Sounds reasonable, until you look at the Silicon Valley experience. Silicon Valley grew like a weed precisely because employees could…
News 8/12/16
Top News



Karen DeSalvo, MD, MPH has resigned as National Coordinator, with her last day being Friday. She will be replaced by Principal Deputy National Coordinator Vindell Washington, MD, who joined ONC in January 2016.
DeSalvo will continue in her full-time role as Assistant Secretary for Health.
Reader Comments

From HIT enthusiast: “Re: Anthelio Healthcare. Acquired by France-based ATOS in a private sale this week.” Unverified. I reached out to the company but haven’t heard back.
From Anointee: “Re: HSM. Have you heard how much Huron Consulting paid to acquire it?” I have not heard. Reports are welcome.
From One Mississippi: “Re: rating the ratings. While working on my masters, I had a class in surveying and research. The class was mostly automotive folks since it was in metro Detroit. The professor brought up KLAS as an example of a horrible surveyor. Their margin of error is huge since participants engage for a variety of unscientific reasons. He said, ‘Research should be conducted for research purposes only,’ while KLAS does research to meet pre-determined criteria for their vendor customers.”
HIStalk Announcements and Requests
Grammar peeves: saying “less” instead of “fewer” when referring to something that has a discrete quantity. A hospital does not have less nurses, although it might well have fewer nurses. I’m also annoyed by “should of” instead of “should have” and “6 a.m. in the morning.” I’m also alarmed at the increasingly common practice of starting a sentence with “So” like the author is telling an overly descriptive tale (“So I walk into this bar …”) I immediately stop reading when I see that.
This week on HIStalk Practice: Justin Barnes brings readers up to speed on life after Greenway, plus offers his take on how the new administration will handle health IT. Pathway Health adds Virtual Health PHM technology to its consulting services for the post-acute care market. Kinsa hopes its smart thermometer tech will help identify Zika Virus hot spots in Rio. PrecisionBI develops ACO module for TouchWorks users. MyHealthDirect integrates online appointment scheduling with Microsoft Office 365. Community Care Collaborative selects Vital Data Technology’s case management, care coordination tools. Navicure CEO Jim Denny offers advice to practices looking to get an analytics program off the ground. Government initiatives to combat the opioid epidemic take center stage this week.
Webinars
August 24 (Wednesday) 1:00 ET. “Surviving the OCR Cybersecurity & Privacy Pre-Audit: Are You Truly Prepared?” Sponsored by HIStalk. Presenter: John Gomez, CEO, Sensato. Many healthcare organizations are not prepared for an OCR pre-audit of their privacy and security policies. This webinar will provide a roadmap, tools, and tactics that will help balance policies and budgets in adopting an OCR-friendly strategy that will allow passing with flying colors.
Contact Lorre for webinar services. Past webinars are on our HIStalk webinars YouTube channel.
Acquisitions, Funding, Business, and Stock
Plymouth Meeting, PA-based Accolade, which engages health plan members to encourage them to make cost-effective healthcare decisions, raises $70 million, increasing its total to $160 million.

CPSI announces Q2 results: revenue up 45 percent, EPS $0.15 vs. $0.52. The company blames the poor results on hospitals taking longer to make decisions as well as lower add-on sales. Share price gapped down on the news and have dropped 37 percent in the past year. From the earnings call:
- The company will no longer provide earnings and revenue guidance due to variability in subscription vs. license sales and challenges in forecasting the contribution of Healthland, which it acquired in November 2015 for $250 million.
- Chairman David Dye said in the earnings call that traditional competitors have largely abandoned the community hospital EHR market and new entrants have fizzled.
- Dye adds that Athenahealth’s claims of displacing incumbent vendors, including CPSI, with the former RazorInsights system reflects their hard-selling of contracts with no money down and a 90-day out clause, meaning the hospital may never even go live, adding that only one Evident customer has gone live on Athenahealth while CPSI has replaced Athenahealth at two sites.
- Dye acknowledges that Athenahealth’s prices are lower and the company could become a formidable inpatient competitor, but adds that of the 23 RazorInsights hospitals that attested for Meaningful Use, three have moved to CPSI, another signed with CPSI this week, three have closed, and another three are converting to another non-CPSI system.
- Dye says that CPSI rarely faces off against Epic, but Cerner’s hosting services and price reductions have allowed it to sell to even the smallest hospitals in competing with CPSI.
Predictive analytics vendor CareSkore raises $4.3 million in its initial funding round. The company’s product analyzes EHR inpatient data to assess a patient’s clinical and financial risk.

NantHealth announces Q2 results: revenue up 167 percent, adjusted EPS –$0.15. Shares are up around 8 percent since the announcement, but are still down 42 percent from their first-day close following the company’s June 2016 IPO.
Sales

In Canada, Joseph Brant Hospital will implement Orion Health’s Rhapsody Integration Engine.
People

Medicomp Systems promotes Jason Valore to GM of Asia/EMEA.
Announcements and Implementations
The HIMSS-SIIM Enterprise Imaging Workgroup publishes a white paper covering enterprise viewers, the fifth in a series that will be published in the Journal of Digital Imaging.
Forward Health Group and Leavitt Partners will collaborate to support practices and payers participating in CMC’s CPC+ payment initiative.
Government and Politics

The VA issues an RFI for change management services related to its potential implementation of a commercial EHR product, with the VA indicating that it is especially interested in companies with prime contractor experience in large EHR conversions. Areas of interest include governance, change management, go-live planning, business continuity planning, testing, patient safety, cybersecurity, and interoperability.
Privacy and Security
From DataBreaches.net: a Virginia dermatology practice notifies 13,000 patients that their information was exposed when it fell victim to a ransomware attack. The practice’s statement did not say if it paid the ransom.
Technology
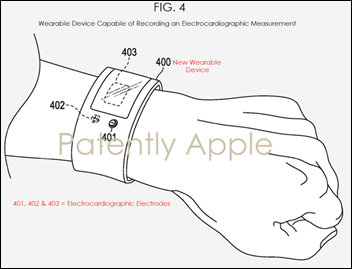
Apple publishes another health-related patent, this one for a wearable ECG monitor.
In other Apple news, the company rehires Evan Doll, who left his Apple iPhone software development job in 2009 to co-found the Flipboard magazine reading app, to develop healthcare-related software.
Other
A Wall Street Journal report notes the 10-fold increase in Medicare payments for tests administered in physician offices over the past two years, although the total is still relatively paltry at $16.7 million. Four of the 10 fastest-growing Medicare service costs involve tests run on new in-office devices that the physician can bill for directly rather than referring them out. Examples include a sweat test device and the TearLab tear osmolarity test for dry eyes, which one “Accredited Dry Eye Center” ophthalmologist ran on 84 percent of his Medicare patients in 2014 for payment of $131,000.

Forbes names Epic’s Judy Faulkner as one of the world’s five richest women in technology, estimating the value of her company ownership at $2.7 billion.
A NEJM op-ed piece by a medical school professor says the hospitalist model is good for hospitals, but unproven when it comes to patients and physicians as it diminishes the physician-patient relationship, introduces coordination challenges, and puts patients in the awkward position of having to trust someone they’ve never meet in times of critical need. It also notes that hospitalists who never see outpatients don’t understand what happens outside the hospital and thus can’t serve as advocates for comprehensive care. The author wonders how physician knowledge sharing and collegiality will suffer as the doctors’ lounge is “depopulated” as inpatient and outpatient physicians stick to their respective turfs. It also notes that hospitals market themselves as being more important than relationships with individual physicians but community engagement is compromised by the reduced role of community-based doctors. The article concludes that “medicine can be practiced without hospitals, but hospitals cannot function without physicians … the hospital itself is ultimately a tool … without which patients can still be given care.”
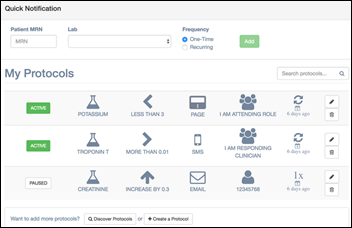
Harvard-based Herald Health will pilot its customizable clinical alerting system at Brigham and Women’s Hospital, integrating with Epic to allow doctors to specify the conditions under which they want to be notified about new results.
An article in The Atlantic says people who go into cardiac arrest might fare better in a casino or on an airplane than in a hospital, where studies show that only two-thirds of providers would notice that a patient is not breathing and without a pulse. Laypeople are more likely to start resuscitation immediately, while clinicians spend time analyzing heart monitors or thinking about drugs to administer instead of starting compressions. The article mentions an algorithm developed by University of Chicago Medicine that analyzes vital signs in real time to predict which patients are likely to have cardiac arrest in the next 24 hours.
An MGMA survey finds that physician-owned multispecialty practices spent $32,500 per full-time doctor on IT in 2015.
Researchers looking at food and exercise studies whose results conflict (are coffee and flossing good or bad?) say most of them contain invalid conclusions or are not reproducible because patients don’t provide good information and the large number of data element possibilities for diet, exercise, and health outcomes can be used to prove almost any desired point. Some experts say that it’s a waste of time to conduct lifestyle studies because they are full of problems and they almost never prove anything useful.
I guess this counts as tele-romance (or is it tele-cardiology?) A company launches a ring ($600 per pair for the basic model) that when tapped, connects to a love one’s counterpart ring via Bluetooth and smartphone to allow feeling each other’s heartbeat in real time. My initial reactions: (a) it’s huge; (b) it’s pointless given that the same smartphone it requires can already send text messages, voice calls, or video for free; (c) it’s yet another gadget that requires regular charging; (d) suspicions might be raised if the heart rate of the “working late” partner suddenly increases; and (e) someone’s going to panic when it can’t connect to the other person and they assume the worst.
Sponsor Updates
- HCI Group offers a Jaguars vs. Packers weekend event September 9-11 in Jacksonville, FL for Epic-certified consultants that includes an open house, happy hour, a beach day, and a pre-game tailgate.
- Twenty Meditech hospitals receive five-star ratings from CMS.
- Navicure will exhibit at the Azalea Health Leaders Summit August 18-20 in Atlanta.
- Netsmart will exhibit at the Mental Health Corp. of America Summer Conference August 16 in Portland.
- Experian Health will exhibit at Florida AAHAM August 17-19 in Clearwater Beach, FL.
- Patientco will sponsor the Decatur BBQ & Bluegrass Festival August 13 in Decatur, GA.
- PatientMatters will exhibit at the HFMA Arkansas Summer Institute August 17-19 in Hot Springs.
- SK&A publishes a complimentary report, “Top 25 Integrated Health Systems.”
Blog Posts
- The Patient Advocate: Meet Spok’s New CNO (Spok)
- CDI embraces patient-centric care with the Lexmark VNA (Lexmark)
- Perinatal Nursing & Technology – Time to Accept & Embrace the Challenge (Part 3) (PeriGen)
- Lessons From Sticking Around (PMD)
Contacts
Mr. H, Lorre, Jennifer, Dr. Jayne, Lt. Dan.
More news: HIStalk Practice, HIStalk Connect.
Get HIStalk updates. Send news or rumors.
Contact us.





Is it just me, or does Judy Faulkner not look 73? I don’t know what they’re eating in Madison but order me up some of that! She looks 20 years younger by her photo (possibly an old photo??).
[From Mr. H] I’ve seen her fairly close up at HIStalkapalooza and she definitely would strike you as being maybe late 50s at the oldest, both in appearance and energy level.
Sad to see that it is 2016 and still the first comment about an entrepreneur who built an industry leading tech company from nothing is about how she looks.
I see that those seeking to take offense, will not be denied.