RE the AI GLP1 company, Washington Post has an article today by someone who used one of those compounded products,…
News 9/9/11
![]() I reported weeks ago that Beth Israel Deaconess Medical Center was prepared to offer its CEO job to Stanford Chief Medical Officer Kevin Tabb MD, who has spent nearly all of his medical career in informatics roles on both the vendor and provider sides of the house as an IT geek. BIDMC announced Tuesday that he has accepted the position. My assessment then was that “he would be a geeky kindred spirit for CIO John Halamka,” which both FierceHealthIT and DotMedNews quoted and nicely credited to HIStalk.
I reported weeks ago that Beth Israel Deaconess Medical Center was prepared to offer its CEO job to Stanford Chief Medical Officer Kevin Tabb MD, who has spent nearly all of his medical career in informatics roles on both the vendor and provider sides of the house as an IT geek. BIDMC announced Tuesday that he has accepted the position. My assessment then was that “he would be a geeky kindred spirit for CIO John Halamka,” which both FierceHealthIT and DotMedNews quoted and nicely credited to HIStalk.
![]() From Inquiring Mines: “Re: Medicare stimulus check. A local group got their federal check and its check number was less than 200, an ungodly low number to have been issued. A provider in the group was told only 6,000 providers had filed to date. Am I missing something? The Medicare spigot doesn’t seem to be flowing as expected.” IM sent a scan of the provider’s check and it does appear that, unless CMS has multiple accounts (this one is called “EHR Incentive Payment Account”) they haven’t issued many checks to date.
From Inquiring Mines: “Re: Medicare stimulus check. A local group got their federal check and its check number was less than 200, an ungodly low number to have been issued. A provider in the group was told only 6,000 providers had filed to date. Am I missing something? The Medicare spigot doesn’t seem to be flowing as expected.” IM sent a scan of the provider’s check and it does appear that, unless CMS has multiple accounts (this one is called “EHR Incentive Payment Account”) they haven’t issued many checks to date.
![]() From Pacman: “Re: Mayo – Elkin lawsuit. A $1.9 million attorney’s fee award for Mayo against Dr. Elkin.” Unverified. This is the suit in which a Mayo doctor (Elkin) sued Mayo over software he developed while employed by them, but then took the source code with him when he left. The jury found in favor of Mayo in April, but also ruled that the doctor is due royalties under Mayo’s royalty sharing policy. As is nearly always the case with lawsuits, the big winners are the lawyers.
From Pacman: “Re: Mayo – Elkin lawsuit. A $1.9 million attorney’s fee award for Mayo against Dr. Elkin.” Unverified. This is the suit in which a Mayo doctor (Elkin) sued Mayo over software he developed while employed by them, but then took the source code with him when he left. The jury found in favor of Mayo in April, but also ruled that the doctor is due royalties under Mayo’s royalty sharing policy. As is nearly always the case with lawsuits, the big winners are the lawyers.
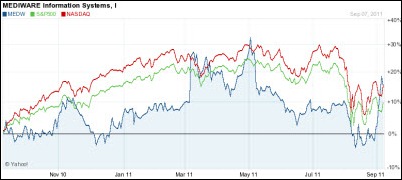
From Harvey: “Re: Mediware. Reported a very solid quarter, but indicated that their labor costs have gone up. It would seem that, despite overall job market woes, there’s a bit of a bidding war on for HIT staff.” Mediware’s Q4 numbers, announced Wednesday: revenue up 20%, EPS $0.25 vs. $0.12, with a big DoD blood bank software contract pushing the numbers up. The one-year share price is above, with MEDW (blue) compared to the Nasdaq (red) and the S&P 500 (green). Market cap is $91 million.
HIStalk Announcements and Requests
![]() Listening: Black and White America, the new album from Lenny Kravitz. Retro 60s funky with big horns in places, modern soul elsewhere, and melodic rocking on some tracks. A great sound throughout and lyrics that aren’t the usual dance track drivel. I get quite a few e-mails from readers wondering how to get back in the habit of listening to new music and I would recommend this as easy to enjoy – it’s got a nice beat, it’s not explicit (he’s religious), and it’s original. And Watching: Mercy (a pretty good hospital yarn) and The Good Guys (a funny cop buddy series). Netflix is predictably in full meltdown mode since any fool could see that its content providers like Starz would be holding it hostage once their old contracts ran out, so I’m watching now before the lack of programming (or increase in price) pushes me to cancel.
Listening: Black and White America, the new album from Lenny Kravitz. Retro 60s funky with big horns in places, modern soul elsewhere, and melodic rocking on some tracks. A great sound throughout and lyrics that aren’t the usual dance track drivel. I get quite a few e-mails from readers wondering how to get back in the habit of listening to new music and I would recommend this as easy to enjoy – it’s got a nice beat, it’s not explicit (he’s religious), and it’s original. And Watching: Mercy (a pretty good hospital yarn) and The Good Guys (a funny cop buddy series). Netflix is predictably in full meltdown mode since any fool could see that its content providers like Starz would be holding it hostage once their old contracts ran out, so I’m watching now before the lack of programming (or increase in price) pushes me to cancel.
Jobs on Healthcare IT Jobs: eGate Integration Analyst, Senior Systems Analyst – Physician Systems, Implementation and Account Manager, Pegasus Health IT Director. There’s quite few interesting jobs there.
HIT is a contact sport, so get off the couch and interact with us: (a) subscribe to the e-mail updates so you can be a like Paul Revere galloping down the cubicle rows shouting out the latest shocking news that I’ll deposit in your inbox if only you’ll allow me; (b) do all that friend / like / connect stuff on your choice of social media sites, seeking out HIStalk, Dr. Jayne, Inga, and me so that we might consummate our union electronically; (c) send me news, rumors, or whatever interests you about the industry; (d) behold with wonderment (and perhaps some strategic mouse-clicking) the graphical proof to your left signifying the unlikely fact that impressively powerful healthcare technology firms are willing to support an anonymous muckraker who struggles to keep a hospital job given the extensive time required to keep up with all the HIT windmill-jousting that needs done; and (e) appreciate that our world revolves around patients, no matter how much electronic insulation separates them from us. Thanks for reading.
Acquisitions, Funding, Business, and Stock
Mediware’s Q4 numbers: $16 million in revenue, up 20% from last year; net income $6.3 million vs. $3.2 million.
Private equity firm The Riverside Company acquires Avatar International, which administers patient satisfaction surveys.
Teleradiology firm Virtual Radiologic acquires the 60-radiologist practice Diagnostic Imaging, Inc. (PA/NJ).
Hospital revenue cycle predictive analytics vendor Apollo Data Technologies Health, Inc. changes its name to MethodCare, Inc.
Sales
CHRISTUS Health (TX) selects HiSoftware’s Compliance Sheriff for SharePoint solution for HIPAA compliance with Sharepoint data.
![]() Royal Caribbean Cruises selects eSeaCare EHR for its Azamara Club, Celebrity, and Royal Caribbean International cruise lines. Dang, I sure need to do a site visit.
Royal Caribbean Cruises selects eSeaCare EHR for its Azamara Club, Celebrity, and Royal Caribbean International cruise lines. Dang, I sure need to do a site visit.
CMS contracts for ICD-10 code translation technology from 3M Health Systems to assist with the conversion of the agency’s systems, applications, and reports from ICD-9.
People
Zynx Health appoints Bill O’Connor, MD (Allscripts) as SVP of global product management and marketing and David Cerino (Microsoft Health Solutions) as EVP and COO.
CSC promotes David Levitt from account director to VP of HIT solutions for its North American Public Sector Health Services division.
Healthcare investment bank Leerink Swann names Bill Suddath managing director of the firm’s Healthcare IT and Technology Enabled Services franchise. He was previously with Robert W. Baird & Co.
AHIMA appoints Lynne Thomas Gordon, MBA, RHIA, FACHE as CEO. She was previously with the Children’s Hospital at Rush University Medical Center.
CentraCare Health System (MN) names Amy Porwoll CIO, replacing the retired Charles Dooley.
Announcements and Implementations
Humility of Mary Health Partners (OH), which includes three hospitals owned by Catholic Health Partners, goes live on its $56 million Epic system.
Accenture completes an assessment and plan to support implementation and interoperability standards for a statewide HIE for the Texas Health Services Authority.
The VA will expand its Virtual Lifetime Electronic Record pilot in which the health records of veterans are electronically shared with the Department of Defense aid private healthcare facilities. It says the HIE capabilities will be live this fall.
![]() The ONC launches HealthIT.gov, a new website which includes HIT information for both healthcare professionals and consumers. It’s definitely prettier and easier to navigate that older ONC site, but contains much of the same information.
The ONC launches HealthIT.gov, a new website which includes HIT information for both healthcare professionals and consumers. It’s definitely prettier and easier to navigate that older ONC site, but contains much of the same information.
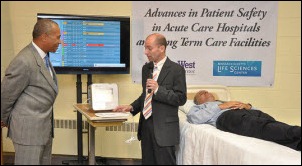
MetroWest Medical Center (MA) debuts its use of the EarlySense system, which uses motion sensors placed underneath beds to track patients’ vital signs. Massachusetts Governor Deval Patrick was on hand.
TeraMedica introduces a medical archiving solution capable of managing from 25,000 to 10 million medical image procedures.
Free EHR vendor Mitochon Systems announces built-in connectivity from its EHR to Hoag Hospital’s Medicity-powered HIE.
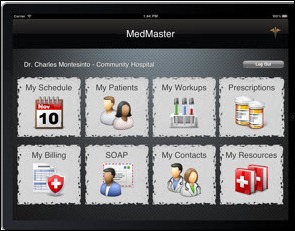
Nuance announces that MedMaster Mobility has added voice-powered navigation and documentation capabilities using Nuance Healthcare’s cloud-based speech recognition. The app is a customizable mobile front end that works with any EHR system.
Athenahealth releases a dashboard showing the progress of its network of physicians toward meeting Medicare Meaningful Use requirements. Inga interviewed Jonathan Bush, athenahealth CEO, president, and board chair right after the announcement was made. A snippet:
Show me how you are going to audit this. I want our clients to prepare for audits now. I want to make sure you audit more your fair share of our clients and I want you to do the audits so you don’t just distress our clients. I want you to audit everyone else so nobody attests without really doing it. Furthermore, let’s get away from this attestation thing if you are not really going to do thousands of audits. Then I want you to stop attestation as part of this larger trend of making unreasonably and obscene rules with massive penalties for non-compliance, and then not auditing, or auditing in such a random way that it really, really, really hampers innovation and creativity and excitement in the healthcare space. If you want information: ask for it, be ready to receive it, and then pay for it as it comes out. Don’t say, “I will pay you if you promise me I will receive, it even if I don’t receive it.” It’s like “don’t ask, don’t tell” — it is the most absurd and embarrassing way because you create distance between what a doctor attests to and what is true.
Clay County Hospital (IL) goes live on Healthcare Management Systems (HMS), announced in a local newspaper story that surprisingly gives the full names of the last “paper patient” and first “electronic patient,” hopefully with their permission.
Qualcomm and Life Care Networks launch a Wireless Heart Health 3G mobile health project in China. Components include smartphones with ECG sensors, Web-based EMR software, and clinic-based 3G wireless workstations that give 30 physicians access to the electronic records and ECG data.
Government and Politics
![]() Federal agents arrest 42 people in South Florida for suspected Medicare fraud. Assisted living facilities and related businesses convinced out-of-state elderly and disabled people to come to Florida for a fresh start (and to bring their Medicare cards along). They’re accused of submitting $160 million in phony claims, of which Medicare dutifully paid $90 million without question. The lead FBI agent chastised HHS for not preventing fraud upfront, saying that it takes extensive resources to catch the crooks, who by the time they’re arrested, have usually spent all the money.
Federal agents arrest 42 people in South Florida for suspected Medicare fraud. Assisted living facilities and related businesses convinced out-of-state elderly and disabled people to come to Florida for a fresh start (and to bring their Medicare cards along). They’re accused of submitting $160 million in phony claims, of which Medicare dutifully paid $90 million without question. The lead FBI agent chastised HHS for not preventing fraud upfront, saying that it takes extensive resources to catch the crooks, who by the time they’re arrested, have usually spent all the money.
Innovation and Research

Albert Einstein College of Medicine of Yeshiva University will use an NIH-funded grant to study advanced retroviral drug therapy in HIV/AIDS patients in Central Africa. Clinics will implement the OpenMRS open source medical record to collect data, also giving governments the option to make its use a national initiative.
Technology
Inova Health System (VA) partners with a genomics company to sequence the genomes of 500 pre-term NICU babies and their parents to identify OB-related diagnoses and treatments. Information from Inova’s EMR will be used to study outcomes.
Other
In the old days, when a patient arrived in my office, I laid the paper chart on the desk between us. I looked directly at the patient. As we spoke, I would briefly drop my eyes to jot a note on the page, and then look right up to continue our conversation. My gaze and my body language remained oriented toward the patient nearly all the time. In the current computerized medical world this is impossible. I have to be tuned toward the computer screen to check labs, review X-rays, read prior notes, document the patient’s current concerns. Like most internists, I know that the interview is the most important part of a patient visit. It always yields far more information than the physical exam, which, in many ways, is an afterthought. But now that the computer is impeding the intimacy normally achieved during the talking part of the visit, I find that I rely on the physical exam more. Once the patient and I have broken free from confines of the desk, with its dictatorial PC, we have a more comfortable realm, that of touch. As soon as there is skin-to-skin connection, conversation flows more easily. In the absence of a machine lodged between us, the traditional doctor-patient relationship is restored.
![]() An Ontario hospital notifies patients that an employed nurse inappropriately accessed the records of 5,800 patients. The mother of one of them was upset by the hospital’s response to her request for details: they won’t release the nurse’s name because doing so would violate the breacher’s privacy.
An Ontario hospital notifies patients that an employed nurse inappropriately accessed the records of 5,800 patients. The mother of one of them was upset by the hospital’s response to her request for details: they won’t release the nurse’s name because doing so would violate the breacher’s privacy.
![]() Weird News Andy likes this ink: an 81-year-old grandmother gets a chest tattoo that says, “Do Not Resuscitate,” fearing that doctors won’t see the DNR entry in her medical record. “I do not want to be half dead, I want to be fully dead … I don’t want to lie for hours, months or even years before dying. I don’t want my family to remember me as a lump. My mother-in-law lived to be 106 and in the last six years of her life she’d have been much better dead. She was miserable.”
Weird News Andy likes this ink: an 81-year-old grandmother gets a chest tattoo that says, “Do Not Resuscitate,” fearing that doctors won’t see the DNR entry in her medical record. “I do not want to be half dead, I want to be fully dead … I don’t want to lie for hours, months or even years before dying. I don’t want my family to remember me as a lump. My mother-in-law lived to be 106 and in the last six years of her life she’d have been much better dead. She was miserable.”
![]() Also from WNA is this story in which England’s Primary Care Trusts are demanding that family physicians reduce their use of ultrasound, MRI, and CT scans. WNA has a cost-saving solution: send them through TSA’s body scanners.
Also from WNA is this story in which England’s Primary Care Trusts are demanding that family physicians reduce their use of ultrasound, MRI, and CT scans. WNA has a cost-saving solution: send them through TSA’s body scanners.
![]() Police in China are investigating the death of a patient during a fire in a hospital OR. Employees evacuated themselves and all patients except one, a man whose leg was being amputated under general anesthesia. When they returned, they found him on the OR table, dead of smoke inhalation.
Police in China are investigating the death of a patient during a fire in a hospital OR. Employees evacuated themselves and all patients except one, a man whose leg was being amputated under general anesthesia. When they returned, they found him on the OR table, dead of smoke inhalation.
Sponsor Updates
- The Disposable Film Festival and Practice Fusion launch Disposable Film Festival Health to encourage original short films about health, medicine, patients, or doctors. Participants will compete for a $5,000 prize.
- Orion Health is adding more than 100 new positions, with about two-thirds in New Zealand and the rest in North American and the Asia-Pacific region. Most of the openings are in R&D.
- Ten unaffiliated physician practices connect to the Coastal Connect HIE (NC) and begin the electronic transmission of patient referral data using Medicity’s iNexx technology.
- Radiology Associates LLC (LA) selects McKesson Revenue Management Solutions for practice management and medical billing services.
- Robert Freedman of Hayes Management Consulting will moderate an ICD-10 panel discussion at HCCA’s New England Regional Annual Conference on September 9 in Boston.
- Stockell Healthcare Systems and ZirMed announce a partnership in which ZirMed’s claims management will be integrated with Stockell’s Insight Revenue Cycle Information System.
- Decatur Medical Center (IL) will deploy Wolters Kluwer Health’s ProVation Order Sets. Wolters Kluwer also signs a multi-year contract with Health Shared Services British Columbia for its Lexicomp solution.
- TeleTracking Technologies announces the formation of its RTLS Workflow Consulting Group. The company is also hosting a free webinar, RTLS Asset Management and How to Make the Most of Your Owned Equipment Resources.
- MediServe clarifies the PAI Discharge Window.
- Cumberland Consulting Group promotes Tom Howard to principal.
EPtalk by Dr. Jayne
JAMA is e-mailing physicians to take part in a survey regarding mobile electronic devices. Questions included: what devices are owned; plans for new device purchases; how much time is spent each day using a mobile device for medical information; when during the day devices are used; how important the device is for various pursuits; and desirability of a medical journal app for full text articles.
Mailbox alert: The Centers for Medicare & Medicaid Services will be mailing revalidation requests to over a million health care providers, more than half of which are physicians. Providers who enrolled prior to the institution of new screening criteria on March 25, 2011 will have 60 days to recertify their enrollment or be blocked from billing Medicare. Providers worry that the already cumbersome Medicare enrollment process will negatively impact honest providers rather than catch the crooks for which it was intended.
This week’s New England Journal of Medicine includes Electronic Health Records and Quality of Diabetes Care. The authors looked at diabetes care data from 569 providers at 46 practices from 2007 to 2010, concluding that the “findings support the premise that federal policies encouraging the meaningful use of EHRs may improve the quality of care across insurance types.” The practices included safety-net providers and publicly reported performance data. On composite standards for diabetes care, EHR locations scored higher than paper-based locations for outcomes and also showed a higher annual improvement (after adjusting for insurance, age, sex, race, ethnicity, language, income, and education.)
The authors note that this is in contrast to other recent studies showing no improvement in quality for practices using EHR. They attribute their favorable results to looking at systems with clinical decision support that is specifically designed to improve care and which include mechanisms for care coordination and provider communication. Additionally, patients had to visit the practice two or more times during the study period for inclusion. The authors propose that this demonstrates a “mutual commitment to longitudinal care” which may have been lacking in other studies.
Medical Economics recommends some LinkedIn groups for social media savvy physicians to join. I was disappointed to not see the reader-created HIStalk Fan Club on the list. With over 1,800 members, it beats all but two of the groups listed.
Several of my friends who are consultants in the health IT realm spend most of their weeks traveling from practice to practice. Since food is no longer served in most parts of the not-so-friendly skies, road warriors are often subjected to the carry-on fare of their neighbors. One former colleague was so offended by his neighbor’s snack he e-mailed me from 30,000 feet looking for sympathy. Normally I’d tell him to “suck it up,” but he snapped a photo of the fare: Ahi tuna jerky. The aroma was bad enough that someone asked a flight attendant to speak with the passenger about putting it away. I’m not sure about the rationale behind dehydrating a perfectly good piece of fish, but to all the road warriors out there, may your flights be fish-free.
Have a health IT road warrior horror story? E-mail me.
Contacts
Mr. H, Inga, Dr. Jayne, Dr. Gregg.






















>>> This week’s New England Journal of Medicine includes Electronic Health Records and Quality of Diabetes Care…
This is another worthless retrospective, single arm, biased review of a select group of patients, run to “prove” that HITECH works.
The only study that I’ll believe in is a prospective, blind, 2-arm study pinning the HITECH-mandated EHR vs. a paper system/EMR/combination of paper+EMR looking at similar parameters. Both arms need to have similar numbers of committed patients with similar disease types. Parameters should be applied to both groups equally.
The studies that I’ve seen do this in the past showed NO difference in care. This NEJM study is the typical “yellow journalism” printed to “exploit, distort, exaggerate, promote and hype information or stories of questionable relevance, importance or probity for the purpose of [promoting an agenda]” (from http://newsroom-magazine.com/tag/yellow-journalism/ ).
Another annoyance is that they fail to post the overall cost of the HITECH-EHR, as this is an important part of the equation. The question is- should government policy waste $20-$40 billion in a HITECH technology “cash for clunkers” which in places like Great Britain have failed, or should that money go to fund free clinics for people without health insurance. Think of the children of the poor- how many lives would you save with this infusion of money?
Although I’m not surprised at the bias of the NEJM- it is published in Massachusetts where forced EHR use is the norm, it should do a better editorial job or else their readership will continue to slide. I used to pay for the NEJM; nowadays I get it for free, and frequently it’s the first journal that I throw away.
If you believe there is NO difference in care, then it makes even more sense to invest in EMRs. They will be more efficient in the end (obviously many argue they are today), not to mention the mountains of data we’ll have available. Now, you might debate how long it will take to happen, but we have to start somewhere. Rome wasn’t built in a day.
Ok, then I’ll get Obama to buy me my HITECH-ready EHR and I’ll also ask him to get me the staffers to do all of the uploading of mandated data. If he wants unproven technology, then he should pay for it and for its use… not have ME pay for it from my dwindling Medicare dollars.
If I were President of the United States, I’d take $20 MILLION (not billion, not trillion) and give it to a group of programmers to come up with a national EMR. Make it available for free and naturally everyone that would use it would be interconnected and have a great working EMR. None of this back-door dealing with HIMSS to prop up their favorite, most-lobbied “enterprise” EHR artificially with meager HITECH grants then penalties against doctors.
As it stands now, the HITECH Act will kill off Medicare participation by physicians and stands to weaken the program for the elderly just when their numbers are slated to grow exponentially.
@Dr.Borges Or, you could use Practice Fusion’s HITECH-ready EHR entirely for free and save your Medicare dollars. Just a thought.
Hi Emily: Practice Fusion seems to be a fine EMR, as are the likes of Amazing Charts, the one put out by ePocrates, the one by Office Ally, and other free, or low-cost EHR systems. Some “enterprise” EHR systems have potential- my hospital’s Siemens’s EMR is real neat in that it interfaces radiology with any computer system. Its interface, though, needs work. At a cost of $14 million, I would have expected better.
I use a MS Office-based EMR that I first programmed back in the DOS days and which I transferred over to MS Office in 1995. It uses the power of MS Access and interfaces it with MS Excel and MS Word to cover all bases in my medical/oncology practice, including billing (through an Office Ally interface that I put together). It works really well, and is almost free- Office Ally charges me $50 a year for their service.
The problem is with the meaningful use concept trying to prop up the unproven value of EHR systems, even the free ones. For every extra 5 minutes that I have to spend with each patient, that translates to about $125000.00 over 5 years just for my Medicare patient population. There are of course other costs, including hardware, and of course the cost of uploading the meaningful use data on a daily basis. The overall cost of an average “enterprise” meaningful-use EHR was estimated by me in an editorial to be about $60000.00 per year (or more since I left out hardware costs and only calculated an extra 5 minutes per patient). If the EHR is free, then the cost would still come out to $35000.00 per year to deal with the Obama-mandated bureaucracy- still an exorbitant amount.
Citation- http://www.hcplive.com/publications/mdng-primarycare/2009/Mar2009/PC_Medicare_HIT_mandate
Another source used totally different numbers to arrive at similar overall costs- http://blog.srssoft.com/2010/01/readers-respond-the-exorbitant-cost-of-meaningful-use/
President Obama just announced that this week will be “HIT week.” (URL- http://benton.org/node/89793 ) He doesn’t realize that he’s further poising the well by making HIT political.
Bottom line: big government has to get out of the certification and propping up of the HIT industry. Let EMR systems attract users through their value, not through some Obama “cash for clunkers” deal where the purchaser is guaranteed to lose no matter the choice- 1) buy the EHR, get raped over the next 5 years vs. 2) not play and get penalized beginning on 2015.