Netflix and Reed Hastings: Ghost of Christmas Past
By Chuck Dickens
As the countdown to Christmas 2022 ticks away, Reed Hastings sits alone in the dim basement of his parents’ house, lost in the immersive world of video games. But the monotony of his day job at Blockbuster weighs heavy on his mind.
Every day, he dutifully rewinds VHS tapes and updates spreadsheets, tracking the $5 fines for customers who neglect to rewind their rentals. It’s a tedious task, but it’s a necessary one. After all, late fees and rewind fines are the company’s second-largest source of profit, surpassed only by the seemingly endless stream of “Die Hard” rentals that pour in every holiday season.
But just as Reed finishes his fifth cup of coffee, something strange happens. A shimmering light appears out of nowhere, coalescing into a humanoid form that seems to float effortlessly in the air. For a moment, Reed is startled, but then he recognizes the ghostly figure as the Ghost of Christmas Past, as depicted in countless retellings of “A Christmas Carol.” With a jolt, he’s suddenly transported back to 1997, reliving the excitement of a disruptive new idea that once seemed destined for greatness.
After cashing in on the sale of his software company, Reed was on the hunt for his next big opportunity. He wanted something innovative and disruptive, and he had his sights set on the movie rental industry.
In 1997, movie rentals were a major form of entertainment in the United States, with most employers offering them as a employment benefit and the government eventually extending the perk to everyone over the age of 65. As a result, movie theaters dwindled in number, and the rental market was dominated by a few large players such as Blockbuster and Hollywood Movies.
But after paying a hefty late fee to Blockbuster for “Apollo 13,” Reed began talking to his friend Marc Randolph about the frustrating experiences they and their friends and family had had with the rental giants. The local store had limited titles, and the popular ones were often unavailable. Even though movie rentals were offered as a benefit, the co-pay was still substantial, and if customers wanted to drive to a different location to find a specific movie, they had to pay extra out of pocket.
Determined to bring a better rental experience to customers, Reed and Marc came up with the idea for Netflix. The company that would offer DVDs by mail for a low, fixed monthly fee, with no late penalties, a vast selection of movies to choose from, and fast turnaround time. They were confident that their service would revolutionize the industry and put an end to the frustrations of traditional rental models. They were so convinced of the superiority of their service that they invested a large part of their own money in addition to VC funds to get the company off the ground.
But by next Christmas, as Reed and Marc struggled to scale up their business and delved deeper into the movie rental market, they discovered a number of strange quirks and injustices.
The compensation paid to movie industry professionals was set by a committee (Relative Video Unit Update Committee – RUC) that was largely composed of people involved in a genre called “film noir,” who claimed that these films were the most expensive to produce and should therefore be paid the highest rates. This left other genres such as romantic comedies, which were popular with customers but low on the payment scale, struggling to find funding and talent.
Another example was that every time a movie was rented, Blockbuster used a special code to designate the genre of the movie and other details. These codes eventually determined who got paid how much for the rental. Not only did the American Movie Association (AMA) controlled who got paid, but they charged everyone a licensing fees to use the code set itself in a classic case of double-dipping.
Additionally, the distributors were owned by Blockbuster and Hollywood Movies. They negotiated with movie studios and employers to determine which movies would be made available and at what rental price. Since everyone got a percentage of the rental price, lowering the rental price wasn’t in anyone’s business interest collectively. Further, government was not allowed to negotiate late fees and penalties, as it was prohibited by law (American Movie Association and American Hollywood Association had strong lobbying arms).
From the very beginning, Netflix faced an uphill battle in convincing consumers to sign up for its flat fee subscription model. Many people received movie rental benefits through their employer and weren’t willing to pay for Netflix out of pocket. And while the company’s vast library and lack of late fees were appealing, people were hesitant to trust a new company with such a crucial part of their entertainment.
Netflix tried to appeal to employers, offering to provide subscriptions as a benefit to employees, but benefits managers were resistant due to long-term contracts with established rental companies like Blockbuster and Hollywood Movies. As for other charges, such as late fees and facility fees — to compensate them for higher operational expenses of a physical location – Blockbuster and Hollywood Movies had arranged it so that those charges were paid directly by the employer and people never perceived those being charged to them, even though indirectly, it was all coming out from their paychecks and taxes.
Undeterred, Netflix approached Blockbuster and Hollywood Movie (because everyone said that that’s where the money was) with the idea of using their advanced technology to lower the cost and improve the availability of movie rentals. But they were met with laughter and derision, as the traditional companies saw higher costs as a way to increase revenue.
Despite this, Reed and Marc remained convinced that technology could be a game-changer for their company. So when their engineering team came up with the idea of streaming movies directly into living rooms all over the country, they were thrilled. However, they quickly realized that employers and the government wouldn’t pay for these streaming movies. Regulations prohibited them from streaming across state lines, requiring them to set up streaming centers in each state and significantly increasing their costs.
But even with these setbacks, Reed and Marc were undeterred. They saw the potential for incorporating AI into their streaming service to create an even more attractive offering. As Christmas Eve 2007 approached, they had signed up a few thousand direct subscribers, mostly in affluent communities, and a few progressive employers were conducting pilots with their service. Despite the challenges they faced, they remained convinced that they were on the cusp of something big.
Despite its advanced technology and AI, Netflix struggled to overcome the stranglehold of monopolies and regulations in the movie rental industry. For over two decades, the company barely made a profit and continued to hemorrhage money.
But in the winter of 2020, everything changed. A global pandemic swept the world, forcing people to stay at home and closing down stores like Blockbuster and Hollywood Movies. In response to widespread discontent, the government allowed nationwide streaming of movies and set up a system to pay for it. Suddenly, Netflix was a household name, valued at billions of dollars despite still not turning a profit.
However, the success of the streaming service sparked a wave of competition, including from Blockbuster and Hollywood Movies, which created their own streaming video service with the help of their legacy IT vendor. As the pandemic waned and the traditional players saw their core business model threatened, they worked to regain the upper hand. They pressured the government to reinstate state-level restrictions on streaming and encouraged the movie industry to charge a “streaming fee” for on-demand movies.
By Christmas 2021, Netflix was deep in debt and Reed and Marc were forced to liquidate the company to avoid personal bankruptcy. They both moved back in with their parents and took jobs at Blockbuster and Hollywood Movies, which were thriving again thanks to government loans during the pandemic.
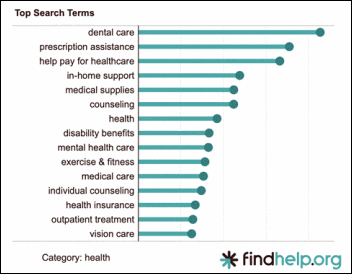
As he headed off to work at Blockbuster, Reed couldn’t help but wonder why the movie rental industry couldn’t use technology to improve customer service and reduce prices like other industries such as healthcare. In fact, at every innovation forum, people kept asking him, “Why can’t movie rental business be innovative like healthcare and be agile at adoption of technology?”
“Because healthcare is not insanely regulated and doesn’t have government and private monopolies to distort the market and incentives like the movie rental business,” he muttered to himself, recalling the Ghost of Christmas Past’s explanation. And with that, he set off for another day at the grindstone.







![image[6] image[6]](https://histalk2.com/wp-content/uploads/2023/03/image6_thumb.png)










Sounds reasonable, until you look at the Silicon Valley experience. Silicon Valley grew like a weed precisely because employees could…