Traditionally Professional Courtesy is something that physicians gave each other - but we had to be careful with it when…
Monday Morning Update 12/9/13
From Beyond the Legalese: “Re: revised Stage 2 timelines announced late Friday. What exactly does this delay mean? If we are a hospital that must attest to Stage 2 by end of fiscal year 2014, does this mean we now have until end of fiscal year 2015 for our first MU2 attestation year?” My impression is that the Stage 2 start date hasn’t changed, only the end date, so it’s not really a “delay” as much as it is an “extension” to make Stage 2 a three-year program. In that regard, I’m not sure the extension is cause for universal celebration since the 2014 dates remain unchanged for Stage 1 and Stage 2 – it’s really only Stage 3 that has been delayed. Feel free to leave a comment. CMS and ONC “announced” the change in a potentially obscure blog post late on a Friday without making supporting material available to clarify, but I expect they will provide more details. CHIME is already complaining that the 2014 start dates haven’t changed as it and other organizations wanted (nobody feels guilty about looking the taxpayer gift horse in the mouth, apparently.)
From The PACS Designer: “Re: smartphone overview. With the holiday season upon us, TPD thought it would be useful to post features of the smartphones currently available from various sources. As smartphones get more integrated into everything we do daily, it’s important to match the intended use with the right smartphone features, whether it be iOS or an Android system.”
Respondents are split on whether the FDA should regulate clinical software to any degree. New poll to your right: have you made a personal medical decision based on published hospital quality data in the past one year? I’ll admit that having worked almost my entire adult life in hospitals, I’ve never looked at the published quality data of local hospitals, including my own (although I’ve also never been hospitalized, so I had little motivation.)
I’ll be writing from the mHealth Summit this week. Drop by the microscopic HIStalk booth (#1305) and say hello if you are so inclined. The event has more than doubled in attendance since the last time I attended in 2010 and I’m hoping that the conference logistics have improved after HIMSS took it over from the National Institutes of Health.
Welcome to new HIStalk Platinum Sponsor Juniper Networks. A secure, reliable network is mandatory for EMRs, HIEs, telemedicine, PACS, high definition video, remote patient monitoring, real-time wireless location, and mobile clinicians. Juniper’s Healthcare Network Solution provides clinician access from any mobile device, secure access to patient records, a single user policy for all network points, and reductions in cost and risk via a unified wired and wireless infrastructure. Juniper’s WLAN solution provides the highest levels of reliability, scalability, management, and security to meet the needs of a mobile healthcare workforce. See “Top 10 Reasons Healthcare Prefers Juniper Wireless.” A case study quote from Juniper customer Lurie Children’s Hospital (IL): “We need to broker the complex relationship between stability and speed. We want to be able to put new applications on the network and adjust the network to meet the need. But on the other hand, we want to retain a stable network. We need a network that has very predictable behavior.” Juniper powers 60 percent of the world’s Internet transactions. Thanks to Juniper Networks for supporting HIStalk.
I found this new Juniper Networks video on YouTube.
Thanks to the following sponsors, new and renewing, that recently supported HIStalk, HIStalk Practice, HIStalk Connect, and HIStalk Webinars. Click a logo for more information.
Medicaid fraud is too common to be newsworthy, but not when foreign diplomats are involved. Among the 49 people charged with defrauding Medicaid of $1.5 million are dozens of Russian diplomats and their wives, who federal prosecutors say misstated their income to get Medicaid to pay their medical bills and then used the money for luxury vacations and helicopter rides. The government, of course, didn’t blame itself for happily paying the bills of non-citizens.
Nashville-based healthcare IT consulting firm eMids raises $13 million in funding.
Emory University Hospital (GA) uses IBM InfoSphere Streams real-time analytics and data acquisition software from Excel Medical Electronics to analyze ICU patient data in real time. If you want to play around with stream computing, there’s a free download of InfoSphere Streams.
Huntsville Hospital Health System (AL) chooses Caradigm Health Information Exchange to connect its affiliates. Caradigm signed a partnership deal earlier this year to market Orion Health’s HIE product.
A former Epic employee files a class action lawsuit against the company, claiming he and hundreds of other Epic quality assurance employees should have been paid overtime wages over several years. Epic disagrees, saying federal law is clear in classifying QA people as salaried rather than hourly.
Keith Seaman (Department of Veterans Affairs) joins VMware as chief technology executive for healthcare.
Saint Francis Health System (OK) chooses Epic.
Norton Healthcare (KY) reports that it has earned $12 million in HITECH payments in the third year of its $200 million, five-year Epic implementation.
Houston Methodist Hospital reports that a laptop containing the information of 1,300 transplant patient was stolen last week, but as is rarely the case when these announcements are made, the laptop was encrypted.
A 22-year-old woman sues a doctor, Northwestern Memorial Hospital, and the Feinberg School of Medicine (where the doctor is a pain management fellow) after he posts pictures of the woman drunk in the ED on Facebook and Instagram. The doctor also posted a Facebook invitation to join him for cocktails near the ED while waiting for the woman to recover from alcohol poisoning. He wasn’t actually her doctor – he came to the ED at the request of a mutual friend – and the hospital now claims he inappropriately accessed the patient’s medical records.
Illinois chiropractors consider going off the insurance grid and making patients pay cash due to high patient deductibles, medical coding issues, and the cost of software. According to one chiropractor, “The Affordable Care Act will make deductibles so high that people will soon be paying out-of-pocket for chiropractic medicine anyway. So why not go cash-only? This way, I can get rid of the headache of dealing with insurance companies, bring costs down for my patients, and get back to spending more time helping people.”
Ed Marx got a lot of responses to his “Identity and Leadership” CIO Unplugged post last week and has decided to delve deeper into the topic in the specific areas of titles and physical appearance. Watch for his next post.
The last 100 directory assistance operators in Connecticut will lose their jobs in February due to smart phones, which caused 411 calls to drop by 70 percent in the last three years.
Congratulations to those physicians (Dr. Jayne among them) who received notice Friday that they passed the exam to become board certified in clinical informatics.
Contacts
Mr. H, Inga, Dr. Jayne, Dr. Gregg, Lt. Dan, Dr. Travis, Lorre.
More news: HIStalk Practice, HIStalk Connect.



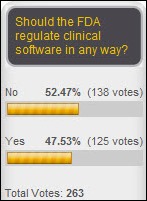
























“Respondents are split on whether the FDA should regulate clinical software to any degree.”
I read this to mean that about 1/2 of respondents hold enough concerns about the current safety and efficacy of HIT to warrant more than the status quo, while 1/2 are satisfied with the current lack of involvement by the FDA.
Cerner figured out this whole Employment Law issue.
The solution is very simple – go off shore.
https://recruiting.cerner.com/psp/hrprd/EMPLOYEE/HRMS/c/HRS_HRAM.HRS_CE.GBL?Page=HRS_CE_HM_PRE&Action=A&SiteId=7
The 850+ associates working in India represent a key component of Cerner’s overall strategy and are integral to the transformation of health systems around the world. India operations are set to experience significant growth as Cerner continues to develop the technology that will solve key challenges in global health care.
—
Wonder if this Epic kid doing the class action lawsuit dreamed it up on a Fiji beach while on his sabbatical. Or maybe the Taco Bell protests last week got him fired up in the spirit of justice.
If no jobs are good enough for us while we live on debt or break the bank with pensions we can’t afford, they’ll all move off shore. My gosh, when is a great job good enough?
Oh and anybody who doesn’t like the idea of American Stimulus dollars going off shore with Cerner and others should probably shut up and realize that much of Healthcare.gov was done off shore. Yup, your own government is struggling to figure out how to get things done in this country.
Dear Employment Law- offshore doesn’t work real well with agile development methodology-see all of Epic’s competitors for examples. And if you think he QA job at Epic is nice, why don’t you apply?
Wonder if Cerner having almost 1,000 staff doing their development in India will impact a possible DoD bid?
How on earth could we let even more American jobs go overseas funded by taxpayer dollars. Not to mention the security risks involved with having source code generated off shore in a country with less than stellar intellectual property track record.
Just a few subroutines to report out military readiness by region would be certainly helpful to foreign interests.
Re: Employment Law
“My gosh, when is a great job good enough?”
As a former Epic employee…when 60 hour weeks are the bare minimum to not get fired (and 70 will help you keep your head above water), you realize that a ‘great job’ leads to a terrible life and you would have been better off working nearly anywhere that does pay OT.
Re: “Board certified in informatics”
Now those lucky physicians can spend their time as board-certified-in-informatics specialists who the industry ignores, not just physician health IT amateurs who the industry ignores.
“Epic disagrees, saying federal law is clear in classifying QA people as salaried rather than hourly.”
The key difference is not salaried vs hourly, it’s exempt (from overtime regulations) vs non-exempt (from overtime). A salaried employee who is not exempt from overtime regulations is still entitled to overtime pay for hours worked over 40 hours. So while it is up to Epic’s discretion whether to pay their employees hourly or a salary, the fact that they can pay employees a salary does not necessarily mean the employees are exempt from overtime pay.