The UHC hiding the breach notice page is one thing but it looks like Nebraska is suing Change Healthcare for…
News 9/11/09
From Chi Lover: “Re: Eclipsys. Eclipsys is having another round of layoffs today (9/10/09). How can they sustain their implementations with so few staff?” Unverified. Another rumor making the rounds is that Allscripts is thinking about buying Eclipsys, but I mention that purely for entertainment rather than business value since lots of signs point to the likely inaccuracy of that speculation.
From Bobby Orr: “Re: Cerner. I’m disappointed in your thoughts that Neal would do anything that is not motivated by money. Cerner would compile a massive database of patients that could de-identified and sold to the pharma companies for research, trending, etc. Go with the cynical version because it is great business idea that big pharma would be willing to pay big dollars for. The stock is not blowing everyone out of the water because Neal has bad business ideas.” You’re probably right, especially with all the non-proprietary ways the government could get surveillance data (I let my cynicism down for one moment and got busted!) One reader commented on the article, asking how Cerner would deduce H1N1 given that there’s no ICD-9 code for it; another replied that they would simply be looking at ED admissions in which the patient has a temperature that’s a certain amount above normal. If that’s all it does, then it’s worthless.
From Who Pays For EHRs? Patients: “Re: Cerner. People might have forgotten that Cerner already is selling patient data to pharma and there really isn’t any such thing as anonymized data. I guess no one is buying Cerner, so they need to do something.”
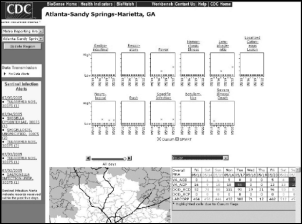
From Sr Health Integration Tech: “Re: Cerner’s H1N1 surveillance tool. I believe the CDC already has the capability, known as BioSense. It takes HL7 messages, which are made anonymous prior to transmission, and the aggregated data is analyzed for the region to determine if a ‘biological incident’ exists.” That brings back a memory that UPMC had developed a biosurveillance tool for the CDC or NIH years ago (I remember downloading it). I don’t know if it’s the same one.
From Cal Worthington: “Re: HIEs exchanging data. From what I’ve seen at many of the state-wide HIE conferences being put together to respond to the HITECH act, only the PhD/MDs are salivating over the HIE to HIE exchange because of the research they are doing. Most are professing my patient imperative, ‘the closer to the patient the faster the information is needed’ — which I believe cannot be done in a cost-effective way as you get farther and farther away from the patient’s home turf. However, I do believe that certain CMS, CDC, SSA, and research data could be exchanged in that manner, making reporting a behind-the-scenes activity to healthcare delivery. Once that happens, we’ll get better data without the administrative overhead. HIEs are effective collaboration tools in a community of healthcare providers with significant overlapping patient populations.”
From Mike Mills: “Re: iPhone emergency apps. I bike a lot, so I bought the Road ID, a wrist bracelet with my wife’s name and number and an 800 number and PIN. The system ‘talks’ to the EMT and tells them my name, blood type, any medical conditions, meds I am on, allergies, etc. That is much better and easier than a phone app, easier to find, and they make one version of the wrist band that is nice looking so you can wear it all the time.” Pretty cool for $9.99 a year. EMTs call the phone number or go to the Web page on the bracelet and a text-to-speech app reads off the information.
From Colorado Kid: “Re: Steve Hess. He left Christiana Care and joined the University of Colorado Hospital as CIO.” Thanks to the several readers who passed that info along. I feel like John Walsh for tracking him down publicly.
From The PACS Designer: “Re: wait times. As we digitize more health information, we start to see more innovations migrate to the Web. Middlesex Hospital (CT) is one institution that is going digital in their Emergency Department when it comes to posting wait times on the web for treatments which exclude real emergency situations.”
dbMotion, Allscripts, and Initiate Systems will host a Healthcare IT Executive Summit later this month in San Francisco. The topic is, of course, ARRA, which has dislodged every other topic from every HIT event (maybe HIMSS will be nothing but people talking about Meaningful Use and getting government money). It’s invitation-only, so if you didn’t get one, join the club.
Readers have added quite a few events to the HIStalk Calendar in the last few days, so check them out or add your own events for free (I keep saying “for free” since I don’t think everyone has caught on).
Listening: brand new from Phish, who shows they’re more than spaced-out live jammers. Lots of little 70s prog bits in there. Meanwhile, the music industry’s only possible savior is a group whose last album was recorded in primitive tape equipment nearly 40 years ago, the 50%-still-alive Beatles. Quality really does last, apparently.
Midwest Orthopaedics chooses SRS after taking its free EMR free trial.
Dell gets into the PM/EMR business, offering a sponsored solution to hospital-affiliated doctor groups that can include hosting, HIE services, a monthly lease payment, onsite services such as practice and workflow assessments, and 24×7 hardware and software support. Tufts and Memorial Hermann were early adopters. Partners include eClinicalWorks and Perot. That’s bigger news than the Sam’s Club announcement, I think, since Dell is offering everything for one monthly payment and practices need a lot of support. We’ll have our interview with Bill Shickolovich, CIO at Tufts-New England Medical Center, posted shortly.
The Dell story made The New York Times, which dug deeper to see what other vendors are doing. GE will roll out a hosted version of its systems in a few months, eClinicalWorks has 10 data centers for hosting, athenahealth will announce a marketing drive and technical assistance program within the next three weeks, IBM is creating a cloud-based service for EMRs, and Verizon started a 500-employee healthcare unit that will offer hosting and data sharing.
Construction will start soon in Wyandotte County, KS on an 18,500-seat soccer stadium and a 4,000-employee Cerner office park with 600,00 square feet of office space. The $414 million project, funded by bond money, covers the two organizations that Neal Patterson and Cliff Illig own most of — Cerner and the pro soccer team there. Not shown: the pizza delivery man observation platform atop the giant ticking clock.
The CRIMSON Initiative, a physician profiling system sold oddly enough by The Advisory Board Company who bought the company last year, announces that it’s being used by over 200 hospitals. One hospital CEO is quoted strangely: “If I had the ear of President Obama, I would tell him that we need two things, a national fishing holiday and the CRIMSON application.” He also calls it “a diamond in the rough,” implying there’s something “rough” about it.
The Physicians’ Drug Reference (PDR) is merging with the Health Care Notification Network to form PDR Network, offering the online drug reference and FDA provider alerts. A reader reported in May that something was up with Medfusion and Medem, Medfusion bought Medem’s health services business in July, and former Medem CEO Ed Fotsch is now listed as CEO of the new PDR Network.
The cost to McKesson to provide security to John Hammergren: $402K per year, the fifth-highest cost in the Fortune 100, way more than the cost of protecting the CEOs of ExxonMobil and the car companies.
Rockingham Memorial Hospital (VA) chooses NextGen’s PM, EMR, imaging, and community health solutions.
I missed this: Medicity CEO Kipp Lassetter, MD spoke Wednesday at the Robert W. Baird Health Care Conference.
Who believes this? Delnor Hospital (IL) says it hasn’t had a medication error in 15 months. I guarantee I could snoop around for an hour and find several, although maybe they really meant medication-related sentinel events.
Halo Monitoring announces that its home monitoring and personal alert system can send data to Microsoft’s HealthVault.
Informatics Corporation of America brings on three new regional sales directors for its ICA CareAlign data sharing and portal solution.
The State of Kentucky opens registration for its e-Health Summit, which is Wednesday at the Hyatt in Louisville. John Glaser is on the agenda (warning: PDF) representing ONCHIT.
GE Healthcare announces its plan to develop wireless monitoring systems it calls Body Sensor Networks, replacing hard-wired medical monitors with wireless versions that could be used anywhere in a hospital or at home. The company has also petitioned the FCC to create a dedicated frequency band for low-power, short-range monitoring systems. That sounds like a great alternative to moving patients around in the hospital just to get them to a monitor-covered location.
Insurance company WellPoint apparently has cleaned up its much-publicized software glitches that nearly drove the company out of business, receiving notice from CMS this week that it can resume selling its Medicare insurance plans.
Mediware announces Q4 numbers: revenue up 4.3%, EPS $0.07 vs. $0.04.
HERtalk by Inga
Fall River Health Services (SD) alerts patients they are converting to Meditech Client Server EMR this week, a change that will allow them to connect with Rapid City Regional Hospital.
The DoD signs a contract with CliniComp to deploy its Essentris inpatient clinical documentation package at 36 additional military treatment facilities.
West Park Healthcare Centre (Toronto), Northeast Georgia Health Systems, and Hunterdon Medical Center (NJ) are awarded 2009 QuadraMed User Excellence in Software Technology awards. The award recognizes success in maximizing operational efficiencies and delivering high quality through QuadraMed technologies.
Weeks after MetroSouth Medical Center hosts a first year anniversary barbecue, the Blue Island, IL hospital lays off 120 employees. Just a month ago the Chicago Tribune reported things were looking up at the former St. Francis Hospital & Health Center. Now administrators are blaming the decline in patients for creating additional financial pressures.







Re: ……….Delnor Hospital (IL) says it hasn’t had a medication error in 15 months………..
The weblink article refers to OB discharges, not medication errors.