Weekender 4/13/18

Weekly News Recap
- FDA approves IDx’s AI-powered diabetic retinopathy screening system for use by PCPs.
- Theranos lays off most of its remaining employees, having cut its 2015 headcount of 800 down to around 20.
- Mayo Clinic offers voluntary severance packages to 400 transcriptionists whose it no longer needs because of speech recognition.
- The Coast Guard announces that it will piggyback on the DoD’s Cerner contract, with the additional contract cost yet to be determined.
- Netsmart acquires Change Healthcare’s home and hospice care software solutions.
- Facebook acknowledges that it tried to convince the American College of Cardiology to share de-identified patient data with it.
Best Reader Comments
I have to beg for de-identified data for EHR testing purposes, but Facebook gets it wholesale from a professional organization. If this isn’t a HIPAA violation, particularly with the re-identification plans, what is? And who can be called upon to get medical data protected properly? (Kitty)\
I’m not sure I’d want to pay for Facebook’s ad targeting or trust that they could re-identify data correctly. (1) Facebook flagged me with their African-American multicultural marketing flag. I am in fact a white Midwesterner who didn’t even encounter a black person until college, so even if they couldn’t tell from the hundred pictures they have of me, it’s not like I’m steeped in African-American culture. It’s very flattering that Facebook feels I empathize, but I’m pretty sure no actual person would identify me this way. (2) After I looked up Chicago the band, I got ads for weeks about events happening in Chicago the city. If this is representative of their big data skills, let’s hope that Facebook isn’t starting a self-driving car business anytime soon. (Midwest User)
While healthcare is much more complex than banking, the bankers had their game together very much earlier. I could travel 2000 miles and withdraw cash from my bank account in 1990. I would still have problems today to give a doctor 2000 miles away ANY electronic access to my medical records. (Fat Hertime)
Watercooler Talk Tidbits
Readers funded the DonorsChoose teacher grant request from Ms. O in Texas, who reports on her class’s use of a programmable robot. “My students are having a blast making our Lego robot. They learned quickly that they would need to talk to each other to figure out which part came next. Once this was established, the quick building began. They have loved putting this robot together so much that I do not think they realize how much they were learning. My students are using area and perimeter with the robot, along with following directions from pictures (no teacher help). Next they will be coding the robot to walk and move around. Thank you so much for bringing this activity to my students.”


We provided after-school STEAM project kits for Ms. P’s special needs K-5 class on a Native American reservation in Idaho. She reports, “After showing everything and talking about them, the students wanted to make slime first! I was so amazed at how much they listened to and remembered the information about polymers. The students have stepped up to the plate and have accepted the challenge to work together to figure things out. They are coming up with so many more ideas than I thought they would. They love to be able to take turns to be the teacher to explain their project. You are a hero to me and my students. They recognize that we wouldn’t have these things without your help.”

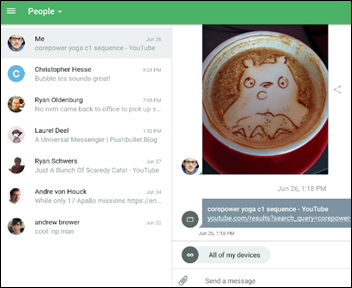
I downloaded Facebook’s archive of information it knows about me (click Settings, then “Download a copy of your Facebook data.”) even though I do basically nothing on Facebook, rarely look at it, and don’t use Messenger or any app. The archive included:
- All contacts from my phone (the contact name I assigned and their phone number)
- Every login date and time
- Facial recognition data
- Messages
- Ads I’ve clicked
- A huge list of advertisers who uploaded a contact list with my info (a subset is above), an odd lot that included politicians from states I’ve never even visited, Dierks Bentley, drug companies, bands, and for some unknown reason, a ton of rappers.
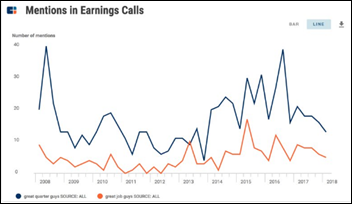
CB Insights mined its earnings call transcripts to see how often Wall Street analysts suck up to company executives while asking them questions and found that use of “great quarter, guys” peaked in 2008, although the most common compliment remains, “Congratulations on a great quarter.” I’m signing up to see how often analysts use trite terms in asking questions like, “Can you provide some color around that number?”
Talkspace, which offers online counseling and therapy, claims it has 1 million users, is marketing services to employers, and is contemplating an IPO. A Verge review from late 2016 wasn’t complimentary, noting:
- Therapists are hired as 1099 independent contractors and bear all the responsibilities since the company says it’s not a medical provider. The company pockets half of their billed amounts.
- Talkspace owns the medical records of patients and therapists don’t have access to them once they’ve stopped working for the company, making the patient transition difficult.
- Therapists are required to follow scripts.
- The company set a rule that therapists could not complain about it internally on its Slack channels.
- Patients are anonymous, so therapists have no way to contact authorities if they appear to be a threat to themselves or others.
- Therapists say the company places client retention above all else.
- Talkspace’s terms of service agreement says patients should not make health or well-being decisions purely on their use of the service, which they add is not a substitute for face-to-face therapy sessions.

Kaiser Family Foundation SVP Larry Levitt notes that despite this short-term insurance plan’s name and choice of cover stock photos, it doesn’t cover mountain climbing injuries. The plan – of the type the Trump administration wants to roll out more widely – also doesn’t cover pre-existing conditions, prescriptions, pregnancy and childbirth costs, kidney disease, skin conditions, long-term care, sports injuries, or injuries incurred while under the effects of alcohol or drugs. The insurer also has no provider network, which I assume means that services will be billed as out-of-network visits with the patient being balance-billed – the plan pays a flat 150 percent of Medicare-allowable expenses and you’re on your own after that. I checked premium prices for a 30-year-old male in Chicago and they ranged from $88 to $177 per month with deductibles from $1,500 to $5,000. It may be better than having no insurance at all for some people (like those who don’t expect to actually require care), but make no mistake, those having it could be wiped out financially very, very easily from the unjustifiably high charges generated in a single hospital or ED visit.

Japan-based drug maker Otsuka, whose antipsychotic drug Abilify is available in a “smart pill” form using technology from Proteus Digital Technology, has owned California winery Ridge Vineyards since 1986. The company says the winery is profitable, but its other use is for executives to entertain business partners during the JP Morgan Healthcare Conference in January.
BMJ Case Reports describes an ED patient who complained of dry heaves and thunderclap headache after eating one of the world’s hottest chili peppers in a contest, causing reversible cerebral vasoconstriction syndrome in his brain that could have caused a stroke or heart attack. The article didn’t mention his final standing on the leaderboard.
Police file charges against a nursing student who was shadowing staff nurses at Lahey Hospital and Medical Center (VT) after he was caught hiding a video camera in an employee restroom. A housekeeper found the pen-sized device almost immediately. He wasn’t smart — a review of the camera’s contents clearly showed his face and ID badge as he recorded himself adjusting the camera’s angle to face the toilet.

Stat excerpts fun stories from the new book (due to be released on May 21) about Theranos, written by Wall Street Journal reporter John Carreyrou, who exposed the scandal:
- Theranos faked a demo of its non-functional technology to drug company executives way back in 2006, and when the CFO of Theranos heard about it and raised concerns, Elizabeth Holmes fired him on the spot.
- The head of the software development team bragged that he could write the company’s software faster in Flash, after which someone noticed a “Learn Flash” book on his desk.
- Elizabeth Holmes hired her brother – who had no obvious qualifications – as a product manager, after which be brought on several of his Duke University fraternity brothers to form what insiders called the “Therabros” or “The Frat Pack.”
- A former employee heard Holmes speak in a higher-pitched voice, leading them to speculate that she intentionally speaks in public in a low baritone to fit in with Silicon Valley’s male-dominated executive culture.
- Carreyrou writes that Holmes had a romantic relationship with Theranos President Sunny Balwani, breaking up with the man 20 years her senior only after she had to fire him as the company’s story began unraveling.

Bizarre: a plastic surgeon in Germany is arrested for unintentionally killing a woman he met online for sex by sprinkling cocaine on that particular part of his anatomy to which she was voluntarily providing oral attention.
In Case You Missed It
- News 4/13/18
- EPtalk by Dr. Jayne 4/12/18
- News 4/11/18
- Curbside Consult with Dr. Jayne 4/9/18
- Monday Morning Update 4/9/18
- What I Wish I’d Known Before … Serving on the Board of a Company or Non-Profit
Get Involved
- Join my Rolodex to provide occasional news reaction or ideas
- Contribute regularly as a provider CIO, IT director, or informatics nurse (anonymous or not)
- Be interviewed (providers)
- Deliver an educational webinar (providers)
- Sponsor
- Report a news item or rumor (anonymous or not)
- Sign up for email updates
- Connect on LinkedIn
- Contact Mr. H
















































































One solution would be federal (or state) requirements; but more ideally health systems would view their digital patient tools as…