Hard agree, and not just because I'm a spreadsheet nerd. Why are we all here? Isn't it in the service…
News 4/3/20
Top News
Health IT consulting firm CereCore lays off dozens of employees contracted to work for parent company HCA Healthcare, which has announced plans to cut costs in order to avoid its own layoffs.
The hospital operator has already seen several of its outpatient facilities close as procedure volume takes a nosedive in the wake of COVID-19.
The company’s senior leadership team will take a 30% pay cut for the duration of the pandemic. CEO Sam Hazen will donate his salary in April and May to the company’s charitable fund.
Reader Comments
From Slag Pile: “Re: hospital layoffs. How can this happen when they are staring down the barrel of crushing COVID-19 volumes?” Let us ponder the “only in America” healthcare system that we have allowed to be created, in which the million-dollar executives of architecturally imposing hospitals are responding to the most destructive health crisis in generations by firing their caregivers because of insufficient pandemic profit margins. I doubt any other country in the world would allow this to happen, but that’s true of nearly all aspects of US public health and healthcare delivery, where even hospices and nursing homes have been snapped up by private equity firms. We let healthcare become a big business, but then are surprised when it acts like one.
From Tilted Beret: “Re: HIMSS20 cancellation. This ‘interview’ with Hal Wolf is a fluff piece with no mention about refusing refunds, what it means to vendors and sponsors, etc. The ‘journalist’ is the director of content development for HIMSS – unbelievable!” I wouldn’t expect too many hardball questions or brutally honest answers when a HIMSS employee interviews the HIMSS CEO for a HIMSS publication, but maybe they could have put their collective heads together to come up with something more useful than to express “all about me” regrets that the HIMSS rebranding and new product announcements didn’t go as planned, that cancelling was the right call (which we now know), and a pitch for HIMSS Digital (which Hal says was already being worked on before HIMSS20). Hal also says that it’s a “great thing” that registration fees roll into HIMSS21, which is a less-great thing than getting your money back.
From YouveGotMailToIgnore: “Re: medication change request. Sent my specialist one through their portal. Before, the CMA would talk to the doctor and send an update back. Now the response is to schedule a telehealth visit. Maybe they are hurting for revenue, but it’s ironic since the last time I requested a telehealth visit I was denied.” My oft-repeated summary: people and companies will always choose the action that pays them the most. They didn’t need the money then, and now they do and insurance will pay – your preferences as a customer weren’t important then and they aren’t now. In fact, I should correct myself in calling a patient a customer – unless you’re paying cash or have full discretion about who and how much your insurance pays, you aren’t really one.
From Administrator: “Re: patient surveys. The company that does ours sent a note telling us why we have to keep spending on sending these to patients during the crisis. Our clinicians would be fine if we stopped. Are revenue pressures forcing healthcare systems to try to get out of existing contracts or push for concessions?” I doubt most contracts contain customer “I can’t or really don’t want to pay” clauses that would render their contracts void or convince the vendor to renegotiate terms, but maybe readers can elaborate. I doubt anyone will do better than getting extended payment terms (with interest accruing).
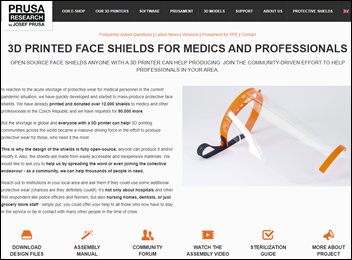
From AM: ”Re: 3D printing. One of our patients donated face shields to our family medicine office that he printed. Pretty cool, and makes me think it would be worthwhile to purchase a 3D printer for the office. People are doing really good things out there, including developing cleaning stations in shipping containers and the couple who had gourmet chocolates delivered to our office. Sometimes negative attitudes and people usurp all our energy, but it’s important to remember that there are so, so many awesome people in the world who keep us going during the stressful days, and we have had an endless run of those lately.” Instructions and design files are here. Everybody is noticing the sudden mainstreaming of virtual visits, but 3D printing will also earn a spot on the list of technologies that coronavirus will turn into a standard.

From CopyPaste: “Re: ‘HIPPA.’ Even the government can’t spell it right all the time, at least in this Senate document.” We can only wish that this was the worst example of the federal government’s healthcare failings.
Webinars
April 15 (Wednesday) 1 ET: “Scaling front-line COVID-19 response: virtual education, screening, triage, and patient navigation.” Sponsor: Orbita. Presenters: Lawrence “Rusty” Hofman, MD, medical director of digital health, Stanford Health Care; Kristi Ebong, MPH, MBA, SVP of corporate strategy, Orbita. The presenters will describe how chatbots can be quickly deployed to streamline individual navigation to the appropriate resources, administer automated virtual health checks for monitoring and managing specific populations, increase access to screening and triage for high-risk populations across multiple channels (web, voice, SMS, and analog phone), and reach individuals in multiple languages.
Previous webinars are on our YouTube channel. Contact Lorre to present your own.
Acquisitions, Funding, Business, and Stock
Startups are desperately trying to save their businesses in the suddenly terrible economy by remotely laying off masses of working-from-home employees.
People

Healthcare analytics technology vendor Geneia promotes Heather Lavoie, MBA to president and CEO.
Announcements and Implementations
![]()
CloudWave announces GA of OpSus Edge, on-site infrastructure technology designed to help healthcare organizations manage, secure, operate, and maintain critical applications.
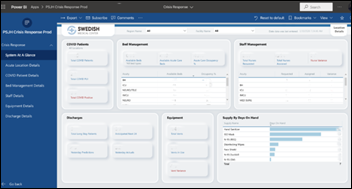
Swedish (WA) implements an app developed with Microsoft that helps staff track COVID-19 patients, and hospital capacity and supplies.

OptimizeRx announces GA of TelaRep, giving physicians the ability to virtually consult with medical science liaisons about patient treatment plans.
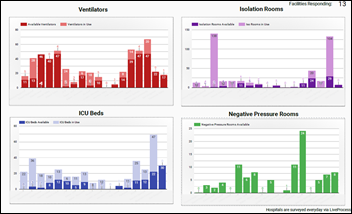
LiveProcess offers health systems free access to its COVID-19 Response Package, which includes a virtual situation center for shared awareness, coordination, and tracking. It is based on the company’s SaaS-powered LiveProcess Emergency Manager for emergency response.
Lumeris develops a free and open source model to predict COVID-19 hospitalizations, essentially creating a patient registry that requires about 60 minutes worth of user work. The authors say the model tested as being more accurate than others, in the process finding that another company’s model delivered results that were less accurate than simply guessing when applied to people under 65. It works with population health platforms from Cerner, Athenahealth, EClinicalWorks, and Epic. Lumeris SVP of analytics Michael Cousins, PhD was involved and he is a biostatistician with a ton of experience.
Health Catalyst offers free use of its Patient Safety Solution COVID-19 module and Capacity Planning Tools to healthcare organizations.
Premier, Stanford Medicine, and Resilinc form The Exchange at Resilinc, a cloud-based platform for hospitals to identify, locate, and exchange critical medical items during the COVID-19 outbreak. The group purchasing organization-agnostic system is accepting provider and industry group members at no cost.
First Orion offers providers free use of its programmable Inform product, which allows them to show their organization’s name on Caller ID to avoid the 84% of calls – including medically critical ones — that aren’t answered by people because they don’t recognize the caller’s number.

CPSI offers free access to TalkWithYourDoc.com, a new, standalone telehealth platform that was developed by its Get Real Health subsidiary.
KLAS finds that while organizations are highly satisfied with standalone Epic ambulatory implementations, those who use it via the Community Connect model of signing up with a host organization are less satisfied, although even then their satisfaction is about the same as that of competing ambulatory EHRs. Some Community Connect users fault Epic for allowing host organizations to sell a subpar offering, with some perceiving lower value even though Community Connect costs less than contracting directly with Epic.
Government and Politics

The Department of Defense presses pause on its roll out of MHS Genesis to better enable its care teams to focus on treating COVID-19 patients. The Cerner-based EHR software has already gone live at eight sites. Original implementation plans had called for the system to be deployed in 23 waves through 2024.
The CDC seeks a new chief data officer.
The HHS Office for Civil Rights loosens HIPAA regulations to give healthcare business associates more leeway in sharing PHI “in good faith” during the pandemic.
Privacy and Security

As remote workforces increase, Microsoft alerts several dozen hospitals to VPN infrastructure vulnerabilities that may attract ransomware attackers.
COVID-19
England’s NHS is considering developing a contact tracing app that alerts people if they have had recent contact with someone who later tested positive for COVID-19. Oxford researchers proposed such an app in a March 31 in Science, saying that it can help avoid mass quarantines while still helping contain coronavirus spread.
Fred Hutchinson Cancer Research Center computational biologist Trevor Bedford announces the launch of the NextTrace project, which aims to help coordinate data from commercial, state, and academic testing labs and voluntary contact tracing data to better inform public health responses to COVID-19.
A follow-up hospital supply survey from Premier finds that active care for COVID-19 patients creates a surge demand 17 times greater than typically seen for N95 respirator masks, nine times greater for face shields, six times for swabs, five times for isolation gowns, and three times for surgical masks.
New York City records its first COVID-related homicide victim, an 86-year-old hospital inpatient who was assaulted by another patient for breaking social distancing guidelines. Cassandra Lundy, a 32-year-old seizure patient with 17 previous arrests, was charged with disorderly conduct.

The Army Corps of Engineers converts the Javits Convention Center in New York City to a care facility for 2,000 non-COVID-19 patients. Military personnel have also helped to transition the Billie Jean King National Tennis Center in Queens into a similar facility.

The State of New York launches an online portal to connect healthcare facilities with volunteer healthcare workers. The portal is part of Governor Andrew Cuomo’s recently announced Central Coordinating Team, a hospital network that will help facilities share data, staff, and beds.
Health officials in China developed the country’s world-class infectious disease tracking system after the SARS outbreak that was supposed to prevent political meddling with outbreak detection, but local health officials who were afraid of sending bad news to Beijing withheld coronavirus information and overrode doctors, delaying the country’s response. Central health officials learned about the outbreak from whistleblowers who leaked internal documents rather than the early warning system. Later, local authorities minimized the severity of the situation, created narrowed reporting criteria, and required cases to be reviewed by bureaucrats before reporting them to Beijing.
Other
In what’s being touted as a world first, a medical team successfully delivers diabetes medication and receives a patient’s return blood sample via drone delivery to a remote island off the coast of Ireland.

Several health systems in Wisconsin make headlines for continuing to sue patients for unpaid bills during the pandemic. Patients in default have reported being served papers by processors (without masks or gloves) as recently as March 28.
Sponsor Updates
- Wolters Kluwer Health accelerates roll out of coronavirus alerting, reporting, and ICD-10 and SNOMED CT codes.
- Frost & Sullivan recognizes Greenway Health with its 2020 North American Customer Value Leadership Award.
- SyTrue will provide its SyHealth for Population Health solution free of charge to qualified public health organizations.
- ComputerWeekly.com profiles Google Cloud CEO Thomas Kurian and the company’s efforts to support the fight against COVID-19.
- Engage receives a five-star rating from Securance Consulting for the fifth year in a row as a Best Practice Meditech Hosting Provider.
- Clinical Computer Systems, developer of the OBIX Perinatal Data System, offers free system configuration, connectivity, and licensing for customers who are setting up temporary units or isolation suites for COVID-19 patients, which includes pregnant women who need fetal monitoring.
- Elsevier releases a new episode of its COVID-19 podcast, “Medical Informatics and COVID-19: Role and Utility of Hospital Digital Resources and Telemedicine in Managing the Pandemic.”
- Imat Solutions enables real-time health data reporting and analytics for its customers in response to COVID-19.
- InterSystems releases a new PulseCast podcast, “Lygeia Ricciardi: Prioritizing Patient-Centered Design.”
- Intelligent Medical Objects publishes a new white paper, “Interoperability, information blocking, and the coming data tsunami.”
- PatientKeeper announces GA of its Meditech-friendly Clinical Communications Suite Now.
- Health Catalyst adds registry, dashboard, and capacity planning tools to its suite of COVID-19 solutions, and will soon add a new set of financial impact planning resources.
Blog Posts
- Feature Releases in PMD: A Lesson in Teamwork (PMD)
- How SG Pediatrics is Using TeleVisits to Help Patients (EClinicalWorks)
- Speeding Up Discharge Communication with Post-Acute Providers in a Crisis (Ensocare)
- New Virtual Training in Response to COVID-19 Restrictions (EPSi)
- COVID-19 public dataset program: Making data freely accessible for better public outcomes (Google Cloud)
- New resources to help you report for 2019 (Greenway Health)
- Introducing the Digital Healthcare Transformation Playbook (The HCI Group)
- The Impact of COVID-19 on Prescription Renewal Requests (Healthfinch)
- Forgiveness and Grace: Surprising Advice for Working from Home (Healthwise)
- COVID-19: Planning to Support Temporary Facilities (Optimum Healthcare IT)
- Close paper gaps with intelligent medical records classification (Hyland)
- Imat Solutions Helping Customers to Identify Patients at Risk of COVID-19 (Imat Solutions)
- Pivoting to Quickly Operationalize Teleheatlh for COVID-19 (Impact Advisors)
- Provider systems face a new crisis from COVID-19: Staffing (Imprivata)
Contacts
Mr. H, Lorre, Jenn, Dr. Jayne.
Get HIStalk updates.
Send news or rumors.
Contact us.



More on 3D printing… I’ve been helping with a team making face shields as well. 3D printed headbands, and 3 hole punched plastic sheets for the shields. I’m in MA, but there are participants as far away as HI. https://www.mrscottbot.org/p/covid.html
“The company’s senior leadership team will take a 30% pay cut for the duration of the pandemic. CEO Sam Hazen will donate his salary in April and May to the company’s charitable fund.”
The rest of senior leadership is taking a 30% pay cut but the CEO is only donating 2 months (i.e., less than 17%)?
They’re taking the pay cut for the “duration of the pandemic,” so 2 months being ~17% is accurate only if the pandemic lasts 12 month. If the pandemic is over by September (as determined by who? HCA’s counsel? The president? Public opinion? the WHO? It’s unclear) then two months works out to more than 30%.