Giving a patient medications in the ER, having them pop positive on a test, and then withholding further medications because…
Monday Morning Update 11/21/11
From FunFacts: “Re: Newt Gingrich. The 2010 Cerner Health Conference had a speaker from Newt’s Center for Health Transformation, Melissa Ferguson. Any idea what she talked about?” Newt’s business is getting scrutiny from everywhere now that the dearth of decent Republican candidates puts him in front of the pack by default. The Washington Post says his think tank pocketed $37 million from healthcare companies. Not to mention that HIMSS gave him its Advocacy Award in 2005, admiring his “consistent support and insight for the adoption of interoperable health records” as a “key collaborator and advisor with HIMSS and others on healthcare information technology topics.” CHT has locked down its online membership list, but I mentioned some of Newt’s clients back in 2007: GE Healthcare, Siemens, Allscripts, CHIME, and more.
From From the ONC Annual Meeting: “Re: Epic. In the usability session, Janet Campbell from Epic said the government would need to pay Epic to perform usability safety validation. An audience member asked how much more than $27 billion would be needed. Silence from young Ms. Campbell. Is this an indication of the way the EHR industry (or maybe just Epic) is going to react to the IOM report on HIT safety?” Unverified. The shame is that customers aren’t pressing vendors for improvements. That being the case, I can see the vendors’ point of view: why should they (and thus their customers) be forced to pay for an unfunded mandate for changes that customers aren’t demanding? (much like EHR certification.)
From Quixotic: “Re: Epic moving into Meditech territory. The board of Poudre Valley Health System has approved the decision to move from Meditech to Epic. This comes right on the heels of the Edwards decision you published last week. Both were Meditech 6.0 sites.” Unverified. Poudre Valley is a Baldrige winner and CIO Russ Branzell (above) is a pretty high profile, quoted on Meditech’s site from 2009 as saying, “being committed to excellence also meant being committed to our Meditech system.” It was just this past January that Russ said PVHS’s Meditech implementation would be complete right about now after spending $30-40 million.
Regardless of whether this item is true, what can we learn from recent decisions that have gone Epic’s way?
- It used to only be Cerner who needed to worry about Epic and even then only with its bigger customers. Now it’s every vendor of inpatient clinical systems and hospitals of every size.
- Epic used to be selective about which customers it would take on. Either it has relaxed the requirements or the demand must be overwhelming given the huge ramp-up of customer count, most of it in last two years.
- As hospitals and practices consolidate, Epic’s footprint grows by default since its large customers are usually the acquirer rather than the acquired.
- Everybody said Epic couldn’t scale up to handle a lot of business. They were wrong, at least so far.
- Epic’s revenue is up to around a billion dollars a year. The “small company risk” argument used by big competitors isn’t working.
- Hospitals are so anxious to move to Epic that they don’t care about the money and organizational energy they’ve spent on recent implementations. Hospitals with freshly implemented systems costing dozens to hundreds of millions of dollars are happy to dump them and move to Epic, so incumbents can’t even count on switching costs to protect their customer base.
- If even seemingly happy customers of Epic’s competitors are willing to replace their current systems with Epic, imagine how easily Epic could steal the unhappy ones if it wanted.
Since both Epic and its competitors just keeping doing what they’ve always done, you might suspect the leading team will keep piling on points in this embarrassingly lopsided victory. Time and customer money is running out to mount significant competition, so the only Plan B is to hunker down, try to keep existing customers happy since new ones will be hard to come by, and hope Epic’s dominance causes it to stumble to the point that customers will walk away from their huge investment and go shopping yet again for systems they didn’t want the first time around. That or just cede the core inpatient systems market to Epic and find less-competitive territory, which some pretty cool small companies are already doing.
From Clearing House: “Re: Netwerks. They are our clearinghouse and changed to 5010 on November 7, 2011. The vast majority of our claims have not been processed by payors. We have physicians having to go to their line of credit to make ends meet. Almost two weeks and counting.”
From All Hat, No Cattle: “Re: EHR oversight. I would be interested in your thoughts on these ideas.” This is in reference to a Journal of Patient Safety article by Hardeep Singh MD, MPH; David Classen MD, MS; and Dean Sitting, PhD. It follows up on the IOM’s healthcare IT patient safety report by recommending a national EMR oversight program.
The article advocates the National Transportation Safety Board model mentioned repeatedly in the IOM report. A federal group would work with hospital EMR safety committees to collect and analyze events and near-misses and then publishing prevention strategies (that sounds like the Institute for Safe Medication Practices model, which has been amazingly successful working in exactly that manner).
Provider organizations would have an EMR safety officer (not necessarily a full-time job) who would investigate issues and perform self-assessments. A national board would review aggregated data to spot trends and send out mitigation recommendations, but would also have some clout in working with EMR certifying bodies, NIST, and ONC in a coordinating role.
Recognizing that few clinicians are reporting EHR-related problems, the article proposes two ways to increase data collection: building error reporting tools into EMRs (like “click here to report a problem”) or setting software triggers to detect possible errors (like quickly cancelled orders).
Here’s where it gets a bit uncomfortable: it suggests mandatory investigations. The example given incident is EMR downtime that affects two or more clinical functions and that lasts for more than a day. It also suggests unannounced on-site EMR safety inspections with inspectors armed with a Joint Commission-like list of items to check.
My thoughts:
- I think the NTSB model is probably a good one, especially since NTSB is an independent agency and has no regulatory authority. I’d be fine with it as long as it didn’t become the usually swollen federal bureaucracy run by big-pension political appointees.
- I really like the idea of having one individual in a provider organization (a licensed clinician – MD, RN, RPh, whatever) designated as being responsible for collecting local problem reports, regularly evaluating the clinical systems setup against accepted standards and avoiding known problems. A single point of contact would be useful, not to mention that most hospitals have no single, empowered individual assigned to over see EHR-related patient safety issues – usually it’s just a CMIO whose role has been marginalized as the see-no-evil IT cheerleader.
- The idea of a “click here to report a problem” button is one I’ve advocated previously. It would be nice if vendors would build that in, but that’s really not necessary – somebody could write a little app that would pop up a screen or Web page outside the application to capture the information. The problem is that there’s no way a short description of the perceived problem will be useful without follow-up. Imagine having to sit in DC and track down daily stacks of unrelated rants, petty whining, and “problems” that are of the PEBMAC variety (problem exists between monitor and chair).
- I don’t think the triggers idea would work. The number of false alarms generated would be overwhelming, and before you know it, you’d have hundreds of overpaid civil servants pushing paper with no real benefit.
- I don’t like mandatory investigations or safety inspections. That’s more of a stick than a carrot and encourages an adversarial relationship with providers who aren’t intentionally doing anything wrong.
Education is the key, along with setting some general standards. How many providers run through a test plan before slamming in vendor upgrades? Expire their order sets to make sure they are still relevant? Test every change in a non-production environment? Have non-IT beholden clinician users test and sign off on any changes?
I’ll say again: follow the Institute for Safe Medication Practices model. They are an excellent example of improving patient outcomes without requiring taxpayer subsidies or government bureaucracy. They make one major assumption that I don’t see reflected in this paper: that providers want to do the right thing and will actively participate in the best interests of their patients, making the stick-wielding unnecessary. ISMP uses education, not regulation. They carry clout with drug manufacturers to eliminate product issues that cause medication errors (poor labeling, bad packaging design, confusing instructions.) They provide self-assessment tools, Webinars, and on-site consulting help. If you have a serious patient incident, you call them rather than vice versa.
The most significant but not really stated idea in the article is that EMRs themselves aren’t the problem in most cases – it’s how they are used. That’s a provider problem, not a vendor problem. You can put all the inspectors you want in vendor development centers and you still wouldn’t catch most of the problems as customers develop their own terminologies, screens, interfaces, reports, and workflows. The suggestions in the article put the burden mostly on the customers, not the vendors, and I think that’s fair (it’s their job to put the heat on their vendors for optimal design and fast problem resolution.)
I personally think you could start to turn the battleship with non-governmental non-profit of 5-20 employees. It wouldn’t provide oversight, but leadership. Work on awareness and best practices. Take voluntary reports and even if you don’t get many, blast them out there and let the reaction go somewhat viral. Develop constructive relationships with vendors and call out the obstructionists publicly. Make best friends with all those REC people out there. Align with the people who talk a lot about patient safety but don’t have technology expertise (Joint Commission, state licensing boards.) Steer clear of endless theoretical debates and react to real-life incidents. Stay well away from HIMSS and CHIME if you want to keep your objectivity, but think about working with AMIA. Self-fund through educational and consulting offerings. We have a highly collegial and collaborative industry, so use a network of experts as needed to bolster staffing for specific projects. Even if the government eventually does something, this kind of work will still be needed – ISMP’s work isn’t diminished by the fact that there’s a plodding FDA out there.
Listening: a rare “highest recommendation” for reader-recommended Zip Tang, the most stunning, heart-racing progressive rock I’ve heard since early Genesis or Kansas. For my fellow prog heads, think Flower Kings or Spock’s Beard without the wimp factor and with regular wisps of Gentle Giant, ELP, and maybe a little Styx thrown in, but stripped of the 70s excesses and with a harder edge, more soul, and catch-your-breath harmonies. They are just stupendously good, to the point that I can’t sit still while listening and I almost got a lump in my throat a couple of times from the sheer brilliance of it. Their version of Tarkus is better than ELP’s. Here’s the kicker: these are day-jobbers, with Passport Health SVP Marcus Padgett on horns and keyboard and Richard Wolfe MD of Resurrection Health Care on bass (but I’m not giving them a mulligan for that – their excellence requires no asterisk.) These guys make me remember why I love prog so much. I’ll be playing Zip Tang’s three albums all weekend and buying them from iTunes for the Nano. Truly awe-inspiring, and I’m not prone to hyperbole.
My Time Capsule editorial this week from November 2006: The Bandwagon Effect and Healthcare IT Purchases. A test dose: “After all, everyone whose organization is as good and well-known as yours is buying Vendor A’s products, they say. Those customers are not only deliriously happy, they’ve formed a high school-like clique that makes fun of Vendor B losers and dates cheerleaders after football practice instead of attending chess club meetings. ”
Thanks to one of my CIO readers for this great idea. He gives HIStalk sponsors first crack when seeking consulting help and suggested I create a single form that allows prospects to contact any or all of them in a single step. The result: the Consulting Engagement Request for Information page. Fill in the very basic information about your needs, add a supporting attachment if you like, check off the companies you want to send it to (one, many, or all) and click Submit. Your work is done – the companies you chose get your information immediately by e-mail. I’ll be adding a linked graphic later, so if you can think of a more memorable name for it (I thought of RFI Blaster, but couldn’t warm up to it) let me know.
OhioHealth selects the athenaCommunicator patient communication service from athenahealth. It’s an odd-looking press release since both organizations surgically excised the logical space between their two names, with one choosing to capitalize both names of their artificially conjoined twins while the other chose to capitalize neither. I blame marketing people run amok.
Want to see Farzad Mostashari and Aneesh Chopra bust a move? I’m not exactly sure who shot this video at ONC’s annual meeting (the screen capture above is the best I could get), but I have to say that the bow-tied National Coordinator Dr. FM is looking good out there on the makeshift dance floor with some nice improvisational and rhythmic movement, while the US’s CTO appears somewhere between bemused and mortified. I like to think that they were pulled to the dance floor by the excellent music, the legendary Meaningful Yoose Rap from Dr. HITECH (Ross Martin, MD.) I like that they loosened up and aren’t afraid to have fun. Inga and I tried to connect with Farzad’s predecessors (Brailer, Kolodner, and Blumenthal) and all of them stiffed us repeatedly like we were unworthy interlopers on sacred ground, but the new boss seems a little more tolerant to riffraff of our ilk.
Speaking of Farzad Mostashari, is it just me, or does he strongly resemble the outstanding actor Enrico Colantoni (Veronica Mars)?
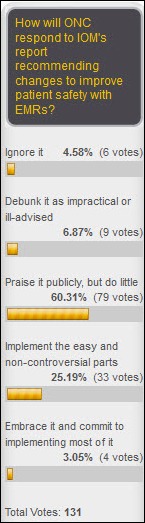
And speaking of ONC, 60% of readers say it will do little in response to the IOM’s healthcare IT safety recommendations. New poll to your right: are HIT Regional Extension Centers worth the $650 million in federal grants designated to fund them?
Two tiny Washington hospitals consider affiliating with Swedish Medical Center, with one carrot being that they’ll get Epic cheap. Jefferson Healthcare, with 25 beds, says they could never afford Epic on their own, while 45-bed Forks Community Hospital says it’s facing a $1 million Meditech upgrade anyway and would welcome Epic at a lower price even though it “may be overkill” for a small hospital.
A Maryland woman says she may sue the hospital where her baby was born after nurses restricted the time she was allowed to spend with her newborn son. The baby had tested positive for drugs, but as an addictions nurse herself, the woman demanded to be tested and was found to be drug-free. The hospital later apologized, saying scheduled computer downtime resulted in erroneous lab results.
Weird News Andy makes a rare weekend appearance, calling out this story in which a woman suddenly goes completely deaf after delivering her third child (and not from the crying, WNA helpfully adds.) The happy outcome: a University of Utah surgeon diagnoses her condition as otosclerosis, a genetic condition in which the hearing bones are fused together. He fixed her problem and she says she’s hearing better than she has in decades.
Another WNA find: a three-year investigation by a group of 21 scientists concludes that there’s not enough evidence to prove that drinking water prevents dehydration, so bottled water companies will be prohibited by law from claiming otherwise. Said a Member of European Parliament, “This is stupidity writ large. The euro is burning, the EU is falling apart, and yet here they are: highly-paid, highly-pensioned officials worrying about the obvious qualities of water and trying to deny us the right to say what is patently true. If ever there were an episode which demonstrates the folly of the great European project then this is it.”










“Speaking of Farzad Mostashari, is it just me, or does he strongly resemble the outstanding actor Enrico Colantoni (Veronica Mars)?”
Come on Mr H, I look like these cats too and you didn’t run my photo.
[rave]
Interesting analysis about Epic. Although, I think ceding defeat to primary systems and finding ancillaries will only be a temporary strategy for any competitors… in the last 10 years I have been working for Epic they have slowly started rolling out new modules to serve additional areas. For instance Beacon (Oncology), Willow (RX), MyChart (Online Portal), Kaleidoscope (Ophthalmology), Phoenix (Transplant), Stork (OB), Welcom (Patient Kiosk) are all Epic modules that have either been developed or become popular in the 12 years I have been working with their products. I imagine in years to come you will see Occupational Health and other modules being developed by Epic to the point where they will have an application for everything. Also, at UGM I notice the majority of new customers are licensed for “Epic Enterprise” rather than individual modules.
Epic is taking over the market. (I’m not complaining, I think it is a great product.)
I think part of their dominance is their responsiveness to their customers. We always complain (people I know as well as myself) that Epic is not responsive or “they live in a fantasy world of fake perfect workflows” but overall they have made huge improvements year-to-year in their software and take the time to listen to their customers.
OK – rave over.
[/rave]
re: Consulting Engagement Request for Information
TPD suggests “RFI Collector” since HIStalk is helping gather everyone’s vendor selections in a folder, and forwarding the details of the RFI to the vendors selected to participate.
Re: Epic Analysis and rave by Timmy D: and don’t forget that Epic is partnering with companies like Hill-Rom for the fetal monitoring strip with a terrific integration between Epic’s Stork and NaviCare WatchChild. Customers can have their cake and eat it, too. Clinicians have smooth workflow and reduced double documentation in a highly litigious area of the hospital. Smart move on Epic’s part.
You ask a good question in your lead report: Why should vendors address safety and usability issues when customers are not demanding such?
The customers are not demanding it because the users at the hospitals are silenced by administrative policies that bring about threats of retaliation in the form of sham peer review and more for those pointing out the dangers and poor usability.
The administration on the other hand have gotten financial “favors” for beta site testing of CPOE and add ons, and have signed hold harmless and do not disclose clauses in their contracts which essentially quiet the administration too.
Thus, it a a specious argument that Judy extends. She has it rigged so that very few complain.
It is good to see that you are devoting so much space to matters of safety and usability. Suzy, RN would be proud of you.
Well then but, so Mr. Newt G. took $ millions from the HIT vendors for his insight on HIT and won HIMSS award for well, his support. What insight would a politician like him have, you know then?
You then now have him frontrunners for president. Oh my golly gosh, what has become of the great United States when someone then like him to have insight on HIT.
Well then, how is this then not big conflict, you know? He should go to hospital in Miami’s Northern Shores Hospital where man died from paralysis after CPOE was switched on and tell family of his insight on HIT, you know, and why the HIT there then did not save him.
Re: Forks Community Hospital
Does that mean Dr. Carlisle Cullen will become an Epic user? Can’t wait to see him present at UGM about optimizing OB workflows for half-vampire births.
I applaud the IOM report which declared that that HIT is unsafe in its present form. I would hope that the Newt read the IOM report and does not stick foot in mouth and suffers the same fate of his competitors.
It behooves the Supercommittee to read the IOM report. It could save the country the $ billions it needs to balance the budget by doing away with this farce of HIT saving money.
Newt brags on HIT and IOM says it is unsafe. Who do you believe?
And, what is HIMSS and LIEberto do now? BTW, HIMSS had its reps on the IOM Committee that produced the report; and also had its reps edit it before publication.
You can only imagine how damning the IOM report would have been had HIMSS not come to HIT’s rescue.
Thank you.
The end.
Ok Mr. H, I think that a lot can be gleaned by analyzing the amount of funk that the vendors (Zip Tang) bring to the stage as opposed to the ONC team. Kuddo’s to the Vendors for brinking great music on a Monday morning. My iTunes is already updating with Zip Tang taking center stage… unfortunately I will not be buying the ONC’s thoughtful version of “Respect my Privacy”
I keep seeing people give kudos and whatever to the IOM. Where was the safety analysis of the paper chart? Even beyond a 1 to 1 comparison, why hasn’t the IOM dissected the gross patient safety issues inherent in the pre-EMR world? Let’s be brutally honest – patient safety was a problem before EMRs and will be a problem after EMRs. At least EMRs provide transparency and an opportunity to measure those errors that lead to patient safety issues. IOM isn’t helping anyone by raising a red flag that panders to the anti-change crowd out there. I’d rather see solutions presented than more problems outlined. And no, yet another government committee is not a solution.
“Non-profit”? What’s non-profit go to do, go to do with it?
Mr. H – could you please read your summary of Epic’s market position, then go read your 2006 column, then revisit your Epic market position summary again? Repeat as necessary…….
And could SOMEONE develop a de-Gupta-izer that would translate his comments to a readable format. Oh my golly gosh, it hurts my head.
When you start putting your political views in, you lose me(but hey, it’s your blog). Hey Gupta, ever looked into what the Secretary of Health And Human Services did previously? I’m guessing you don’t want Kagan to recuse herself from the impending ruling on Healthcare either. Newt’s Center for Healthcare Transformation has spent along time working on Healthcare and quite frankly I welcome the insight and research of his organization. The mission of his organization is directly aligned with his belief that “helping organizations create and implement high-impact strategies and solutions that leverage the scientific breakthroughs, new technologies and transformational opportunities present in times of great change.” Sounds horrible doesn’t it. He has always pushed for free market solutions and individual responsibility as solutions to drive down health costs. Thank You Newt. With all the attacks on people who attempt to serve the people, it’s amazing anyone wants to run for any office. Would you put yourself up to the same scrutiny?
SIC, there is a death in a Miami North Shore Hospital run by Tenet that has contracted with Cerner to deploy CPOE and EMR Millenium with barcoding Bridge to enhance safety applications. The patient received a paralytic instead of a proton pump inhibitor in the ICU. Who knew? No one until respiratory arrest took over.
Safety_NOT
The heartbreak of CPOE: all that money spent and the patient could not be saved.