Amazing that the takeaway is that its easier to buy a gun than to get credentialed as a physician is…
News 10/30/15
Top News

Rep. Tammy Duckworth (D-IL), a former Army helicopter pilot who lost her legs when her Black Hawk took rocket-propelled grenade fire in Iraq, joins several other members of Congress who are fed up that the VA and Department of Defense still haven’t integrated their systems. Lawmakers are reviewing VA-DoD progress in a joint hearing of two House committees this week. Duckworth says that as a former VA employee, she regularly saw the DoD stonewall the VA’s projects in defending its turf. She’s also still mad about her first VA visit where she was asked to take her clothes off to prove that she was still an amputee since the VA wasn’t allowed to accept her DoD medical records, to which she replied to the physician assistant, “I’m not a gecko. They don’t grow back.” Chris Miller, who runs the DoD’s DHMSM project, testified that connecting the VA with DoD is harder than it seems, while the GAO’s IT director observed that her watchdog agency still doesn’t understand why the DoD and VA decided not to build a single system together in the first place. The GAO still wants that answer, but says that neither the VA nor DoD are responding to its inquiries. The GAO suspects that the VA and DoD have spent more than billion dollars in trying and failing to share information, which doesn’t even include the countless mega-billions of taxpayer money that was spent building and supporting their systems.

Speaking of the VA-DoD imbroglio, some members of Congress are convinced that the only way to get the VA and DoD play nicely together is to have the President personally make them. Rep. Dan Benishek (R-MI) says of his peers, “We can’t stand the fact that we’re spending a billion dollars on integrating healthcare and you tell us it can’t be done. We get sick of this.” DHMSM’s Chris Miller says the organizations weren’t ready in 2011 because while the IT part is easy, nobody wanted to address the people and process issues. He opined that interoperability is worse in civilian healthcare, raising the ire of Rep. Gerry Connolly (D-VA), who scolded him by saying that both agencies deal with a specific population but “can’t get their acts together on behalf of the men and women we’re serving.”
Reader Comments

From Don’t Mess with Texas: “Re: vendors pressuring clients. I heard that the day Texas Health Resources issued its press release blaming Epic for its improper treatment of its Ebola patient, Judy and Carl flew to THR that night to pressure the CEO into putting out a retraction, which they did. Epic plays hardball – they’ve done it at our site, too. I don’t blame Epic for being unhappy with the press release, and while veteran CIOs like me knew to take the release with skepticism, flying down in person to get a retraction is pretty heavy handed. I’m sure Epic’s spin is that they care so much for their clients that they wanted to show up in person and offer their help.” That entire process was bungled, although nothing in the THR recap describes a visit by anyone from Epic. THR leadership appears to have thrown Epic under the bus as a knee-jerk reaction without even talking to their own IT folks, who would have been involved with the configuration of the system that was blamed incorrectly (given their quick retraction) for missing their patient’s travel history. Any EHR vendor would have protested and asked for proof of their customer’s claim, although I agree that Epic is among the most vigorous enforcers of its own interests and I’m sure calls were made. THR wasn’t great at managing the Ebola virus, but it was much more aggressive in trying to manage the viral spread of unfavorable publicity.
From Uneasy Detente: “Re: vendor gag clauses. I’ve never seen them pre-loaded into one of my contracts, but I’ve signed a few with a major health IT software vendor as condition of contract settlement, where software doesn’t work and we refuse to go live, for example. The vendor may offer concessions or a refund conditional on signing a number of terms, which generally includes not going out and talking about the problem we’ve discovered. Here’s an example for your eyes only.” I can see why both parties would approve that condition given that they are reaching agreement on either a parting of ways or deciding not to implement a specific application. I’m on the fence about whether that’s a gag clause, but leaning toward no since the customer never actually went live. You would think that customers who did actually implement the application would see and report the same issue, but that’s wishful thinking. That leads us back to the same challenges we have with interoperability – as much as we as patients would like providers to publish and share information that might benefit us, there’s no incentive for those providers to do so and therefore they don’t bother. In fact, going public with software problems introduces the near-certain risk of creating an adversarial relationship with the vendor to which they’ve expensively hitched their wagon. I don’t know of any solution except maybe FDA-type oversight that requires companies to report the patient-endangering defects they discover. Just about any solution that requires providers – competing or otherwise – to voluntarily share information is not likely to succeed. Replace “providers” with “attorneys” or “car dealers” in the previous sentence to put it into a less emotional perspective.

From QM Employee: “Re: NextGen Hospital Solutions. Can anyone explain why QuadraMed acquired it? QuadraMed has not sold their current solution for three years and their product has so many holes (surgery, emergency, scheduling, etc.). There are constant layoffs and some really great employees have left. NextGen customers are in the under-100-bed hospital range and their product is unstable.” The Canada-based parent of QuadraMed (Constellation Software) seems to have broken its own acquisition rules in buying both QuadraMed and NextGen Hospital Solutions since it claims to be interested only in companies that are #1 or #2 in their market, have at least “hundreds” of customers, and face “unimposing” competitors. I can see why QSI wanted rid of its failed hospital business, but agree that it’s puzzling why someone else would want it, although that brings up the strong possibility that it was basically given away just to eliminate distraction and appease torch-wielding QSI shareholders.
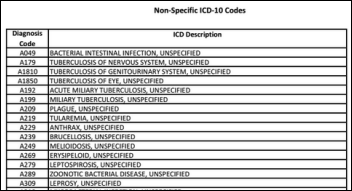
From Erstwhile ICD-9er: “Re: Georgia Medicaid’s stance on ICD-10 coding specificity. The CMS leniency was limited to Medicare. Medicaid was given the authority to make the decision for themselves. Georgia is the first to come out with aggressive messaging around their acceptance of ICD-10 specificity. An important distinction is that they related all of their ICD-10 edits for UB claims, but are holding firm on CMS 1500 claims. They have posted notice of this to providers along with a list of codes that will likely be denied. They are accepting feedback from providers about which codes should be accepted.” Thanks for that clarification.
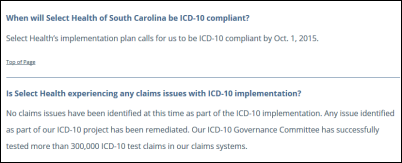
From Kilt Lifter: “Re: ICD-10. Select Health Medicaid in SC refused to do any user testing prior to implementation. They are now telling practices they will not pay any claims until the end of November at the earliest.” The company’s ICD-10 FAQ page brags confidently about their testing, remediation efforts, and overall readiness for October 1.
From Public Health Helpful: “Re: public health. I’m a long-time HIStalk fanboy, but you hit it out of the park with your comment that we ‘irrationally celebrate advancements that are very narrow in scope.’ We should be doing what will benefit the most people in the most significant way – immunizations, blood pressure control, weight loss, cancer screening, following preventive guidelines, and using proven treatments.” The only way to fix “healthcare” is to embrace public health as other countries have done rather than tinkering with how we deliver reactive health-related interventions. We don’t like thinking about that because it requires uncomfortable discussions about social services and the role of government that quickly degrade into political divisiveness. It’s easier and much more profitable to focus on expensive interventions that benefit a small percentage of the population while the far larger population suffers (and drags down economic growth) with chronic conditions whose management standards are well known, just not well practiced by either providers or the patients themselves. We have all the knowledge we need to make the country healthier and therefore more economically competitive, just not the will to use it.
HIStalk Announcements and Requests

I put the $750 raised by Dana Moore’s Epic vs. Centura basketball game to immediate use, applying matching money from my anonymous vendor executive as well as from other charitable organizations to fund these DonorsChoose projects:
- A document camera for Mrs. Marler’s third-grade class in Phenix City, AL.
- A video camera and accessories for recording advanced placement calculus and physics lessons so that absent students can review them later for Mr. Blachly’s high school class in Indianapolis, IN.
- A STEM bundle for Ms. W’s elementary school class in Englewood, NJ.
- An iPad Mini to support STEM studies in Mrs. K’s middle school class in Brooklyn, NY.
- Four science activity tubs for Mrs. N’s elementary school class in Dothan, AL.
- Two tablets for Ms. S’s first grade class in East Haven, CT.
- A laptop and accessories for Ms. M’s class of eight emotionally disturbed first grade boys in South Bronx, NY.
- Hands-on materials for Ms. M’s advanced placement statistics seniors in Denver, CO.
This week on HIStalk Practice: The wave of physician "Just Say No to Meaningful Use" movements rolls on. American Well digs further into the employer market. AdvantageCare Physicians achieves Stage 6 EHR adoption. ZocDoc and Kareo top the list of US-based deals with Q3 VC funding. A GAO "sting" results in further Healthcare.gov scrutiny. The Interstate Medical Licensure Compact Commission meets for the first time. Maine ups its healthcare price transparency efforts.
This week on HIStalk Connect: the FDA releases its inspection findings from an unannounced visit to Theranos, concluding that their nanotainer technology is an uncleared medical device. IBM Watson will debut on the Apple Watch in 2016 within a patient engagement app being developed by Welltok. Carnegie Mellon University researchers create an app that uses iBeacon technology to provide navigational support for blind users. The team behind the app hopes to add facial recognition features in the coming years. HealthTap launches a suite of new patient engagement apps in a bid to move into the enterprise healthcare space.
Webinars
November 11 (Wednesday) 2:00 ET. “Trouble Upstream: The Underinsured and Cash Flow Challenges.” Sponsored by TransUnion. Presenter: Jonathan Wiik, principal consultant, TransUnion Healthcare. The average person spends nearly $15,000 per year on healthcare as deductibles keep rising. Providers must educate their patients on plan costs and benefits while controlling their own collection costs by using estimation tools, propensity-to-pay analytics, and point-of-sale collections. This webinar will highlight industry trends in managing underinsured patients and will describe ways to match patients to appropriate funding.
November 12 (Thursday) 1 :00 ET. “Top Predictions for Population Health Management in 2016 and Beyond.” Sponsored by Medecision. Presenters: Tobias C. Samo, MD, FACP, FHIMSS, CMIO, Medecision; Laura Kanov, BS, RRT, MBA, SVP of care delivery organization solutions, Medecision. With all the noise and hype around population health management, the presenters will share their predictions for 2016 and their insight into meeting the mounting pressures of value-based reimbursement and the tools and technology needed to manage care delivery.
Contact Lorre for webinar services. Past webinars are on our HIStalk webinars YouTube channel.
Acquisitions, Funding, Business, and Stock

McKesson announces Q2 earnings: revenue up 10 percent, adjusted EPS $3.31 vs. $2.79, beating Wall Street expectations for both. The company raised guidance and announced an additional $2 billion in share repurchases. Technology Solutions revenue dropped 6 percent, much of that due to “our decision to exit the Horizon hospital software business,” with good performance from payer solutions and RelayHealth.
Theranos continues its fascinating, overly defensive implosion by eliminating seven of its 12 board member positions – including those held by Henry Kissinger and George Shultz – but creating a new board of counselors (which includes all of the old board members) and a medical advisory board. CEO Elizabeth Holmes claims the changes were made in July, although as in the case of the company’s proprietary lab methods, she provides no data to back up that assertion. The company’s new board includes Holmes, her COO, a billionaire who inherited his grandfather’s construction business, a retired general, and a wealthy lawyer who sues big companies. Some speculate that the departed board members wanted to distance themselves from the company and any potential litigation that may result. Meanwhile, Theranos, which has already raised $752 million, authorizes new shares that will value the company at over $10 billion, although that happened right before the critical Wall Street Journal came out.

Leidos reports Q3 results: revenue up 2 percent, adjusted EPS $0.71 vs. $0.65, beating expectations for both.
Sales

Carilion Clinic (VA) chooses Sagacious Consultants, now owned by Accenture, for revenue cycle improvement.
People

Timothy Johnson, DO, MMM (Children’s Mercy Integrated Care Solutions) joins Valence Health as SVP of pediatrics.

Ingenious Med names Scott McClintock (Have Marketing, Will Travel) as chief marketing officer.

Corepoint Health names Dan Simenc (3M HIS) as sales VP.
Announcements and Implementations
Analysis by The Advisory Board Company finds that hospitals are increasingly implementing CDC-recommended antibiotic stewardship programs to reduce inappropriate use, but many of them are too short on staffing and data to be effective. Most organizations have pharmacists rather than the prescriber review orders, most don’t record monitoring overall antibiotic use by prescriber, and few have adequate data to determine whether their programs are improving patient outcomes.
UV Angel announces an ultraviolet-powered patient room IT device disinfection system that automatically runs a cleaning cycle up to 40 times per day when it detects that a targeted device has been used.
Atlantic Medical Imaging (NJ) goes live on patient self-scheduling from OpenDr.
Hackensack University Medical Center (NJ), which self-styles itself with the annoying one-word nonsense of “HackensackUMC,” will integrate Gauss Surgical’s iPad-powered Triton blood loss estimation system with Epic.
Government and Politics
A study finds that the FDA is approving cancer drugs based on short-term patient response rather than their effect on overall survival, with the agency often neglecting to require manufacturers to perform the post-marketing studies that FDA required as a condition of approval. That means many of the most expensive and most important drugs on the market haven’t proven that they actually work, which has been a problem with oncology drugs for decades – drug companies, oncologists, and hospitals make tons of money pumping them into patients with soothing optimism but no guarantee that the patient will live longer or better.
While deaths from overdoses of heroin and prescription narcotics are skyrocketing – the former because addicts are switching from expensive and heavily marketed prescription drugs to cheaper heroin – 80 percent of addicts couldn’t get treatment even if they wanted it because capacity is lacking. I was talking to a first responder the other day who said exactly the same thing – in his tiny, rural town, heroin deaths are common since addicts can buy it on the street for a few dollars per dose vs. the high cost (no pun intended) of oxycodone and other prescription narcotics. The so-called war on drugs has been lost as prisons and morgues fill up and suppliers get even richer as reduced availability drives up prices (a lesson possibly learned from their legal but equally morally challenged pharma counterparts). As usual, these studies are coming from public health experts (Johns Hopkins Bloomberg School of Public Health in this case) since it’s not considered a healthcare or medical issue that provides a business opportunity.
The Department of Justice arrests the former president of drug maker Warner Chilcott, owned by Allergan, for conspiring to pay kickbacks to doctors who prescribed its drugs. The company will also pay $125 million in fines and plead guilty to criminal charges. Meanwhile, Ireland-based Allergan and competitor Pfizer begin merger talks in what would create the world’s biggest drug company with a combined market value of $340 billion, making that $125 million fine look like a valet tip. It would also provide a way for US-based Pfizer to dodge US taxes in declaring the headquarters of the newly created company to be Ireland.
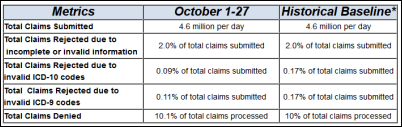
CMS announces that it’s been a quiet October for ICD-10, with the number of claims submitted due to incomplete or invalid information remaining unchanged at 2 percent. The denial rate and percentage of claims rejected due to invalid ICD codes also hasn’t changed much. It a bit early to declare ICD-10 victory, but CMS seems to have defied the naysayers who didn’t believe its optimistic testing status reports.
Other
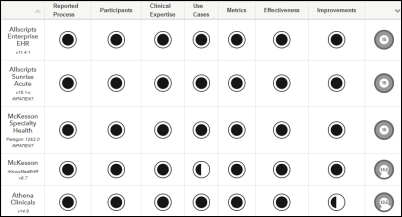
The AMA and MedStar Health publish their review of EHRs for user-centered design, which instead of looking at actual user usability or testing anything against standards, simply reviewed ONC’s certification test results for use of best practices. The top-scoring products were Allscripts Enterprise, Allscripts Sunrise, McKesson Paragon, McKesson IKnowMed, and Athena Clinicals. Bottom-scoring products are EClinicalWorks Version 1.0, Dr Systems, Greenway PrimeSuite, Epic EpicCare Ambulatory, and NextGen Ambulatory. The analysis used factors such as the vendor’s self-reported UCD process, the involvement of clinicians in testing, and the design of rigorous use cases for testing. It’s a puzzling list when the ancient Meditech Magic finishes one spot behind Cerner in the top 10. I also wonder how meaningful it is to critique user-centered design process by repurposing certification submissions for individual products – you would think a given vendor would use the same design and testing methods for all of their products. The end result will be what it always is in healthcare IT: the top-ranked vendors will brag loudly about the results while glossing over the methodology and applicability, while the low-ranked ones will criticize the methodology and applicability while glossing over the results.

Santosh Mohan, a management fellow at Stanford Health Care and long-time HIStalk reader, sent over this photo if the IT department’s Halloween celebration, in which the three folks above are dressed up as the (a) electronic (b) medical (c) record. I like subtle humor like this because once you get it, you can feel superior in imagining folks who didn’t get the joke.

Meanwhile, PatientSafe Solutions tweeted out this photo of its team. It brings back not-so-fond memories of my hospital’s IT department Halloween celebration, which despite featuring nothing more interesting than pumpkin bowling and orange-iced cupcakes, had to be renamed to the politically correct “fall festival” when a couple of employees complained that it celebrated devil worship.
Weird News Andy cries, “Bring out your dead” as he reads how New York’s health insurance exchange enrolled 354 dead people for health insurance, paying out $325,000 in claims to 230 of them. Design flaws, including people having multiple identification numbers, caused another $3.4 million in overpayments in the program’s first year.
Sponsor Updates
- Healthcare Data Solutions publishes a white paper titled “Understanding the Opportunities & Challenges of Telehealth 2015.”
- Impact Advisors sponsors an article titled “A Unique Approach to Business Analytics: The Scottsdale Institute Health IT Benchmarking Program.”
- Stella Technology and DataMotion will participate in the interoperability showcase at the New Jersey and Delaware Valley HIMSS chapters conference in Atlantic City October 29-30.
- InterSystems CEO Terry Ragon is featured in MIT’s Spectrum Magazine.
- PDR and Leidos Health will exhibit at the NextGen User Conference November 1-4 in Las Vegas.
- LiveProcess will exhibit at the New England Rural Health Round Table November 5-6 in South Bridge, MA.
- Wellcentive CEO Tom Zajac will present at the inaugural meeting of The Leader’s Board for Population Health Management November 5 in Dallas.
- MedCPU is recognized as one of Entrepreneur’s “Best Entrepreneurial Companies in America.”
- Navicure will exhibit at Michigan MGMA October 30 in Mount Pleasant.
- Recondo Technology and Sutherland Healthcare Solutions will sell each other’s solutions.
- Over 1,000 health and human services leaders attended Netsmart’s Connections 2015 client conference, which featured mental health advocate and former Congressman Patrick J. Kennedy.
- NTT Data will exhibit at the 2015 LeadingAge Annual Meeting and Exposition November 1-4 in Boston.
- Obix will exhibit at the 14th annual Perinatal Conference November 5 in Dublin, OH.
- Epworth Eastern Hospital (Australia) realizes improved outcomes with Oneview interactive patient care technology solutions.
- PerfectServe will exhibit at ASN Kidney Week November 3-8 in San Diego.
- The SSI Group will exhibit at the Georgia HFMA Fall Institute November 4-6 in Savannah.
- Streamline Health will exhibit at the Health IT Leadership Summit November 3 in Atlanta.
- Surgical Information Systems will exhibit at HealthAchieve 2015 November 2 in Toronto.
- Surescripts will exhibit at the NextGen 2015 user group meeting November 1-4 in Las Vegas.
Blog Posts
- Population Health: Not a One-Size-Fits-All Endeavor (Medicity)
- Building Your Breach Resistance First Line of Defense (ID Experts)
- Three Things Images Need to Do to Be Interoperable (LifeImage)
- They Like Us, They Really Like Us (MedAptus)
- Growing, Teaching: a Way of Life at Nordic (Nordic)
- Population Health: Where the Rubber Meets the Road (Orion Health)
- Communicate smarter, not just more often (PatientSafe Solutions)
- Four ways to prepare for next year’s price transparency dialogue with patients (Recondo Technology)
- Inspiring Newport (PatientKeeper)
- Secure Texting Trends: The Benefits of Patients, Physicians & Healthcare Orgs (Practice Unite)
- Accurate Provider Information is Essential for Operational Efficiency (Phynd Technologies)
- Predictions of Apple Q4 Earnings from Medical Charge Capture and Secure Messaging Users (PMD)
- More States Revise ePrescribing Regulations (Point-of-Care Partners)
- Three Weeks into ICD-10: Seven Areas to Watch in the New Frontier (Sagacious Consultants)
- DV-NJ HIMSS Conference Interoperability Showcase: Quality Control Score for C-CDA Delivery Services (Stella Technology)
- GeneInsight Clinic at Brigham and Women’s Hospital (Sunquest Information Systems)
Contacts
Mr. H, Lorre, Jennifer, Dr. Jayne, Dr. Gregg, Lt. Dan.
More news: HIStalk Practice, HIStalk Connect.
Get HIStalk updates.
Contact us or send news tips online.




Totally cool! Mr H got to do company sponsored devil worship!
Curious choice of words in regards to Meditech Magic’s rating relative to Cerner when Meditech continues to this day making enhancements to the platform and adding new modules on a legacy system. In reality isn’t Cerner simply doing the same thing to technology that isn’t exactly modern in today’s software world? Magic is certified for Stage I and II which as we know are not ancient standards but current ones. Are studies designed to prop up conventional wisdom or to flesh out the actual realities?
MEDITECH C/S 5.66 also had the same score as Athena Clinicals at 13.5 to also be considered a “top-scoring product”.
Regardingt the VA and DoD. Why don’t we give all service members Medicare primary and a supplement specific to the needs of the service members (active, retired, etc…) and we can have the supplement process at 100% or some % of the remaning Medicare co-insurance, deductible, etc…? VA hospitals can be sold to the highest bidder and people in the military can choose their provider of choice.
Regarding public health, and Mr. H’s comment “The only way to fix “healthcare” is to embrace public health as other countries have done rather than tinkering with how we deliver reactive health-related interventions.”: I think this is right on the money, literally and figuratively. I found this profile on how Montefiore in NY does things very interesting. It appears to be a cheapskate but very effective approach:
https://www.advisory.com/research/population-health-advisor/case-study/montefiore-medical-center
It portends deeper vertical integration for integrated delivery organizations.
This whole usability publishing is a scam.
http://www.medicalhumanfactors.net/consulting-services/#q={}
This company actually consults with vendors on usability.
Keep digging and you’ll find something interesting here.
Just a thought. I enjoy reading how donations are helping students and teachers. Possibly for the holidays, you encourage all of us, a little more, to give. Those of us in HIT are very fortunate.