Hard agree, and not just because I'm a spreadsheet nerd. Why are we all here? Isn't it in the service…
News 11/13/19
Top News
Google announces Project Nightingale, a partnership with 150-hospital Ascension in which the company will gain access to the identifiable data of potentially all of Ascension’s patients to apply predictive analytics for patient care.
Business Insider reports that the information of 20 million patients has been uploaded to the cloud, with that of another 30 million patients scheduled for transfer in February.
The Wall Street Journal says the data being shared is not de-identified and is essentially the patient’s entire record. It also notes that at least 150 Google employees have access to the data.

The organizations are testing EHR search software and tools that present EHR data graphically to clinicians.
Ascension’s patients and doctors were not notified of the project, except for the 2,000 doctors and nurses who are testing the EHR search function.
Ascension says the deal meets HIPAA requirements because Google has signed a Business Associate Agreement.
Quoted in the announcement was Ascension EVP / Chief Strategy and Innovation Officer Eduardo Conrado, who spent 26 years as a Motorola IT and marketing executive and four years as an Ascension board member before joining the health system’s executive team in September 2018.
Reader Comments
From Laid Off and Up: ”Re: recent layoffs. Why do companies fail to understand how bad they look laying off employees in November and December?” I assume that unrestrained desperation to make Excel cells jump forcibly through hoops to earn a bean counter hurrah outweighs the justified black eye that results from showing previously valued “associates” the door during the two-month holiday window. It’s never a great time to lose your job, but prospects are dim until after New Year’s, long nights invite depressing self-analysis, and it’s an unenviable acting job trying to appear upbeat along with holiday-spirited family and friends. Layoffs are a management failure, but November and December cutbacks suggest a higher level of knee-jerk incompetence. I’ll offer my advice from having served on both sides of the forced march out the door — you don’t want to work for a company that conducts regular layoffs anyway, so they’re doing you a favor by forcing you to choose a better employer.
HIStalk Announcements and Requests
I’m excited that my pre-ordered copy of “Man’s 4th Best Hospital” by Samuel Shem was deposited into my Kindle library upon its release today. I expect that will be the subject of my next book review. Meanwhile, if you think I should read a particular book and report on it, let me know.
Webinars
None scheduled soon. Previous webinars are on our YouTube channel. Contact Lorre to present your own.
Acquisitions, Funding, Business, and Stock

Cerner lays off 131 employees in its latest round of cost-cutting.

Value-based care clinical quality platform vendor Apervita raises $22 million from an incremental investment.
Premier launches Contigo Health, a network of member health systems that will use EHR-integrated, evidence-based clinical decision support to optimize care for employees of its employer members. It will also identify available employer health and wellness programs. Premier acquired evidence-based clinical decision support vendor Stanson Health a year ago for $51.5 million, which I would guess forms a key part of this offering. This announcement is a pretty big deal – as big tech companies start trying to figure out this maddeningly complex market, publicly traded Premier knows it inside and out (supply chain, quality improvement, analytics, technology, clinical delivery, etc.) and has now, via Contigo Health, formed relationships with 35 health systems representing 440 hospitals as well as several national employers to address cost and quality issues (also note that health systems are longstanding Premier member-owners). I wrote here several years ago that Premier was the company to watch in terms of disruption and execution and this announcement doesn’t throw water on that prediction. If I were Google or Amazon and was anxious to get a healthcare foothold… well, let’s leave it at that.
Sales
- Mercy will implement Bright.md’s asynchronous virtual care platform to provide online triage, diagnosis, and treatment for patients at any location at any time.
- In Northern Mariana Islands, Commonwealth Healthcare Corporation will upgrade its Medsphere legacy system to CareVue EHR and revenue cycle.
People

Jon Zimmerman (Athenahealth) joins Holon Solutions as CEO.

Datica CTO Travis Good, MD will leave the company’s management team. He will remain a Datica board member and is starting a new venture that is focused on personal data and privacy
Announcements and Implementations

Cricket Health Chief Product Officer Geoffrey Clapp builds VA Care Finder, a free Amazon Alexa skill that allows veterans to provide an address and to be given the closest three VA locations by driving distance (including traffic conditions), powered by the VA’s Facility API. The screenshot above is from an Echo Show device. He’s working on enhancements to use Alexa’s default home location, answer questions about specific facility hours or address, and answer questions about service lines, such as mental health, rather than all locations. Alexa’s limitations don’t allow him to link to external services or to use mapping tools. He’s hoping to explore the VA’s many other APIs to see if appointment scheduling is a possibility. He concludes in his Veterans Day post,
With these APIs — and there is much, much more than just the facilities subset API that I’ve exposed here — the developer community can now get access to data we only dreamed about back in the highly-mentally-scarring VistA integration days of yore. The fact that nearly all the data that is available to internal development teams at the VA or USDS is also available to every hacker, startup, and BigCo means we can do what APIs are meant to — OPEN THE DATA — and build stuff no one ever thought of (or, thought of but didn’t have the budget for…I see you, VA) and there are few populations as deserving of innovation as our Veterans.
A Black Book survey of health information management professionals finds that 93% are optimistic that AI can streamline document creation and capture a holistic patient history to improve outcomes and revenue integrity.
Prepared Health develops an API that users FHIR 4.0 to connect home care agencies and other providers to health plans and hospitals for referrals, care management, and billing.
Government and Politics
Politico reports that CMS Administrator Seema Verma signed a $2.25 million government contract to hire at least 40 consultants to polish her personal brand, several of them former Trump campaign workers who billed taxpayers up to $380 per hour to perform tasks that have always been managed by CMS’s civil servants. HHS cancelled the contract in April 2019 after Politico reported on it, but at least $744,000 had already been spent.
Other

In Israel, Sheba Medical Center says it will create “the first fully VR-based hospital.” That’s certainly a press release stretch, unless the hospital plans to sell off all those buildings in the photo above and instead pass out VR headsets to patients. They calmed down a little further down the page, specifically listing that the hospital will use virtual reality for therapy services and education.

The non-profit Health Care Cost Institute gains access to de-identified Blue Cross Blue Shield claims in a multi-year partnership agreement. UnitedHealthcare stopped sharing its claims data with the group earlier this year, citing privacy concerns about HCCI, which is a non-profit competitor to its claims data-selling Optum subsidiary.
The Environmental Protection agency is proposing to ignore the conclusions of academic studies in its rulemaking unless the authors submit all raw data, including any patient medical records that were reviewed, for public inspection. EPA says outsiders should be able to independently review all study data to verify the conclusions of the researchers. The measure would make it more difficult to pass new environmental laws because the personal health information that was involved is often collected under confidentiality agreements. EPA’s proposed standard would exceed those for published medical studies, which do not require investigators to submit raw data.
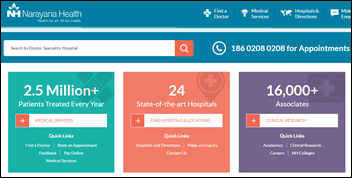
A newspaper in India interviews Viren Prasad Shetty, the COO of India-based Narayana Health, which plans to expand from its 30 hospitals and 6,000 beds to 30,000 beds. Interesting points:
- The company plans to create a virtual health network that involves apps rather than buildings in an Uber-like model that will allow it to grow more quickly at a lower cost.
- He says India’s plan to add a new medical school in every three districts of India isn’t adequate because many of the graduates leave the country, noting that the US has more India-graduated nephrologists than India itself.
- He predicts that “the biggest export-earning industry of this country will be our manpower,” specifically medical caregivers as declining populations leave Western countries with no one to care for their senior citizens.
- Narayana’s 20% annual growth in cancer services eclipses that of its primary focus of cardiac services, so “we will want to convert all our hospitals into cancer hospitals.”
- He says the company’s strength is that is led by a core group of doctors – including cardiac surgeon and CEO Devi Shetty, MBBS – instead of business executives, which makes it attractive to doctors.
A man who expected his hernia repair to cost around $10,000 is shocked at the for-profit hospital’s $116,000 bill for the 91-minute outpatient procedure, including $1,700 for a pair of scissors. He had passed on buying real health insurance and instead enrolled in a health-sharing ministry that pools medical bills among self-pay patients outside the purview of insurance regulations. He was approved for up to $50,000, but inadvertently chose the most-expensive area hospital and didn’t realize that patients who are covered by health-sharing ministries are billed at the same rate as uninsured or cash-paying patient without the benefit of heavy insurer-negotiated hospital discounts. The hospital refuses to budge on the $67,000 balance he owes. He’s demanding that Virginia’s consumer protection office force the hospital to write off his balance, but an attorney with Virginia Poverty Law Center says the hospital will probably just sell off his debt to a collection agency for 10 cents on the dollar.

An American Osteopathic Association survey finds that 75% of Americans feel lonely. My free advice – forget your pretend friends on Facebook and make an effort to interact with actual human beings instead of accidentally trampling them on the sidewalk while staring down in wonderment at your phone’s compelling but imaginary world. The most provocative art I’ve seen recently is by photographer Eric Pickersgill (above), who showed what real life would look like once the “small, cold, illuminated devices” of social media addiction are removed. He describes it as: “This phantom limb is used as a way of signaling busyness and unapproachability to strangers while existing as an addictive force that promotes the splitting of attention between those who are physically with you and those who are not.”
Sponsor Updates
- Apixio will exhibit at the Rise Annual Risk Adjustment Forum November 12-14 in Scottsdale, AZ.
- Clinical Architecture will exhibit at AMIA November 16-20 in Washington, DC.
- Diameter Health will exhibit at the Advent HEDIS 2020 Client Conference November 19 in Scottsdale, AZ.
Blog Posts
- Give your practice the financial breathing room it needs (AdvancedMD)
- You don’t have to list your negotiated rates (yet): Our 3 key takeaways from the HOPPS final rule (Advisory Board)
- Better. Faster. More Efficient. (Agfa Healthcare)
- Keys to a Successful Laboratory System Implementation (Optimum Healthcare IT)
- Analytics for Whole-Person Care: The Rise of the Connected Behavioral Health Network (Arcadia)
- HIPAA Security Rule Checklist: What is the HIPAA Security Rule? (Atlantic.Net)
- The State of AI in 2020: 35 Stats You Need to Know (Avaya)
- HIPAA vs. HITRUST (Datica)
- 6 Reasons to Initiate a Network Assessment Now (Burwood Group)
- nteroperability: Why It Matters So Much to the Current and Future State of Healthcare (ChartLogic)
- Basic Principles That Could Transform Your Practice (EClinicalWorks)
- Recap: ACEP19 Focused Heavily on Workplace Violence (Collective Medical)
- Why a Manufacturer Cash-Price Program Can Be a Better Option for Patients Purchasing Prescriptions (CoverMyMeds)
Contacts
Mr. H, Lorre, Jenn, Dr. Jayne.
Get HIStalk updates. Send news or rumors.
Contact us.





Re: Project Nightingale
“It’s not who has the best algorithm that wins,It’s who has the most data”. Andrew Ng,
What does this do trust in the doctor-patient relationship? It seems that confidentiality has been broken; will patients be willing to talk honestly with their doctor about potentially embarrassing experiences (sexual partners, suicidal thoughts, mental health problems, abortions, etc.) now that they know everything they say will got straight to Google–with their name attached?
Why didn’t nightingale project include a de-identification process ?
Remove the HIPAA related elements BEFORE uploading the data to the Google cloud ?
It would still be very valuable, without HIPAA… just because of its size.
Nightingale got data greedy ?
Re: November and December layoffs
Layoffs are almost always painful, but it feels worse during the holidays. As a recruiter, I get to see where the layoff leads. It’s remarkable how often it turns out to be for the best. I’ve seen so many people take layoffs hard only to look back a few months later with gratitude that it led them to something better. My heart goes out to all those who get laid off this holiday season; I wish they would all be able to realize they’ll probably end up in a better place.
Teletracking let go of 20% of its workforce recently.
Re: Project Nightingale
From the quite straightforward explanation from Google, the data is being moved to the Google Cloud to be used by Ascension. Google Cloud does not share data with other Alphabet units, it provides a service as an extension of the IT infrastructure of Ascension.
The AI/ML algorithms part of the deal seems to be an additional aspect of the project, that hasn’t started yet. It would make sense that this part only would use a (very likely de-identified) subset of the data.
From yesterday’s headlines: https://cloud.google.com/blog/topics/inside-google-cloud/our-partnership-with-ascension
Right. I’ve said this exact thing to others who were freaking out about this. This really isn’t different from other data consolidation projects and pop health warehousing that Epic and others have done with their customers. The fact that Google is involved is bringing out all the politicos who want their name in the WSJ.
Epic or Cerner has not shared that with any 3rd party yet. If they were to do so, they will face the same backlash as Google/Ascension is facing. My guess is that Epic will never share such data without patient’s consent as recorded in Epic’s research module.
Im sorry, but EPIC and CERNER are THIRD PARTIES!!!!!!!!!
Their clients deployment of their software is their clients, What the client allows them to access is in the fashion of them being a third party!
Per news articles, Epic’s data warehouse, Cosmos, uses deidentified data. So not exactly the same as Google here.
Five years from now, some security researcher discovers that data got shared with the other Alphabet units, Google releases press release saying they’re sorry and they’ve updated their terms to say that data may be shared with other units for business reasons, and it’s now covered under the business agreement.
Yeah UnitedHealthcare stopped supplying claims data to HCCI because of privacy concerns . . . and the moon is made of cheese and inhabited by little green men.
RE: Project Nightingale.
Sorry, but I am just not buying it. Movement and sharing of identified patient information like this should be illegal. I don’t trust Google, or Amazon, or… fill in the blank. I am glad I am not a patient of Ascension. I would surely demand my record to be removed with a verifiable chain of trust. It is one thing to have a cloud based service for an application, database, etc. It is something entirely different as to what this is, or so it seems.
It certainly bends to the extreme point, if not breaking, the intent and spirit behind the passage of HIPAA.
Just because this has been occurring a lot in other instances doesn’t mean it is “ok” or that it should be readily accepted as just a normal business practice.
Data is going to be the 21st century version of oil and while I accept that legislation will always lag considerably behind the pace of technological innovation there needs to be some level of balance through federal legislation. Not crazy patchwork state by state variation in privacy safeguarding and data collection practices.
So with that logic, do you not trust Epic’s Healthe Planet, Cerner’s Healthe Intent, Change Healthcare, IBM Watson or anyone of the dozens of AI engines that are out there that almost every single Health System is using? I think the only reason people are having this kind of strong reaction is because its Google. If Ascension had come out and said that it was Cerner’s Healthe Intent instead, would you still feel this way.
Lets give the benefit of the doubt before jumping to conclusions. This is one of the biggest reasons why our industry falls behind almost every other industry when it comes to tech, AI and data. We refuse to give an inch in order to move forward a mile.
Epic and Cerner make money selling EHRs to healthcare systems. Google makes money collecting users’ PII and selling it to other people. I don’t know anything about this deal or Watson or Change Healthcare but I think it’s easy to see why people treat the companies differently.
Cerner makes money how?
From recent earnings call:
“As the acknowledged data source, we plan to develop a monetizable distribution model that provides access to legacy client segments and adjacent market prospects such as biopharma, payers and actuaries, to name a few.”
Or this from Donald Trigg, Cerner EVP of Strategic Growth:
“Our global market share, our clinical research practice and our overall platform leverage provide natural points of differentiation in a segment with a significant $60-plus billion addressable market.”
Would be curious what protections the DoD and VA have in their contracts.
You know, I used to think that de-identification was something of a universal privacy shield, a good answer. I no longer think that.
Studies and articles like the following have been available for some years now.
Using Big Data techniques and correlating datasets, you can reveal patient identities with shocking frequency. Something on the order of 2/3 of the time, you can unmask exactly what person a particular datapoint applies to. The exact number of course depends on things like how de-identified the data was in the first place.
That is way, way too often! And Big Data isn’t just for NASA and the CIA anymore; these are widely available technologies ready for anyone to use. Do you need a correlating data set? Outfits like Experian are only too happy to sell you as much as you need.
Second try at posting links:
https://peachtreetranscription.com/re-identification-of-anonymized-data/
https://phys.org/news/2017-12-reveals-de-identified-patient-re-identified.html
RE: “Ascension’s patients and doctors were not notified of the project, except for the 2,000 doctors and nurses who are testing the EHR search function.
Ascension says the deal meets HIPAA requirements because Google has signed a Business Associate Agreement.”
OK, so how is this any different than when Practice Fusion shared patient data many years ago?
The patient should be the SOLE owner of his / her data.
NOT the healthcare organization, not the clinic, not the 4th best hospital, not even the best physician ever born.
Then, Google or anybody else for that matter can bid on this data.
The patient can decide then if the personal, intimate medical info should be shared with others and how many $ is it worth.
Maybe it can help pay the medical bills incurred…
I believe Google needed to win a Big Fish to try to light a fire and show the industry they have value in healthcare, alongside the recent big hires such as Karen DeSalvo. Ascension is just the Big Fish they needed for the headlines and to get others to notice them. Unfortunately, without the depth of those like Karen DeSalvo at the helm when this deal was negotiated, they overlooked the potential backlash and risk.
Ascension is traditionally very conservative, and would not do something like this without significant upside opportunity. The reason the records are not de-identified likely has more to do with the fact that Ascension has a large volume of disparate systems, largely due to their grand size is a result of significant acquisition of health systems in the past decade. Without a National Patient Identifier, the combined data would not be statistically valuable as they need to merge multiple patient files for a single patient. And the value for combined data, that can be centrally managed in the cloud is a significant long-term asset for Ascension as they morph into the “outside of the four walls of the hospital” era. And then, of course, like with EMR’s, it may enable them to optimize billing and collections.
We can bash Google and Ascension all day, yet neither are the culprit. The core issue is the current industry regulations and protections need to evolve to meet modern realities . When the Ascension patients signed patient consent forms, most were likely signed pre-Ascension ownership/management. AND, most importantly, they did not give patients the opportunity to “opt-out” of such a large scale project. And, of course, there will never be a balanced and logical explanation for how the providers/physicians were compromised in all of this. Ultimately, the traditional BAA agreement is not enough to address the volume of potential risk. To think Ascension needs to go to Rome and get Vatican approval with most of their M&A activity, but their most sensitive “product”, PHI, can pass through without further investigation is a bit fascinating. It will be captivating to follow what may occur. Maybe ONC can create an arm like the FDA for PHI Data Projects?
@My Data – I agree with you that it is solely the patient’s data. What bothers me is that many hospitals willingly give the data away or sell it to entities such as Google, but when the patient asks for copies of his or her own records they are charged. Some states have gone so far as to pass laws regarding how much can be charged. As example, North Carolina:
https://www.lamblawoffice.com/north-carolina-medical-records-copying-charges-law-statute/
So it’s ok to take something from a person, charge them to get it back, but then profit off of it by selling it to others. If we were talking about a car, the hospital or health system would be facing grand theft charges. You took my car, are extorting me to get it back, and now you’re going to sell it to a used car dealer. As a patient, that is what it feels like.
I agree it is patient’s data but that is not the business model in other industries. What about credit information? Isn’t that consumer’s data too? but credit agencies hog it and sell it without any explicit approval from the individual to collect/distribute it.
People perceive the credit data industry as being extremely unethical. “But Equifax does it!” is not an argument that sways minds. There are two presidential candidates with meaningful policy initiatives. One of them established the CFPB and it would be an understatement to say that the other is not fond of the banking industry.