Yeah i'm not sure this ruling really moves the needle on Epic's behavior at all, the non-competes were always believed…
News 4/1/20
Top News

CMS issues coronavirus waivers and rules:
- Physicians can bill for telehealth visits at the same rate as in-person visits.
- Hospitals can bill for services that are performed outside their four walls, such as directing patients via telehealth to offsite screening locations.
- CMS will pay for 80 additional services when provided via telehealth.
- Hospitals can hire local clinicians.
- Hospital physician assistants and nurse practitioners can practice without physician supervision as permitted by state law.
- CRNA’s can work without being supervised by a physician.
- Hospitals are allowed to provide personal services for medical staff, such as meals or laundry service, while they are working at the hospital.
- Supervision of medical residents can be performed virtually.
- Medicare will pay for respiratory equipment for any medical reason.
- Hospitals will not be required to create written visitation policies for COVID-19 patients.
- The time in which hospitals must give patients a copy of their medical record is increased.
- Hospitals can triage patients in state-approved community settings in a “hospitals without walls” model, such as ambulatory surgery centers, hotels, and dormitories.
- Hospitals can contract with ASCs to provide essential surgeries, for which Medicare will pay hospital rates.
- COVID-19 testing can be performed in homes, dedicated testing sites, and other community settings.
- Hospital EDs can perform COVID-19 tests at drive-through testing sites.
- Ambulances can transport patients to a wide range of locations when other transportation is not appropriate, such as community mental health centers, FQHCs, physician offices, urgent care facilities, and ambulatory surgery centers.
- Physician-owned hospitals can temporarily increase their number of beds, ORs, and procedure rooms.
- Hospitals can provide physician practices with medical equipment and telehealth equipment and provide childcare services for workers.
Reader Comments
From Booth Happy Hour: “Re: HIMSS. Have they responded to your recap of HIMSS21 exhibitor plans?” No, and I wouldn’t expect them to since that wasn’t the point. I did the survey only because I was getting lots of exhibitor complaint emails and I don’t know how HIMSS is communicating individually with the 1,300 of the booth renters, especially the significant percentage of them that are vocally unhappy about being told to suck up their exhibit, hotel, and travel costs for the cancelled conference and return happily for another round in HIMSS21. HIMSS is no doubt busy dealing with the aftermath of HIMSS20, running Virtual HIMSS, frantically planning for HIMSS21, and trying to save the organization. Hopefully its transparency and humility will ramp up once the dust settles. Meanwhile, my body clock can’t comprehend that it was just three weeks ago today (as I write this on Tuesday) that the HIMSS20 exhibit hall would have been opening for the first day. I just read the book “A Short Stay in Hell” as urged by Mrs. HIStalk, and while I didn’t get much out of the rather depressing tome because I prefer quality entertainment such as “Tiger King,” today’s real world seems similarly never ending.
Webinars
April 15 (Wednesday) 1 ET: “Scaling front-line COVID-19 response: virtual education, screening, triage, and patient navigation.” Sponsor: Orbita. Presenters: Lawrence “Rusty” Hofman, MD, medical director of digital health, Stanford Health Care; Kristi Ebong, MPH, MBA, SVP of corporate strategy, Orbita. The presenters will describe how chatbots can be quickly deployed to streamline individual navigation to the appropriate resources, administer automated virtual health checks for monitoring and managing specific populations, increase access to screening and triage for high-risk populations across multiple channels (web, voice, SMS, and analog phone), and reach individuals in multiple languages.
Previous webinars are on our YouTube channel. Contact Lorre to present your own.
Announcements and Implementations

London’s 4,000-bed COVID-19 emergency treatment facility, Nightingale Hospital – created inside a convention center — will run Cerner Millennium, extended from the implementation of Barts Health NHS Trust.
Government and Politics
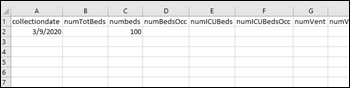
CMS asks hospitals to report their COVID-19 testing data to HHS. HHS also asks hospitals to report their bed and ventilator supply and COVID-19 patient counts by emailing a manual worksheet every afternoon. The electronic gaps in our public health and surveillance reporting are startling.
COVID-19
China ships the first of many shipments of COVID-19 emergency medical supplies to the US – 12 million gloves, 130,000 N95 masks, and huge numbers of masks, gowns, hand sanitizer units, and thermometers. An additional 22 flights are scheduled over the next two weeks. The government is paying for the flights, but a distributor is paying for its contents, 60% of which will be sold to the federal government and the rest to the distributor’s own private customers. We were sending respirator masks and protective suits to China just two months ago, so maybe we’re buying some of our own stuff back.

New Yorkers crowd together in defiance of public gathering regulations to get their flag-waving selfies with USNS Comfort, missing the irony that their irresponsible actions might land them or someone else a coveted COVID-19 respirator spot.
European Union countries struggle to develop virus-tracking apps that do not infringe on personal rights or GDPR, noting the apparent success in Singapore and South Korea of using phone-based digital tracking of those who are infected. Poland is tracking people who are under home quarantine via an app, while Germany’s health minister demands a national debate on the ethics of using cell phone tracking technology.

Google opens free access to several public COVID-19 datasets to researchers, accessible from its Google Cloud Console and its BigQuery ML.
Experts warn that the US’s fragmented health system will create financial hardship for patients who are tested for COVID-19, especially since it’s early in the insurance deductible year. Insurers have agreed to waive co-pays for the test itself, but visits to the ED to have the test performed, surprise bills from out-of-network EDs and contracted ED doctors will increase, and surprise billing protections were excluded from the federal government’s coronavirus bill after lobbyists for hospitals and physician staffing firms played “the COVID card.”

Nursing homes are refusing to accept hospital patients until they test negatively for coronavirus, a practice that frustrates hospitals that are anxious to free up beds. Hospitals say it takes days to test patients who were not suspected of having COVID-19 even when tests are available, but nursing homes don’t usually have separate isolation areas and worry about fatality rates of up to 50% once coronavirus starts spreading inside their walls.
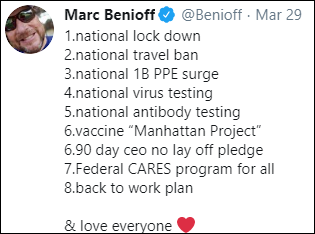
Salesforce CEO Mark Benioff lays out his plan for combatting COVID-19. Few of his items are being discussed by the actual people in charge.
Other

Intermountain Healthcare cuts the pay of physicians, nurse practitioners, and physician assistants due to “changing needs created by COVID-19.”
The New York Post reports that while frontline workers at Mount Sinai Health System are forced to beg for protective gear and wear garbage bags in its absence, CEO Kenneth Davis, MD was working from home in his six-bedroom, eight-bathroom Miami waterfront mansion, having been there since early March and advised to stay there by his doctor to avoid coronavirus exposure. He chose the $3.4 million Florida home over his $2 million one in Long Island and the $7 million one he owns in Aspen. Davis made over $12 million in 2017 and $6 million in 2018. Meanwhile, the hospital’s health network president is also in Florida, working from his oceanfront condo. I understand that much of what these guys do can be virtual, but somehow I expect more them given that they are both (a) doctors; and (b) health system leaders. Not to mention highly paid compared to the troops they’re sending into battle short on weapons against an enemy that targets not just themselves, but their familes.

University Medical Center (TX) suspends an anesthesiologist who wore a respirator face mask in the hospital hallway as he was leaving an emergency intubation. The chief of anesthesia texted him: “UR WEARING IT DOWN A PUBLIC HALL. THERES NO MORE WUHAN VIRUS IN THE HALLS AT THE HOSPITAL THAN WALMART. MAYBE LESS.” (the all-caps styling and insistence on calling it “Wuhan virus” isn’t encouraging). Meanwhile, an anesthesiologist at Seattle hospital was also threatened with firing for wearing a surgical mask in the hall. Other hospitals have taken the opposite approach in requiring all caregivers to wear a mask in all hospital spaces. You would think that non-clinical hospital suits could find something more useful to do than fret over trained doctors protecting themselves in whatever way they feel is appropriate, or barring that, just work from home and stay out of the way of people who are saving lives in between watching them end.
The Department of Defense orders all medical and dental facilities to postpone elective procedures for 60 days.
Hospitals in New Zealand will use 1000minds “knowledge codification” software – which scores patients to decide which of them get surgery – to guide ICU doctors in choosing which COVID-19 patients get an ICU bed. The software’s non-healthcare uses include businesses evaluating potential new products, shortlisting RFPs, selecting students for admission or scholarships, picking an engagement ring, evaluating job candidates, and choosing “best actress” type arts awards.

The home of an Arkansas family practice medical resident who is separated from his wife and one-year-old as he treats COVID-19 patients is destroyed by a tornado. A friend started a GoFundMe with a goal of $2,500 that has raised $108,000 so far. The photo above was of Jared Burks, MD watching his son crawl for the first time as he came home after a two-week stretch, right before his home was destroyed while he was inside. Maybe those Mount Sinai executives can loan him one of their mansions.

This is the cover of the current issue of The New Yorker.
Sponsor Updates
- Arcadia helps to form the COVID-19 Healthcare Coalition.
- Avaya expands free offers for work-from-anywhere apps to help businesses respond to the COVID-19 pandemic and protect employee health.
- Bright.md adds B Capital General Partner Karen Page to its board.
- Nordic offers free best practices and suggestions as responses to healthcare organization questions in its Ask Nordic service.
- Meditech offers free, six-month access to its Scheduled Virtual Visits functionality to its patient portal customers.
- Datica releases a new podcast, “ONC Final Rules on Information Blocking – Part 1.”
- CI Security makes available a work-from-home security assessment.
- CompuGroup Medical offers free telemedicine software to members of the Arizona Medical Association.
Blog Posts
- The Vital Role that HIEs can Play in Disease Control and Outbreak Management (314e)
- EHR Patient Reporting Module to Help Combat COVID-19 (AdvancedMD)
- Avaya Cloud Office is Here, and Your Workplace Will Never be the Same (Avaya)
- The Interoperability and Patient Access Final Rule: The Importance of PACs (CarePort)
- ONC & CMS Interoperability Regulations: Part 4 – Clinicians and Caregivers (Diameter Health)
- Going remote: Creative solutions to keep projects moving (Nordic)
- Health IT Support: Making the Shift to Remote Management (CereCore)
- Leveraging Technology Against COVID-19 in the Pacific Northwest (Collective Medical)
- CoverMyMeds’ Affinity Council Fosters an Environment of Inclusion (CoverMyMeds)
- Should I Still Be Interviewing During the Coronavirus Pandemic? (Direct Recruiters)
- The Growth of Telehealth and How Analytics Can Support It (Dimensional Insight)
- 6 Ways to Build a Medicare Advantage Partnership (Dina)
Contacts
Mr. H, Lorre, Jenn, Dr. Jayne.
Get HIStalk updates.
Send news or rumors.
Contact us.



10+ years after the HITECH act, countless billions of dollars being invested into EHRs, and endless hype about information exchanges. The government solution right now is to have everyone send VPOTUS a spreadsheet.
I’d wager the problem exists more on the receiving end than the sending end.
The amount of items to comment on in this update are astounding. The dysfunction and regulatory ridiculousness of our health care system is laid out in perfect form when you look at all of the items CMS must DEREGULATE in an health care emergency — with the only interpretation being that more are completely unnecessary burdens on the physicians and other health professionals working day in and day out to treat patients. Absolute absurdity all around.
And then you add to the that the craziness of EU privacy policies and GDPR and think, well maybe we don’t have it so bad.
Health “care” is being exposed for all of its warts right now and I hope at the end of all of this people do not forget and our system has a chance to be reborn.
I fail to see how deregulation related primarily related to reimbursement for services and staff certification requirements undermine the importance for strong consumer and patient privacy rights. Italy temporarily suspended GDPR for civil protection personnel who are supporting their COVID-19 efforts. That seems very reasonable. They still have, and deserve, strong privacy protection against private companies using apps and websites to gather and sell identifying data.
The NY Post article about the “not-for-profit” millionaire Mount Sinai executives holed up in their FL vacation homes is just so…yuck. I am at a loss for words.
might even be that a extraneous and tangential event might not relate the operational state of federal systems accurately…
I’d venture that someone just got bed-counts fast. Should be a no-brainer to get that information without every hospital having to shuffle the cards, or beds as it may be.