EPtalk by Dr. Jayne 3/12/26
Dr. Jayne Goes to Las Vegas

I’ve always taken a taxi when visiting Las Vegas. It has been years since I had to stand in a crazy long line, and today I figured out why. It’s because everyone is packed into the Uber/Lyft pickup area.
The kitschy neon artwork was the only good thing about the experience, which is in desperate need of a process improvement project. I was only there because I had an Uber voucher that was about to expire. I’ll be back in the taxi line next time for a cheaper and less stressful experience.
I spent some time Monday catching up with old friends at the HIMSS Native American & Indigenous Health Symposium. The clinicians in this space care deeply about their patients and the populations they serve, and are often working with minimal resources.
One session featured representatives from GDIT and Oracle Health. An attendee pointedly asked how the company will ensure that facilities that serve this population won’t experience the issues that some of the Veterans Administration hospitals have had. The answer was not reassuring.
From there, I headed to the exhibit hall for a sneak peek at the setup process. I didn’t have an exhibitor badge, but no one challenged my entry. That was a big change from the recent ViVE conference where the door teams checked every badge at some entrances.

CoverMyMeds has a swag machine in the lobby, and I received a pouch with some nail clippers that I’ll be donating when I get home. I was actually hoping for the hand sanitizer since I had forgotten to replenish my supply, but I was confident that I could find some in the exhibit hall when it opened.
I put my feet up for a bit and then was off to the opening reception. It was held once again at Caesar’s Forum, which is across the street from Caesar’s Palace. That created confusion among attendees and taxi drivers alike.

It was a target-rich environment from a footwear perspective. I found myself also eyeing these embroidery and pearl-embellished jeans. I’m not sure who the team was with the matching Nikes, but they looked sharp.
I had a chance to catch up with the incomparable Ross Martin, MD, who shared a great story about performing as Elvis for HIStalkapalooza 2013. He was even able to produce the highlight reel from the event on his phone, which was a nice treat.
On the way back, I did a detour to the Bellagio Fountains. I was lucky enough to catch my favorite song, which made for a perfect cap to the evening.

The next couple of days were a whirlwind, with plenty of sessions and laps around the exhibit hall. It felt a lot like the old days of HIMSS. I saw fewer influencers and more people ready to do business than I did at ViVE.
Some complained that HIMSS doesn’t include meals with registration, but those who ventured down to the Hall G lower level were rewarded with cookies, fruit, brownies, blondies, and the elusive Kouign Amann pastry. The lower level was dubbed “The Park” and also included the odd tree here and there, as well as a food court and a place to pet kittens.
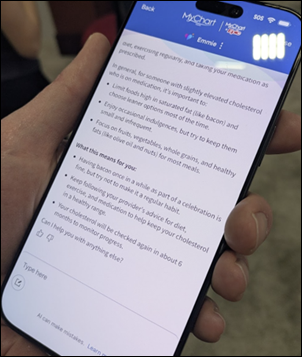
At the Epic booth. I was pleased to see that their new AI solution offers sensible patient-facing information for a scenario where a patient asks if they can celebrate with bacon while in Las Vegas even though they have high cholesterol. As usual, the Epic booth had the most plush carpet in the exhibit hall. I didn’t know that I needed a coffee table that was embellished like the painting “The Starry Night” before I went there, but apparently, I need that in my life.

It’s great to see the next generation of healthcare tech professionals coming to see the big show. I enjoyed an impromptu demo from graduate student who was working on the TheraCare.ai platform.
It seemed like everyone was talking about AI or SaaS solutions, but I always enjoy visiting vendors that offer physical technology, such as waterproof keyboards, innovative crash carts and workstations, and communications devices.
During my booth crawl with Dr. Craig Joseph from Nordic Global, we scoped out Athena Security’s hospital visitor management system technology, which includes AI-powered concealed weapons detection. Having worked at hospitals that have had serious security incidents and even injury to staff, such solutions are unfortunately necessary, and it’s nice to see innovation.

The show floor had a couple of themed seating areas, one of them complete with a digital fireplace. For the zone that had the bean bag chairs, they were less occupied than the more traditional chairs, which might say something about the agility of the average HIMSS attendee and our willingness to risk being unable to arise from a soft surface. The main floor also included a puppy park, although I didn’t see any dogs during the times I passed by.

First Databank had a cool giveaway with its adult coloring book.
The best booth slogan goes to connectivity vendor Digi International, which promised “The Ultimate Hookup.” CognomIQ was close behind with their offer of a chance to “win a prize that doesn’t suck,” which was funny since it was a Dyson vacuum.

The footwear game was strong this year. IMO Health brought their shoe and sock A-game as usual. I’m sure they are looking forward to next year, when HIMSS returns to their hometown of Chicago.

American Messaging had light up shoes for the whole team.

The ever-dapper Jonathan Shivers of Relatient married form and function with oxfords and argyle.
My spotters were calling in outstanding outfits from across the show, but I wasn’t fast enough to catch the woman in the hot-pink suit with matching shoes or the pair of gents who were wearing matching brocade dinner jackets.
Wednesday afternoon featured a number of in-booth happy hour events. Drinks were flowing as long as you were willing to have your badge scanned. I always wonder about the return on investment for those events, since a good number of the attendees aren’t decision makers or budget owners. I’m sure it falls into the category of all publicity being good publicity, but I can only imagine what the event services vendors charge for a happy hour service.
I had to head for the airport due to some obligations at home, so I’ll be missing Thursday morning’s session covering the future roadmap for the Centers for Medicare & Medicaid Services featuring Dr. Mehmet Oz. I’ll be interested to hear from those who attended and whether you found the content inspiring. There is much work to be done in the US healthcare space.
If you attended HIMSS, what was the highlight of the event? If you didn’t attend, why not, and where are you spending your budget instead? Leave a comment or email me.

Email Dr. Jayne.
















“ Pondering: if medical practices really care about patient health and access, why are their offices closed 75% of the…