Monday Morning Update 9/11/17
Top News

HHS Secretary Tom Price, MD declares public health emergencies for Florida, Georgia, and South Carolina as Hurricane Irma surges through central Florida and the Tampa Bay area. Nearly 3.3 million homes and businesses in Florida are now without power. The storm marks the first time a tropical storm warning has ever been issued for Atlanta, which is expected to feel Irma’s windy and rainy aftershocks Monday.

Vice President Mike Pence has assured state officials that the federal government will be ready to mobilize relief teams as soon as the storm has safely passed. Those teams include 300 healthcare personnel flown in Saturday by the Air Force to Orlando, where the hurricane is expected to hit early Monday morning.
As is becoming the trend, several providers – including St. Vincent’s, Florida Hospital, Nemours Children’s Hospital, and Orlando Health in Florida – have stepped up to offer free virtual consults to victims of Irma. DrFirst has made its mobile iPrescribe prescription look-up tool free to select prescribers as well.


Greenway Health CEO Scott Zimmerman cancels the company’s annual user group conference set to take place this weekend in Orlando. Verscend Technologies also made the similarly tough yet necessary choice to cancel its customer event in Miami.
Reader Comments

From Van Helten: “Re: Data silos. Here’s an exclusive photo of one being installed at a hospital in Virginia.”
HIStalk Announcements and Requests
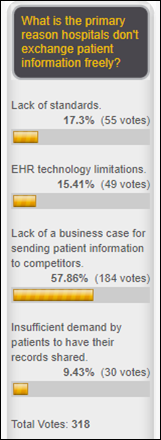
Cash seems to be king when it comes to why hospitals don’t freely exchange patient information. Over half of respondents believe hospitals don’t share information because the business case for sending patient health data to competitors is lacking. Print Geek contends, “There should an option here for ‘lack of government leadership and intervention supporting interoperability.’ As much as it pains me to put more of healthcare in the hands of the fed, the banking and travel businesses seemed to figure it out themselves. Healthcare’s inability to solve this themselves screams for government intervention.” Clustered points out that, “There is a business case *not* to use shared data. Facilities can bill for repeating a procedure/test, if they don’t have access to the results (e.g., if an MRI exam was performed elsewhere). They can’t bill for requesting and receiving prior medical records. While that may sound irresponsible to a clinician, it certainly makes sense to the CFO/CEO of a hospital. We’re in the business of facilitating information sharing and we see it all the time (‘yet another piece of software that will help me decrease revenues’ – sometimes we can almost see the thought bubble).” Anonymous asks, “Aren’t ‘insufficient demand by patients’ and ‘lack of a business case’ hugely overlapping? Patients need to create the business case. If we had a health system where patients felt empowered to own their data, instead of feeling like Elaine in the Seinfeld episode where she just wants to be treated for her rash, I think the business case would be obvious.”
New poll to your right or here: Has a lack of interoperability ever hindered your or a loved one’s ability to receive healthcare services in the midst of or after a natural disaster? I’m thinking especially about hurricane evacuees who’ve wound up away from their homes for weeks or months. Please leave a comment as to what happened and how you resolved the situation. Your experience may end up helping those struggling to jump through the hoops of finding post-Harvey and (eventually) post-Irma healthcare.
This Week in Health IT History

One year ago:
- The NHS names 12 health IT “global exemplars” that will receive $13 million in health IT funding to establish best practices and a new digital health academy.
- The DoJ and FTC back Teladoc in the telehealth vendor’s legal battles with the Texas Medical Board, saying that the board’s restrictive telemedicine rules are anticompetitive and were not appropriately reviewed.
- France-based consulting firm Atos will acquire Anthelio Health Solutions for $275 million.
- Cleveland Clinic files plans to build a 205-bed private hospital in London’s upscale West End.
- HHS will provide $87 million to 1,310 safety net health centers for purchasing or upgrading EHRs.
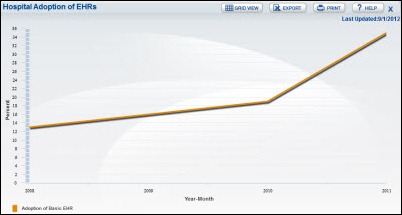
Five years ago:
- ONC publishes a Health IT Dashboard that includes six views and 250 custom dashboards for states, ONC programs, and grantees.
- The board of Allscripts approves a $1.9 million 2012 incentive for CEO Glen Tullman.
- Elsevier acquires ExitCare, LLC, an enterprise-wide solution for patient education and discharge instructions.
- PE firm Thoma Bravo acquires Mediware for $195 million.
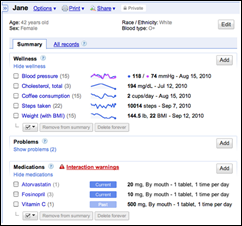
Ten years ago:
- Google unveils an upgraded version of Google Health that includes a cleaner interface and more focus on wellness.
- Stanford’s Lucile Packard Children’s Hospital appeals the $250,000 fine levied by the state’s health department when the hospital waited 11 days before reporting a stolen, PHI-containing laptop.
- MyChart comes to iTunes.
- Outpatient imaging center operator RadNet acquires Image Medical Corporation for $10.75 million in cash and notes.
- EHealth Ontario signs a $46 million contract with Canada-based CGI Group to develop and manage a diabetes management portal.
Last Week’s Most Interesting News
- STAT investigates IBM’s failure to develop Watson into a revolutionary technology for cancer care, highlighting the fact that its marketing blitz may have over-promised on the machine’s capabilities.
- The FDA launches a Digital Health Entrepreneur-in-Residence program to help develop and launch its Software Precertification Pilot.
- Equifax informs the public that a data breach discovered in late July could affect up to 143 million people.
- Fidelity National Financial will acquire emergency department clinical documentation and coding vendor T-Systems for $200 million in cash.
- Jeanne Lillig-Patterson, founder of the First Hand Foundation and wife of Cerner co-founder Neal Patterson, dies at the age of 59 after losing her battle with cancer.
Webinars
September 13 (Wednesday) 1:30 ET. “How Data Democratization Drives Enterprise-wide Clinical Process Improvement.” Sponsored by: LogicStream Health. Presenter: Katy Jones, program director of clinical support, Providence Health & Services. Providence is demonstrating positive measurable results in quality, outcomes, and efficiency by implementing clinical process improvement solutions in arming operational and clinical stakeholders with unlocked EHR data. Providence’s army of process engineers use their self-service access to answer questions immediately and gain an understanding of how their clinical care delivery is impacting outcomes. The presenter will describe practical applications that include antibiotic stewardship, hospital-acquired infections, and comprehensive knowledge management.
September 28 (Thursday) 2:00 ET. “Leverage the Psychology of Waiting to Boost Patient Satisfaction.” Sponsored by: DocuTap. Presenter: Mike Burke, founder and CEO, Clockwise.MD. Did you know that the experience of waiting is determined less by the overall length of the wait and more by the patient’s perception of the wait? In the world of on-demand healthcare where waiting is generally expected, giving patients more ways to control their wait time can be an effective way to attract new customers—and keep them. In this webinar, attendees will learn how to increase patient satisfaction by giving patients control over their own waiting process. (Hint: it’s not as scary as it sounds!)
Previous webinars are on our YouTube channel. Contact Lorre for information on webinar services.
Acquisitions, Funding, Business, and Stock

Wellsoft enlists consulting firm MedProjects to help market and implement its EDIS at St. Luke’s Medical Center in the Philippines as part of a broader push into the region.
Technology

With help from UPS, the Red Cross will begin test flights this week of a drone that will assess damage and potentially deliver aid to areas devastated by Hurricane Harvey. The deployment, which comes a year after the Federal Aviation Administration loosened up its restrictions on using drones for commercial activities, could lead to additional flights into areas affected by Hurricane Irma.

Users of DexCom continuous glucose monitoring products will soon be able to track their CGM data on FitBit’s Ionic smartwatch.
![]()
Navicure announces integration of its automated patient payment tool with Epic.
Smart Communications will integrate its communications management technology with Casenet’s TruCare population health and care management platform for payers.
Privacy and Security
University of Wisconsin-Madison’s Department of Family Medicine and Community Health notifies select patients that it violated HIPAA when it sent information about a quality improvement survey on a postcard rather than in a sealed envelope. The postcard referred to individual patient medications and family planning services.
Innovation and Research
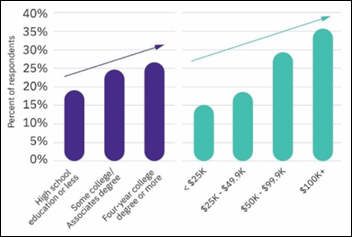
A Truven Health Analytics survey finds cost to be the top reason patients don’t fill their prescriptions. A third of those surveyed look at drug costs before filling their prescription – a practice that decreases with age. Looking for lower prices, twelve percent have taken to filling their prescriptions outside of the US. Strangely, those with higher incomes and levels of education are more likely to miss a dose.

Henry Ford Macomb Hospital and the AMA see an increase in patient referrals to diabetes prevention programs six months into piloting a pre-diabetes registry developed with help from Epic.
Other

The New York Times looks at the ways in which emergency relief procedures for Hurricane Harvey compare with those of Katrina, highlighting the work done by Congress and FEMA in the intervening years to make sure resources, strategies, and playbooks were in place and trusted by community leaders well before Harvey spun its way into Texas and Louisiana. The author also points out the work HHS has done to make sure hospitals and nursing homes are better equipped and trained to evacuate, with the ultimate goal of only having to move residents once.
Surgeon, author, and speaker Atul Gawande, MD places blame for the opioid epidemic squarely on the shoulders of physicians, attributing the propensity of physicians like himself to unknowingly overprescribe to medical training that encouraged such practices:
“The cause in the opioid epidemic starts with getting a prescription of opioids from physicians. We weren’t recognizing — I certainly wasn’t recognizing — the extent to which we were putting people at risk. I think the key thing that has stuck in my mind was that when you go in for an operation, and you give a supply of opioid pills, that if people are on those pills for 7 days they have an 8 percent chance of one year later still being on those narcotic pills. It is huge. It is startling. I had no idea. Basically, I was like more is better, take some.”
Sponsor Updates

- West Corp. volunteers pack 8,790 meals in under an hour for Omaha Against Hunger.
- Bernard Tyson (Kaiser Permanente) joins Salesforce’s Board of Directors.
- Surescripts will exhibit at the AAFP Family Medicine Experience September 12-16 in San Antonio.
- Verego awards Sutherland its Corporate Social Responsibility certification.
- Wellsoft will exhibit at HIMSS AsiaPac17 September 11-14 in Singapore.
- ZirMed will exhibit at the CareVoyant User Group Conference September 13-15 in Schaumburg, IL.
Blog Posts
- Healthcare Accelerators for Startups (Redox)
- 5 Pieces of Advice for Female Entrepreneurs Who Have Been There, Done That (Salesforce)
- Hospital EHR Adoption Rates Rise, Don’t Necessarily Ease Information Flow (Definitive Healthcare)
- Patient Navigators and Your Hospital Revenue Cycle (The SSI Group)
- Cultivating Your Practice’s Unspoken Voice (Solutionreach)
- Clinical Technology. Does it have to be so disruptive? (Sphere3 Consulting)
- Automated workflows, current knowledge make precision medicine possible (Sunquest Information Systems)
- Thinking inside the box with a provider decision quadrant: monitoring provider network stability (Verscend Technologies)
- CRISPR-Cas9 Trials Target Cancer Cell Research (Definitive Healthcare)
Contacts
Mr. H, Lorre, Jenn, Dr. Jayne, Lt. Dan.
Get HIStalk updates. Send news or rumors.
Contact us.



I want to add the following. I'm an IT professional. In the course of my professional duties, I'm expected to…