I was born roughly 2 months after the US space program began (Explorer 1), and I've followed it all my…
News 11/4/09
From The PACS Designer: “Re: Windows 7. Microsoft has released a 90-day trial copy of Windows 7 for IT professionals to use in testing Windows 7.”
From Charles Chips: “Re: road rage story. The doctor was found guilty on all counts.” Thanks for the link. After some soul-searching, I’m going to pass on running specifics even though I said I would once the jury had reached a verdict. The person’s in enough trouble already (looking at up to 10 years in jail) without having the details trumpeted to the industry just because their employer is an HIT vendor and just because I happen to know that. I’m a Golden Rule kind of guy, so I’ll sleep better knowing that, right or wrong, I didn’t go against my conscience. You can probably Google it.
This moment brought to you by Weird News Andy: “Snoring less improves your golf game. Yes, a bit late except for those in Florida, but remember it for the spring.” Another reason to seek treatment for sleep apnea — the handicap of golfers studied improved by three strokes. I like that the UK newspaper, obviously scratching their heads at not having a photo of a CPAP-wearing golfer on the links, stuck in an unrelated picture of Barack Obama holding a golf club.
Ingenix Consulting names John Nackel as CEO, replacing Ted Chien.
Thanks to the reader who sent over the six best practices for medication administration from CALNOC, which dramatically reduced errors in several large hospitals. They are simple: (a) check the medical record against the med; (b) don’t get distracted; (c) leave the label on the med until it’s given; (d) use to methods of patient identification and explain the med to the patient; (e) chart the med immediately after giving it; and (f) check the Five Rights. Bedside bar code verification isn’t on the list. I supposed you have to assume that if these steps reduced errors, they weren’t doing them before, but it’s not much of a magic bullet for those looking for one.
eHealthOntario issued another $236 million in contacts after CEO Sarah Kramer resigned in July over excessive consulting expenses. A political opponent is outraged that the government made no announcement about the new agreements, saying “It’s very ominous that at the height of the controversy around the billion-dollar boondoggle at eHealth, the government slipped another $236 million out the door.”
MD Buyline jumps on the ARRA EHR bandwagon, offering an odd lot of services (a glossary, a list of Web links, customer survey results, etc.) Maybe their services have improved since I was pressured to subscribe to them years ago.
The Advisory Board Company reports Q2 results: revenue up 1.2%, EPS -$0.14 vs. $0.32, but a lot of that loss was one-time write-offs. Shares that were in the high 60s three years ago are at $25.45 now, dropping the market cap to around $400 million. None of the executives are big holders, with even the president holding only around $350K worth.
A guest editorial in a Toronto newspaper says the Canadian government’s H1N1 vaccination rollout “looks like rush hour at a Mexican bus terminal” (I’m a bit uncomfortable with that choice of words). It lauds, however, a clinic that used its scheduling system to book vaccinations and its EMR to verify that recipients were high risk, resulting in no patient waiting. It summarizes, “If there were a Group Health Centre in every Canadian community, the H1N1 vaccination campaign wouldn’t make us look like a Third World country. We need more effective primary health care in Canada and we need to seamlessly link primary health care to public health.” Don’t we all.
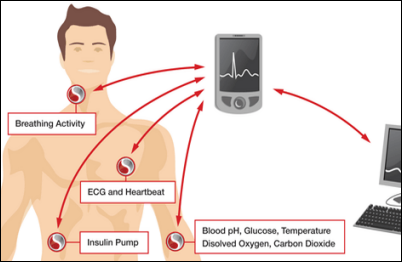
London hospitals are testing a “digital patch” that allows wireless patient monitoring, with information being downloadable into a smart phone or integrated directly into EMRs. Toumaz Technology, which makes the Toumaz Sensium, says its on-board chip extracts critical information and not just raw data, working over low-power radio.
Here’s a fun blog post complaining about EMRs from the perspective of a family practice doc who can’t get information about his or her ED patients. What’s notable: the gripes (“The Emergency Department EMR from Hell”) apparently involve Epic (it’s too detailed to summarize). I really liked this comment from an anonymous reader of that site, though:
“Medicine is often compared unfavorably to the airline industry in its failure to use checklists to avoid mistakes. Well, I’m pretty sure there’s no checklist that requires a pilot during take-off to go into the cabin and ask who ordered the fruit plate. But the forces that run modern medicine (including our professional societies) feel that there is no administrative task too trivial that it should not be allowed to interfere with the doctor’s interaction with his patients. This trend is only exacerbated by making an EMR the focus of the physician’s concentration. Basic point: anything that reduces the time and mental energy a physician has to bring to direct, one-on-one patient contact is BAD.”
From accidental Googling, I see that Sharon Howard, formerly of Sage, is now VP of marketing at RelayHealth.
I editorialize on PR-fueled H1N1 data reporting in my guest editorial at Inside Healthcare Computing this week. I must have had too much soda since I sound manic: “Just be aware that people exaggerate their own illness for maximal sympathy or as justification for skipping work, so any kind of sniffles or tiredness will convince people to say they have H1N1 because they heard about it on Oprah (‘headaches’ become ‘migraines’, ‘a cold’ becomes ‘the flu’, and ‘getting sick from too much Super Bowl beer, wings, and guacamole’ becomes ‘food poisoning’).”
I see HHS got a few EMR comments on its site, some of which are good. Here’s a snip of one I agreed with as a contrarian: “The fictional scenario of showing up unconscious at some distant medical center, alone and without ID and contact information, and needing instant treatment that solely depends on an EHR (not on physician judgment) is so rare as to be nil.” Most medical care is delivered near the homes of patients, so it would be a stretch to justify spending a lot of interoperability money to avoid the oft-told “unconscious in a Florida ED on vacation alone and avoided a penicillin allergic reaction” fable that happens, but rarely.
In England, three thumb drives are lost that contained information on 76 cancer patients, stored in unsecured Word documents.
Odd lawsuit: a woman sues her former lover, the married head of the OB-GYN department of Greenwich Hospital, claiming the doctor used the OR for their trysts, told her to get Hepatitis C vaccine afterward, and illegally injected her with Botox. He says she’s out to get him after he dumped her at his wife’s insistence, saying the former mistress posted Internet comments under his wife’s name that called him “a pervert”.
John Fontanetta MD, CMO of ED systems vendor EDIMS and a practicing ED physician, is named a Top Emergency Doc in a survey by New Jersey Monthly Magazine.
A psychiatry magazine says stimulus dollars won’t encourage psychiatrists to buy EMRs because the Meaningful Use criteria will be aimed at generalists controlling chronic physical disease. A New York state mental health official says quality indicators exist for psychiatry if HHS really wanted to use them to define Meaningful Use for that specialty. He also pointed out that hospitals look harder for physical conditions whose treatment generates revenue, which has encouraged vendors to focus on the broader market.
Fletcher-Flora announces GA of its lab outreach portal.
Jeff Arnold, a founder of WebMD, launches Sharecare.com, which features expert advice from “celebrity physicians”, big-name hospitals, and “Knowledge Partners”, advertisers who provide answers marked as sponsored comments. Oprah is a backer.
HERtalk by Inga
From DragonGuy: “Re: conversations meeting. Had a great Dragon conference in Vegas last week. Dragon 10.5 will (we all hope) partially solve the ‘Citrix issue’. The room was mostly filled with Epic-based hospital IT people wanting to improve the experience for their docs: Kaiser, Cleveland Clinic, and similar.”
Drummond Group, which provides interoperability/performance testing and certification, announces that it will apply to become an EHR certifying body once ONC releases its requirements. I think mixing things up a bit and giving CCHIT some competition isn’t a bad thing. Of course the introduction of choice is bound to lead to strife, with certifying bodies and their constituents each claiming superiority. Perhaps competition will reduce certification fees, which would be especially appealing to smaller vendors. Now that Drummond has announced its intentions, will other entities step forward as well? Could be fun to see what unfolds.
Perot Systems is now Dell Services Global Business Unit, following Dell’s purchase of 90% of Perot’s outstanding shares. Perot CEO Peter Altabef was named president of the division.
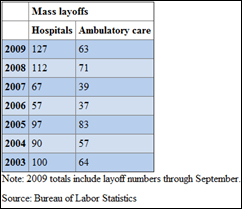
Hospital have had a total of 126 mass layoffs (50 or more employees) through the end of September, which exceeds the 112 layoffs for all of 2008.
dbMotion opens a regional office in Singapore to address the growing demand for EHR solutions in Asia-Pacific.
Mediware reports a 184% increase in earnings over last year, and a 9% jump in revenue. Shares climbed 15% based on its better-than-expected numbers.
West Penn Allegheny Health (PA) makes plans for a new medical school, as well as an overhaul of its 700 member physician practice group. Despite a $34.6 million loss for the nine-month period ending March 31, West Penn is investing big money in EMRs for its physician offices.
McAllen, Texas once again makes healthcare headlines. The area’s largest hospital system agrees to pay the federal government $27.5 million to settle allegations that it paid doctors illegal kickbacks to refer patients to its facilities. The government claims that South Texas Health Systems disguised payments to doctors in a series of sham contracts that included medical directorships and lease agreements.
St. Rose Hospital (CA) deploys Horizon Cardiology CVIS from McKesson. Meanwhile, Crittenton Hospital (MI) selects McKesson’s Horizon Enterprise Revenue Management solution.
The seven-physician Toledo Orthopaedic Surgeons group selects SRS EMR.
HHS says it’s taking HIPAA violations seriously, imposing significantly stiffer penalties for HIPAA breaches. The maximum penalty for a civil violation jumps from a mere $100 to a hefty $25,000 fine. The penalty cap was also raised from $25,000 to a whopping $1.5 million.
Following what seems to be low-tech techniques, VHA helps 28 hospitals in Oklahoma and Arkansas improve ER traffic. Most of the EDs made significant reductions in wait times and LWBS rates, despite increases in patient volumes. I was surprised that VHA did not attribute the improvements to some new HIT tool. Instead, old-fashioned internal competition and communication were the main forces at work. One VHA official says, “The real driver for improvement for these hospitals is not comparing themselves to national standards, but with each other. Once a hospital administrator sees that another hospital has achieved success, he or she picks up the phone and asks how.” Now that’s innovative.
Bermuda’s primary hospital and urgent care center are getting rid of paper processes and installing MEDHOST’s EDIS.
CareTech Solutions reaches an agreement to acquire IGCN, which helps hospitals build and manage Web sites.
Moses Taylor Hospital selects ClaimTrust’s InSight Denials to track and analyze claims.
Cortland Regional Medical Center (NY) contracts for ProVation Order Sets to automate evidence-based order sets.








RE: complaining about EMRs from the perspective of a family practice doc who can’t get information about his or her ED patients:
This doctor drones on and has pretty good command of the F-word, but doesn’t seem to have particularly good command of the facts.
This typifies the national problem.
How many people have to die to convenience doctors in this country?
And by the way, doctors do get to see Nurses Notes, Triage Notes and all the history they can take the time to review in the ED. A heck of a lot more access to information than they’ve ever had before.
“unconscious in a Florida ED on vacation alone and avoided a penicillin allergic reaction” fable that happens, but rarely”
I guess we as a society could legally put the burden where it belongs and make it the responsibility of individuals to always wear notification of any medically significant allergies and conditions (remember the medicalert bracelets?) and eliminate the entire issue.
I saw several comments yesterday on a Modern Healthcare article regarding EHRs. The gist was that it would be smarter to let HHS and/or some ‘commission’ standardize medical terminology and to also develop a baseline EHR model – much like they have done with the Medicaid Management Information System for claims processing. Yes, I am very aware of the Vista fad and spent time looking at it’s limitations but, to get past the issues of interoperatibility, standardization, etc. this idea has merits – would be interesting to see what the vendor banditos on this site think of this – recognizing that they would still have a dog in the fight but would have something more substantive than the meaningful use crock to build to.
“Most medical care is delivered near the homes of patients”
Obviously true for routine medical care, but is it true for emergency care? Urban areas yes, but I just took an extended road trip through rural small-town America. Serious emergency care – stroke, heart attack, trauma – where you’re likely to be unconscious or otherwise unhelpful in providing allergy info – can be 100 or more miles from home.
In response to being unconscious in Florida alone:
My reaction to this is the in Florida ED and has a penn allergy is rare but the not so rare cases are someone in a car accident locally but does not have their driver’s license (we’ve all done it) and needs medical attention or EMS arrives at their home and their condition doesn’t allow for information exchange. To ask EMS to search the house for relevant info in a time sensitive scenario is not reasonable. Also Doctor’s need information to make informed judgments and decisions.
Even if we solve it locally and not necessarily nationally or globally we win for patient safety. The cost of the service should NOT be a factor….this is healthcare – isn’t that why we need reform?
re. Not running with the details or link on the road rage doc.
Nowww that’s not really fair is it? I remember a few years back a MEDITECH hottie was convicted of trying to run down a cop directing traffic because she was late for work. That got covered…
[From Mr. HIStalk] I know I’m walking a fine and possible indefensible line, but Meditech’s name was prominently mentioned in all the Anna Gitlin news reports and she was on her way to work when she tried to run the police officer down, so everybody knew the connection. In this current example, the mainstream article didn’t mention the employer (I figured it out from the name, location, and the license plate) and the person involved wasn’t doing anything work related. And, this person is an executive, so it puts the employer more on the spot than when it was a software engineer.
The HHS EMR site snippet you mentioned seems to have been censored, so here it is in its entirety:
… The need for standards seems to be oriented towards a medical system where patients are moved around from doctor to doctor against their will, as in – socialized medicine.
When patients move themselves voluntarily, they can bring their records with them on paper, and a new practitioner can backload what they need into the new EHR.
The fictional scenario of showing up unconscious at some distant medical center, alone and without ID and contact information, and needing instant treatment that solely depends on an EHR (not on physician judgment) is so rare as to be nil.
In summary, there is no substantial benefit to patients of “standards”, only to payers and government regulators. It would be a lot cheaper to deliver paper records by FedEx than build a “national interoperable health IT system” at a cost of tens or hundreds of billions of dollars. Give that money to the poor so they can get care.
Elimination of the $$$ spent on all this would also allow hospitals to counterbalance medicare cuts.
[From Mr. HIStalk] It appears that HHS removed this comment (and several others) for unknown reasons. If you hover over the comment date, the comment number displays. Several numbers are missing, presumably meaning they were removed.
“Tired of Complainers Says: How many people have to die to convenience doctors in this country?”
Considering the hostile environment most doctors now struggle in, that is an outrageous and entirely inappropriate accusation. And you are actually working in healthcare? What “conveniences” do you purport to be killing patients? Perhaps rejection of poorly designed EHR’s that distract and make doctors even more miserable?
“Suffering Seminole says: someone in a car accident locally but does not have their driver’s license (we’ve all done it) and needs medical attention”
Well if they have no I.D. on them, then EHR’s are useless, are they not? And doctors are pretty darn good at handling the emergency aspects of trauma cases without needing to know that John Doe has a penicillin allergy or a history of cardiac problems…
“or EMS arrives at their home and their condition doesn’t allow for information exchange.”
Again, stabilizing a patient in a home emergency does not require an interoperable EMR that costs tens of billions and deprives the needy of care, just well trained clinical personnel who know what they are doing.
“[From Mr. HIStalk] It appears that HHS removed this comment (and several others) for unknown reasons.”
The reasons are pretty O-O-O-O-O-bvious.
Re: the “fun blog post”, here was another comment with a different perspective from the one you chose to quote:
“Um.. we use epic at my current hospital and you can actually make changes (our IT dept does it all the time), and there are ways to send notes prior to doing the discharge instructions, and I can see any notes or any other info entered by any person taking care of the patients….it’s actually a cool EMR system, I think. I like it.
Unless the hospital got some sort of cheesy Epic knock-off… maybe made in China with the lead that they can’t put in childrens’ toothpaste any more?”
Re: Win 7
I’m running it right now on a spare machine, a lowly Celeron 351-based machine with 1.5 Gb of RAM and an ancient ATI card. It runs quite well, the user experience is refined and well thought out, and makes the computer a pleasure to use.
Of course, it took many years to arrive at this level of user experience. Now, if only the major health IT vendors would get to work on doing the same thing with their applications.
And by the way, to the person who asked how many people have to die to convenience doctors in this country, perhaps you would prefer physicians do this: http://www.philly.com/inquirer/home_top_left_story/20091104_Nutter__Rendell_blast_SEPTA_union_for_surprise_strike.html
Early in my career as medical programs manager for this transit authority, I observed this labor union, TWU234, in action.
I didn’t like them, then, but have grown to rather admire their take-no-bullshit approach to defending their members’ interest.
— SS
Ladies and Gents, I worked for a suspiciously similar company on their ER software and I can say for a fact that in January 09 a request for this was pushed through yet again and a CO was put together that cost roughly 10k. It was 5 lines of code in the ADT module. Nobody would pay for it and without that CO money coming through we weren’t allowed to push a much needed change into place. This physician has every right to complain, if you already have the data how idiotic is it to keep having to re-enter? Physicians count clicks let alone having this on their plates, we should be forcing the software companies to stop trying to bleed their patients dry.
The fictional scenario of showing up unconscious at some distant medical center
It’s not that, it’s the 80yo showing up at the ED with an adverse drug reaction and they ask her what meds she’s on and she goes “Um… little pink ones, an orange one and a purple one.”
“It’s not that, it’s the 80yo showing up at the ED with an adverse drug reaction and they ask her what meds she’s on”
They treat the symptoms, fluids/pressors/diuretics or whatever is needed then they can ask her what drug store she goes to.
Lots cheaper than spending tens of billions on interoperable EMR no?
“Lots cheaper than spending tens of billions on interoperable EMR no?”
Um.. no. When your spending trillions on anything it might make sense to spend 1% of that on keeping track of what you’re doing.
Healthcare spends the lowest percentage of revenue on IT of any industry. It is also, along with education, the most inefficient. Indeed, both industries are inefficient for the same reason – they are unwilling to leverage technology to increase efficiency and improve productivity.