Merry Christmas and a Happy New Year to the HIStalk crowd. I wish you the joys of the season!
News 6/11/14
Top News


Our intrepid beltway reporter Dim-Sum has been telling us for months that IBM and Epic are pitching for the DoD’s $11 billion EMR contract, which IBM now confirms in announcing its intentions. Heading the project will be IBM CMIO Keith Salzman, MD, MPH, who was an Army doc for 22 years. Dim-Sum’s reports have been minor masterpieces of puns, semi-obscure references, and teasing hints, but I just realized that even his or her phony name is yet another one: the bid falls under DHMSM (DoD Healthcare Management Systems Modernization). I suspect we will get a June report shortly, but in the meantime, you might want to refer to his or her updates from March 5, March 28, April 9, and May 2 now that their accuracy has been confirmed (he or she reported here that it would be IBM-Epic two months ago.)
Reader Comments

From Big Sky: “Re: Benefis Health System in Montana. Has an RFI out for EMR replacement.” Unverified. I don’t know what they’re running for inpatient, but they finished a huge NextGen ambulatory rollout a couple of years ago.
From Speechless: “Re: HIMSS chapter speakers. We are putting together a panel discussion for the fall on healthcare IT innovation. If you could choose one or two East Coast speakers, who would they be? We’re thinking of a progressive hospital CIO, someone interesting from one of the incubators, and a provider-side innovation leader.” Let’s crowdsource it with HIStalk readers – leave a comment with your suggestion or if you’d like to volunteer to present (or you can email me.) I’ve been a HIMSS chapter program chair and it’s hard to get good non-vendor speakers.

From Demon Deacon: “Re: Wake Forest Baptist Medical Center. Successfully launched Epic Inpatient for the Lexington Medical Center, which was the last Wake Forest hospital to go live.” Congratulations to WFBMC for getting the job done despite some disastrous (and preventable) early missteps that cost the health system a lot of money and credibility. My fellow barbeque fans might consider a site visit given that Lexington, NC has the highest ratio of pits-to-people in the country and one joint (Lexington Barbeque, aka “Honey Monk’s”) fed world heads of state at a 1980s summit at the request of President Reagan.

From Power Seeker: “Re: power strips. Joint Commission says that CMS ‘is no longer allowing relocatable power taps, referred to as RPTs or power strips, to be used with medical equipment in patient care areas, including operating rooms, patient rooms and areas for recovery, exams, and diagnostic procedures. The restriction does not apply to non-patient care equipment such as computers and printers or to areas such as nurse stations, offices, and waiting rooms.’ If this is true, time to invest in companies that sell UPS solutions.” It’s true. Patient care rooms are going to need a lot of red wall jacks to plug in medical devices individually. Hospitals will also need to check their liability insurance since power cords will be running all over the place and tripping people. I see the point – even UL-approved power strips aren’t intended for critical medical devices where failure could be disastrous (if there’s no battery backup, anyway) — but alleviating that risk will be ugly in already-crowded patient rooms.
From Wayne Tracy: “Re: Monday’s post. I’m very cynical about the VA’s problems and agree that because of commercial vested interests, VistA is quite likely to become a fall guy. VistA in my opinion is the most comprehensive user-developed healthcare clinical application. My fear is that the lack of advocacy is because: 1) Sonny Montgomery is no longer in Congress, 2) No vender will make money on it, 3) No consulting company can charge an arm and a leg to implement it. The proposals to do away will the VA healthcare system are at best naive. Last time I looked at our mental health system, I’m compelled to assert that it is woefully inadequate. What system can deal the population of amputees and brain trauma cases plaguing some two million recent vets? Some have suggested that some 50 percent are or will experience PTSD and related psychological problems. What civilian healthcare organization is prepared to deal with that large a patient population, or more importantly, has the proven expertise? If you think the backlog is bad now, just wait. This administration and Congress has good intentions that will potentially result in a diminished quality of care at greater expense.” Wayne is an industry long-timer and a retired Navy officer. I agree with all of his points. VistA will take a fall because the VA’s volume and people problems are drawing beltway buzzards and arrogant DoD’ers who can’t wait to see VistA replaced with something way more expensive even though it has been a poster child for doing IT the right way for patients (although the VA has struggled with automating patient scheduling). Nobody wants to talk about his second conclusion – we civilians weren’t really paying attention to what was happening in Iraq and Afghanistan because the death toll didn’t seem all that high. Our military participants were coming home alive but physically and mentally mangled and now we have to figure out how to pay for their care whether it’s delivered by the VA or otherwise. I’ve argued in the past that the VA should be dissolved and care provided by the existing healthcare system, but I’m not confident that system can handle the volume any better or that we can manufacture enough additional red ink to cover the cost.
HIStalk Announcements and Requests
Listening: Circa Survive, thoughtful indie rockers from Doylestown, PA. I’ve been listening to them nonstop once I got over my disappointment that the singer isn’t a sensitive female but instead is a high-voiced guy. Those of us with a clinical persuasion will appreciate this song title: “The Difference Between Medicine and Poison is in the Dose.” They’re touring now with Ume, who I also like a lot. Also, new albums from First Aid Kit and Passenger.
I was reviewing Steve Blumenthal’s slides from the June 24 webinar below – he’s going to be fun, I suspect, especially for a lawyer. I also sat in on the rehearsal for the radiology workflow one and it was interesting to hear about teleradiologist workflow with the high volumes of images they deal with – no wonder they sit in a quiet, dark room and look at on-screen pictures while talking into a microphone all day. Like programmers, I’m guessing they rarely see daylight.
Upcoming Webinars
June 11 (Wednesday) 1:00 p.m. ET. A Health Catalyst Overview: An Introduction to Healthcare Datawarehousing and Analytics. Sponsored by Health Catalyst. Presenters: Eric Just, VP of technology; Mike Doyle, VP of sales; Health Catalyst. This short, non-salesy Health Catalyst overview is for people who want to know more about the company and what we do, with plenty of time for questions afterward. Eric and Mike will provide an easy-to-understand discussion regarding the key analytic principles of adaptive data architecture. They will explain the importance of creating a data-driven culture with the right key performance indicators and organizing permanent cross-functional teams who can measure, make and sustain long-term improvements.
June 24 (Tuesday) noon ET. Innovations in Radiology Workflow Through Cloud-Based Speech Recognition. Sponsored by nVoq. Presenters: David Cohen, MD, medical director, Teleradiology Specialists; Chad Hiner, RN, MS, director of healthcare industry solutions, nVoq. Radiologists – teleradiologists in particular – must navigate multiple complex RIS and PACS applications while maintaining high throughput. Dr. Cohen will describe how his practice is using voice-enabled workflow to improve provider efficiency, productivity, and satisfaction and how the technology will impact evolving telehealth specialties such as telecardiology.
June 24 (Tuesday) 2:00 p.m. ET. Share the Road: Driving EHR Contracts to Good Compromises. Sponsored by HIStalk. Presenter: Steve Blumenthal, business and corporate law attorney, Bone McAllester Norton PLLC of Nashville, TN. We think of EHR contracts like buying a car. The metaphor has is shortcomings, but at least make sure your contract isn’t equivalent to buying four wheels, an engine, and a frame that don’t work together. Steve will describe key EHR contract provisions in plain English from the viewpoint of both the vendor and customer.
June 26 (Thursday) 1:00 p.m. ET. The Role of Identity Management in Protecting Patient Health Information. Sponsored by Caradigm. Presenter: Mac McMillan, FHIMSS, CISM, co-founder and CEO of CynergisTek. Identity and access management challenges will increase as environments become more complex, users create and manage larger amounts of sensitive information, and providers become more mobile. Learn how an identity and access management program can support regulatory compliance, aid in conducting audits and investigations, and help meet user workflow requirements.
Acquisitions, Funding, Business, and Stock

T-System sells its ED billing business to Intermedix, saying it will focus on its clinical and coding initiatives that will continue to be offered under the RevCycle+ brand.

Indianapolis-based startup Indigo Biosystems raises $8.5 million in venture capital and replaces its CEO with the company’s founder. Its clinical laboratory software interprets visual results from instruments such as mass spectrometers, flagging outlier data for human review.

Oncology drug maker Celgene invests $25 million in NantHealth to develop personalized medicine for cancer. There’s a connection: NantHealth founder Patrick Soon-Shiong sold his own chemo drug company, Abraxis BioScience, to Celgene for $3 billion in 2010.
Sales

The federal government awards ScImage a two-year, $45 million contract for its Picom365 Enterprise system, including PACS, diagnostic viewers, VNA, and workflow tools.
United Arab Emirates-based physician helpline vendor Mobile Doctors will implement mobility solutions from Cerner.

Freestanding Cypress Creek ER (TX) chooses Wellsoft’s EDIS.

Mission Health (NC) will advance its population health management with Health Catalyst’s Late-Binding Data Warehouse and Analytics platform.
Children’s Health Alliance (OR) chooses Wellcentive’s population health management solutions.
Catholic Health (NY) selects Perceptive Software’s enterprise content management system to integrate with its Infor financial and HR systems.
People

Sunquest officially announces that Matthew Hawkins (Greenway Health) has joined the company as president.

Capsule Tech promotes Kevin Phillips to VP of marketing and product management.

Former athenahealth CFO Carl Byers (Fidelity Biosciences) joins the board of Netsmart Technologies.
Announcements and Implementations
ZeOmega announces the 5.6 release of its Jiva population health management system.
Healthcare Engagement Solutions signs an agreement with Cleveland Clinic Innovations to further develop its Uniphy mobile technology platform.

Rockcastle Regional Hospital (KY) goes live on Medhost, sending data to the Kentucky HIE through YourCareLink.
IntraCare North Hospital (TX) goes live on Medsphere’s OpenVista.
Belmont University and the Tennessee chapter of HIMSS launch a healthcare IT certification program for individuals.
The mHealth Summit announces that it will host the Global mHealth Forum for low- and middle-income countries, to be co-located at its December 7-11 conference in National Harbor, MD.
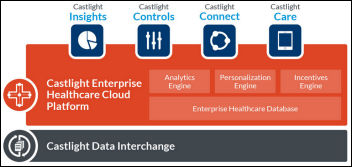
Castlight Health announces GA of Castlight Enterprise Healthcare Cloud, which provides four solutions for self-insured employers: cost-optimization analytics, benefits design, a catalog of available third-party services, and a mobile benefits app for employees. Shares were up 3 percent Tuesday, but still down 58 percent from the closing price on IPO day less than three months ago. The company’s valuation is $1.5 billion on $20 million in annual revenue and $75 million in annualized losses.
Government and Politics
A VA self-audit of 731 facilities finds that 13 percent of schedulers were told to enter desired appointment dates different from what the patient requested, eight percent of facilities kept external scheduling lists invisible to the VA’s EWL/VistA systems, and unrealistic targets encouraged facilities to game the system. New patients waited up to three months to see a doctor. The VA announced immediate changes: eliminating the 14-day appointment target as unreasonable, implementing real-time patient surveys, conducting an external audit, freezing new hires and eliminating bonuses at VA headquarters and regional offices, and creating an HR team to get clinicians hired faster.
CMS may be congratulating itself publicly for releasing Medicare payment data (which it did only after losing a lawsuit in trying to prevent it), but the more the statistical jockeys play around with the databases, the more obvious it becomes that CMS is asleep at the taxpayer wheel. A Wall Street Journal analysis finds that 2,300 providers were paid $500,000 or more from performing single procedures or services, some of them operating well outside their area of expertise. A non-cardiologist was paid nearly all of the $2.3 million he billed Medicare for in 2012 for performing a rare and questionable cardiac procedure (“exercise while lying on your back,” advertised on his site above) on all of his Medicare patients, with his entire training in the procedure consisting of “reading lots of articles, studies, and clinical trials.”An orthopedic surgeon billed Medicare for $3.7 million in one year even though he didn’t perform a single surgery – he charged for 108,000 massages and manual manipulations. It was billed by his former employer, Abyssinia Love Knot Physical Therapy, a PT chain run by self-proclaimed “Pastor Shirley.”

HHS tweeted this picture, which it captioned, “Welcome Secretary Sylvia Mathews Burwell!” I haven’t seen anything official that she has been sworn in.
The Indian Health Service contributes its VistA-based RPMS scheduling system to the OSEHRA open source community.
The Alliance for Connected Care writes to Sylvia Burwell even before she takes office as HHS secretary, urging her to use her authority to open up telemedicine reimbursement for all ACO providers, not just those located in specific rural areas as is the case today. The trade association, run by former government officials Tom Daschle, Trent Lott, and John Breaux, actually sent two letters, one signed by its business members (Walgreens, WellPoint, and Teladoc, for example) and the other signed by a couple of dozen big health systems. The American Telemedicine Association sent Burwell a letter of its own listing sweeping improvements that would be enabled by paying everybody for delivering telehealth services, with that letter signed by mostly by big vendors (and HIMSS.) One might infer that while patient care could improve under such an arrangement, vendor and provider revenue would most certainly do so. Sylvia hasn’t even found the restroom yet and already the special interests are pawing at her.
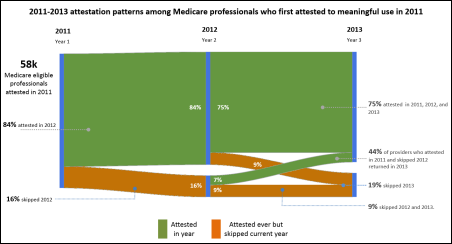
Statistics presented at Tuesday’s HIT Policy Committee meeting indicate that of EPs who first attested for Meaningful Use in 2011, 84 percent attested in 2012 and 75 percent in all three years of 2011, 2012, and 2013. Nearly half of those who attested the first year and then skipped 2012 returned in 2013. EHR incentive payments totaled $24 billion through the end of May.
AHRQ, presenting at the HIT Policy Committee meeting Tuesday, says that lack of EHR interoperability is a big problem, recommending that ONC define an “overarching software architecture” within 12 months and require EHR vendors to develop and publish APIs to support it. I’m pretty sure that’s not going to happen.
Other
St. Francis Hospital (GA) admits that one of its employees sent a mass email to 1,175 patients using CC: instead of BCC:, exposing the email addresses to all recipients. Apparently even that triggers the breach notification rule, at least according to the hospital’s interpretation.
BetaBoston profiles Seratis, a secure messaging app for care teams. The company is offering free personal use and hopes to get a Boston pilot. Their site is light on details, so it’s hard to determine whether its product is differentiated from similar apps from bigger players.

Victor Dzau, MD, stepping down as CEO of Duke University Health System (NC) on June 30 to become president of the Institute of Medicine, looks back on his tenure with comments about Duke’s $700 million Epic system:
I think we all recognize that to provide the best care for patients, you need an integrated information technology system … you can capture all the information of the patient made available to the providers and the patient, and make it available throughout the entire system … Through Epic, we are able to connect with other systems that have Epic, such as Novant and many others; now UNC just implemented it … It really is an entire information system that allows you to look at charge capture, laboratory testing, finances, work flow, decision-making … it’s a phenomenal system that can help us really improve patient care … about a year ago, I launched an institute called Health Innovation to try to make the whole place think about better ways to think about patients to try to bring together this whole large amount information that we have now through electronic health records and the use the analytic capabilities to look at data, big data, to determine how we can be a learning health care system, and try to use the new technology of digital technology sensors and others to manage patients better in the community in their homes and so they don’t have to use our facilities as much … we have Durham Health Innovation which is an initiative that we will work with the Department of Health and others bringing in geographic information systems, mapping the patient, the community, where do they live, what are the economic factors, what’s the closest clinic where’s the closest grocery store, the closest barber shop to work together to improve their health.
This seems like the worst app idea ever. A Singapore company creates Hospital PIX, the usual lame hospital finder app that also allows users to “post reviews about OBAMACARE.” That’s not even the “worst” part: it also encourages doctors, nurses, and patients to post their hospital photos (we have this thing called HIPAA over here). The fake photos from “Benson Hospital” feature an entirely Asian medical staff and the hospital distances shown are all from Indonesia, so perhaps the app’s localization isn’t quite complete.
In Alberta, Canada, the government-backed Telus Wolf system goes down on Monday, leaving practices without access to lab results, medical histories, and medications. According to one doctor, “There is no longer any government support. We pay $2,000 a month for this. Who is going to hold Telus accountable now? The government has abandoned us. Cost and issues switching patient data when systems are not compatible prevents us from going somewhere else.” Telus acquired Wolf Medical Systems in February 2012.
The Apple Toolbox site files a Freedom of Information Act request to find out what was discussed in several meetings between Apple and the FDA last year. The highlights:
- Apple thinks the FDA’s guidance on mobile medical apps is appropriate.
- The company believes it has a “moral obligation” to do more given the increasing number of available mobile sensors.
- FDA will regulate apps based on their intended use, not necessarily because they use a particular sensor. For example, FDA wouldn’t regulate an consumer-oriented information nutrition app that uses a glucometer, but would consider the same app a medical device if it is targeted to diabetics.
- Apple and FDA will work more closely together to ensure that Apple’s plans don’t run afoul of FDA’s requirements (it’s good to be Apple).
Weird News Andy questions whether this was really the “responsible” anesthesiologist. Washington’s health department suspends the license of a Seattle anesthesiologist for sexting during surgeries, accessing patient images for sexual gratification, and having sex at the hospital. Investigators found 250 sexually related messages he had sent while in surgery, including pictures he sent to patients of his exposed genitalia, one of which he captioned, “My partner walked in as I was pulling up my scrubs. I’m pretty sure he caught me.”
Sponsor Updates
- Greenway customer ARcare (AR) earns recognition as Stage 7 of the HIMSS Ambulatory EMR Adoption Model.
- Impact Advisors is named to Crain’s Chicago “Fast 50 List” of high-growth companies.
- A pMD blog post addresses “Medical scribes: the solution to EHR inefficiencies, or just a temporary bandage?”
- First Coast Cardiovascular Institute (FL) reduces charge lag after going live on MedAptus charge capture.
- Kareo and ChartLogic partner to deliver cloud solutions for surgical, orthopedic, and otolaryngology specialties.
- Gartner names AirWatch as a Leader in the 2014 Magic Quadrant for Enterprise Mobility Management.
- Verisk Health SVP Matt Siegel will moderate a panel discussion on value-based healthcare at AHIP Institute June 12 in Seattle, WA.
- Truven Health Analytics launches its cost-sharing reduction analysis and reconciliation solution for health insurance exchanges.
- Merge Healthcare is hosting a Coding Contest for Computer Science students June 11 at the University of Waterloo in Canada.
- ADP AdvancedMD supports the Greater Springfield Habitat for Humanity during a corporate team-building day.
- NaviNet collaborates with Informatica to deliver a “smart” network.
- E-MDs will offer Lightbeam’s population health management solution to its clients.
Contacts
Mr. H, Inga, Dr. Jayne, Dr. Gregg, Lt. Dan, Dr. Travis, Lorre.
More news: HIStalk Practice, HIStalk Connect.
Get HIStalk updates.
Contact us online.







Re: Benefis has Meditech for inpatient. Not surprised they are considering replacement.
Question: So if the software for the IBM-Epic DoD project is $11 Billion, can we use the usual ratio of 3 to 5 times the cost of the software to calculate the true cost with implementation? Or is implementing something like that much more complex?
Ross, that amount is mostly for the SI, Implementation and Operation over a 10 year lifespan. The software cost will be a very small fraction of that amount.
But, given the depth of your previous research, I assume you already knew that.
US like every country almost never takes adequate care or fufillls its promises to veterans especially the wounded and mangled ones. US did it after the Revolutionary War when they could give away cheap land grants especially in Ohio as compensation or after WW2 due to the sheer numbers of veterans who returned and a political party who believed in granting them a lot of govt benefits.
Another Question: How come there are always billions of dollars laying around to pay for technology (and I agree $11 billion seems way low), but we never can find spare change to put people in a room with a doctor?
I suggest David Whitlinger, Exec. Director of the NY eHealth Collaborative, as a speaker for the HIMSS event you mentioned. He is an expert re digital health innovation.
Ruminations today:
Incentive payments of $24 billion. ROI anyone? Have there been any data consistent with improved ooutcomes, more patient satisfaction, or reduced costs? Hard to imagine costs of health care will be reduced when the IT costs are included.
With all due respect to the brilliance of Dr. Dzau, his testimonial fails to disclose when he last entered an order using CPOE. Our group of doctors always find it odd that those claiming the greatest benefits of HIT never enter the orders or read the 8 page progress notes.
Funny how departing Hosp CEOs always make it a point to defend their actions, especially massive investments in tech that is not well suited to a future of mass transformation in how healthcare will be delivered. Much like the newspaper industry, the healthcare industry is just digging itself deeper into the well.
Seriously, Mr. H, you need to come to Texas for real barbecue. That stuff that passes for BBQ in the Carolinas wouldn’t get a sniff from a dog in Texas. To start with, it’s only pork, so they are missing the best meat. Secondly, they slather it with vinegar, probably because the meat is so bad. Let me know next time you are out farther west, and I’ll treat you to the best barbecue money can buy. 🙂
[From Mr H] Texas barbeque is my favorite — brisket or sausage or preferably both. I’ve eaten it at Sonny Bryan’s, Kreuz Market, New Braunfels Smokehouse, New Zion Missionary Baptist Church, Colter’s, Salt Lick, County Line, Millers, and Black’s. Probably a bunch more I’ve forgotten. Next up: Corkscrew BBQ in a few weeks. I do like North Carolina hushpuppies and coleslaw, though, and the vinegar sauce adds a nice tang to the pork (but Texas beans, jalepenos, and potato salad win.) One of these days I’m going to have some Arkansas pie since I hear that’s the best.
Is there something that Epic cannot facilitate to win DoD contract? Is this why they are teaming with IBM? Curious to know thoughts as to why this partnership is necessary.
As for the IBM/Epic partnership:
The chances of an IBM/Epic partnership winning a DoD contract are ~80% but the chances of achieving a successful result in actual use by DoD and the VA together are less than 20%. A next generation VistA solution would be a better choice since it would reduce the training needs, give the current VistA users the opportunity to suggest improvements for the next version, and increase the likely hood of greater system efficiencies thus improving the overall treatment processes of both organizations.
TPD!
@Iamthewalrus My understanding, and it may be inaccurate, is that the winner of DoD bid will have to assume some significant liability in order to win the contract. The amount may be at a point where most vendors, outside of McKesson, Siemens or GE, could not absorb the liability on their own w/o potentially dissolving their company should that risk come to fruition. I believe this is a main driver for the joint bids (split risk), along with the consulting dollars that inevitably will come to this project.