HIStalk Interviews Michael Rothman, Co-Founder, Rothman Healthcare Corporation
Michael Rothman, PhD is co-founder, chief science officer, and board chair of Rothman Healthcare Corporation of San Francisco, CA.

Tell me about yourself and about Rothman Healthcare.
I have a PhD in chemistry. I’ve been doing data analysis for 30 years. I spent a good chunk of that time working for IBM, including a stint at IBM Watson Research Lab. I then went off and did consulting for a while.
The reason that I got involved in this whole thing is a personal one. My mother was a patient at Sarasota Memorial Hospital. She went in to have a valve replacement operation. She did well initially, and then started fading. The problem is that no one understood that she was getting sicker until she was very ill. Without going into the whole story, she ended up dying about a week and a half later.
My brother and I spent a long time trying to understand what had gone wrong. What we decided was that, in a way, the system had failed her. It really is almost impossible to look at the electronic medical record and catch a slow deterioration in a patient’s condition, especially with the fact that there are so many different doctors and nurses that take care of a single patient.
We asked the question: why isn’t there a simple measure of a patient’s overall condition that can be plotted versus time to show a doctor or a nurse that someone is getting sicker?
We went in and spoke to the CEO of Sarasota Memorial, who let us come in to the hospital and try out some ideas for several weeks. That led to a real project about four months later. Over the next couple of years, we analyzed about 60,000 patient visits and data extracted from the electronic medical record at four different hospitals. That led to development of software — in fact, a product and a company to deliver that product — to do that very simple thing that we started out to do: provide a measure of a patient’s condition so that a doctor or nurse can see if a patient is getting sicker.
I have to ask the obvious question in terms of how Sarasota came to be involved with your product. Was that related to … you know what I’m getting at. Was this in terms of a lawsuit or something about your mother’s treatment, or was this just their interest in improving what you had seen firsthand?
That’s interesting. No, it was not involved with a lawsuit. We actually considered the idea of suing and rejected it because it’s an empty thing to do. It would not have been of any value to us to get a sum of money. What we wanted to do was try and prevent what happened to our mother from happening to someone else. No, there were no legal negotiations involved.
Did they undertake this with you in the spirit of recognizing that they had room for improvement and that you had something to offer as someone with skin in the game?
They were a pioneer in electronic medical records. My mother died in 2003 and they had already had an EMR, I think, seven or eight years.
Yes, they’re an Eclipsys client.
Yes, yes, and they had been frustrated really, by the lack of insight that they had been able to extract from all this data. They had all this data and it’s difficult to maintain, it’s expensive, and they were waiting for the real demonstration of value.
My brother had worked in data visualization for many years, and as I said, I worked in data analysis. When we came there, it just caught their attention. The CEO was very sympathetic about what had happened in my mother’s case, but there was something else in the background. There was this underlying feeling that something should be done with all this data.
Maybe what we want is people who are coming at it in a very fresh way. We did not have medical backgrounds. In fact, if we had, I don’t think that we really would have been successful, as it turns out.
If this could happen at Sarasota, it could happen anywhere because that’s a highly regarded hospital using a highly regarded clinical system that they’ve used very well for a long time. If you were talking about the experience of Sarasota to this point, what would be their results?
We developed this index, which we named in honor of my mother — the Florence A. Rothman Index. This is a general measure of a patient’s condition. It’s now part of a software product which we deliver and is being used at Sarasota Memorial.
In terms of a measure of success of this endeavor, it really was if we could help one person avoid what had happened to my mother, then that was the sign of success. But I think we’ve helped many people at this point, but I also think we can help many more.
I guess the toughest part is that you don’t really have any way to know whether your product helped. There’s no recordable event that says, “Hey, we just saved this patient because of something we showed a clinician.” Is that going to be a challenge to go into another site to have something more than just anecdotal discussion?
In fact, we did a clinical trial at Sarasota with 1,600 patients over about five months. It was with a randomized, concurrent control group. If a patient was born in an even year, his doctors or nurses would be able to see the graph, and if he or she was born in an odd year, they wouldn’t be able to see the graph.
We then looked at the outcome as measured, in this case by discharge disposition. What we found was that more patients ended up in a healthier condition and so were able to be discharged to home rather than to rehab or skilled nursing facility. We had a seven per cent increase in discharges to home. It turned out to be a number that was statistically significant.
We’re in the process of setting up clinical trials at a number of other hospitals to replicate this and to extend the work, and to show that we have benefit at not just Sarasota, but other hospitals as well.
As I was trying to conceptualize why this works, I thought of the stock market, where you may track five stocks and think you know everything there is until you look at a stock market index and a long-term trend. Then you realize that you got so wrapped up in the trees that you didn’t see the forest. Does it happen often that the data there but clinicians miss the trend?
Yes, that’s part of it. The thing is, there’s plenty of data. We’re not creating any more data. What we’re doing is two things. We take 26 different medical measurements which are available, basically, at all hospitals. We extract the amount of risk which is inherent in the value of each of these measurements and come up with a single score.
Now in a sense, that’s what a doctor or nurse does when they go in. They come up with an overall sense of how the patient is and a good doctor does it well, or a good nurse does it well. But the problem is if a doctor is rushed, a nurse is rushed, how completely can they really evaluate all the data that’s there? Even even more importantly, do they really know how that patient was the day before when maybe this is the first time they’ve ever seen the patient?
Getting that trend is very difficult to do, even if you’re a doctor and you’re sitting down and studying what’s in the medical record. It’s hard to figure out what the trend is, especially if it’s a gradual deterioration.
There’s one other thing, and that is doctors tend to look at three things when they’re doing an evaluation. They look at vital signs, they look at lab tests, and they look at the last doctor’s notes. However, there is a source of information that they tend to overlook, and that is the nurse’s assessments.
The nurses do what is called “the head to toe assessment” of the patient. It’s something that’s taught at nursing school. They evaluate each physiological system and they record it on the computer. Really, doctors don’t look at it.
One of the things that we’ve done is we’ve said, “Hey, this is actually very valuable information about how someone is.” So we used nursing data in the calculation of our score. It gives the doctor access to something that he doesn’t normally look at.
How did you come up with the 26? How do you know those are the most relevant ones? Are you continuing to see how well the correlate with patient status changes, or do you think you’ll be adding more measures?
We started by going to the electronic medical record and saying, “What’s there?” We looked to see what measurements really are available on all patients. Not only are they available on all patients, but they’re available and they are taken on a continuing basis on all patients. That really brings you down to a relatively small number of potential variables.
Then we tested the variables against different measurements and we looked at the independence of variables. We spent a long time working on the model building itself, but in answer to your question, are we continuing to test it and look for opportunities to enhance it? The answer is yes, although we are comfortable with what we have now. I’m sure that there will be opportunities to enhance it in the future.
Do you think there’ll be ways that you can build into the presentation of the information the ability to collect new information that will help you determine if the correlation is better since your system does not accept data entry?
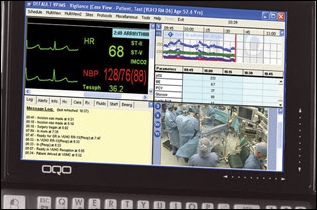
Let me say two things. One is we’re presenting doctors and the nurses with this graph, and basically, every time a piece of data is entered into the electronic medical record, we recalculate the score and we put another point on the graph. That’s the operational side of it.
But what you’re getting at really is something that we thought of right at the outset, and that is when someone is doing medical research, one of the tough things is to have a good measure of an outcome. If you’re looking for mortality as an outcome, generally mortality is very low in procedures or when you’re dealing with one drug or another. So you need large sample sizes to get specifically significant differences between drug A and drug B, or procedure A and procedure B.
At the point at which our index becomes generally accepted as a measure of patient condition, all of a sudden you have another measure of outcome. You can say, “Hey, we have procedure A and the folks who went through procedure A ended up with an average score of 75 after a week, and procedure B, the folks ended up with a score of 65. And just to calibrate you, 100 is the best and 0 is close to the worst.”
You have a way of getting a quick read on the impact of procedure A versus procedure B, or drug A versus drug B, or workflow A versus workflow B. I think there’s a lot of potential in terms of helping in medical research.
Do you see it as being something that’s applied like a pain scale or a blood sugar reading where there’s a standing order that says if the patient’s Rothman Index gets to this, then transfer them to ICU?
We are not prescriptive, nor diagnostic. We’re not telling a doctor or a nurse what’s wrong with the patient or what to do. We’re basically alerting them that something is happening. But what you’re talking about sounds like the rapid response team Initiative. Is that what you’re referring to?
Yes. It seems like one of the key problems is failure to act. There’s something going on, no one notices, there’s no predefined pathways — someone just says, “Wow, this is bad,” and then nothing happens.
Absolutely. There was a talk given by Dr. Edgar Jimenez, who is the president of the World Federation of Societies of Intensive and Critical Care Medicine. He’s also an assistant professor of medicine at the University of Florida, University of Central Florida, and Florida State University, as well as director of medical critical care at Orlando Regional Medical Center. It was a talk given at the 6th International Conference on Rapid Response Systems in May at Pittsburgh. He was talking about some work that he’s done, preliminary work at Orlando Regional Medical Center with regard to rapid response teams.
One of the problems with rapid response teams is it takes the nurse on the floor to activate the system. Some nurses are going to be great at it, some nurses are not going to be great at it, but many times nurses are overwhelmed. As you say, someone can deteriorate and no one notice, so the team doesn’t get called.
They are very excited about the system because of a capability that we have. We produce a graph showing the patient’s condition over time. We can actually produce a single screen with several hundred graphs on it so you can look at the entire hospital on one screen. The graphs are color-coded and it’s really quite easy to see a decline, even though the size of the graphs themselves is small.
One of the clinical trials that we’re going to be doing is on the order of surveillance, where a member of the rapid response team sits in an office and looks at the entire hospital and says, “Hey, there’s a downturn on the sixth floor,” and picks up the phone and calls the nurse on the sixth floor and says, “What’s going on with Mr. Smith?” If the answer is, “I thought he was going home tomorrow, I didn’t know there was anything going on,” then the rapid response team becomes proactive. They activate themselves. They really become a backup for the doctors and nurses to try and prevent people from falling through the cracks.
I would think there’s some potential use even for things like staffing or for nurse acuity; where you have patients whose diagnosis doesn’t really tell you the significance of their care requirements. The number is relative, right? It isn’t just that your number gets worse, but that if your number is lower than some other guy’s number, you’re in worse condition?
It’s an absolute value and it also shows you changes. It’s interesting that you say that because whenever we’ve spoken to, especially a chief nursing officer, she says, “Hey, I can use this as an acuity tool to help me with staffing.” I think there is some dissatisfaction with the tools that are out there because they require nurses to enter data and they can be subjective.
Our system is, in a sense, an absolute measure of the patient’s condition. As I’ve said, we color-code the graph — red being the worst — and so you can say, “Hey, if I have five red patients in one nursing unit, one thing I’m not going to do is assign them all to the same nurse because that’s going to lead to a bad outcome.” It could also be used at a higher level in terms of management of nursing hours, although we’ve not gone down that pathway yet. But it’s been suggested.
I’m a believer in the 80/20 rule –– show me the 20% of patients who are the sickest and if I manage those well, I’ll improve my overall outcomes.
Yes, I think you are right on. We really think that we have a potential of making significant impact in the quality of healthcare and we have people who have had many years’ experience in hospitals who feel the same way. It’s very exciting for us.
I know that you worked with Helios, or ObjectsPlus as it used to be called, when you started connecting to Eclipsys at Sarasota. What kind of interfacing would be required for a non-Eclipsys user and how difficult is it to manage those interfaces?
We’ve spoken to a couple of the other EMR vendors. We are prepared to interface with any of the systems.
Really, we are self-contained. We touch the world in two ways. On the one hand, we go up to the hospital’s database and we extract data periodically, but we do it in a way which has no impact on response time. Hospitals are very sensitive to anything that may degrade their response time for doctors and nurses, so we have a way of not doing that. Basically, it’s not a real-time query, so we wait for real-time queries to finish.
The other place is when a nurse goes to a nursing station and she goes to her computer and she wants to see the graph. All we need to do is know who the current patient is that you’re looking at and we can be either loosely integrated or tightly integrated with the system. With Eclipsys, we’re tightly integrated, so that there’s actually a tab on the main screen that says Rothman Index. A Sunrise Clinical Manager user wouldn’t know that they’re not using Eclipsys-native software.
But if it’s a looser integration, it might be an icon on the desktop. You click on that icon and you’re already logged on to our system through a single sign-on software system which is controlling their screen. We would know which patient you’re pointing at. We just need to know which patient it is and our server has the data and has the values of the Index, and would then be able to display a graph.
Does it alert or is it just display? Does somebody have to notice that the number’s bad or can it automatically page and escalate?
We produce a graph, but we also produce a number. That number can be used in a rule that is created by the hospital to generate an alert.
What parts of the system do you consider the proprietary and how do you envision this turning into a business?
The algorithm is proprietary, although we’re submitting an article for publication which will give the general outlines of what we’re doing. Doctors don’t like the idea of a black box. I guess that’s the proprietary element of it — the algorithm.
We’ve submitted several patent applications on the work. But we’ve spent years now validating this and so, in a sense, the protection that we have is the fact that we’ve done all this work. If someone wanted to do the same thing, it’s going to take them quite a bit of time.
Are you going to try to sell this directly to hospitals or partner with vendors? How do you see this getting out in the field?
We’re starting out by selling it to individual hospitals. We’re starting clinical trials at a number of them. The basic idea is an annual license fee, which is based on the size of the hospital. But we can see going into the future that we might partner with one or another or maybe all of the EMR companies to make it available to their customers.
Is it satisfying to see this turn into a business when the original point of it was a very personal circumstance that you knew you could improve for others?
I think that in order to deliver this and really have the largest impact, we needed to make it into a business. If it were simply a study or a paper, I don’t think that it would have reached a lot of people.
The fact that we were willing to go the extra distance to make it into a product that hospitals would be able to use easily and it will reach a lot of people, that really is a way to achieve our original goal. We just didn’t want this to happen to someone else’s mother. I think we’re going to end up accomplishing that goal.






































































You are so absolutely right. But all these issues were there before AI became a big thing. Sothis is all…