RE the AI GLP1 company, Washington Post has an article today by someone who used one of those compounded products,…
News 3/14/12
Top News

Blue Cross Blue Shield of Tennessee will pay $1.5 million to settle potential HIPAA violations, a result of the first enforcement action triggered by HITECH-mandated breach reporting. Fifty-seven unencrypted hard drives containing the PHI of over 1 million people were stolen from a BCBST-leased building that did not have access controls.

From HIT Cynic: “Re: EMRs and test ordering. Finally someone says what lots of us out here are thinking.” The authors of the Health Affairs article respond to criticism of their study by Farzad Mostashari in an ONC blog post titled Recent Study: Get the Facts and a sub-headline of “Don’t Believe the Hype.” The original article suggested that EMR usage is associated with higher ordering rates of imaging tests, concluding that expected EMR-driven diagnostic savings may never materialize.
Mostashari said (a) any HITECH-related conclusions from an observational study using 2008 data are worthless, especially since it did not consider clinical decision support and information exchange; (b) EMR users didn’t order more tests, but high-volume imaging prescribers are more likely to view those images using an EMR; (c) the study didn’t look at appropriateness of ordering, so comparing the number of imaging orders omits important factors such as practice demographics and whether the high-volume physicians have a financial stake in the imaging centers they use; and (d) EMR cost savings aren’t dependent on reducing test volume.
The authors respond: (a) physicians who viewed images electronically ordered 40-70% more of them; (b) the famous RAND study that Cerner helped pay for said billions would be saved by reducing imaging and lab test volumes; (c) even though the study data were from 2008, the same EMR vendors are selling pretty much the same products; (d) Mostashari’s explanation that high-volume prescribers probably bought electronic systems specifically to view the results was tested and rejected in their analysis; (e) the study did take into account patient demographics, severity of illness, and other factors; and (f) while observational studies can’t prove causation vs. correlation, ONC has used cherry-picked studies of similarly dubious methodology to cheerlead EMR success and plenty of other studies have found no IT-related quality improvements. The authors conclude:
Dr. Mostashari is also correct in reiterating that randomized trials are the best way to assess health IT. In fact, no randomized trial has ever been published that examines patients’ outcomes or costs associated with off-the-shelf health IT systems that dominate the U.S. market. No drug or new medical device could pass FDA review based on such thin evidence as we have on health IT. Yet his agency is disbursing $19 billion in federal funds to stimulate the adoption of this inadequately evaluated technology. Dr. Mostashari is perhaps the only person in our nation who commands the resources needed to mount a well done randomized controlled trial to fairly assess the impact of health IT, and the comparative efficacy of the various EHR options. Finally, Dr. Mostashari’s unbridled faith in technology is mirrored by his belief that ACOs are the next panacea for health costs and quality. That health policy flavor-of-the-month also remains wholly unproven.
I’m going to score this as a win for Mostashari even though the lady doth protest too much, methinks. The study was only marginally interesting and I would have serious reservations about drawing any conclusions whatsoever from it (particularly in comparing electronic image viewing to the use of full-blown EMRs,) but the authors seem to want to elevate it to a government policy argument, and now are launching a second front on ACOs for no apparent reason. Lazy journalists wrote their usual hysterical headlines with obviously limited understanding of anything in the article, which got Mostashari fired up to launch an unnecessary counterstrike in a war that he not only can’t win, but shouldn’t be fighting in the first place since it just gives the article more exposure.
My conclusion: don’t believe either side. Nobody knows if having previous images available would reduce new orders for them, especially if doctors receive benefit from unnecessary tests. Even if the conclusions of both sides are data driven, unbiased, and definitive (which I’d say is highly doubtful in both cases) they are also irrelevant. Taxpayers are already paying for EMRs and we won’t know for years whether we’ll get our money’s worth in the form of lower healthcare costs. My crystal ball says we won’t unless they’re used to prod patients to change their health risk behaviors, like convincing the 75% of the population that’s overweight to eat better and exercise more.
HIStalk Announcements and Requests
Inga is taking a semi-break, so it’s just me (Mr. H) this time around, other than for a few items she sent over. I’ll dispense with the red/blue icons for today.
Acquisitions, Funding, Business, and Stock
Jiff Inc., a developer of a HIPAA-compliant private healthcare social network and digital health apps platform, completes a $7.5 million Series A financing round led by Aeris Capital. The company also named Derek Newell (Robert Bosch Healthcare) as CEO.
Vocera expects to price its 5 million IPO shares at $12 to $14, using the proceeds to pay down debt and potentially to make acquisitions.
Greenway Medical Technologies announces its first quarterly results as a publicly traded company: revenue up 30% to $29 million, EPS –$0.01. Shares closed Tuesday at $13.75, up from February’s IPO price of $10 but down from their high of just over $15.00 on March 1.
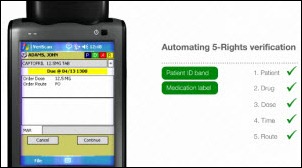
Milwaukee-based point-of-care technology consulting company True Process Inc. acquires the PDA-based VeriScan bedside medication verification system from Hospira. Does anybody even make PDAs these days, and if so, who’s buying them?
Sales
Geisinger Health Plan chooses NaviNet’s Insurer Connect solution to give providers online access to patient benefit information.
Tyrone Hospital (PA) selects Promantra’s RCM system for billing and claims management.
St. Jude Medical Center (CA) chooses PerfectServe’s clinical communications platform.
MedAssets appoints Michael P. Nolte (GE Healthcare) as EVP and COO.
MEDecision promotes Ken Young from VP of finance to CFO.
Announcements and Implementations
The Wexner Medical Center at The Ohio State University goes live on its $102 million Epic system. The hospital appended “Wexner” to its name last month to honor $200 million donor Les Wexner, chairman and CEO of Limited Brands (Victoria’s Secret, Bath & Body Works.) He’s worth $3.2 billion, lives in $47 million house, and has a 315-foot yacht.
Health Language Inc. announces that its data mapping software and content support all terminology standards required by MU Stage 2.
NYU Langone Medical Center announces that 125,000 of its patients are using the PatientSecure palm vein scanning identification solution, launched nine months ago and integrated with Epic.
T-System offers integration with the iTriage Web and smart phone applications, allowing hospitals to list their ED wait times and patients to notify the ED that they’re coming in.
Patient teaching technology vendor Emmi Solutions announces that its products now work on Android and iOS smart phones and tablets.
SCI Solutions offers order entry and results reporting via mobile devices for its Order Facilitator product. The new service provides a national physician directory so that hospitals interested in improving their physician outreach and referral programs can integrate with physicians even if they don’t use the hospital-preferred EMR.
Government and Politics

OSEHRA, the open source community created by the VA in August 2011 to oversee VistA and VA-DoD EHR integration projects, announces three new members of its inaugural board: James Peake MD (SVP of CGI Group, retired Army officer, and former VA secretary), John Halamka MD (CIO, Beth Israel Deaconess Medical Center), and Michael O’Neill (senior advisor of the VA’s innovation program.)
AHRQ is soliciting proposals for the validation of a workflow toolkit it developed to identify and avoid workflow-related problems with technology implementation in the ambulatory setting.
West Virginia’s Department of Health and Human Resources is forced to throw out bids for a Medicaid computer system and start over when HP’s proposal lists a subcontractor that employed the COO of the West Virginia Health Information Network. Philip Weikle says he had nothing to do with the bidder selection and has since left the consulting firm to become a full-time state employee. DHHR had already restarted the Medicaid system bidding last year for unstated reasons.
Innovation and Research
An article in Archives of Internal Medicine supposedly finds that medical residents using iPads felt the devices made them more efficient. I don’t trust the conclusions of reporters when reviewing research articles, so all I’ll say is that the article isn’t available to non-subscribers. I’ll try to remember to pull it up from my hospital PC to see what it says.
A JAMA article concludes that Ontario hospitals that spend the most under the universal healthcare system deliver the best patient outcomes. Patients at the top-spending hospitals had lower rates of death, readmission, and cardiac events and were more likely to be given evidence-based care. However, the authors note that lower-spending hospitals can’t just increase their spending to improve outcomes since the drivers seem to be the use of evidence-based medicine, better nurses, more specialists, and more technology. It may also be that the higher-spending institutions are teaching hospitals. As is always the case, correlation was modest and the unknown or unmeasured factors could be skewing the conclusions.
Other
Poudre Valley Health System (CO), which says its transition to Epic will decrease transcription needs, will outsource 37 transcription jobs to Nuance.
A company that reviews medical insurance claims shuts down, blaming the compliance cost of dealing with a medical data breach after a break-in at its headquarters. Impairment Resources LLC was required to report the breach to numerous federal and stage agencies and says that expense, plus threat of lawsuits by those whose data was exposed, forced the company to declare Chapter 7 bankruptcy. In snooping around, I found that the company’s chairman, Christopher Brigham MD, was a MUMPS programmer at Mass General in 1972.
The local newspaper covers the $750 million implementation of Epic at Providence Health Services. Richard Gibson MD, who runs informatics for Providence’s Oregon Region, says Epic will reduce costs through optimal physician ordering and analytics. He said, “If we’re going to survive and needlessly take money from roads, schools, lunch programs and world peace, let’s not go into diagnostic studies and treatments that don’t do any good.”
TEDMED 2012 will offer a free HD streaming live simulcast at regional locations such as hospitals, medical schools, government agencies, and corporations. It is also offering $2 million in scholarships to in-person attendees, expected to number 1,200 for the April 10-13 conference in Washington, DC. Registration is $4,950.
Several healthcare-related associations release two brochures on personal healthcare records, one for consumers and one for clinicians. They can be downloaded here. They probably should have had readability experts help out since the verbiage is a bit dense for mass consumption. They also mention Google Health, which of course has shuffled off this portal coil (OK, lame pun there by me.)
Here’s another of those overpromising, underdelivering headlines. TV doctor Sanjay Gupta provides his plan to eliminate medical errors, as gleaned from note-taking at weekly hospital M&M (morbidity and mortality) conferences. He’s conveniently included them in his just-released first fictional novel rather than publishing them in a peer-reviewed journal. I’d keep expectations correspondingly modest.
An Oregon jury orders Legacy Health System to pay a couple $2.9 million in their wrongful birth lawsuit. The hospital incorrectly told them their unborn daughter would not have Down syndrome. When she did, they filed suit, saying that if they had been told, they would have had an abortion.
Sponsor Updates
- United Regional Health Care System (TX) builds on its Allscripts portfolio with the selection of Allscripts Care Management.
- Robin Tardif of Hayes Management Consulting posts Part 1 of her series “Reduce Human Error in EHRs.”
- Sam Whitaker, CEO of Greenphire, and Zaher El-Assi, GM for Merge eClinical will present a webinar discussing payment and integration processes for healthcare facilities.
- Versus will participate in the AONE 45th Annual Meeting & Exposition this month.
- Billian’s HealthDATA offers a white paper, Providers’ Perceptions: Accountable Care Organizations.
- OrthoKansas selects SRS for its 12 providers.
- An Aspen Advisors white paper describes the company’s involvement in developing the Epic rollout plan for specialty clinics of University of Utah Health Care.
- Healthwise adds the concept of Patient Response to its patient education EMR module, which allows prescribers to order health education and tools and receive reports back of their degree of compliance.
- Sunquest Information Systems will participate in the 2012 Patient Safety Awareness Week after releasing Collection Manager 5.0, which focuses on POC patient safety.
- Xpress Technologies integrates with DrFirst to launch its end-to-end eRX solution.
- Intelligent InSites integrates WaveMark’s consumables asset tracking system with its RTLS.
Contacts
Mr. H, Inga, Dr. Jayne, Dr. Gregg.
More news: HIStalk Practice, HIStalk Mobile.















If OSEHRA succeeds, it basically represents a job killing federal take over of the EHR space with the long term outcome of us all using Vista or most likely something even less competitive that Vista is today given the lack of market driven escalation.
If it fails, our service men and women, their families and our Veterans will have another decade of AHLTA and Vista failing to meet their needs and perform at the level of commercial alternatives.
Where is the win in the 20+ Billion dollar federal spend other than that make Senator Jay Rockafeller (D) of West Virginia a shoe in for reelection in a district that houses thousand of Vista programmers.
He was the one who got the “open source” commitment into HITECH in the first place.
Obamacare isn’t the last step in the government take over of medicine and medical technology.
OSEHRA will do to EHRs what Medicaid has done for patient care.
Where’s Jimmy Carter with his sweater when you need him!
“Xpress Technologies integrates with DrFirst to launch its end-to-end eRX solution.”
What are the two ends? I’m seriously confused.
Your comment about the readability of brochures on personal health care records was on target. “Readability Studio” software scored the Blue Cross-Blue Shield FAQs for Conumers at 1st-2nd year college reading level (grade 13 – 14), “difficult” (45) on Flesch’s Reading Ease formula. This is typical of most health information for consumers (like HIPAA notices); many consumers won’t understand their personal health care records. Although federal agencies often recommend an 8th grade reading level for consumer health information, that’s almost never achieved.
I agree with McCormick et al that the evidence supporting EHR and CPOE devices is flimsy at best.
If Mostashari wants to keep Secretary Sebelius happy, who in turn wants to keep President Obama happy who in turn wants to keep his pal, Glen Tulman happy, he must continue to trumpet the virtues of EHRs, even though the outcomes and costs are no better than with the systems of care that have been replaced.
What is most troubling about all of this is that there have been many deaths of patients who would not have died when they did if it were not for the care disruptions, care delays, conitive errors and other errors faciliatated by these unvetted CPOE medical devices.
However, no one seems to want to know and when the truth is outed by authors such as McCormick et al, they are attacked by the likes of Farzad Mostashari.
Has Farzad himself managed citically ill patients with multi organ failure using CPOE devices?
The rapid deployment of these devices with oft inadequate back up for crashes and supported by thin evidence, is becoming a public health hazard.
In defense of Dr. Gupta’s promo–it is far faster to get action with a popular book than wait for peer review to move change.
Mr. H. – Just an acknowledgement of the pleasure you provide for so many of us with your insightful analysis of the ONC playing field. The discussion regarding the Health Affairs piece is spot-on in my opinion. It’s nice to have you intermingle discussion of more scholarly work (be that as it may) with the useful running commentary of the day-to-day industry. Through the looking glass we go..
Re not tired of suzy rn: This commenter seems to frequently mention many deaths of patients due to issues or crashes with CPOE but I don’t believe I have ever seen any news or research reports suggesting the same thing. If this is true, why isn’t anyone hearing about it and why aren’t more people mentioning it? Also, several of the factors she mentions seem to be failures to have adequate disaster response plans in place. I would not categorize these as failures of EHR systems but rather management/leadership failures. Clearly EHR systems are far from perfect and there is much room for improvement but I haven’t seen anything that makes me think they are public health hazards. I think Mr. H’s comments about the Health Affairs piece is better reasoned and would like to see some other readers comments (on both sides of the issue)
Fudd Medical Center
Not to scoff at a $200 million donation, but the first thing that I thought of when I read the blurb on Les Wexner and Ohio State was classic Bugs Bunny.
“My name is Elmer J. Fudd, millionaire. I own a mansion and a yacht”
Well, you know then but, it was encouraging to see the researchers showing increase in testing with EMR stand up to Mostashavi. My golly gosh, who is this Mostashavi to attack these humble researchers.
Well then, what Mostashavi should be spending time on is the reasons for excessives orderings of expensive tests. My golly gosh, when I first used a CPOE, well you know then, I want to learn if a MR image was ever done.
My golly gosh, there is no any searching functions. Scrolling, scrolling, scrolling til my eye ball blurs. What horrible state of affairs. Of course more tests will be ordered when it is, you know then but, quickers to order a new test than to scroll, scroll, scroll, to find a prior one.
Welll then but, this is not a meaningfully useful device when such times is wasted.
Mostashavi should be doing something about this ridiculous weakness instead of covering for the flawed devices to keep his job.
My golly gosh, who says “my golly gosh” three times in three paragraphs? Well then but, Pradba writes like a schizophrenic friend of mine speaks.
I’ve always assumed Pradba aims for sarcasm and comes off as smarmy and ignorant. But I have a hard time trusting the POV of someone who can’t be bothered to spell Mostashari’s name correctly.
Pradba, your theatrical approach is taking away from any nugget of a message you may have. It’s tiring.
Agree on the Prabda comments.
Between Prabda, Suzy RN, not tired of Suzy RN – feels like I’m growing less interested in HISTalk in general.
We all enjoy anonymity, but beyond a point these guys drone on and on and on without any new contribution the core discussion.
Prabda, Suzy RN, not tired of Suzy RN and SS all the same??