RE: Change HC/RansomHub, now that the data is for sale, what is the federal govt. or DOD doing to protect…
News 6/7/17
Top News
VA Secretary David Shulkin, MD announces the VA will shut down its VistA EHR and join the DoD in implementing Cerner Millennium, explaining, “The VA’s adoption of the same EHR system as DoD will ultimately result in all patient data residing in one common system and enable seamless care between the Departments without the manual and electronic exchange and reconciliation of data between two separate systems.”
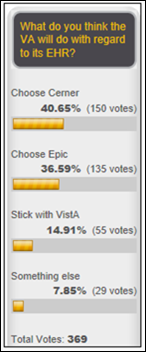
HIStalk readers (who predicted the Cerner decision in a reader survey earlier this year) didn’t waste time weighing in once the news crossed the wire yesterday – nearly a month before Shulkin’s self-imposed decision deadline. VA Worker says, “Here we go again. VA wants to replace VistA with Cerner but will never be able to afford it.” USA First? points out that, for all the Trump Administration’s efforts to keep American jobs on American soil, they’ve chosen a vendor that has sent 3,000 software jobs overseas.
Epic also shared its reaction via a presumably non-marketing rep: “As the largest electronic health record vendor in the United States, covering two-thirds of the nation’s patients, we are proud to serve our veterans both through the VA scheduling project and through our customers that care for millions of veterans across America. These customers are the top health systems in America and we stand with them, committed and eager to ensure veterans get the very best medical care regardless of where they receive it.”
My thoughts are these: Cerner was the only reasonable choice since the DoD had already selected it, but it’s still surprising they went without bidding and named Cerner before negotiation with them began (that’s more of how Epic customers buy software). The company will presumably have more control over naming its price than it did with DoD, where it was a subcontractor under Leidos, and it may be that Cerner gets to keep all the money this time. It’s also to the company’s strong negotiating advantage that both Congress and the President have publicly cheered the VA’s choice of Cerner, making it unlikely that the VA wants to rule out Cerner over price negotiations. The VA has previously suggested that its price tag will be multiples of the DoD’s, perhaps well over $10 billion to $12 billion.
The systems will be theoretically interoperable, but there’s still a lot of work to be done to standardize terminology and functionality to make even the same system talk to another user whose workflows and use cases are different. There’s probably still a lot of consulting work required. It will be interesting to see which firms attempt to feed at the trough of this contract, as well as whether or not the VA and DoD will truly work as a single customer. Will Cerner and the inevitable consultants get stuck trying to broker agreements on major decisions so they don’t end up creating dissimilar systems?
It’s also worth noting that project timelines will need to be synched to avoid temporary interfaces to the legacy systems. Ironically, having the same system may require more VA-DoD cooperation than running separate ones. On the flip side, it’s also important to recognize that the VA and DoD have vastly different needs, and that in the case of the VA (unlike the DoD), its VistA system contains a lot of VA-specific non-clinical functionality, such as management modules for departments that aren’t involved in patient care. VistA is not just an EHR.
Reader Comments

From Mighty Med: “Re: Walnut Hill Medical Center closure. The self-touted hospital of the future abruptly shuts its doors after being open for less than three years. It’s just another example of healthcare disruption gone awry.” The $100 million, 100-bed Dallas hospital did indeed cease operations as of June 1, citing only it’s decision to no longer participate in the Medicare program. A former employee wrote a Facebook farewell message (later taken down) praising his colleagues for working without the “unlimited resources” of traditional hospitals, implying that it was struggling in some way. Officials touted the facility as being designed “completely from the patient’s perspective to create a stress-free atmosphere for healthy recovery.“

From Just Wondering: “Re: John Fleming’s desire for a single unified EHR. Is he as stupid as he sounds?” Hardly. The former Louisiana representative, businessman, and MD has done stints at the Navy Regional Medical Center (CA) and in private practice. He implemented his first EHR in 1997 and went fully paperless two years later. Fleming’s belief that “every American should have a single, unified electronic health record system that resides in the cloud and is under full control of the patient, of the individual, of the American” is the same pipe dream that dozens, if not hundreds, of health IT companies and venture capital firms have been throwing millions of dollars at for years. As the new deputy secretary of health technology reform, he’s becoming privy to the many public- and private-sector interests that will keep that pie-in-the-sky patient record from being developed anytime soon.
HIStalk Announcements and Requests
An anonymous vendor has graciously donated $500 to my project to fund DonorsChoose teacher grant requests in return for mentioning a survey they’re interested in. They’ll also donate a bunch more money if the survey gets at least 100 responses. Providers, please click here and spend a handful of minutes and together we’ll to help a classroom in need. Thanks.
Webinars
June 22 (Thursday) 1:00 ET. “Social Determinants of Health.” Sponsored by Philips Wellcentive. Presenter: David Nash, MD, MBA, dean, Jefferson College of Population Health. One of the nation’s foremost experts on social determinants of health will explain the importance of these factors and how to make the best use of them.
June 29 (Thursday) 2:00 ET. “Be the First to See New Data on Why Patients Switch Healthcare Providers.” Sponsored by Solutionreach. As patients pay more for their care and have access to more data about cost and quality, their expectations for healthcare are changing. And as their expectations change, they are more likely to switch providers to get them met. In this free webinar, we’ll look at this new data on why patients switch and what makes them stay. Be one of the first to see the latest data on why patients leave and what you can do about it.
July 11 (Tuesday) 1:00 ET. “Your Data Migration Questions Answered: Ask the Expert Q&A Panel.” Sponsored by Galen Healthcare Solutions. Presenters: Julia Snapp, manager of professional services, Galen Healthcare Solutions; Tyler Suacci, principal technical consultant, Galen Healthcare Solutions. This webcast will give attendees who are considering or in the process of replacing and/or transitioning EHRs the ability to ask questions of our experts. Our moderators have extensive experience in data migration efforts, having supported over 250+ projects, and migration of 40MM+ patient records and 7K+ providers. They will be available to answer questions surrounding changes in workflows, items to consider when migrating data, knowing what to migrate vs. archive, etc.
Previous webinars are on our YouTube channel. Contact Lorre for information on webinar services.
Acquisitions, Funding, Business, and Stock

Learning management systems vendor Relias Learning acquires WhiteCloud Analytics for an undisclosed sum. Reliance has been on a bit of a spending spree since March of last year, acquiring six other companies including analytics firm Care Management Technologies.

Aegis Health merges with digital marketing firm Clariture to form Trilliant Health. The companies will retain their brands as separate business units.
Announcements and Implementations

Mayo Clinic (MN) will use 2bPrecise’s clinical genomics solution to add genomic information into its Epic EHR. The organizations will also work together to research and develop genomics-based care protocols, particularly for patients with cardiovascular genetic disease.
Aprima announces record growth for the fiscal year, including revenue, customer retention rate, and the relocation and expansion of its headquarters.
Technology

Apple announces new devices and features at its developers conference – none of which are all that earth-shattering and only some of which are relevant to healthcare. The company will attempt to keep up with the virtual assistant Joneses with the introduction of a Siri-powered HomePod. It has added AI capabilities to its Watch, giving it the ability to serve up motivational fitness messages when steps are down. Users will also be able to link their devices to Dexcom’s glucose sensor via a new API. Perhaps the most potentially life-saving enhancement is the Iphone’s forthcoming “do not disturb while driving” feature, which shuts off all distracting notifications when the phone is connected to your car.

Casenet develops a prior authorization submission and tracking tool.
PointClickCare adds Ability Network’s claims management capabilities to its EHR for long-term and post-acute care providers.

Safety Net Connect releases an enterprise version of its Converge referral and care coordination technology that brings together behavioral and physical health, and social services.
ICare adds order sets and care plans from Zynx Health to its EHR for acute care providers and SNFs.
Government and Politics
ONC announces the winners of its Privacy Policy Snapshot Challenge, the aim of which escapes me as the number of these contests seems to increase in direct correlation to the market-worthy usefulness of their winning ideas.
Sales

Tufts Medical Center (MA) chooses ZappRx to automate the ordering of specialty drugs, expecting to reduce the average prescribing time from 20 minutes to three minutes.

Children’s Hospital of Wisconsin selects CRM software from Healthgrades.
Privacy and Security

HHS alerts providers to the “significant” challenges two unnamed multi-state hospital systems are still experiencing as a result of WannaCry malware, noting that the virus can live on a machine that has been patched, and that its repeated attempts to scan can disrupt Windows operating systems.
Innovation and Research
Early performance data on IBM Watson for Oncology shows that Watson-generated treatment plans for 362 cancer cases were found to be in line with oncologist recommendations in 96 percent of lung, 81 percent of colon, and 93 percent of rectal cancer cases.
People

Michael Caponetto (West Health) joins government healthcare program services company SynerMed as CFO.
Other

The New York Times addresses the “virtual velvet rope” creeping into healthcare – one that is moving beyond celebrities and sheikhs taking over hospital wings and turning the more mundane world of direct primary care into one of ultra high-end concierge practices. Private Medical, for instance, charges between $40,000 and $80,000 per year per family for round-the-clock physician access and near-immediate access to specialists and hospitals across the country. Launched by HealthLoop founder Jordan Shlain, MD in 2002, the company has almost no Web presence, gaining new patients almost exclusively through word of mouth.
Sponsor Updates

- Direct Consulting Associates donates fabric and stuffed animal kits to help middle-school students make stuffed animals, blankets, and pillows for local charities.
- ClinicalArchitecture partners with OpenAirWare to more easily integrate patient data from standard clinical information exchange formats with its Advanced Clinical Awareness Suite.
- Software Advice names AdvancedMD a 2017 Mental Health FrontRunners Quadrant Leader.
- Agfa HealthCare successfully completes the recertification audit cycle for its information security management system.
- Aprima Medical Software will exhibit at the NJ MGMA meeting June 14-16 in Atlantic City.
- Bernoulli Health will exhibit at AAMI Conference and Expo June 9-12 in Austin, TX.
- Besler Consulting releases a new podcast, “Looking at price data on local healthcare markets across the United States.”
- Kyruus will host its ATLAS Conference on patient access September 19-20 in Boston.
- Casenet, Cumberland Consulting Group, EClinicalWorks, InstaMed, and InterSystems will exhibit at AHIP Institute & Expo June 7-9 in Austin, TX.
- Dimensional Insight remains a top performer in the Wisdom of Crowds 2017 Business Intelligence Market Study.
- Casenet clients and employees donate gift bags to children at CHA Cambridge Hospital (MA).
- ECG Management Consultants will present at the 2017 Science of Team Science Annual Conference June 13 in Clearwater, FL.
- Glytec will exhibit at the American Diabetes Association Scientific Sessions June 9-13 in San Diego.
- Healthwise will exhibit at the Cerner North Atlantic Regional User Group June 12-14 in Springfield, MA.
- Iatric Systems will exhibit at the NCHICA AMC Security & Privacy Conference June 12-14 in Chapel Hill, NC.
- The Atlanta Business Chronicle names Ingenious Med a “Pacesetter” for the fifth consecutive year.
- Kyruus will exhibit at the Annual Conference of Healthcare Call Centers June 7-9 in Salt Lake City.
- Inc. Magazine includes PMD on its list of best places to work.
- Definitive Healthcare CEO Jason Krantz is named a finalist for E&Y’s Entrepreneur Of The Year 2017 New England Award.
- Imprivata releases a new report, “High-value, complex clinical workflows require enhanced communications capabilities.”
Blog Posts
- Medication Adherence in the Safety Net: Where Simple Innovations Make Big Impact (FDB)
- 5 areas to focus your 2017 MIPS strategy (Nordic)
- CMS Quality Payment Program – MIPS Path (Culbert Healthcare Solutions)
- Take Action Now to Protect Your Online Information (Dynamic Computing Services)
- Key Takeaways from the 2017 Wisdom of Crowds BI Market Study (Dimensional Insight)
- Healthcare Informatics: One-On-One with CEO Jason Mabry (Optimum Healthcare IT)
- Putting ClinicalKey in doctors’ hands through Research4Life’s developing country access (Elsevier Clinical Solutions)
- Can interoperability defeat the asymmetry beast? (EClinicalWorks)
- The Art & Science of Understanding Physician Activity and Referral Patterns (Evariant)
- 5 Cool Things in Healthcare (Hayes Management Consulting)
- Three considerations when implementing two-factor authentication (Imprivata)
- A Healthcare CIO’s Consumer Experience Wish List (Influence Health)
- A quick and painless intro to rolling out your EHR (Nordic)
- 10-Step Guide to Securing Data at Your Hospital (Spok)
Contacts
Mr. H, Lorre, Jenn, Dr. Jayne, Lt. Dan.
More news: HIStalk Practice, HIStalk Connect.
Get HIStalk updates. Send news or rumors.
Contact us.



I love the subtle digs you make at Cerner in regards to their VA win. I’m sure if Epic had won, it would have been nothing but praise. You could at least try to make the illusion of being fair and balanced…
It’s hilarious that readers persist in posting this kind of nonsense about HISTALK despite the fact that a.) HISTALK regularly posts things critical of Epic and b.) HISTALK is critical of Epic in this very newsitem. Grow up people. You don’t need to spew your propaganda 24-7.
While I applaud the decision of the VA to also adopt Cerner, I am not looking forward to increased negative impact from this new large and one continuing implementation that is affecting those of us implementing Cerner now. It has been an extreme challenge to find qualified Cerner implementers, including from Cerner itself.
Re: Justa CIO For the DOD, Leidos is supplying most of the resources, not Cerner. As for the VA, I cannot speak to the resourcing structure. The issue with Cerner resources is that many of the good ones have gone either full time to a healthcare system because of work slowing down OR they have priced themselves out of the market because today’s rates are much lower than what they were a few years ago. If you are struggling with resources, I have several contacts that could help in almost every solution area. Full transparency, I used to run a consulting practice, but got out about 2 years ago and have focused more on strategy, not EMR implementation. Happy to help where I can
Mr. H couldn’t have phrased it any more factually: “theoretically interoperable.” Betting $12 billion on the strength of Cerner-to-Cerner exchange is a longshot with odds worse than picking a single number on a roulette wheel. Cerner customers connect amazingly well at their flagship customer, PowerPoint Health, and very few other places.
So, the VA just announced Cerner? I remember working on that disgustingly huge response to the RFP, in partnership with GE, many, many years ago. Then I was out of healthcare IT vendorship for a while. I’d say I can’t believe it took so long for them to make a selection, but… government.