Hard agree, and not just because I'm a spreadsheet nerd. Why are we all here? Isn't it in the service…
News 10/16/19
Top News

Northwell Health extends its Allscripts Sunrise contract through December 2027.
Northwell’s 19 hospitals have been live on Sunrise since 2005, making it the largest customer of Allscripts.
Northwell extended its Allscripts TouchWorks agreement in 2018.
MDRX shares rose 1.4% Tuesday after the announcement, performing slightly better than the Nasdaq Composite index for the day.
Reader Comments
From Grim Sleeper: “Re: Allscripts and Northwell. What are the odds that their collaboration will result in a commercially viable inpatient product that can compete with Epic or Cerner” Zero, my reasoning being thusly even though all of us should be wishing for new inpatient EHR competitors:
- Allscripts says the new product will be based on Avenel, which is targeted to ambulatory practices but hasn’t sold well in its 18-month history. The company has admitted to stock analysts that it misjudged market interest in a cloud-based EHR that doesn’t offer a paired practice management product, which is a significant oversight for an EHR/PM company.
- Northwell said in the Allscripts press release that Avenel is immature and its usability needs help from Northwell’s experts, a comment that I’m surprised Allscripts approved.
- Allscripts has a low-and-dropping inpatient market share in which Sunrise has been replaced with broader, integrated offerings from Cerner and Epic. Northwell will continue using Sunrise for inpatient.
- Custom developing a product around a key customer’s specifications is a strategy that usually fails miserably except for that one customer, who gets their quirks and petulant demands baked into code that someone has to try to sell to the next hospital. Coding to spec as a follower than a leader is not the best way to create an innovative product that the broad market wants.
- My conclusion is that Northwell took advantage of knowing it had Allscripts over a barrel as its largest client. I obviously haven’t seen the contract, but I would bet that Northwell is the big financial winner, Allscripts saves face and slings a Hail Mary about a new product (created by improving a not-new product), and we will see in future Allscripts earnings reports whether the new R&D costs and possibly lower revenue contributions from Northwell can be offset by increased additional revenue.
- The key metrics to watch are overall EHR market share and Allscripts stock price. MDRX shares are up 10% since Paul Black took over as CEO in late 2012, vs. the Nasdaq’s 167% gain and Cerner’s 75% rise, and have shed 23% in the past year.

From Market Watcher: “Re: Epic contracts. They’re usually a source of mystery, but a moderately redacted copy of one popped up on SEC’s Edgar. I don’t see anything that looks like a gag clause, although there’s a lot of concern about protecting Epic’s IP.” The contract between Epic and Ardent Health Services doesn’t contain anything shocking:
- Clients pay higher Epic fees as their usage increases.
- Clients must be current on all Epic payments before bringing a new module live.
- Disclosure of Epic confidential information is prohibited, and if required by law (such as Freedom of Information Act requests for contract details), the client must notify Epic beforehand and cooperate with Epic to get the legally required disclosure stopped.
- No non-disparagement clause is present in the redacted version, but the customer is required to make each user sign an agreement to keep Epic’s confidential information confidential. That information includes functionality descriptions, source code, data structures, and implementation methods. Screen shots, which are the most contentious items in that arise in sharing information about system problems among users, aren’t mentioned specifically but probably fall within functionality descriptions (as does documentation, which Epic protects vigorously).
- Use of third parties for implementation, staff augmentation, training, support, and hosting is limited to those companies that have signed an agreement with Epic and that have agreed not to hire employees of clients or of Epic.
- Use of source code, data structures, and APIs can’t be used to develop a product that competes with anything Epic offers or that is “reasonably anticipated Epic software.”
- The customer is not allowed to solicit or hire (as either an employee or contractor) anyone who has worked on an Epic implementation within the past 12 months without the previous employer’s permission and Epic won’t “work with or provide training” for those exceptions.
From NH: “Re: Novant Health. Creating an innovative electronic patient and family advisory council.” Novant will survey volunteer council members about patient room decor, food quality, and nicer waiting rooms. I’m all for those things, but what I really want from a hospital is for them to put my interests ahead of their profits, develop and follow sound clinical protocols, give me access to caring and highly skilled providers, and send me home vertically and better than when I entered. I might enjoy having better coffee or softer chairs at the oil change place, but that’s not much consolation if the tech uses the wrong filter, doubles my cost by acquiring competitors, or claims to be concerned about my car’s overall health when what they really want is to sell me more services. Consumers can see only the most superficial aspects of healthcare and they assume that they don’t need to worry about the rest, which is not true at all.
From Billing Boy: “Re: patient estimates. They are often wrong, this study finds.” It’s easy to get worked up about patients being charged more than they were told to expect (which would be shocking in any business except healthcare), but portraying those hospitals as dastardly rather than incompetent misses the point. Healthcare billing is so arbitrary and complex that even the hospital itself has no idea what will be billed until after the fact, when all the revenue-obsessed hospital departments have picked the insurance bones clean. Here’s an easy test – give a hospital an anonymized copy of the clinical records from someone’s inpatient stay at their own facility and ask them what they think the itemized bill would look like (no dollar amounts, just which line items the patient would be billed for). It would have little correlation to the bill they actually sent to the patient. Hospitals are right that they don’t know what a given patient needs until they have already provided it, but it’s a mistake to ensure that the variability between estimates and actual bills is strictly due to clinical uncertainty or insurance surprises.
HIStalk Announcements and Requests
Thanks to Jenn for covering my absence of a few days for vacation. I kept up with what she was writing and sent her items that looked interesting, but otherwise spent close to zero time using any computing form factor. Other than the many “circling back” and “pinging you again” re-sent emails from PR people who can’t grasp that not everyone stays online 24×7 or finds their self-serving announcements to be of top importance, I saw no evidence that anyone even noticed my absence, which is how it should be.
I rarely think of Forbes as an objective, insightful news publication and this doesn’t change my mind – the company has launched a vanity publishing press and is paid-spamming LinkedIn with boilerplate invitations to “business leaders” who are willing to rent the Forbes nameplate to repackage themselves as quote-worthy experts a la “The Art of the Deal.” Its partner company touts that lazy executives can create an industry-captivating book in under 24 hours. Healthcare clients include former CMS Deputy CIO Henry Chao and about a zillion attention-seeking dentists.
Webinars
October 24 (Thursday) 1:00 ET. “The power of voice: Will AI-drive virtual bedside assistants become mainstream?” Sponsor: Orbita. Presenters: Nick White, co-creator of DeloitteAssist and principal in Deloitte’s Smart Healthcare Solutions practice; Bill Rogers, CEO and co-founder, Orbita. Conversational AI and virtual health assistants are bringing new opportunities to care facilities to improve patient journeys and yield radical workflow efficiencies. Will the hospital rooms of the future continue to provide traditional bedside call buttons? Or will these be replaced with digitally reimagined, AI-driven, voice-powered agents? Learn from the expert who created today’s industry-leading, market-proven, virtual bedside assistant.
Previous webinars are on our YouTube channel. Contact Lorre to present your own.
Acquisitions, Funding, Business, and Stock
Cerner will lay off 350 California employees following Adventist Health’s decision to bring its revenue cycle operation back in house from Cerner RevWorks. Cerner says Adventist Health has offered to hire all of the laid-off employees, while another 1,000 Cerner employees will swap their badges for those of Adventist Health.
Sales
- Bozeman Health (MT) chooses Kyruus ProviderMatch to integrate patient access in its website and access center.
People

Per-diem clinician hiring app vendor ConnectedRN hires Matthew Levesque (Athenahealth) as CEO.

Industry long-timer Kim LaFontana, MBA (Medically Home) joins Livongo as VP.

BHM Healthcare Solutions promotes Jean Neiner to president and CEO.

Ajay Kapare (Ellkay) is appointed to the CHIME Foundation Board and its board of trustees.
Announcements and Implementations
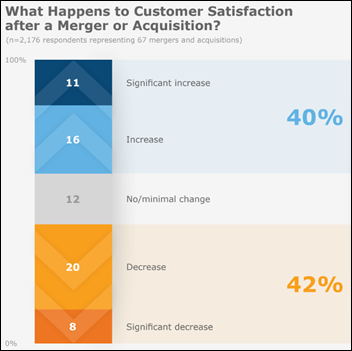
A new KLAS report looks at strategic mergers and acquisitions in healthcare IT, observing that about 40% of customers are happier afterward, 40% are less happy, and 20% see no impact. The percentage of customers anxious to bolt to a new vendor doubles after M&A when long-term customers resent the imposition of intentional nickel-and-diming, crappy support, and R&D slowdowns. Customers are better off if the acquirer is privately held and thus not desperate to pander to shareholders in chasing short-term profits at the expense of long-term strategy. KLAS concludes that M&A fails when the acquirer saddles the former company with layers of bureaucracy and sales-focused goals; fails to get its executives interested in the acquired company; makes grand promises that aren’t kept; and cuts back on support so that the resulting financial numbers make the acquirer’s executives look smart.
Family history vendor Ancestry launches AncestryHealth, which will sell a $149 profile of genetic screening results that are matched to specific medical health conditions, as well as a more expensive, membership-based service that provides deeper screening and quarterly screening updates. The company has contracted with an independent physician group to order the tests. Stat notes that the tests of competitor 23andMe are regulated by the FDA since consumers order them themselves, while AncestryHealth won’t get FDA oversight because the tests are ordered by doctors but instead will be under CMS’s physician-ordered diagnostic testing rules. Experts note that only 2% of patients who don’t have a family history of a disease will learn something new from such tests, while others say that genetics accounts for less than 10% of longevity, but lack of rigorous science doesn’t usually stand in the way of companies making big money from irrational health concerns (see: Goop).
A Black Book provider survey of vendors of software and services for coding, clinical documentation improvement, and HIM finds Nuance topping most categories, but Optum360, MModal, Dolbey, Adadyne, Qventus, and Fujitsu also finished first in some areas.
Nvidia and King’s College London create a platform that allows organizations to contribute their imaging data for machine learning-powered brain tumor research without copying it offsite or sharing it directly, with the federated learning system keeping patient data confidential.
Canada-based EHR vendor Premier Health Group will add AI from IBM Watson to its telemedicine app to use a chatbot to reduce clinician time on each call.
Other
In Australia, the new head of EHealth Queensland says its struggling Cerner implementation can be turned into a showcase project, but urges all of the state’s health bodies to help in getting new sites live while optimizing existing ones.
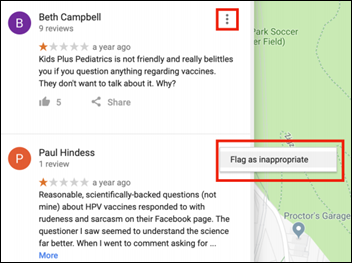
A reader sent this article about Shots Heard Round the World, a “rapid-response digital cavalry” that helps providers whose vaccine-related social media messages – such as “flu vaccine has arrived – get your shot today” — trigger an electronically mobilized torrent of negative comments, scathing Yelp and Google reviews, and threats from anti-vaxxers from around the world. The group was founded by two employees of Kids Plus Pediatrics, a Pittsburgh area practice that was attacked relentlessly after it published a video explaining the value of HPV vaccine in preventing cancer. They offer the highly detailed and excellent Kids Plus Anti-Anti-Vaxx Toolkit to help practices defend themselves online harassment. Fascinating to me is their analysis of who created the 10,000 negative anti-vaxx comments on their site:
- 95% were female, most of them either of age 18-24 or over 50.
- The vast majority were uneducated and either unemployed or underemployed.
- Attackers were mostly extremist in their politics, both to the left and the right.
- Every single person who visited the practice’s Facebook page during the eight-day siege whose profile photo featured one of those dopey filters was an anti-vaxx attacker.
In England, a hospital won’t be fined the prescribed $190,000 for 600 incidents in which it placed male and female patients in the same room. The hospital says it has a zero-tolerance approach for mixed-sex rooms, but then stretches the definition of “zero tolerance” by adding that it sometimes does it anyway when all beds are full. NHS England says mixed-sex rooms are detrimental to safety, privacy, and dignity, which it fails to note are already endlessly compromised throughout all aspects of hospital care, but especially when any patient is forced to room with another. Imagine if a hotel did this, even without all employees running in and out, awkward moments involving specimen collection and bedpan usage, receiving visitors, and being separated by just a thin curtain from a dying, moaning, or loudly delusional roommate.
Odd: the elected part-time coroner of an opioid-ravaged Ohio county is charged with illegally prescribing 1.5 million opioid doses over two years and fraudulently billing Medicaid and Medicare in his day job as a pain management doctor. On the other hand, he donated to the county’s Staying Clean Club and its drug task force, so there you go.

Even odder: Tampa General Hospital opens an OnMed telemedicine consult and drug dispensing booth in its food court so that its employees — who are inside its walls — can seek medical care from clinicians who aren’t. Maybe this is a Halloween-appropriate “the call is coming from inside the house” type situation. It’s not really an admission that employees don’t have time to deal with their own hospital employer’s bureaucracy as patients – the hospital is in business with the vendor and this first booth is a pilot for a broader rollout. The hospital CEO says millennials won’t wait to see a doctor in person, which if you’re a doctor who actually wants to care for patients, is depressingly accurate. The oldest millennials are now in their late 30s, so it would be interesting to see how those who are doctors run their practices and patient encounters.
Georgia lawmakers will require the state’s rural hospital CEOs, CFOs, and board members to complete eight hours of classes in financial management and strategic planning (in an apparent lack of irony).
Sponsor Updates
- Netsmart processes a record 300 million secure transactions through its CareFabric solution suite in a single month, triple the number of a year ago.
- AdvancedMD will exhibit at ASDS October 24-27 in Chicago.
- Apixio will exhibit at the RISE HEDIS & Quality Improvement Summit October 23-25 in Miami.
- Culbert Healthcare Solutions will exhibit at the Association of Administrators in Academic Pediatrics meeting October 17-18 in Miami.
- Cumberland partners with Chronicled’s MediLedger Project to advance blockchain supply chain networks for pharma manufacturers.
- Dimensional Insight will exhibit at the Massachusetts Health & Hospital Association event October 18 in Burlington.
- ONC names Surescripts as an ONC Program Partner for Electronic Prescribing, proving EHR vendors an alternative test method to ONC-ATL.
- Netsmart will present and exhibit at the American Health Care Association/National Center for Assisted Living 2019 Convention and Expo through October 16 in Orlando.
- Prepared Health will exhibit at HLTH, October 27-30 in Las Vegas, as part of the Matter Showcase Pavilion.
Blog Posts
- Agfa Healthcare’s Francisco Perez elected HL7 Fellow (Agfa Healthcare)histalk2.
- Pause to Consider: Data Loss Prevention (Fortified Health Security)
- Beth Israel Deaconess Care Organization: Leaping Forward in Analytics for Population Health Management (Arcadia)
- How HIPAA Compliance Affects Employees (Atlantic.Net)
- Increasing Physician Engagement with a STS Program (Optimum Healthcare IT)
- Choosing the Optimal Path to Cloud for Unified Communications (Avaya)
- Tree Talk: A “Simple” Way to Big Gains! (Bluetree)
- Support for Amazon S3 and EC2 Now Available in Latest Release of Datica Monitor Cloud Compliance Management System (Datica)
- Coming Soon: ChartLogic to Debut Electronic Faxing Solution (ChartLogic)
- How Collective Can Help D-SNPs with New Information-Sharing Requirements (Collective Medical)
- Pharmacist Spotlight: Utilizing CoverMyMeds’ Technology to Simplify Prior Authorization Requests (CoverMyMeds)
- How to Implement an EHR Change Management Program Using ITIL Practices and Survive to Tell About It (Divurgent)
Contacts
Mr. H, Lorre, Jenn, Dr. Jayne.
Get HIStalk updates. Send news or rumors.
Contact us.





While that telemedicine booth is kind of odd, I think a lot of people still underestimate how much employees don’t want their employer to have permanent access to their full health record, regardless of what kind of end user confidentiality might sit between other colleagues and their data. I know a lot of people who would gladly talk to a booth over anyone that’s also employed by their employer. Though, I would bet there’s some type of interoperability that exists between their existing records and this vendor.
The restrictions that Epic places on his customers, employees, and third parties on hiring is so frustrating. While I understand they want to protect their IP and reduce poaching, it creates such a toxic attitude among their employees and frustrations to employees who have life changes that require them to move away from Epic. Rather than being able to utilize your skills in the free market, they use a big stick to hold people hostage. They extend those restrictions on their own customers, keeping them from hiring really qualified people that could help make them successful and avoid really expensive consulting costs.
It also make hiring Ex-Epic people in the Madison job market incredibly risky because many are just trying to burn their 1-yr non-compete rather than looking for a longer term role.
Agreed. Epic is just generally anti-worker with their regular labor violations, over aggressive non-compete, etc.
Mr. HIS – you, once again, do this world a great service. For me personally I’ll say thanks for posting to a document that affirms every post I’ve ever made regarding the reality of what doing business with Epic is like in the real world.
Yes, they have a right to protect their IP, yes (evidently) their clients knowingly and willfully enter into these agreements and yes, the ecosystem that those agreements creates imposes outrageous costs on EVERY client implementation. The clients, who by definition have no way of understanding the implications of what they have agreed to, find deep into their initial build leading to a first ‘go-live’ that there are associated areas of the project for which they desperately need help – only to learn when they turn to the market for those services that it is not a free and open market – it a market, to a large degree defined (and somewhat controlled) by Epic. If you don’t adhere to their rules they will not allow your contractor or direct hire access to the vast Epic controlled technical resources that those very same resources must leverage in order to be effective at their work.
As stated by me before – I’m not offering a complaint or suggestion that what Epic does is in some fashion bad or wrong – far from it. My family has been well provided for due to the innovation and genius that is Epic.
The sad part, and the one that based on over a decade of direct involvement appears to be absolute – Epic has no interest in, desire for, or plans to modify it’s positions in these areas. Every client, in every install is forced to reinvent the wheel in related (and critically important) areas due to their very strict restrictions on innovation of anything of any relation to Epic. Change control is an easy example. The complexity of an Epic implementation requires very strict, very well defined and very well audited controls for introducing changes from POC (dev) -> TST (test) to PRD (production). Epic provides very limited tools in support of this, yet the demands remain for every client. By restricting clients ability to learn from other clients and certain people resources that may or may not be at some point in that arbitrary 12 month ‘magic’ window, there is an undeclared and undefined layer of risk and cost imposed on every site.
The part that always amazes me is that, at every site I’ve supported (over a dozen over more than a dozen years) when you sit down with project leadership and help them understand both the demands for the implementation and the CLEAR restrictions their employers agreed to when signing the contract with Epic they cannot imagine that such a thing is possible and realistic. They they quickly realize that (a) without effective solutions they are up against the wall and (b) there is no budget for any of the required resources needed to mitigate the risk.
Makes sense – the C-Suite and the Approval committee and the Drs. committee and whoever else is involved in agreeing to the terms Epic demands haven’t a clue (can’t possibly have a clue) as to the full impact of the terms they are agreeing to in the signing.
Existing sites are reluctant (if they will connect at all) to raise the issue with prospective clients as they are heavily dependent on the financial rewards that come with adhering to and supporting Epic’s guidelines for the continuing use of the software.
For those of us who participate in this market as HUMAN resources (fte or contractor) it is a strange situation to learn that, after working hard to be offered a role/contract your customer/employer will have to submit you to Epic for ‘approval’ before they agree to grant you access to both (a) the resources at Epic’s UserWeb and (b) – potentially access to Epic at the client site (even if you’ve been hired).
It’s a sobering moment to jump from one employer to another or in and out of the contractor-fte world to learn that you are not actually in charge of the outcomes of your own decisions and that you never agreed to the terms that are being imposed on your life and livelihood.
Of course, for both client orgs and individuals participating in this world the key is be aware, informed and do all you can to in fact retain control of your respective worlds and actions.
As I’ve said before, Mr. H – sharing this information, while it can’t/won’t change the structure of this market it sure does help all of us in it to have a clearer understanding of the contractual realities for participation.
“no evidence that anyone even noticed my absence” portrays what I think is the basic tenet of professionalism (completing services defines professionalism). And following it up with “which is how it should be” just sounds badass. Thanks for that, it was nice to see.
re: Queensland’s Cerner project
* Delayed … check
* Over budget … check
* “Not fit for purpose” … check
* Buyers still think they’re trailblazers … check
The only way you could tell this isn’t the DoD/VA was that it’s just a $1.2 billion project and only an adorable $256 million over.
Ancestryhealth. Interesting. People won’t willingly share a social security number with anyone yet will gladly send off DNA to organizations who have no obligation to tell you exactly who/what they’re sharing with their partners.
You are not the customer, you are the product – Pernille Tranberg