Neither of those sound like good news for Oracle Health. After the lofty proclamations of the last couple years. still…
News 12/9/20
Top News

Canada-based long-term and post-acute care software vendor PointClickCare will acquire care transition notification startup Collective Medical for $650 million.
The companies have been partners for a little over a year.
The deal marks PointClickCare’s third acquisition in two years. It acquired Co-Pilot analytics from Consonus Healthcare in May and LTC EHR vendor QuickMar last year.
Salt Lake City-based Collective Medical, whose product is used in 20% of US hospitals, was valued at $170 million in its most recent funding round in 2017.
I interviewed Collective Medical CEO Chris Klomp a few months ago.
HIStalk Announcements and Requests
Today I learned about the “Texas sharpshooter fallacy,” in which an armchair expert mistakes a random clustering of data points as being indicative of a trend. The title refers to someone who shoots a bunch of random bullets at a blank wall, then paints a target around the tightest grouping to claim expert marksmanship. As with the cherry-picking sharpshooter, data similarities are stressed and exceptions are ignored. The most recent offenses involve COVID-19 and the election.
Webinars
December 15 (Tuesday) 1 ET. “Highlights from the 2021 CPT Code Set Update.” Sponsor: Intelligent Medical Objects. Presenters: June Bronnert, MSHI, RHIA, senior director of global clinical services, IMO; Shelly Jude, RHIA, RHIT, mapping manager, IMO. Top coding professionals will highlight the most important changes to the Current Procedural Terminology code set that take effect on January 1, including crucial additions, deletions, and revisions; how to communicate Official Coding Guidelines changes to the healthcare team; and a description of the impact that the code set update could have on practice.
Previous webinars are on our YouTube channel. Contact Lorre to present your own.
Acquisitions, Funding, Business, and Stock
Talkspace considers putting itself up for sale, leading analysts to speculate that an acquisition could value the online therapy app startup at $1 billion. It has raised $107 million since launching in 2012, and made its first acquisition — a couples therapy app — last year.
Verily co-founder Tom Stanis launches Story Health with $4 million in seed funding. The startup has developed software to enhance patient care between office visits, including virtual programs and analytics.

Cerner invests in Elligo Health Research and will use its technology to offer clinical trial opportunities to providers and patients. Allscripts has offered Elligo’s services since 2017. The company was awarded an FDA grant in October 2019 to work on real-world data harmonization for 21st Century Cures Act data sharing use cases.

I listened to the business overview by UnitedHealth Group CEO Dave Wichman at the company’s virtual investor conference, assuming that the strategy of a company that has a $330 billion market cap, that expects $277 billion in 2021 revenue, and that has penetrated every aspect of healthcare and insurance is worth hearing. Clearly UHG is targeting every profitable aspect of healthcare in a way that will turn the hospital industry on its ear and is leading the charge with its high-growth Optum business. UHG says it has 3.6 million customers covered by some degree of value-based care in 44 states and is pushing hard to move surgeries from expensive hospitals to ambulatory surgery centers. Points:
- Nearly every aspect of UHG’s strategy involves consumer technology, data, and AI, all of which it expects to lower costs, provide a better experience for patients and physicians, and expand affordable access. Wichman says that no country’s health system was strong enough to respond to COVID, but technology, information, and systems are now capable of showing how healthcare can evolve.
- An individual’s entire health history will live in the cloud, will be constantly updated by real-time systems, and will be backed by an AI-powered care team that will offer both virtual and face-to-face services in which evidence-based medicine will guide next-best-action and care plans.
- Everything will be on demand, such as flu meds stored in a remotely controlled lockbox, home IVs, and virtual help for stress.
- Doctors will be paid in real time for following science, while patients will be rewarded for their healthy behaviors.
- The company’s growth pillar 1 is to reinvent healthcare delivery via high-performing local medical practices that are paid for value-based care and backed by national support such as a digital clinical home, virtual primary care, analytics-supported telemedicine visits with your own doctor, house calls for seniors, home infusions, retail pharmacy, and digital pharmacy powered by analytics.
- Growth pillar 2 is pharmacy services, especially specialty pharmacy and direct-to-consumer offerings. The company has introduced daily dose packaging (similar to Amazon PillPack), home infusion, the Optum Store, digital pharmacy, and the opening of 60 retail dispensing sites.
- Growth pillar 3 is consumer-centered benefits, with wider choices and digital therapeutics and coaching for diabetes (again seemingly aiming at Telehealth’s Livongo business).
- Growth pillar 4 involves insights — digital scheduling, health record scaling, development of proprietary telemedicine, and use of AI in practice. The company has invested in 30 startups, most of them related to technology.
- Growth pillar 5 is health fin tech, such as digital payment and authentication for rewarding consumers and high-performing clinicians.
Sales
- Hampton Regional Medical Center (SC) will use consulting services from Engage for its Meditech Expanse implementation.
- Thriving Mind South Florida selects Netsmart’s CareManager population health software.
People

Eagle Telemedicine promotes Jason Povio to president and COO.

Richmond University Medical Center (NY) names Tom Pagano (Johnson County Community College) VP of IT and support services.

Johns Hopkins Health System names interim Sibley Memorial Hospital President and COO Hasan Zia, MD, MBA to the permanent role. He is an informaticist who served as Sibley’s CMIO from 2011 to 2015 and led its Epic implementation.
Announcements and Implementations
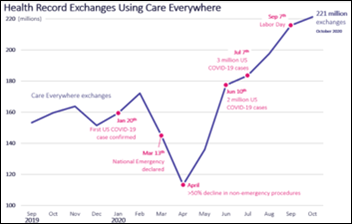
Epic’s Care Everywhere reached 221 million health record exchanges in October 2020, up 40% from the same period a year ago.
A Black Book survey names The HCI Group as the top rated health IT consulting firm for system-wide technology, innovation, and organizational digitalization strategy.
Avera Health goes live with Meditech’s Google Cloud-powered High Availability SnapShot to give clinicians access to patient data via a web browser during unexpected downtime.
COVID-19

In the UK, a 90-year-old grandmother gets the first shot of Pfizer’s COVID-19 vaccine. In the US, Pfizer’s vaccine cleared FDA’s safety and efficacy review on Tuesday, and if the company’s data is accepted in Thursday’s advisory committee review, the first doses could be administered by this weekend.
Monday continued the trend of every day setting new US COVID-19 records, with 180,000 new cases, 102,000 Americans in the hospital, and 2,204 seven-day average deaths.

HHS publishes COVID-19 hospital capacity data at the facility level on a weekly basis dating back to August 1. Previous data sets were compiled by state. A group of data journalists, data scientists, and healthcare system researchers who have reviewed the data have put together a FAQ.

California Governor Gavin Newsom announces that CA Notify — an app-based, COVID-19 exposure-tracking tool — will launch statewide later this week. The app was developed using technology from Google and Apple and was piloted at the University of California. Several regions across California have imposed stay-at-home orders through the holidays in an effort to alleviate virus spread. The state reached a single-day record of 34,000 new cases on Monday.
Meanwhile, a New York Times review notes that US consumers and state governments have shown little interest in using the Google-Apple COVID-19 smartphone exposure notification app that California is launching statewide. Only 13 states have developed their mandatory public health add-on to the app (it has since been made optional) and most of those states are seeing single-digit percentages of residents using them. Experts also note that people are loading the app to receive warnings of their exposure to infected others, but then refuse to allow the app to notify their fellow users when they themselves test positive.
COVID-19 vaccines have not been tested to see if they prevent transmission of coronavirus, meaning that people who have been vaccinated still need to wear masks because they could still be contagious. Nobody knows whether enough antibodies will circulate to the nasal mucosa to prevent its growth there, which is why some respiratory virus vaccines work better as nasal sprays.
Pfizer board member and former FDA Commissioner Scott Gottlieb, MD says in a USA Today interview that:
- The hardest 4-6 weeks of the pandemic are ahead of us, with COVID019 hospitalizations expected to peak in mid-January at up to 175,000 and 50,000 in the ICU.
- US deaths will reach 400,000 by the end of January during the infection’s final surge, with the situation improving in February and March as the virus will “largely collapse” and its major spread will end.
- Flu rates will likely drop sharply because the mitigation steps for COVID-19 are more effective in flu.
- Vaccine distribution will seem slow to people who are anxiously awaiting it, but supplies will be adequate by March to make it available to most people.
- Gottlieb urges the US to “get as many shots in arms as possible” in using available supplies immediately instead of holding the required second doses for January, when the virus will begin to decline.
- The vaccine will be effective if 50% of people get it instead of the previously accepted 70-80%, especially if follow-up studies find that it prevents viral spread.
- The summer’s big spread was surprising to experts, who didn’t predict that Southerners would congregate indoors under air conditioning or that the Sturgis motorcycle rally would be allowed to proceed and spread virus all over the Midwest.
- The federal government didn’t take an active role in the production of monoclonal antibodies, so supplies will be rationed and not widely available in the foreseeable future, a lesson that should be learned for future health issues.

The CDC’s text messaging system that COVID-19 vaccine recipients can voluntarily use to report side effects — which was developed by Oracle and HHS as part of Operation Warp Speed — contains security vulnerabilities, experts say. Anyone who gets the QR code that is contained in the patient immunization kit – such as when it is discarded — can file false reports to the V-safe system that would need to be evaluated. The federal government issued a $2.3 million contract to an IT company to process the incoming reports.
Experts warn that otherwise careful workplaces are exposing their employees by allowing them to socialize and eat together in break rooms, as happened in Mayo Clinic.
More than half of surveyed Fire Department of New York union members say they will not get a COVID-19 vaccine if the department offers one, even though their jobs make them 15 times more likely to be infected.
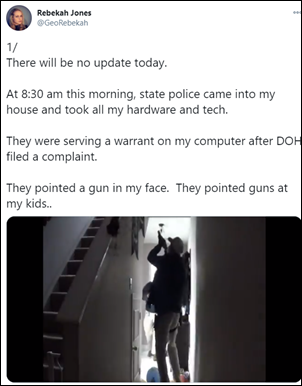
Florida state police raid the Tallahassee home of Rebekah Jones, a former state data scientist who was fired in May for insubordination following what she says was her refusal to manipulate data to make Florida’s COVID-19 dashboard data look more favorable for reopening as Governor Ron DeSantis was urging. The state’s health department says someone using the Comcast IP address of Jones logged in to its emergency messaging system on November 10 to send messages that were critical of the state’s response. Ten armed FDLE agents entered her home and, according to Jones, pointed pistols at her husband and two children before seizing her computer equipment. The incident was recorded on her home’s security camera. The state FDLE says that Jones refused to open the door and that weapons were not pointed at anyone.
Other

Greater Baltimore Medical Center deals with a ransomware attack that forced it to take down several of its IT systems on Sunday. Reports suggest the ransom note came through a fax machine (!!), demanded a response within three days, and provided contact information using the Dark Web.
Sponsor Updates
- Access releases a new Access Points Podcast, “Blending in with a New Team.”
- IDC MarketScape includes Arcadia in the Leader category in population health analytics in its “US Population Health Analytics 2020 Vendor Assessment.”
- OptimizeRx integrates Komodo Health’s Healthcare Map with its digital health savings and educational content software to enhance clinical decision-making at the point of care.
- CareSignal develops AI to improve patient engagement.
- New England Venture Capital Association names Kyruus the winner of its 2020 Powerhouse Healthcare Company Award.
- Cerner releases a new podcast, “The value of preparing for innovation.”
- Team members from The Chartis Group share “Lessons from the Pandemic.”
- Clinical Architecture releases a new Informonster Podcast, “The Impact of Logica and How the Healthcare IT Industry Can Come Together, Part 1.”
- Dimensional Insight publishes a new white paper, “Staying Ahead of COVID-19 with a Data-Driven Response.”
- Ellkay exhibits at the virtual Node.Health Digital Medicine Conference through December 11.
- Black Book gives several HIStalk sponsors top consulting rankings, including Bluetree (Epic implementations), Hayes (RCM optimization, hospitals), Impact Advisors (enterprise resource planning), and The Chartis Group (value-based care transformation and strategy, hospitals).
Blog Posts
- Physician Burnout (314e)
- Mobile readiness is a must-have for scheduling software (Ability Network)
- 3 Things That Might Be Preventing Your Patients From Using Telemedicine (AdvancedMD)
- Clinica Universidad de Los Andes, Chile: Transition Project to Enterprise Imaging (Agfa HealthCare)
- The 21st Century Cures Act: Updated Deadlines and Considerations for Payers (Bluetree)
- The Cleveland Clinic: Leveraging CarePort to Achieve BPCI – A Success (CarePort)
- Moving Patients In, Out, & Around the Health System: How Central Logic is Transforming Care Transitions (Central Logic)
- Why Parents Love Working at CoverMyMeds (CoverMyMeds)
- Connecting to the Home? Put People Front and Center (Dina)
- Kiosk, HEDIS, and More: Welcoming Patients to the Medical Landscape (EClinicalWorks)
- 5 Forces for the Future: Accurate and actionable data across care settings becomes the currency of the new health ecosystem (Wolters Kluwer Health)
Contacts
Mr. H, Lorre, Jenn, Dr. Jayne.
Get HIStalk updates.
Send news or rumors.
Contact us.



Here is my UHG call summary for big healthcare providers. UHG knows they can do the procedures you make your money on. They know they can do them much cheaper and they actually know exactly how much cheaper.
They need to get between you and the patient to direct them to that cheaper service. They intend to do that in a couple ways. First, they intend to be much more convenient for the patient. They want to be the getting an Uber to your calling a cab. Second, they want to track the patient through time and intercept them at the right moment to get them to cheaper care. The first is possible and happening as we speak. The second is harder within the current healthcare landscape.
Re: UHG. They already employ or are affiliated with over 40k physicians, so they need to work with those physicians to refer them to specialists that are aligned with Ambulatory Surgery Centers UHG is building out.
The second part – identifying patients to redirect them to intervene — is not as difficult to do when you have patient history and lagged claims submission. The current healthcare landscape is diffuse, but it all goes to the payer, and UHG has building the technology to put them together for awhile.
True. The quality of that data is quite bad from what I’ve seen. The complexity of that intervention is also hard to scale.
Internet advertising has a similar model of collecting data then trying to deliver an intervention. It is really hard. People get toaster advertisements right after they bought the only toaster they will use for a decade. The successes seem to come when a company dumps a ton of money into buying ads for when someone searches or buys something even remotely related to the companys product. New toaster means you get a ton of appliance ads and some targeted consumers actually did move and the company snags a few more sales. UHG can’t spam their members without driving up utilization and destroying their margins.
Re: UK vaccinations. Fun fact: William Shakespeare was the second person to receive the vaccine in the UK, prompting a plethora of puns and witticisms. A favorite tweet: “Actually I heard the second person to get the vaccine was Christopher Marlowe but William Shakespeare took all the credit.” #TamingoftheFlu
https://abc7.com/shakespeare-vaccine-william-covid-great-britain-coronavirus/8619062/
I had the unfortunate “opportunity” to visit the ER as a patient at Greater Baltimore Medical Center twice in the past week – once prior to the ransomware attack and once after. I was pleasantly surprised to find that there was no obvious difference in care between the electronically-enabled visit and the paper-based visit – both were excellent. Also surprising was that not a single staff member used the excuse “sorry, our computer systems are down” and we didn’t experience any delays in care – even though it appears that almost all of their electronic systems are down: at a minimum the Epic EHR, lab system, and their HR/payroll systems. The only time we saw a computer used was for check in and printing ID bands. Kudos to GBMC as it was obvious they were prepared for this. We walked through the downtime command center where I saw an HR station for dropping off time sheets, a clinical station with plentiful stacks of every form, and a wall of giant sticky notes with schedules and protocols including shift sign ups for taking on specific down-time roles include Runner and Safety Nurse – complete with a rack of different colored safety vests that had those roles printed in big letters on the backs. Sadly this situation seems to be more common so it was reassuring as patient that they still seemed to be maintaining safe and effective operations.