Sounds reasonable, until you look at the Silicon Valley experience. Silicon Valley grew like a weed precisely because employees could…
Monday Morning Update 6/22/20
Top News

In Russia, President Vladimir Putin calls for the healthcare system there to roll out out digital systems and to use artificial intelligence.
Putin told health workers in a videoconference that Russia should use its experience in successfully addressing coronavirus to improve the overall reliability of its healthcare system.
Reader Comments
From Options Exercise Program: “Re: PatientPing’s delayed funding announcement. If you’re going to disclose a raise, make it timely. When public companies do this, we (the investor research community) used to call it ‘painting the tape.’ It matters because the backdrop between now and then is very different. Raising the money during this current time (COVID) sends a very different signal of optimism than it did when the raise occurred. Same quarter plus or minus is fine, but not 16 months.”
HIStalk Announcements and Requests
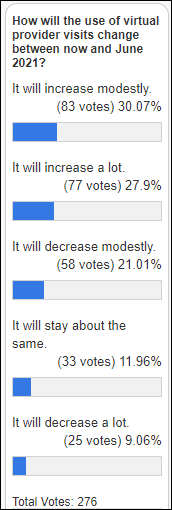
More than half of poll respondents expect the use of virtual provider visits to increase in the next year over today’s already-increased levels, although two commenters correctly observed that the challenges are not related to technology limitations, consumer or provider preference, or clinical outcomes – it’s all about payments by CMS and insurers.
New poll to your right or here: For those who have had a recent telehealth visit: how was pre-visit information (allergies, meds, recent history, current problem, etc.) collected?
Listening: new from Travis, a Scotland-based (“Glaswegian,” a new word to me) indie band that has been around for 30 years. They couldn’t make a video for the new tune because of coronavirus lockdowns, so singer Fran Healy and his son drew their own.
Webinars
None scheduled soon. Previous webinars are on our YouTube channel. Contact Lorre to present your own.
People


Arcadia promotes Debbie Conboy to VP of risk adjustment and quality products and hires Catherine Turbett, MHA (Lumeris) as VP of ACO and health plan account operations.
Announcements and Implementations
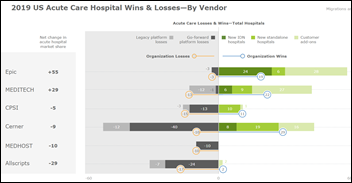
KLAS didn’t send me its “US Hospital EMR Market Share 2020” report, so I’ll summarize what its blog post says. Only Epic and Meditech had a net gain in hospitals in 2019. Epic has won most of the new big-hospital decisions over several years, but Cerner bagged the DoD/VA elephant. KLAS says there is room for another market entrant, but it glosses over the time, money, and determination that would be required to develop, sell, and install a new hospital EHR. On an unrelated note, I have a minor grammatical quibble with KLAS for writing “multi-tenet” instead of “multi-tenant.”
COVID-19

The New York Times reports that nursing homes are taking advantage of being off limits to ombudsmen during the pandemic by evicting low-profit residents — such as those on Medicaid — to free up beds for profitable COVID-19 patients. Some facilities have discharged residents with no notice to unregulated boardinghouses and cheap motels, sometimes without notifying their families. Nursing homes make much of their profit from post-surgery rehab patients who are covered by private insurance, the supply of which has dwindled as hospitals halted non-essential services. Seventy percent of US nursing homes are for-profit businesses, with 11% of them being owned by private equity firms.
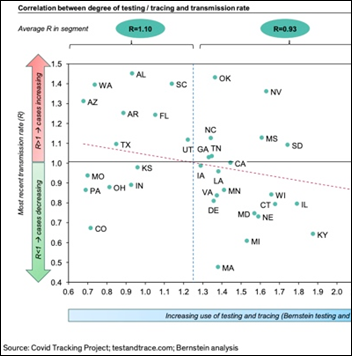
Former FDA Commissioner Scott Gottlieb, MD says that the 10 states that are seeing record-high new COVID-19 cases (AL, AZ, CA, FL, NV, NC, OK, OR, SC, TX) are losing control of the epidemic, as doubling time has fallen to under 10 days. He questions whether the governments of those states possess the political will to implement mitigation steps that could slow the spread. Researchers have noted that states that have higher mobility and low testing and tracing are more likely to be experiencing outbreaks. Arizona’s positive test rate is at 17% and its case count has turned sharply upward, far more than any other state. Thoughts that COVID-19 will throttle itself back in the heat – which were already questionable given its early impact in warm areas of the globe – should consider Arizona (highs in Phoenix are at 110 degrees) as evidence to the contrary, or perhaps more specifically, that congregating indoors under air conditioning without masks once lockdowns have eased is great viral exploit.
President Trump tells attendees of his Tulsa rally that he ordered government officials to slow down COVID-19 testing. He explained, “When you do testing to that extent, you’re going to find more people. You’re going to find more cases. So I said to my people, slow the testing down, please.”
The American Red Cross says blood donations have dropped sharply due to lockdowns and coronavirus fears, and as an incentive to lure donors back, is offering them a free COVID-19 antibody test.
A Harvard working paper finds that the COVID-19 mortality rate of black people ranges from seven to nine times higher than that of white people, depending on age group, meaning that the “years of potential life lost” of both blacks and Hispanic / Latino populations are higher than that of whites despite their much smaller population.
ProPublica reports that 12% of New Jersey’s nursing home residents died of COVID-19, along with 6% of all nursing home residents in New York, when the states ordered unprepared nursing homes to take all hospital transfers and prohibited them from testing prospective residents for COVID-19 in a “reverse triage” attempt to free up hospital beds. State officials based their order on federal guidance that allowed such transfers if the nursing home met a list of criteria, but nobody was sure who was responsible for assessing their readiness. A Wall Street Journal investigation found that 50,000 of the country’s 122,000 COVID-19 deaths have involved long-term care residents and employees.
Former FDA Commissioner Robert Califf, MD says that while the US is applying impressive technology expertise to COVID-19, we’re ignoring the basics, such as wearing masks and distancing.
Other
A federal grand jury indicts a Detroit man for the 2014 hack of UPMC’s HR system, where he is accused of selling the information of 65,000 employees on the dark web to conspirators who used it to file fraudulent tax returns. The LinkedIn of Justin Sean Johnson says he is a Oracle PeopleSoft expert who worked as a a self-employed cybersecurity researcher for several years, now employed as an IT specialist at FEMA.
Sponsor Updates
- Premier develops Intersectta, an oncology-focused group purchasing organization to source cancer and other specialty drugs.
- Relatient publishes a new case study, “Cherokee Health Systems Powers Telehealth with Patient Engagement, Goes Live Across 24 Locations During COVID-19.”
- CareSignal publishes a case study titled “How Mercy Built a Technology-Enhanced Care Management Model to Scale Care Management and Increase Patient Engagement.”
- Saykara congratulates customer OrthoIndy on receiving the Healthgrades 2020 Patient Safety Excellence Award.
- Spok appoints Brett Shockley (Journey.AI) to its board.
- TriNetX will partner with Parexel to advance real-world data use in clinical development.
Blog Posts
- IT Assessment: Am I Organized for Success in the Long Run? (Impact Advisors)
- PMD: Helping Practices and Patients Navigate Telehealth When They Need it Most (PMD)
- Getting Back to Regulatory Readiness (Premier)
- How to Put Your RPA in 6th Gear (Summit Healthcare)
- Leading a Data-Driven Healthcare Marketing Culture (SymphonyRM)
- Year of the Nurse and Midwife 2020 – What’s Your Story? (Vocera)
- More than PPE: Safety Precautions for Physical Therapists in the Age of COVID-19 (WebPT)
Sponsor Spotlight
Get-to-Market Health is a specialized consultancy focused exclusively on accelerating sales and driving revenue growth for healthcare solution providers. We work with business leaders to simplify the complexity and unique buying patterns of the healthcare market. Bringing deep, broad experience and valuable network connections, the partners at Get-to-Market Health are industry experts. We have worked at and with dozens of healthcare technology businesses ranging from small startups to large, established companies. We help our clients navigate the challenges they face as they work to drive revenue and market innovation.
(Sponsor Spotlight is free for HIStalk Platinum sponsors).
Contacts
Mr. H, Lorre, Jenn, Dr. Jayne.
Get HIStalk updates.
Send news or rumors.
Contact us.




GIve KLAS credit for consistency with the new word usage. Multi-tenet means each place has an installation on premise.
Mr. H is right on this. I’ve seen multi-tenant incorrectly written as multi-tenet several times lately. Multi-tenant enables multiple users or groups to share a single instance of a software application and its underlying resources. A “tenet” is a principle or belief, and is not the right word in this context (which is a tenet I ascribe to).
Attention to detail is why Mr. H. is my favorite pundint.
RE: Putin push for digital systems in healthcare
I wonder if the rural Russian hospitals have regular access to hot water yet?