The company confirms.” HIS vendor Healthcare Management Systems (HMS) confirms the rumor I ran here Friday from HMSUser: President and CEO Tom Stephenson, a 25-year company veteran, has left “to pursue some long-time interests.” According to his LinkedIn profile, he is now assistant grass cutter at Stephenson Landscaping Services LLC. Pretty darned witty if you ask me.
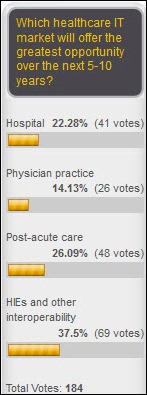
Survey respondents say that companies in the hospital and physician practice market will lag those that are working in interoperability and post-acute care. New poll to your right: how will the Supreme Court rule on PPACA? (no fair answering after the decision is announced.)
My Time Capsule editorial this week from the 2007 vault: Brailer’s Santa Barbara RHIO Baby Goes Down the Tubes. The expensive flop that was the Santa Barbara RHIO launched David Brailer into the first ONC job and got everybody stoked about interoperability despite not having one iota of impact on patients or providers. Some of my parchment-scribed words from way back then: “SBCCDE was a ‘big hat, no cattle’ kind of project that left two sad legacies: (a) it blew millions in grant money, and (b) it seduced politicians and reporters into thinking they’d seen the Second Coming of CHINs, only destined for success this time. They were half right.”
Readers keep asking me to do some kind of “top stories” summary each week. I used to do that with the Brev+IT newsletter I started, in which I rattled off stream-of-consciousness cynical musings about the week’s top news, usually after I was tired from writing HIStalk for the weekend and therefore likely to blurt out just about anything to get finished. I’ll revive that practice at the bottom of this post and give it a try for a few weeks. I’ll kill it if I get bored with it, if I don’t have the time, or if nobody seems to care much one way or another. I’m not looking to create more work for myself, but I’m pathologically eager to please.
Welcome to new HIStalk Platinum Sponsor TrustHCS. The Springfield, MO company’s consulting expertise covers coding, compliance, ICD-10, and cancer registry. Vacant coder positions threaten financial performance and TrustHCS can help out with staff augmentation or full outsourcing of coding services, with every one of the company’s employees holding AHIMA and/or AAPC credentials. They can work on-site or remote, with flexible pricing to meet budget requirements. The company can help provider organizations take advantage of the ICD-10 breather by performing the assessment, analysis, and education that they might have skipped back when the implementation deadline was looming. TrustHCS works with hospitals, practices, ambulatory surgery centers, and any other provider organization that does coding, offering whatever level of support is needed to optimize the revenue cycle. The company can provide the oversight and coding compliance training needed to avoid headlines that throw the whole “bad press is better than none” concept into serious doubt. Relationship matters and experience leads at TrustHCS, whose support I gratefully acknowledge.
Weill Cornell Medical College establishes the Center for Healthcare Informatics and Policy, which will conduct HIT-related research and offer a two-year fellowship in quality and informatics. Rainu Kaushal MD, MPH, a medical informatics professor and director of pediatric quality and patient safety at New York-Presbyterian Hospital, will serve as executive director.
A nice HIStalk Practice post by Dr. Gregg poses the question: are EMRs to blame for terse physician documentation, or are lengthy patient “stories” less common due to (a) lack of physician time, (b) wordy residents who grew up to be more concise, or (c) lack of value when documenting the same old acute conditions over and over?
Vince continues his HIS-tory this week with Part 2 on MedTake. These pieces aren’t just overly fond looks back at long-dead companies – they always contain lessons that might prevent someone from repeating the same mistakes.
HIT Application Solutions raises $2.75 million in a Series A funding round. The Exton, PA company offers the Notifi communications platform for alerts, broadcast communications, and critical test results.
San Francisco-based healthcare IT incubator Rock Health will expand to Boston in June, adding a program on the campus of Harvard Medical School.
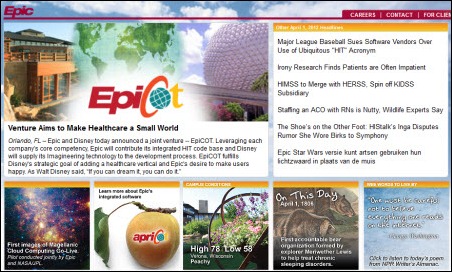
Epic did its always entertaining April Fool’s Day page, even dropping in an Inga mention with ”The Shoe’s on the Other Foot: HIStalk’s Inga Disputes Rumor She Wore Birks to Symphony.” I like it because I did a similar HIStalk spoof years ago and referred to Epic as the Birkenstock-wearing crowd.
The Healthcare IT Week in Review
1. Vocera IPO Shares Jump 50%, Meaning the Company Paid Good Money for Bad Pricing Advice
Facts and Background
Shares in mobile healthcare communications Vocera jumped almost 50% in their first three days of trading after Wednesday’s initial public offering, opening at $16 and closing Friday at $23.40.
Opinion
The company either priced its shares incorrectly or intentionally undervalued them to create positive press from the price run-up. Either way, investors and not the company pocketed the $41 million price difference in the 5.9 million shares offered. Still, the company was smart enough to up the originally planned $12-14 price. A $100 million IPO yield is impressive for a company that isn’t all that widely known and that lost money in FY2011.
Musings
- Timing is everything when it comes to IPOs. Riding Facebook’s IPO coattails isn’t such a bad thing, at least unless Facebook stumbles.
- The company, like most hardware vendors that are anxious to avoid commoditization and increase margins and professional services income by turning themselves into software vendors (think RTLS and bed management systems), markets benefits around its “Star Trek” badge communicators that include care transition, patient transfer optimization, and patient discharge communication.
- Vocera made some key acquisitions in the past couple of years: Wallace Wireless in January 2011 (delivery of alerts to smart phones) and two White Stone Group spinoffs in November 2010 (handoff communications.)
- More acquisitions are sure to come now that the company has $94 million of IPO money in the bank and needs to feed the earnings engine. A priority will almost certainly be value-added software for nurses that can run on the company’s existing communication platform since nurses are its primary users and therefore are most likely to advocate new purchases to otherwise indifferent hospital executives.
- Chairman and CEO Bob Zollars, who joined the company in 2007, was best known as having run high-flying healthcare supply chain vendor Neoforma, and before that having executive roles at Cardinal Health and Baxter. He rode the irrational exuberance bubble hard in January of 2000, when Neoforma.com’s IPO, priced at $13 for 7 million shares, soared to $52.38 on their first day of trading. Not bad for a company with revenue of $464,000 in the previous nine months, in which the company lost $25 million but formed a complex ownership and incentive agreement with hospital buying groups VHA and UHC. Neoforma announced plans to buy Eclipsys for $2.1 billion of its stock in March 2000, but backed off two months later when its own shares dropped by 70%. He knows how Wall Street works and has a real company with strong revenue this time around.
- It’s interesting that the Vocera IPO did so well while investor interest in the HITECH-goosed side of HIT seems to be waning. But everybody likes IPOs, at least for the first few weeks before the quarterly earnings grind sets in.
- I don’t see Vocera getting into the mHealth market, but the successful IPO gives it a strong position in mobile apps for clinicians. It needs a doctor product, though, preferably one with direct impact on patient outcomes since that’s what hospitals will pay big bucks for.
2. Tampa Doctors, Hospitals Fight Over Which Group Will Lead Their Selfless Data Sharing Efforts
Facts and Background
A group of Tampa-area hospitals and the county medical association are pursuing independent efforts to share electronic patient information.
Opinion
Florida has quite a few active HIE/RHIO projects that haven’t made much progress, probably because competition there, particularly among large health systems, is intense. This is one of few times where the previously unstated suspicion and distrust came right out on the table, as observed by a perceptive local reporter.
Musings
- Neither group seems to be making much progress, which isn’t surprising when asking competitors to collaborate selectively with unknown benefits to each.
- Florida’s AHCA issued a four-year, $19 million contract to Harris Corp. in late 2010 to develop a statewide HIE. Two months later, Harris announced that it had acquired Carefx, which offers the Fusionfx data sharing technology for competitors that need to exchange information. The only progress I’ve heard of is the availability of a secure e-mail program for providers and limited patient look-up services among the Big Bend RHIO and a couple of health systems, but it’s only been a year. I don’t know who’s getting ONC’s HIE grant money in Florida.
- Hospitals bring most of the money and technical expertise to the table, while practices create much of the information that needs to be shared. Doctors also believe their motivations are purer than those of hospitals, which have a reputation for wanting to control anything they’re involved with for their own financial or strategic benefit. That plus the technical challenges may kill this initiative off early.
- The main benefit of interoperability comes from hospitals exchanging information with their affiliated practices, which they often undertake without going to a third-party interoperability project. Unlike in some areas, Epic does not dominate the Tampa market. That would be an interesting follow-up article for the reporter – how well do the hospitals that want to control this project interoperate with their owned or affiliated practices?
3. Post-Op Patients Love iPads So Much They Don’t Mind that their Surgeons Don’t Visit Them
Facts and Background
Henry Ford Health System implements telerounding, where post-operative patients are given iPads to communicate by video with their surgeons, who may be miles away.
Opinion
This is a really good idea since it seems cool and high tech, but basically frees surgeons of the requirement to actually make post-op rounds and makes them immediately available so that delayed actions don’t hinder the discharge pathway. But most of all because this is the first high-profile use of the iPad by patients since video projects usually involve Skype on PCs.
Musings
- Post-op patients are usually coherent and can report their own medical situation, so this is more like ambulatory telemedicine than remote ICU monitoring.
- Using iPads is a smart idea since they are portable and cheap. Installing telepresence hardware in individual patient rooms would be ridiculously expensive, and the enhanced video quality would offer no advantage when the intention is simply to chat with the patient. Observers often overlook the iPad’s price and maintenance advantage – it does a lot for $500.
- Cynics might say that a phone call would work just as well as a video call, but physicians like seeing and not just hearing.
- Once the iPads are in the hands of patients, their use could be extended to video-based patient education and self-documentation.
- Once again Apple products prove their medical value not because of more in-depth technical capabilities over PCs, but because they are easy and fast to use, especially since a lot more people know how to use iOS products like the iPhone than have Windows expertise.
- It’s easy to see how this project could be translated into home health or skilled nursing care, where it’s just not practical to have an ongoing physician presence. For that matter, a nurse could round with a single iPad as the physician participates by video.





Mr. H, I am new in the HIT area and definitely appreciate the top stories summary. Thanks.
I also love the top stories summary. I often see news stories, but skim them without being able to add the context of your musings that come from working on the ground. Thanks!
Darn it! I made a mental note to check the Epic home page Sunday but am suffering from CRS (can’t remember @#$%) and so missed the annual April Fool’s fun. Thanks for posting a screenshot, although my aging eyes can’t make it all out 🙁
Next year for sure………….