EPtalk by Dr. Jayne 4/2/26
Epic once again understood the April Fools’ Day assignment. They shared a trio of tricks this year.
The first was the addition of “introvert mode” for AI-powered charting, which is designed for physicians “who would really rather not have to narrate everything out loud.” It promises to convert “pauses, sighs, key taps, and meaningful silence to generate complete documentation of the conversation that almost happened.” I’ve helped train a number of physicians that fit the introvert profile, so this definitely generated a chuckle.
The second joke involved the remaining of Epic’s AI assistant Penny to Nickel in recognition of the US Mint halting production of the one-cent coin. Epic poked fun at itself. An FAQ published for affected hospitals reportedly includes the question, “Will Nickel cost five times as much?” followed by the single word, “No.”
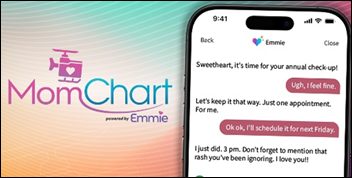
The one that had me rolling the most though was “MomChart” powered by Epic’s new patient-facing AI assistant, Emmie. The spoof logo included a helicopter and the sample conversations incorporated typical mom-style guilt, including preventive care reminders such as “You know I don’t ask for much. Just One Screening. For me.” Describing the new persona as “warm, persistent, and just wants what’s best for you” had me laughing out loud, which fortunately was not while multitasking on a call involving video.
I cackled at the mention of MomChart combining “evidence-based clinical guidance with the unconditional love of someone who has been worried about you since the day you were born.” Future personas were proposed including “The Friend Who Happens to Know a Lot About Medicine,” which should resonate with every physician who has been on the receiving end of questions from well-meaning friends and family. “Dad Mode” was also mentioned as being in development, including daily weather updates, oil change reminders, and random news articles under the header “Thought you should see this.” Well played, Epic, well played.
I spent a big chunk of today playing phone tag with a physician who doesn’t seem to understand basic workplace courtesies. He emailed me asking for the opportunity to chat about a recent change to the EHR, and when I offered times, he countered with a request to “send me a secure chat at 8 a.m. and we’ll see what my day looks like.” We are all about serving our internal customers, so I did as he asked.
He then texted me multiple times over a 10-minute period, telling me he was free at the moment, He then escalated to tell me that he only had a few minutes and then that he could no longer wait for me. I guess I didn’t understand that I was supposed to text him to see what his day looked like and then sit staring at my phone just in case he was free.
I replied again and outlined my schedule, letting him know what blocks of time I had available. He then called in the middle of two meetings in a row. When I was finally able to reach him, he asked if I had any training materials for the new feature that explained why his department should use it, and if so, could I send them.
I’m still baffled why that request couldn’t have been included in the original email or why it required several rounds of phone and chat tag between two physicians who have plenty of other things demanding their time.

An Original Investigation in the Journal of the American Medical Association this week looks at the impact of AI-powered scribe tools on clinician visit quantity and time expenditure. Across five academic medical centers, they examined the metrics of 8,581 clinicians, including 1,809 who were using AI-powered scribe tools. The locations were diverse, including Mass General Brigham, Emory Healthcare, University of California San Francisco, Yale New Haven Health, and the University of California Davis.
The sites used three AI scribe tools, Ambience, Nuance DAX Copilot, and Abridge, either individually or in combination. The institutions provided data on clinicians over at least a 12-week period, including six weeks pre-adoption and six weeks post-adoption for those using the tools.
Using data from Epic’s Signal database, the authors found decreases in total EHR time and documentation time, and an increase of approximately one half patient visit per week. They felt that due to the multisite nature of the sample, they were able to identify the characteristics of clinicians who benefitted most from using the tools, namely female clinicians and those practicing in primary care and medical subspecialties.
I didn’t see specific mention of results for surgical subspecialists, but based on my own experience, a recent office visit with a surgical subspecialist probably contained fewer than 100 words, and was largely procedure focused. From experience with their EHR in a past life, I suspect that the visit could have been documented in fewer than five clicks, so I can’t imagine that having a scribe, whether human or AI, would have been helpful.
I would say that I can’t wait to see the visit summary from that one, but I guess I’ll be waiting a long time because they didn’t offer me access to their patient portal or even mention having one. I was so glad to be in and out quickly that I didn’t think to ask.
The biggest limitation of study in my mind was the fact that the study focused on academic practices where the average weekly visit volume was 20. Most of the clinicians I work with see more than 20 visits per day, so it’s likely that they would demonstrate different results than were seen in the study.
A corresponding Editorial notes that “what is known today about the effectiveness of ambient AI scribes reflects outcomes that are easiest to count: electronic health record (EHR) time, documentation minutes, visit volume, and billing.” It goes on to question whether the time saved “is reinvested in ways that measurably improve outcome and equity for patients.”
I would go farther to ask whether the use of AI-powered scribes impacts clinical outcomes on a per-encounter basis, such as by helping clinicians better organize their thoughts or better focus on their patients and therefore arrive at different recommendations than they might have had they not used scribe technology.
The editorial calls the relationship of productivity to value: “If health systems rely on increasing visit volume to justify the cost of ambient AI adoption, they risk squandering the benefits of time savings if that time is simply converted into more visits per clinician, rather than investments in higher-quality care.”
Based on my interactions with hospital leaders for a few decades now, I’d bet the farm that a large number of hospital executives are looking strictly at the cost/benefit analysis and how they can use the technology to trigger more visit revenue. The editorial specifically calls on organizations to evaluate how AI scribe use impacts chronic disease management, preventive care, and delivery of unnecessary services.
Is your organization looking at how AI tools can improve care quality as well as how they can reduce documentation burden? Or is the focus on improving coding and billing? Leave a comment or email me.

Email Dr. Jayne.


Reed, thank you for sharing your insights and market perspectives. Shaun