RE the AI GLP1 company, Washington Post has an article today by someone who used one of those compounded products,…
Readers Write 11/2/09
Submit your article of up to 500 words in length, subject to editing for clarity and brevity (please note: I run only original articles that have not appeared on any Web site or in any publication and I can’t use anything that looks like a commercial pitch). I’ll use a phony name for you unless you tell me otherwise. Thanks for sharing!
Web Services, A Real-World Example
By Mark Moffitt and Kevin Hornberger
In this article, we will give an example of the use of a “transactional” Web service to request and return clinical data.
GSMC processes about 90,000 patients per year, 1,700 per week, or 250 per day in our Emergency Department (ED). ED physicians at GSMC use MEDHOST to record each patient visit. MEDHOST is a “best-of-breed” ED application. MEDHOST is interfaced to our hospital information system (HIS), Meditech Magic, using HL-7. Meditech and MEDHOST stay in sync by way of HL-7 data transfers. In this example, think of Meditech as our HIS and clinical data repository (CDR).
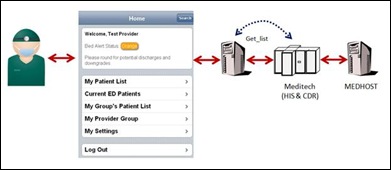
GSMC developed an iPhone web application that physicians use to view clinical data. GSMC ED physicians wanted to use this application to pull up a list of patients assigned to them. Then, they can access clinical data like lab and radiology (audio dictation) on the iPhone. This information (list of patients) is not included in the HL-7 messages sent from MEDHOST to Meditech.
We could modify the HL-7 transaction from MEDHOST to Meditech to include this field. The GSMC iPhone app would then query Meditech (CDR) to get a list or patients associated with an ED physician. This effort would require modifications to MEDHOST and Meditech to process and store this data. See Figure 1.
An alternative approach is to keep the data in MEDHOST (source) and get it using a Web service when needed. See Figure 2. The advantage to this approach is:
- Only one copy of data exists.
- Implementing a Web service is easier than having multiple vendors modify an HL-7 message.
- It is easier to maintain – the Web service only needs updating when changes are made to the underlying MEDHOST database.
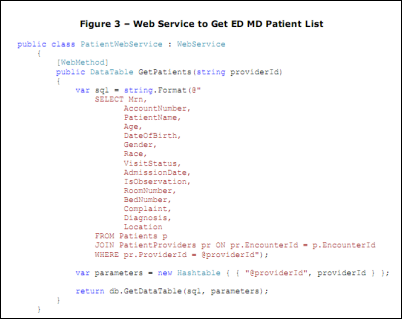
GSMC uses a Web service developed internally using XML over HTTP. The Web service receives a physician identifier, constructs an SQL message and queries the MEDHOST database, and returns the result in a Web service. See Figure 3. The return message contains a list of patients assigned to a specific ED physician. Figure 4 is a return message (with patient identification altered to keep confidential).
Most CDRs in operation today perform two functions: 1) provide easy access to data spread across multiple systems, and 2) serve as a data store for analytics and decision support.
It is fairly easy to construct a Web service to get data from different systems. Web services with direct access to data sources eliminate the need for a CDR with respect to providing easy access to data spread across multiple systems.
New technologies in the business intelligence (BI) space may eliminate the need for a CDR for analytics and decision support. I will be writing about this topic in my next article.
I acknowledge that this is a simple example of the power of Web services. To take Web services to the next level, aka a Service-Oriented Architecture (SOA), you need interoperability and other features. Interoperability, unlike the example above, requires cooperation and coordination from vendors, something not always easy to obtain. MEDHOST is working further on its web services to provide a full SOA.
Figure 2
Figure 3
Figure 4
Mark Moffitt is CIO and Kevin Hornberger is a senior software developer at Good Shepherd Medical Center in Longview, TX.
Strategic IT Investments in the Operating Room: Why Now is The Time
By Kermit Randa, FACHE, CPHIMS
 By now it’s obvious that the current economic downturn has not spared hospital organizations. With capital markets inaccessible to many hospitals, the financing for major investments and physical plant expansion is suddenly unavailable. Additionally, income from hospital endowments, which is often dependent on equity investments, has been dramatically reduced. The recently passed economic stimulus for healthcare and especially the $19 billion for adoption of an electronic health record may offer hospitals some funding relief in the long term, but initial funding for hospitals will not begin until 4th quarter 2010. In addition, the regulations for determining funding and eligibility are still being debated and finalized.
By now it’s obvious that the current economic downturn has not spared hospital organizations. With capital markets inaccessible to many hospitals, the financing for major investments and physical plant expansion is suddenly unavailable. Additionally, income from hospital endowments, which is often dependent on equity investments, has been dramatically reduced. The recently passed economic stimulus for healthcare and especially the $19 billion for adoption of an electronic health record may offer hospitals some funding relief in the long term, but initial funding for hospitals will not begin until 4th quarter 2010. In addition, the regulations for determining funding and eligibility are still being debated and finalized.
Long-term assistance may be on the way, yet demands on hospitals remain high for now and the foreseeable future. These demands include the need to maintain a high level of quality, operate ever more efficiently, continue with patient safety initiatives, comply with regulatory requirements and attract and retain talented clinicians. Certainly, this is not a time for “business as usual” and it offers a real opportunity for renewed leadership, strategic vision and action.
The traditional response to tough economic conditions is to put current project expenditures on hold or to implement an “across-the-board” belt-tightening budget process (“Every department needs to reduce their expenditures by 10%”). This latter approach, while appearing straight forward and fair, may have unintended consequences. But where can an organization begin to effectively navigate through these unprecedented times?
One sound approach involves a back-to-basics look at the economic underpinnings of hospital organizations and the importance of the hospital operating room (OR). According to recent HFMA studies, today’s OR is the economic engine of most hospitals – accounting for up to 60% of a hospital’s revenue and some 35%-40% of the hospital’s expense. Over 60% of the hospital’s margin typically comes from surgical patients. Based on data from DJ Sullivan Healthcare Consulting’s database of 700+ ORs, each empty but open OR suite costs a hospital an estimated average of $1,000 per hour (including pre/post op staffing and anesthesiology costs). The OR is also a primary source of up to 50% of hospital-based errors. The impact of the OR is felt well beyond the perioperative department, according to the AHA’s Quality Center, “Because the OR is a primary source of admissions, it is virtually impossible to streamline hospital-wide flow without first streamlining patient flow through the OR”.
Optimizing the performance of the perioperative department can significantly improve performance of both the perioperative department and the hospital. Through the use of new perioperative information systems coupled with improved work flow processes, hospitals can expect the following improvements in their OR:
- More accurate scheduling resulting in a more rational schedule
- Increased on-time case starts due to an effective pre-surgical screening and documentation process
- Improved quality of care and patient experience by reducing redundant data collection through an integrated digital record
- Reduced supply costs by using preference cards automatically maintained on actual usage, not “what was used last time”
- Documented cost-per-case averages to offer greater access to surgeons with higher margin case mixes
- Generated comparable metrics showing cost-per-case by surgeon by procedure so that standardization decisions can be made based on full information and not just purchasing data
- Published empirical performance outcomes to demonstrate quality and efficiency to other surgeons and the community using analytics and business intelligence tools
- Web access to create a path of least resistance for surgeons and their offices
- Consistent and predictable surgical days for which everyone can plan
- Integrated Anesthesia record driving increased efficiency, charge capture, and safety
To enable hospitals to make a perioperative IT investments now, some healthcare IT vendors have already announced special subscription pricing models that enable hospitals to fund such initiatives from operating budgets rather than capital budgets that may be currently on hold. Hospitals can begin these projects now, spreading payments over a longer time horizon, realizing a positive ROI more quickly.
Surgeon and OR Staff Recruitment and Retention
Another strategic consideration for moving forward with an investment in perioperative IT is that it can be a powerful motivator in attracting talented surgeons, residents, and OR clinicians.
According to James Pennington, Chief Information Officer, JPS Health Network, located in Ft. Worth, Texas, “Our hospital has long been a preferred institution for incoming residents due to its diverse levels of patient acuity, service lines and our use of advanced technology. We recognize that top new residents understand the benefits of advanced IT solutions in the provision of care and expect them to be available”.
One way to increase OR revenue is to attract surgeons with high volume practices from competing hospitals.
The Centers for Medicare and Medicaid Services (CMS) reports that the average surgeon reimbursement from Medicare has decreased by some 7% over the last three years, resulting in surgeons seeking hospitals that can demonstrate efficiencies that will enable them to maximize volume and revenue for themselves and consequently the hospital. I believe that if the following key considerations are met, surgeons will be willing to consider moving their OR schedule to a different provider if:
- Surgeons’ referral patterns are not disrupted
- Surgeons can perform at least one more procedure daily
- They see an improvement in lifestyle (earlier leave times, reduced extended hours)
- They have regular access to OR time using an easy, repeatable process (e.g. guaranteed block times)
- The OR documents high satisfaction ratings from patients and staff
The use of a robust information system that is well integrated into the workflow of a perioperative department can be a key underpinning in recruiting (and retaining) talented surgeons and other perioperative staff.
Conclusion
This is a time for leadership. Recognizing the perioperative department as the economic engine of the hospital offers many opportunities for change that can result in quick economic wins. Prioritizing this area to ensure the ability to gain and maintain economic advantage is a critical step. A robust perioperative system is one of many improvements that can be made relatively quickly with significant and early ROI payback. The strategic long-term benefits can be even more significant. While such investments may seem counterintuitive in challenging economic times, they can in fact result in both tactical and strategic advantages that will lead to financial success for the organization.
To take on this initiative, support from senior management is essential. It requires focus, team work, leadership, and the final key ingredient – courage.
Kermit Randa is Senior Vice President, Surgical Information Systems.




Informative articles by all authors tonight..thanks
You should headline the Randa article, as with others like it, as ADVERTISEMENT.
Secondly as a former CFO, this statement is Grossly inaccurate:
‘ accounting for up to 60% of a hospital’s revenue and some 35%-40% of the hospital’s expense’
No way is OR 60% of hosp revenue. If that’s the case then 40% is medical…so what!
Please either stop the hidden adds, or label them as such.
I know I am nit-picking, but please, there is no such thing as “HL-7”, it is simply HL7…
Kermit,
Nice Ad. Well done!