One solution would be federal (or state) requirements; but more ideally health systems would view their digital patient tools as…
News 5/27/11
Top News
St. John’s Regional Medical Center (MO) may not be salvageable, according to hospital’s president Gary Pulsipher. He says St. John’s, which is part of Mercy Health System, will open a 60-bed mobile hospital by Sunday and will rebuild. The hospital went live on EHR less than a month ago, but will soon be back online to connect the mobile hospital with other Mercy sites.
Reader Comments
![]() From Easily Amused: “Re: magazine typo. A finance newsletter described a vendor as ‘provider of elf-service and revenue cycle management applications.’ I had visions of Santa’s helpers pitching in to improve collections.” At least they aren’t involved in elf gratification.
From Easily Amused: “Re: magazine typo. A finance newsletter described a vendor as ‘provider of elf-service and revenue cycle management applications.’ I had visions of Santa’s helpers pitching in to improve collections.” At least they aren’t involved in elf gratification.
![]() From Meaningless User: “Re: attestation. Do you have any info regarding which hospitals have attested to MU and what their success has been? I have not yet heard any announcements or rumors of a hospital achieving MU yet.” I doubt there’s a publicly available list, but some have met the Stage 1 requirements. It would be interesting to know if any have been turned down, but that’s not the kind of news that makes vendor press releases (not to mention that hospitals probably wouldn’t apply unless they were pretty sure they qualify).
From Meaningless User: “Re: attestation. Do you have any info regarding which hospitals have attested to MU and what their success has been? I have not yet heard any announcements or rumors of a hospital achieving MU yet.” I doubt there’s a publicly available list, but some have met the Stage 1 requirements. It would be interesting to know if any have been turned down, but that’s not the kind of news that makes vendor press releases (not to mention that hospitals probably wouldn’t apply unless they were pretty sure they qualify).
HIStalk Announcements and Requests
![]() In case you missed it this week on HIStalk Practice: Kareo lends advice on how to handle medical billing after a zombie apocalypse. Massachusetts eHealth leads the nation in enrolling primary care physicians for its REC. AMA reports a 45% increase in profits for 2010. Dr. Gregg reflects on egos in the industry. And my personal favorite: the fake doctor who used toothpicks to treat his patient. None of this news appeared on HIStalk , so if you follow the practice side of technology and aren’t signed up to get HIStalk Practice e-mail blasts, then you are getting left in the dust.
In case you missed it this week on HIStalk Practice: Kareo lends advice on how to handle medical billing after a zombie apocalypse. Massachusetts eHealth leads the nation in enrolling primary care physicians for its REC. AMA reports a 45% increase in profits for 2010. Dr. Gregg reflects on egos in the industry. And my personal favorite: the fake doctor who used toothpicks to treat his patient. None of this news appeared on HIStalk , so if you follow the practice side of technology and aren’t signed up to get HIStalk Practice e-mail blasts, then you are getting left in the dust.
![]() I’m taking a few days off for fun family stuff and trying to spend minimal time on the laptop, so I’m a little bit disengaged at the moment as I struggle to resist the gravitational pull of work and focus on non-work. I’ll be happy to get back to endless HIStalk hours in a few days.
I’m taking a few days off for fun family stuff and trying to spend minimal time on the laptop, so I’m a little bit disengaged at the moment as I struggle to resist the gravitational pull of work and focus on non-work. I’ll be happy to get back to endless HIStalk hours in a few days.
Acquisitions, Funding, Business, and Stock
![]()
![]()
Standard Register enters a definitive agreement to acquire 100% ownership interest in informed consent provider Dialog Medical. Terms of the deal were not disclosed.
Resilient Network Systems raises $5 million in Series A funding, led by Alsop Louie Partners. Resilient’s technology facilitates the electronic transfer of health records.
People
Former Healtheon/WebMD CEO Mike Long is named president and CEO of EGHC, of which he was already board chair. The company’s businesses include a health plan, the Lumeris quality management software line, and ClearPractice EMR.
Announcements and Implementations
HIMSS introduces the ICD-10 PlayBook to educate providers on the transition to ICD-10
![]() Allegheny General Hospital (PA) resorts to paper recordkeeping Wednesday after shutting down its Allscripts EMR. The hospital says it upgraded the system over the weekend and began having slowdown problems Monday and Tuesday. The hospital voluntarily shut down the system for about 12 hours while Allscripts fixed the issues.
Allegheny General Hospital (PA) resorts to paper recordkeeping Wednesday after shutting down its Allscripts EMR. The hospital says it upgraded the system over the weekend and began having slowdown problems Monday and Tuesday. The hospital voluntarily shut down the system for about 12 hours while Allscripts fixed the issues.
![]() CHIME reports that 109 individuals have earned Certified Healthcare CIO designation since the credentialing program was launched in July 2009. I said it was a dumb idea then and I’ll stand by that opinion now. Obviously the credential hasn’t exactly gone viral if only 109 out of thousands of hospital CIOs have signed on over two years, voluntarily jumping onto the hamster wheel of spending hospital money on renewals and going to CHIME meetings to earn CE. To each his own, but I’d be embarrassed to use a non-educational credential earned by passing a multiple choice test of job-specific knowledge (designed by asking CIOs what they do on the job, then testing them to see if they theoretically know how to do it). My theory has been that CHCIO appeals to CIOs who feel inferior to their better educated C-level peers because they never expended the minimal effort required to earn a graduate degree by any of a zillion inexpensive, flexible, geography-indifferent programs that are out there.
CHIME reports that 109 individuals have earned Certified Healthcare CIO designation since the credentialing program was launched in July 2009. I said it was a dumb idea then and I’ll stand by that opinion now. Obviously the credential hasn’t exactly gone viral if only 109 out of thousands of hospital CIOs have signed on over two years, voluntarily jumping onto the hamster wheel of spending hospital money on renewals and going to CHIME meetings to earn CE. To each his own, but I’d be embarrassed to use a non-educational credential earned by passing a multiple choice test of job-specific knowledge (designed by asking CIOs what they do on the job, then testing them to see if they theoretically know how to do it). My theory has been that CHCIO appeals to CIOs who feel inferior to their better educated C-level peers because they never expended the minimal effort required to earn a graduate degree by any of a zillion inexpensive, flexible, geography-indifferent programs that are out there.
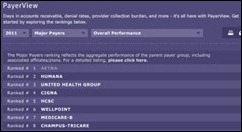
athenahealth releases its sixth annual PayerView Rankings and awards Aetna the top spot among major players. BCBS-RI was the best overall performer, while state Medicaid providers were the worst in terms of days in AR and denial rates. Compared to last year, payers averaged payment one day faster with 5% fewer denied claims.
RCM provider RealMed announces its integration with Epic’s billing software.
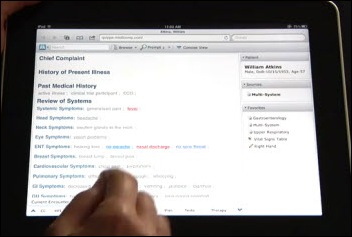
![]() Medicomp Systems announces that its Quippe electronic documentation system SDK is available for licensing to EMR developers. The browser-based, iPad-friendly system (which Dr. Gregg, Inga, Dr. Jayne, and I all raved about after working with it at HIMSS) uses the company’s MEDCIN-powered patented prompting technology to create and present EMR information in an amazingly intuitive way that even a non-doctor like me could use immediately after a ten-minute overview.
Medicomp Systems announces that its Quippe electronic documentation system SDK is available for licensing to EMR developers. The browser-based, iPad-friendly system (which Dr. Gregg, Inga, Dr. Jayne, and I all raved about after working with it at HIMSS) uses the company’s MEDCIN-powered patented prompting technology to create and present EMR information in an amazingly intuitive way that even a non-doctor like me could use immediately after a ten-minute overview.
NCO Healthcare Services earns the “Peer Reviewed by HFMA” designation for several products related to eligibility, bad debt, and and extended office services.
Government and Politics
![]() More grumblings about the proposed ACO regulation, this time from seven US senators. The lawmakers send Secretary Sebelius a letter urging HHS to withdraw its proposed ACO rules, saying, “the proposed ACO regulation will fail to accomplish its purpose” of better quality care and lower costs. The senators claim the proposed rules do not align incentives and accountability and include requirements that are too complex and an ROI that is uncertain.
More grumblings about the proposed ACO regulation, this time from seven US senators. The lawmakers send Secretary Sebelius a letter urging HHS to withdraw its proposed ACO rules, saying, “the proposed ACO regulation will fail to accomplish its purpose” of better quality care and lower costs. The senators claim the proposed rules do not align incentives and accountability and include requirements that are too complex and an ROI that is uncertain.
CMS clarifies financial incentives for ACOs in rural areas, saying participants would be eligible for a savings exemption. CMS says that ACOs with fewer than 10,000 assigned beneficiaries would be exempt from the 2% savings threshold required of larger ACOs.
Add BIDMC to the list of hospitals claiming to be the first to receive HITECH money, $2.57 million in its case.
Emergency physicians claim the biggest challenge to cutting costs in the ED is fear of lawsuits. An American College of Emergency Physicians poll finds that 53% of ER docs say the main reason they conduct the number of tests they do is fear of being sued.
Sponsor Updates
- SCI Solutions is attending and exhibiting this week at the National Association of Healthcare Access Managers conference in San Antonio, providing their traditional “Stress Free Zone” that features massages and cocktails.
- ESD heads to MUSE later this month (booth 910) as well as the Canadian E-Health Conference (booth 203). The ESD folks also shared that their KLAS ratings are up should you be interested in taking a look.
- Oklahoma Surgicare picks Provation MD software for gastroenterology documentation and coding.
- NextGen announces that Springfield Center for Family Medicine (OH) received federal funds for demonstrating Meaningful Use under the Medicare incentive program.
- Tim Reiner, VP of revenue management for Adventist Health System, describes that organization’s use of self-service technology from NCR for patient collections in a YouTube video.
- Yavapai Regional Medical Center (AZ) contracts for several applications from Lawson Software.
- Prime Healthcare Systems, California’s largest for-profit system at 14 hospitals, expands its use of document management technology from FormFast to improve health information, revenue cycle, and patient registration.
- Self Regional Healthcare (SC) chooses RelayHealth as its HIE partner to improve care and support the Meaningful Use efforts of its eligible providers.
- Tele-Tracking releases Patient Flow Dashboard for monitoring enterprise-wide patient flow and getting more efficient use of existing capacity.
EPtalk by Dr. Jayne
I’ve been fairly critical of the federal Meaningful Use program lately. For the record, I want to mention one piece of the program (even if it did get relegated to the Menu Set) that I’m absolutely in favor of: increasing the number of providers who report syndromic surveillance data to public health agencies.
We’ve seen huge benefits to the field of epidemiology with increasing availability of health-related data. I still like the Google Flu Trend site as an idea even if it’s only search data. And “old school” diseases aren’t going away – the number of measles cases reported across the US just hit a 15-year high.
The ability to track, trend, and prevent killer diseases is one of the cooler things we can do with healthcare IT (and one that’s proven to work, mind you). Can you imagine the TV show Quincy ME if Jack Klugman had population-based aggregate data to work with?
In that same vein, a throwdown to my favorite elected officials. Hey Congress, how about putting together a true “Menu Set” of information technology interventions that have been proven to be effective and incentivizing them individually so that providers aren’t faced with the “all or none” problem with Meaningful Use? Any of us who have had to fill out the awful paperwork from the county health department to report a sexually transmitted disease would be happy to interface it directly from our EHR at the click of a button.
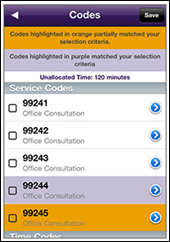
The American Medical Association offers a new app to assist with CPT codes. Only available for Apple users at this point, it allows you to search for, track, and e-mail selected codes. The first problem I had with it is that it apparently ignores the iPad’s gyroscope – it can only be viewed in portrait mode, which is a bummer for those of us that like to prop the iPad on our desk landscape-style so we can stream Netflix while we multi-task.
Navigation to the various sets of codes was pretty easy, but there wasn’t enough information on the screen to make a decision about the right code. The user would have to select each code and read the description. It would be more helpful to have a quick blurb visible on the screen rather than having each entry on the list say “office consultation,” which isn’t very helpful. (It was particularly unhelpful in the preventive codes section, but I couldn’t get a screenshot off my iPad to show, so I clipped this from the AMA Web site.)
I didn’t receive any IT-related checklists for a potential Zombie Apocalypse, but Inga did turn up Kareo’s thoughts on handling medical billing after the fact. I hadn’t really thought about Web-based telecommuting as a strategy to prevent employees from being eaten, but it does make a lot of sense.
Rest assured that due to our decentralized, multi-state virtual office architecture, the HIStalk staff is at significantly lower risk for being decimated by zombie attack than most health IT vendors.
Although Kareo’s piece mentions they didn’t know the code for having one’s brain eaten, I can propose (courtesy of IMO’s Problem IT product): E968.7 Assault by human bite and E979.8 Victim of crime or terrorism.
The Journal of the American Medical Association reports on Navigating the Challenges of In-flight Emergencies. There are apparently minimal standards for emergency medical kits, but kits and employee training vary from carrier to carrier. Airlines also have their own reporting systems and protocols, often relying on physician passengers rather than employed medical control officers on the ground.
The article proposes standardized reporting to the National Transportation Safety Board; expert recommendations for first aid kits (and eventually evidence-based kits based on the data gathered through reporting); enhanced training for flight attendants; and enhanced ground-to-air medical support.
Having had to respond to “Is there a doctor on board” more than once, I’m in agreement. Plus, it looks like an excellent opportunity for vendors to go after another potential customer base. Anyone want to hire a sassy CMIO to write your content for airline medicine? I’d be happy to travel all summer and write code for the most common airline emergencies I encounter along the way.

Contacts
Mr. H, Inga, Dr. Jayne, Dr. Gregg.






If syndromic surveillance from individual providers is so important, why is it so difficult to track down who is going to handle the testing in each test? I was tasked in April with creating a directory for our specialists across the country in all 50 states and several US territories. Less than ten states had a website with the information available. After emailing and calling each states’ Medicaid EHR program, state public health department’s syndromic surveillance contacts, and regional extension centers, we were only able to get information for around 40 of the almost 60 possible recipients of syndromic surveillance. Many state public health department’s syndromic surveillance teams did not even KNOW about the Medicare and Medicaid EHR Incentive program or that providers were required to test with them. The test recipients I was able to reach were uniformly helpful, but all found the idea of syndromic surveillance laughable from our specialty. Eye care is not a field likely to yield ANY usable syndromic surveillance data. Why did the ONC and CMS reach out to the syndromic surveillance community and find out what doctors this data would actually be useful for? Oh right, we know from the implementation guide debacle that they didn’t even BOTHER to talk to the public health constituencies affected by these rules. Perhaps they should learn from that error and create a national directory of who to contact, similar to what the CDC has already compiled for immunization registries?? Even better, how about they reach out to each state and find out if they are ready for testing and automatically waive/require that measure during attestation based on the provider’s address?
“Although Kareo’s piece mentions they didn’t know the code for having one’s brain eaten, I can propose (courtesy of IMO’s Problem IT product): E968.7 Assault by human bite and E979.8 Victim of crime or terrorism.”
Hi Jayne! – Enjoy your articles as usual! The only comment I have about your ICD9 code: “assault by human bite” refers to humans only. Zombies are no longer humans – they’re dead. There is no real classification for dead humans in the ICD9; therefore, a whole new set of codes will need to be developed for them. Because of that, I could see your claim for treatment of any live and breathing human denied by payors until something is agreed upon. Just sayin’…
All time favorite ICD9 code is;
Fall in, on, or from aircraft, injuring occupant of spacecraft [E843.0]
It gets better the more you read it.
Re: HIMSS ICD-10 Playbook. Written by a vendor member of HIMSS, who claims ownership of the content, and who likely wants to sell you ICD-9 to ICD-10 conversion services. And you have to register to get any of the stuff, after which you will almost certainly be promptly called and/or emailed by a salesperson.
Great article as usual, Dr. Jayne… this is one of the objectives I’m a little hazy on… does any one have a list of what is considered a “syndromic event”?
I have to disagree with you on the CHCIO Certification. This is a certification that measures whether a CIO has the appropriate knowledge they need to be able to address the vast amount of issues encountered on a daily basis – such as regulations, professional ethics/behaviors, ethics, patient rights, IT governance, data management and controls, strategic planning, organizational culture, technology planning, IT Department operations etc…. This exam is constantly being kept up to date to align with current trends and regulations. You would be surprised on how many “highly educated” CIOs there are out there that don’t have a clue about aligning the IT vision with the organizational vision or how to successfully create and maintain internal and external vendor/physician/stakeholder relationships. I believe the fear of failure is probably more of a deterrent to CIO’s than a possible opinion that the exam is unworthy.
[From Mr. HIStalk] Considering that taking the exam requires three years of CIO experience, it would be a sad statement about a hospital’s competence if their CIO failed (or if a CIO even felt the need to prove their capabilities by passing a multiple choice exam). You would think if a hospital was going to pay several hundred thousand dollars a year to lead one of the smallest areas of the hospital that they would at least be able to judge the competence of a candidate without having to test them. I don’t think C-level certifications are common, although I could be wrong about that.
Dr Jayne, I think LOINC codes, not CPT’s, will be the key to the future for reporting to Public Health agencies.
RE: St. John’s Regional Medical Center (MO) may not be salvageable, according to hospital’s president Gary Pulsipher.
This has been a very sad story to listen to indeed. Early on, I heard that some residents in the affected area had found Xrays scattered about from the Hospital(s). First thing I thought, of course, was “breach” and that made me wonder about how something like this could be avoided. I wouldn’t want my Xray flying around town, but then again, it’s certainly not intentional. Can you check with your expert gurus on this and enlighten me?
Thanks!
Specialty Provider EHR Land: I agree wholeheartedly. When I was trying to get information about our state’s immunization registry or the availability of any agencies to receive surveillance data, all I heard was crickets. Half the people I was transferred to at various agencies didn’t know what I was talking about. We even debated reporting to another state because they were willing and cooperative.
HIT Worker: There is also no code for alien abduction – I’ve got to think with the prevalence of that condition that maybe there would be one.
Blah: I absolitely LOVE the E-codes. We used to play a game with them in Residency to stay awake on call – some of them are just insane.
Just showed that AMA coding app to my docs last week and we had a good laugh. Of all the useless apps out there…at least it was free. I can’t even hold a docs attention for 3 minutes to give them a coding tip (and I try to keep it light and even funny). This app takes at least 5 minutes to navigate to a code, and you still have to know what ‘expanded problem focused’ is. Um hello AMA? I have coders who still need cheat sheets for this-docs still don’t get it, 15 years after CMS started their rules.